Bone density is a key factor in bond fracture prevention. Bone is made of cells that die and regenerate. When this process is compromised, the risk of fracture arises. During the early stages of life, we can ensure that we intake and store calcium through food to build up our bones, but after a certain age (about 30), the body stops absorbing calcium, and the storage that we created is now our reserve for the rest of life. Cell Regeneration in Bone and Other Body’s Tissues The body’s cells, like muscle cells, skin cells, tendon cells, ligament cells and even bond cells, are in constant change via a process called cell regeneration. Old cells die off and they get replaced with new cells. In the case of bone, the cells that allow this process to happen are called osteoblasts. While we age, this process slows down, meaning that cells would still die, but they don’t get replaced. A typical example is a woman going through menopause. Estrogen, which is the hormone responsible for bond metabolism, allows the activity of osteoblasts. During menopause, indeed, women have a drop in Estrogen production, and osteoblasts are not as operative as they used to be. Strength Exercises and Cell Regeneration As this meta-analysis shows, strength exercises are a positive stress stimulus for the body and can help the osteoblast work harder and maintain bone cell regeneration. When the body perceives stress as physical resistance, it does its best to establish a reparation mechanism. So whenever we pick a weight against gravity, the body would implement a regeneration of the tissue that are used to complete this action. Who Is at Risk of Losing Bone Mass? There are several factors that can contribute to decreased bone mass: Age: Bone density typically peaks in early adulthood and declines with age. Gender: Women, especially postmenopausal, are at higher risk due to hormonal changes that accelerate bone loss. Family History: A family history of osteoporosis can increase risk. Body Size: Individuals with smaller body frames may have less bone mass to draw from as they age. Hormonal Levels: Thyroid imbalances and reduced sex hormones can lead to bone loss. Dietary Factors: Low calcium and vitamin D intake contribute to diminished bone density. Lifestyle Choices: A sedentary lifestyle, excessive alcohol consumption, and smoking are linked to weaker bones. I have included factors like dietary and hormonal levels in the above list. Bear in mind that taking supplements such as calcium and vitamin D (which helps retain calcium) could have severe contraindications. So, always talk to your doctor or specialist about the intake of supplements. How to determine Bone Density? To determine bone density, there is a diagnostic test called Dual-energy X-ray Absorptiometry (DEXA or DXA). This non-invasive procedure measures the mineral content in bones, usually in areas like the spine, hip, or wrist, to assess bone density and identify potential risks of osteoporosis or fractures. The results are given as a T-score, which compares your bone density to the average peak bone mass of a healthy young adult. A T-score of -1.0 or above is considered normal, while a score between -1.0 and -2.5 indicates low bone mass (osteopenia), and a score of -2.5 or lower suggests osteoporosis. Other methods, like ultrasound or quantitative computed tomography (QCT), can also assess bone density, but DEXA remains the gold standard for bone health evaluations. Mobility before strengthening So far, we have discussed how strength exercises are a good way to maintain bond density. Still, I would not recommend that anyone who is not into strength exercise and has bone density issues go and start lifting heavily. Why (?), you may ask. Well, before we start lifting heavy, we want to ensure that the body mechanics are optimal for it, so we better start looking into your mobility and then pass on to the strength part of things. Please be aware that mobility has nothing to do with elasticity or stretching. Those are different practices. How Can We Achieve Great Mobility For people who decide to take a journey to ensure an optimal level of mobility and then strengthen the body, the first step is to assess their joint mobility with active and passive range of motion. After that, we could use a combo of Myotherapy treatment and mobility exercises to ensure they can quickly pick up the best of their mobility capacity, given their subjective presentation. And here is a list of mobility exercises which we may look into at first: Hip Openers to improve range of motion in the pelvis and lower back. Ankle Drills to support proper weight distribution in weight-bearing exercises. Thoracic Spine Mobility Exercises to prevent excessive strain on the lower back. AC Joint External rotation to ensure we can build strong rotator cuff muscles, essential for shoulder health It Is Time To Strength. How Can We Do This? Once the minimum mobility is achieved, which may take 1 to 2 weeks of training, depending on each individual and their subjective history and effort, we can start looking into more strengthening exercises. So, here is a list of different exercises that can help with strengthening, written with the progressions to follow: Calf raises with double leg, single leg and weight Hamstring and Quads Curl that gets weight added as weeks go by Standing Adduction and Abduction at cable machine or with resistance bend Glut Muscles training at cable machine or with resistance bend Deadlift for back and posterior chain muscle strength Squat with weights and explosion variations Cuff rotator-specific strength is Ideal before stepping into more complex arm weight-lifting Cervical muscle strength to prevent cervical headache and sore neck All of those exercises, except the cervical one, can then be modified to achieve plyometric drills and combined movement. But this is a process that would take months, and there is no rush to get to it, as I want you to be safe through out the all journey. Integrating Exercise into Myotherapy Treatment At Melbourne Massage and Treatment, I […]
Tag Archives: fitzroy
Whiplash is a common neck injury caused by a sudden and forceful back-and-forth motion of the head. We often see this in patients who go through a car accident, contact sports injuries (AFL, rugby or even Soccer), or falls. While whiplash is usually not life-threatening, we now know that it can cause persistent pain and discomfort, affecting daily activities. Therefore, it is important to understand its symptoms, causes, and the best exercises for recovery, which can help individuals manage and overcome this condition effectively. Common Causes of Whiplash Whiplash is a term used to describe a fast rocking motion of the cervical area and is most frequently caused by: Car accidents: Rear-end collisions are the leading cause, as the sudden force propels the head forward and backward. Sports injuries: Contact sports like football, boxing, or hockey but even AFL, Rugby or even Soccer increase the risk of whiplash injuries. Falls: Slipping and falling can cause the head to jerk suddenly, leading to whiplash. Physical assaults: Blows to the head or sudden jolts, such as those experienced in shaken baby syndrome, can result in whiplash. What are the consequences of Whiplash for the cervical ligaments? The consequences of whiplash for the cervical ligaments can be significant, leading to long-term instability and chronic pain. When the ligaments are overstretched or torn, they lose their ability to support the cervical spine, resulting in properly: Reduced Stability: Weakened ligaments can no longer provide adequate support to the cervical vertebrae, leading to excessive movement and an increased risk of further injury. That’s why stretching is not recommended either. Chronic Pain and Stiffness: Persistent discomfort may arise as the muscles attempt to compensate for the lack of ligament support. Increased Risk of Degeneration: Ligament damage can accelerate wear and tear on the cervical joints, potentially leading to conditions such as osteoarthritis. Neurological Symptoms: Instability in the cervical spine may irritate or compress nerves, leading to headaches, dizziness, or numbness in the arms. Symptoms of Whiplash Whiplash symptoms can range from mild discomfort to severe pain, and they often appear within hours or days of the injury. Common symptoms include: Neck pain and stiffness: One of the most prevalent symptoms, often worsening with movement. Headaches: Typically originating from the base of the skull and radiating toward the forehead. Shoulder and upper back pain: The impact can cause muscle strain in surrounding areas. Reduced range of motion: Difficulty moving the neck due to stiffness and discomfort. Dizziness and fatigue: A common reaction as the body copes with the injury. Tingling or numbness in the arms: Nerve involvement may lead to sensations of pins and needles. Cognitive issues: Some people experience memory problems, difficulty concentrating, and irritability. Those symptoms may not present all at once, and they can belong to other presentations, while whiplash did or didn’t happen anytime before. That’s why when we go through a clinical history taking, as Myotherapist, we take our time to dig into your past and your body habits, as this can give us important information about your current presentation and what we can do to improve it. Why Can Whiplash Become a Lifelong Issue? In some cases, whiplash can become a chronic condition due to the instability of cervical ligaments. Cervical vertebrae can be divided into two parts, Mobile and Stable joints. C1 to C2 are the mobile ones, whereas C3 to C7 are the stable ones. Now, if along a whiplash incident, the ligaments of either the mobile or, most luckily, the stable side get strained, the muscles surrounding that segment of the joint would have to work harder to maintain stability. This would lead to to ongoing discomfort, reduced mobility due to pain and muscle spasms, and increased vulnerability to future injuries. If left untreated or managed improperly, this is how the condition can become chronic and lead to other injuries along the way. Importance of Thoracic Mobility Thoracic mobility plays a crucial role in preventing the chain effect of mobility and stability issues between the thoracic spine, lower cervical, and upper cervical regions. If the thoracic spine is stiff or restricted, the lower and upper cervical spine must compensate, leading to increased strain and pain. Improving thoracic mobility through targeted exercises can help reduce this compensatory stress, allowing for better neck function and reducing the risk of chronic discomfort. In a case of a previous history of whiplash, maintaining good thoracic mobility would allow the cervical area to focus on its duties, so stability for the lower portion and mobility for the upper. Reducing the risk of overcompensation and muscle fatigue. Effective Exercises for Whiplash Recovery A structured exercise program is essential for whiplash recovery. This program should begin with isometric exercises to restore basic cervical movement, progress to concentric exercises to rebuild strength, and eventually include thoracic mobility drills to enhance overall spinal function. Phase 1: Isometric Exercises for Early Recovery. For the first 2 weeks post-injury, 5 to 7 days a week. Isometric exercises help activate muscles without excessive movement, providing a stable foundation for recovery. This step is essential to start driving more blood to the area irritated by the whiplash and also allow the central nervous system to feel confident in perceiving the cervical structure moving without pain. Isometric Neck Holds: Place your hand on your forehead and gently press against it without moving your head. Push only 25% of your strength, as it has to be a pain-free exercise. Hold for 5-10 seconds and repeat 5 times. These exercises can be done in any cervical movement, such as extension, lateral flexion, or rotation, by using your hand as a resistance and pushing always at 25% of your strength. The strenght of push does not ever progress, what you will progress within isometric exercises are the time fram of push, repetitions and sets. Phase 2: Concentric Strengthening Exercises. From week 3 post-injury onwards,3 to 5 times a week. Once the pain subsides, which we would expect to happen in 2 weeks about it, gradual […]
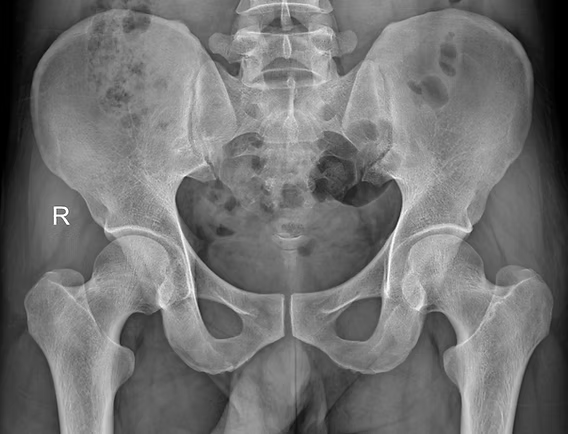
Greater Trochanteric Pain Syndrome (GTPS) is a common condition that causes persistent lateral hip pain, often making everyday activities like walking, climbing stairs, or even lying on your side difficult. GTPS primarily affects middle-aged individuals, particularly women, and is commonly linked to issues such as gluteal tendinopathy and weakness in the hip stabilizing muscles. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. GTPS Symptoms Greater Trochanteric Pain Syndrome can present with a series of symptoms that are local to the side of the hip. Here are the most common: Lateral hip pain: Persistent pain on the outer side of the hip, which may extend down the thigh. Pain when lying on the affected side: Discomfort that worsens when lying directly on the hip. Tenderness to touch: Sensitivity around the greater trochanter, which may be painful to press. Pain with movement: Aggravation of pain during walking, climbing stairs, or standing for prolonged periods. Weakness in hip muscles: Reduced strength in the gluteal muscles, leading to instability in movement. Difficulty sitting for long periods: Sitting on hard surfaces can exacerbate discomfort. Mechanism of Injury for GTPS GTPS is primarily associated with tendinopathy of the gluteus medius and/or minimus muscles, with or without accompanying bursitis. As per many tendon injuries, this condition often arises from repetitive stress or overuse, leading to microtrauma and degeneration of these tendons. On the other hand, abnormal hip biomechanics can exacerbate the issue, as compressive forces cause impingement of the gluteal tendons and bursa onto the greater trochanter by the iliotibial band during hip adduction. Contributing factors to GTPS include acute trauma, such as a fall onto the lateral hip, prolonged pressure from lying on one side, and overuse from activities like running or stair climbing. Additionally, conditions like iliotibial band disorders and gluteal muscle weakness can increase the risk of developing GTPS. Understanding these mechanisms is crucial for effective management and prevention of GTPS. Evaluation of GTPS Diagnosing GTPS typically involves a combination of clinical examination and medical history assessment. After taking your clinical history, including sports and work activity, I will perform a series of tests to validate the suspicions of GTPS. Those tests include single-leg stance and resisted hip abduction, which we would expect to show weakness in single-leg standing and pain during the abduction movement. Lastly, we would also palpate the area, which is a test that is kept for last because we want to avoid flair the presentation, which may be painful with any other test after that. In some cases, imaging techniques like ultrasound or MRI may be used to rule out other conditions and confirm gluteal tendinopathy or soft tissue abnormalities. I personally do not recommend image testing as the first way to go because the impact of seeing physical damage can also have a negative impact on self-perception, making a recovery harder. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. The difference between GTPS and Femoroacetabular Impingement (FAI) The difference between GTPS and FAI stands in the hip area involved in the injury. The GTPS is relative to the side of the hip and involves the gluteus medius and minimus tendon and the bursa that separate that tendon from the greater trochanter of the femur. On the other hand, FAI is a presentation that still involves the hip, but it does take place on the anterior portion of the hip, as is characterised by and overgrowth of tissue on the femur head or the hip socket, and it does manifest with hip flexion and external rotation. That’s why it is important to receive an evaluation of the presentation from a professional, in order not to mix the two presentation, or also, in order to evaluate if both presentation are present at the same time, which can also happen. The Role of Exercise in GTPS Treatment A recent systematic review and meta-analysis analyzing multiple randomized controlled trials found that structured exercise provides significant benefits for individuals with GTPS. The findings revealed that: Long-term pain reduction: Exercise can lead to slight but meaningful reductions in hip pain over time. Improved physical function: Patients who engage in targeted exercise programs experience better mobility and overall hip function. Increased likelihood of meaningful recovery: Compared to corticosteroid injections, exercise significantly increases the chances of noticeable improvement in symptoms. One of the most notable takeaways from this research is that exercise has a long-lasting effect, whereas treatments such as corticosteroid injections may provide only short-term relief. Additionally, no serious adverse effects were reported with exercise-based interventions, making it a safe and sustainable approach to managing GTPS. Why Choose Exercise Over Corticosteroid Injections? Corticosteroid injections have often been used for GTPS pain relief, but the research indicates that exercise leads to better long-term outcomes. While injections may offer temporary symptom relief, they do not address the underlying causes of GTPS, such as gluteal muscle weakness or tendon dysfunction. Exercise, on the other hand, strengthens the hip muscles, improves joint stability, and reduces the likelihood of recurring pain. In a previous blog post, I spoke about the key role of Gluteus Medius as a pelvis stabiliser. Effective Exercises for GTPS At Melbourne Massage and Treatment in Fitzroy North clinic, I design individualized exercise programs to help patients with GTPS regain strength and function. Some of the most effective exercises for GTPS include: Isometric exercises: Holding static positions to engage the hip muscles without excessive movement, reducing pain and improving muscle endurance. Strength training: Progressive strengthening of the gluteus medius and minimus muscles to enhance hip stability. Functional movement training: Exercises that mimic daily activities to help improve movement patterns and prevent pain triggers. These exercises can be performed both at home and under professional supervision to ensure […]
When it comes to maintaining a healthy, functional body, it’s easy to overlook the pivotal role of certain muscles in everyday movement and long-term stability. One such muscle is the gluteus medius. At Melbourne Massage and Treatment, located in Fitzroy North, I see many patients who either love running or love to hit the gym but are not aware of the importance of this muscle for their activity. What is the Gluteus Medius? The gluteus medius (GM) is one of the three primary muscles of the gluteal group, located in the upper part of the buttock. Here is a breakdown of its anatomy: Origin: the gluteal surface of the ilium Insertion: lateral surface of the greater trochanter Innervation: dorsal branches of the L4, L5, and S1 Actions: Abduction and medial rotation of the lower limb. It stabilises the pelvis. Thanks to its positioning, the GM plays a vital role in controlling pelvic movement, specifically in the stabilization of the pelvis during various motions like walking, running, or standing on one leg. More Information About Gluteus Medius actions The GM serves several essential functions that directly affect the stability of the hip and lower body: Pelvic Stabilization: One of its primary roles is preventing the pelvis from tilting excessively to one side when you move, especially when you’re walking or running. If the gluteus medius isn’t working properly, the opposite side of your pelvis may dip downward, leading to an imbalance and compensatory movements that strain other parts of the body. Hip Abduction: The gluteus medius helps to move the leg out to the side, away from the body. This movement, known as hip abduction, is crucial for activities that require lateral movement, such as stepping sideways or maintaining balance while performing physical tasks. Internal and External Rotation: The gluteus medius also assists with the rotation of the hip joint. Depending on which fibers are activated, it helps with both internal and external rotation of the thigh. This is essential for maintaining control and precision in movements. Postural Support: The gluteus medius muscle helps keep the pelvis level when you’re standing on one leg. Without proper activation of this muscle, one hip might drop, affecting posture and causing misalignments in the spine and lower back. The Role of the Gluteus Medius in Hip Stability Why is the GM so important for hip stability? Simply put, this muscle acts as the stabilizer of the pelvis. Without a properly functioning gluteus medius, other muscles and joints are forced to compensate for the lack of stability, leading to overuse and strain. For example, improper GM function can result in excessive stress on the knees, lower back, and even the ankles, which can lead to pain, discomfort, and injury. Clinical implications are vast, especially for athletes and individuals who regularly engage in physical activities. Hip instability can result in difficulty performing simple tasks like walking or climbing stairs, and over time, it may contribute to chronic conditions such as hip osteoarthritis. A common painful presentation that we see in athletes but also the everyday patients is Greater Throcanta Pain Syndrome (GTPS), which is characterised by the side hip pain. This presentation results from a GM tendon irritation. Signs of Weak or Dysfunctional Gluteus Medius Here are some common signs that your gluteus medius may need attention: Pain in the hip or lower back: Since this muscle is integral to proper alignment, dysfunction often manifests as discomfort in the hips or lower back. Difficulty balancing on one leg: Struggling with stability when standing on one leg may indicate weak gluteus medius muscles. Shifting or limping while walking: A noticeable shift or limp while walking can point to weakness in the gluteus medius, causing the body to compensate and disrupt your gait. How can Gluteus Medius impact your run? The gluteus medius is crucial for runners as it stabilizes the pelvis, controls hip movement, and ensures proper alignment during running. This muscle prevents excessive pelvic tilting, reduces side-to-side sway, and helps maintain efficient running form, thereby lowering the risk of injuries such as knee pain, IT band syndrome, and lower back discomfort. A weak or dysfunctional gluteus medius can lead to compensatory movements, affecting performance and causing imbalances. How Melbourne Massage and Treatment Can Help At Melbourne Massage and Treatment, as a clinical myotherapist, I focus on treatment designed to address muscle pain and dysfunction through a variety of techniques. One of the key areas of focus is to create a treatment plan that works for your presentation based on your clinical history. Here is a breakdown: 1. Assessment and Diagnosis: I would conducts a thorough assessment to identify if the gluteus medius is underperforming, weak, or compensating due to other musculoskeletal issues. This involves a combination of posture analysis, movement patterns, and targeted strength tests. 2. Myotherapy Treatment Techniques: I will use various techniques, including trigger point therapy, Dry Needling, myofascial release, and deep tissue massage, to release tension in the gluteus medius and surrounding muscles. This helps to restore proper function, reduce pain, and improve mobility. 3. Rehabilitation and Strengthening: After addressing any issues, we will work to develop rehabilitation strategies, including targeted strengthening exercises for the gluteus medius and other muscles that surround the pelvic, lower back and leg area. These exercises aim to restore proper muscle activation and prevent future imbalances. 4. Injury Prevention: In order to prevent further injury, we will set a target of strength that you want to achieve with your sports activity, and we will do our best to hit that target. Be mindful that based on your presentation, the target could extend from a few weeks to several months. The Takeaway The gluteus medius muscle is far more important for hip stability than many people realize. Its role in maintaining pelvic alignment and controlling movement is essential for pain-free mobility, proper posture, and long-term musculoskeletal health. Whether you’re dealing with hip pain, experiencing difficulty with balance, or want to prevent future issues, understanding and caring for […]
A deadlift (conventional deadlift) is a popular exercise that aims to strengthen your posterior chain muscle, including the erector spinae muscle, glutes, and hamstring. It is considered a really top list of important exercises to do, and it can be fun and rewarding, but when the weight you move starts increasing, it can lead to severe injuries if you are not using the right technique. Let’s then look into what we need to do to get a good deadlift by starting to analyse from bottom to top how the body should be placed. Centre of mass and biomechanics in deadlift To start with, let’s talk about the biomechanics and the centre of mass for a deadlift. When doing exercises, biomechanics plays a crucial role in safety and optimal exercise execution, and there is no exception for the deadlift. Furthermore, along with all exercises, the lifting and the descending part, the weight has to be in line with the centre of mass. These two components are strictly interconnected to the other one, which means if I don’t use the right biomechanics, I am not going to have the weight aligned with the centre of mass, or if the weight is not aligned with the centre of mass, I am not using my biomechanics at its full potential. So, what’s the centre of mass in the deadlift? The centre of mass in a deadlift is that imaginary line that runs right from the mid-portion of your feet up right in front of your shins, and as you lift the weight up, it passes right in front of your pelvis. That’s where the bar is going to end once you complete the lifting motion. What happens if I don’t keep the bar along the centre of mass? At any stage, during the lifting or the descending motion, if you move the bar further away from the centre of the mass line, there is a great danger of injury. This is because, as the weight travels away from the centre of mass, there is an increase in momentum, which means that your muscles and ligaments that are working hard to move the weight are suddenly placed under a greater load. What are then the proper biomechanics to observe along a deadlift? Ankle and Knee To execute a good deadlift, we want to ensure we have good ankle dorsiflexion, which is not as important as when we squat, but still, we better ensure it is working right. This would allow a straight forward movement of the knee, which would not need to find its way medially or laterally along the initial bending for when we go to grab the bar. Moving up the chain, as we said, the knee have to point straight ahead, following the toes direction. Hip and lower back Next is the hip. This is an important joint, and here is where we need to make sure that we tilt the pelvis forward (bring the teil bone upwards) and as we hinge the hip, we have to have enough movement in there that the greater trochanter (bone landmark that represents the side of the femur’s head) is posterior to the malleolus (the bone landmark that make the side and medial portion of the ankle). Now, if we managed to have tailbone project far back and up, and hip hinged with a slightly bent knee, our back up to cervical area would be alrady quiet flat. Thoracic and head If we keep going upwards, we get to the upper thoracic area, right between the scapula. Here, we want to keep the scapula protracted and have the rhomboids and serratus anterior muscles active and strong so that the arms can hang down straight towards the bar and sit right next to the knee. Regarding the head, use your eyesight to look down at the floor at 45° in front of you and feel the ears pulling away from the shoulder. That would keep your neck nice and long and place the head in the right position. Arms and hands Arms hang down from the shoulder in a straight line, from the AC Joint down to the wrist. The arm has to feel heavy and prolonged, and the hands must sit right next to the shin. Indeed, your arms must stay as wide as your shoulders. That would ensure that your arms are at 90° with the bar, and from a vertical pool point of view, they can take the maximum load ever. Lastly, regarding the hands, there are different grip types that can be used for the deadlift. What is most important is that the wrist is straight following the armline. For exercise purposes, you can have a regular grip where your thumb is gripping around the bar. For heavier weights, you may want to do a mixed grip, where one hand (the dominant one) has the palm facing forward, and the other hand has the palm facing you. In conclusion, the biomechanics of the deadlift, if used correctly, will allow you to always weight in a safe spot, in line with the centre of mass. Your back has to be flat at all times, and along the exercise execution, you want to grasp air in, engage the core to flat out the lower back and then you can lift off. Benefits of Deadlifting Now, let’s look into the benefits of deadlifting. Full-body workout: Deadlifts engage multiple muscle groups—glutes, hamstrings, quads, lower back, core, traps, and forearms—providing a full-body workout in a single movement. Improved strength: Deadlifts are among the best exercises for building overall strength, especially in the posterior chain (back, glutes, and hamstrings). Better posture: Deadlifts can improve posture and reduce the risk of slouching by strengthening your back and core muscles. Core stability: The movement requires significant core activation, helping to enhance core strength and stability. Increased athletic performance: Deadlifts translate well to other athletic movements, as they improve explosiveness, agility, and endurance. Fat loss: The intensity and demand on […]
If you or someone you know is struggling with the lingering symptoms of Long Covid symptoms, you are not alone. After the initial acute phase of COVID-19, many people continue to experience debilitating symptoms such as fatigue, breathlessness, and brain fog that can last for weeks or even months. These prolonged effects, commonly referred to as Long Covid, have created a pressing need for effective treatment strategies to manage and alleviate the symptoms. One promising approach gaining attention is Manual Lymphatic Drainage (MLD) Massage, a gentle and non-invasive therapy that can support the recovery process for Long Covid patients. At Melbourne Massage and Treatment, Giovanni, a highly trained therapist from the Vodder Academy, is helping clients recover from the lingering effects of Covid-19 using this technique. But how exactly does MLD work, and can it help you overcome the frustrating symptoms of Long Covid? What is Manual Lymphatic Drainage Massage (MLD)? MLD is a specialized massage technique that uses gentle, rhythmic movements to stimulate the lymphatic system—the body’s waste removal and immune system. The lymphatic system is responsible for draining toxins, bacteria, and waste from the body’s tissues. It plays an essential role in inflammation control, immunity, and tissue recovery. MLD can help to enhance the flow of lymph, reduce chronic-inflammation, alleviate congestion, and promote overall healing. Trained at the renowned Vodder Academy, Giovanni uses the Dr. Vodder method of MLD, a highly effective and evidence-based technique. This form of lymphatic drainage focuses on increasing lymph flow and addressing issues such as fluid retention, swelling, and inflammation, which are common in patients suffering from post-viral syndromes, including Long Covid. Long Covid Symptoms: A Multifaceted Condition Long Covid is a condition where individuals experience lingering symptoms after the acute infection phase has passed. Some of the most common symptoms include: Fatigue: Extreme tiredness that doesn’t improve with rest Breathlessness: Difficulty breathing or catching your breath even after mild exertion Cognitive Dysfunction: Often referred to as “brain fog”, which includes issues with concentration, memory, and clarity of thought Muscle and Joint Pain: Persistent aches and pains that can make everyday tasks difficult Sleep Disturbances: Trouble falling or staying asleep due to physical discomfort or anxiety While medical management of Long Covid usually focuses on symptom control, the current lack of effective pharmaceutical treatments leaves many patients seeking alternative therapies. That’s where Manual Lymphatic Drainage can make a significant difference. How MLD Helps with Long Covid Symptoms A recent study, Manual Lymph Drainage for Post-COVID-19 Related Cough, Breathlessness, and Fatigue, explored the use of MLD as a treatment for individuals suffering from persistent Long Covid symptoms. This study found that MLD helped reduce symptoms like fatigue, breathlessness, and chronic cough, with improvements starting as early as the third treatment. Patients reported increased energy levels, better sleep, and enhanced functional capacity after just a few sessions. Giovanni’s expertise with MLD can be crucial in addressing the inflammation, poor lymphatic drainage, and respiratory issues often associated with Long Covid. Key Benefits of MLD for Long Covid Symptoms Recovery: Reduces Inflammation One of the key factors contributing to Long Covid symptoms is chronic inflammation. MLD helps to reduce systemic inflammation by promoting the drainage of inflammatory waste and toxins, which can alleviate discomfort and promote healing. Improves Breathing Function Many Long Covid sufferers experience breathlessness, a symptom that can greatly affect quality of life. MLD targets the lymphatic pathways in the chest and lungs, which can help reduce inflammation in the respiratory system, clear mucus, and improve lung function. The technique also includes special “bronchitis” maneuvers that help open up the lungs and reduce coughing. Boosts Energy Levels Fatigue is one of the most disabling Long Covid symptoms. By supporting lymphatic flow and reducing congestion, MLD can improve circulation and oxygen delivery to the body’s tissues, helping to restore energy levels and combat the persistent tiredness that plagues many Long Covid sufferers. Supports Immune System Recovery Long Covid symptoms often result from an immune response gone awry. MLD can help recalibrate immune function, promote lymphatic circulation, and enhance the body’s natural ability to heal itself. Enhances Mental Clarity Brain fog and cognitive dysfunction are common complaints among people with Long Covid. By reducing inflammation and promoting better circulation, MLD may help improve mental clarity and cognitive function, allowing patients to regain focus and reduce feelings of confusion or mental fatigue. Improves Sleep Quality Many Long Covid sufferers report difficulties with sleep. By reducing pain and inflammation, MLD helps induce a relaxation response in the body, which can promote deeper, more restful sleep. Giovanni’s Approach: Tailored MLD Treatment for Long Covid Symptoms Giovanni, a skilled therapist with extensive training in the Vodder Academy’s MLD method, offers personalized treatments for those struggling with Long Covid. Each session is tailored to the individual’s specific symptoms, addressing areas such as: Chest and Lungs: To reduce inflammation and congestion Neck and Shoulders: To alleviate stiffness and promote relaxation Facial Area: For sinus congestion or post-viral inflammation Whole Body: To improve general circulation, reduce swelling, and stimulate the lymphatic system. When working with this type of presentation, it is also valid to consider a shorter initial session to ensure that MLD would not spike up your symptoms. If you are not sure what works best for you, just ask to Giovanni. Giovanni’s gentle, compassionate approach helps create a safe space for clients to heal. Many clients report feeling noticeably better after just a few sessions, with improvements in breathing, energy, and mental clarity. Read here about the Melbourne Massage and Treatment testimonials. Real-World Results: Case Studies In a study of two Long Covid patients undergoing MLD treatment, both reported substantial improvements in their symptoms. After just a few sessions, they experienced reductions in breathlessness, fatigue, and overall discomfort. By the time of their follow-up treatment, both patients reported feeling the best they had since before contracting COVID-19, with increased energy, improved sleep, and less reliance on medication. Why Choose MLD for Long Covid Recovery? Non-invasive and Drug-free: MLD offers a natural, […]
A meniscus is a cushion type of structure that sits between the femur head and the tibia, on the medial side of the knee and the femur and the fibula on the lateral side of the knee. Its role is to protect any friction between the femur head and the other bonds. In sports activities where there is a lot of stop-and-go or stop-and-twist type of motion, such as basketball or netball, the meniscus is put under intense stress, and the chance of injuries can increase. Meniscus tear classification? A meniscus tear is a type of injury that can be classified based on its severity and size. There are different types of classifications, but the most used and accepted is Laprade’s classification (LaPrade et al., 2014). Laprade classification of Meniscus root tears (MRTs) is based on the morphology during arthroscopic assessment. The classification includes five distinct lesions: Type 1 tears represent partial root tears that are stable (7% of all meniscus root tears). Type 2 tears represent complete radial tears within 9 mm of the root attachment centre (67.6%). This type of tear is then subdivided in three other sub-group based on the distance of the tear from the center of the root attachment (2A 0–3 mm, 2B 3–6 mm and 2C 6–9 mm). Type 3 tear was defined as bucket-handle tear with complete root detachment (5.6%). Type 4 tears are complex oblique tears with complete root detachment (10%) and bony avulsion of the root attachment (9.9%). Meniscus tear symptoms In order to diagnose a meniscus tear, the gold standard method is an MRI scan. That said, nowadays, the only time you would get an MRI scan to your knee for a meniscus injury, is for surgery purposes, as we now know, that live with a meniscus tear is possible, as long as the muscle that across the knee joint are well looked after. That said, in the early stage, the symptoms of meniscus tear can include: Joint swelling Tenderness in the knee on the medial or lateral portion of the knee A feeling of catch in the knee as is moving Limited range of motion A feeling of the knee not able to hold the weight. Localised pain To alleviate the discomfort, the aid of a crutch, especially in the early stage, is recommended, and as per all acute phase injuries, the first few days, rest and movement with pain-free range of motion are extremely important. In addition to this, heat can be applied for intervals of 15 minutes once or twice a day. How do we rehabilitate a meniscus tear? As with all injuries, there is not one rehabilitation process that works for everyone, but there are guidelines that can be used to lead a recovery process. Let’s start with the acute phase (first phase), which is the first 72 hours. In this time frame, we would avoid putting direct weight on the affected side and, where possible, do simple knee flex/ext pain-free movements. Placing a pillow under the knee could help avoid locking the knee, which may not feel comfortable. Second phase: In this phase, which would be somewhere after the initial 72 hours, if it feels comfortable, we can start placing some gentle weight on the knee, even though using a crutch can still be acceptable, especially in the early stage of this phase. The second phase can last up to 5 or 6 weeks. An active range of motion, where the knee flexion is always greater, and the knee extension is getting closer to full extension, would keep increasing daily. In this phase, we can introduce Isometric exercises for knee flexion and extension. Those types of exercises can be done with a bench curl machine or an elastic band or ankle weight. What is most important is to start with lightweight or resistance, hold the weight for 40 seconds, and release for 40 seconds. The time frame can be adapted to the patient’s comfort. Halfway through this phase, we can start to introduce eccentric and concentric loads with weights and potential assisted sit and stands type of movement, with a chair that is higher than average and something in front of the patient where they can hold on to (like the back of another chair). As the patients’ confidence and muscles start responding more and more to these exercises, we can move to the third phase, and here we are in week 7 or 8. The chair for sitting and standing is now at average height; we may not need anterior assistance anymore. It is now essential to ensure the patient is walking and confident about placing weight on the affected side. Single-leg squats can be initiated, maybe even with the aid of a stick initially, and day by day without. The load on the anterior and posterior chain muscles of the thigh is increased, and as we move forward from week 10 to week 12, plyometric exercises can be introduced. Along those exercises, we look into explosive lunge, squatting, skipping the rope and running. A great test would be the hopping test, which consists of single-leg hopping, side to side. One minute of oping should not reproduce any pain. All these progressions are approximations of a natural healing process, and based on the individual presentation, this protocol can be modified and enriched as needed. Meniscus tear and surgery. In their meta-analysis of 6 randomised control trials, Meng et al., 2024, concluded that data favour exercise therapy over surgery as a first intervention for meniscus tears. These conclusions come from the fact that the pain reduction, estimated with the knee Knee Injury and Osteoarthritis Outcome Score (KOOS), does not show any difference between the arthroscopic partial meniscectomy (APM) and exercise therapy. That said, it doesn’t mean that surgery is never an option. What Meng et al., 2024 prove is that before heading for an invasive procedure, it is worth it to look into exercise therapy on its own. If the conservative method does […]
Fallen arches, or Flat Feet, are often misunderstood and can be a source of concern for many. However, as a Clinical Myotherapist, I want to reassure you that flat feet are not inherently problematic. In fact, they can be pretty standard and, in many cases, don’t require any treatment at all. Let’s learn why. Understanding Flat Feet (FF) When the feet’ arch presents as flat, what is occurring is a flat foot, resulting in the entire sole of the foot making contact with the ground. What you may not have noticed yet is that this presentation can be triggered by being on your feet, as in standing on it, and not by lying down or in a seated position with the feet off the ground. This is what we would call structural FF. What are Structural Flat Feet? Structural FF also known as rigid FF , involve an anatomical abnormality where the arch does not form properly. This “malformation” could be caused by genetic factors or developmental issues. What the arch would look like is lower than usual or absent entirely, which is often a lifelong condition. Now, despite their appearance, structurally flat feet are less likely to lead to pain or discomfort. The body, indeed, as it is a functional bio-machine, would easily adapt well to this anatomical variation, and many people with structural flat feet can lead active and healthy lives without any special interventions. Different is the anatomical presentation for functional flat feet, and let’s see why. Functional Flat Feet Functional FF on the other hand, result from how the foot functions rather than an inherent structural issue. In this case, the foot arch may appear flat when standing or walking due to excessive strain or an imbalance in the muscles and tendons that support the arch. When the foot is not bearing weight, the arch may appear normal. Potentially, you could also have one flat foot and one that isn’t when having a functional presentation. This is a common one for those who suffer from structural scoliosis. The main reasons why you may present with functional FF is due to muscle Imbalance, within the foot and ankle. This might be due to overuse, poor posture, or repetitive stress. Other reasons include conditions such as overpronation or excessive weight. Addressing these underlying issues can often alleviate the problem. What can be done for Functional Flat Feet? Changing in foot wear, could be an option. Based on the activity that you are doing on a daily basis life, certain types of footwear may help more than others. Orthotics, which are custom or over-the-counter arch supports, can provide temporary relief and improve function, but these often are over-estimated tools that get prescribed at random. Exercises: Strengthening exercises for the feet and lower legs can help improve muscle balance and support the arch, reduce the pain and improve motor function. In some cases, as explained in this study by Sanchez-Rodriguez et al. (2020), exercises can change the shape of the feet for the better if the intervention is done at an early age; in others, it can help maintain the feet pain-free. When Should You Worry? Most people with flat feet experience no symptoms, and if that’s the case, you do not need to worry about changing the presentation, as it could lead to pain and discomfort. If you are experiencing pain, on the other hand, is worth it to consult an health care practitioner, that can be a podiatrist, or book an appointment at Melbourne Massage and Treatment, where we are going to evaluate if the pain is due to the flat feet it self, or to other conditions such as plantar fasciitis, shin splints, or other pathologies. The Bigger Picture It’s essential to remember that FF are just one of many variations of normal foot anatomy. They do not necessarily indicate a health problem or affect your overall well-being. For most individuals, flat feet are simply a characteristic of their body and do not require any special treatment. In conclusion, whether you have structural or functional flat feet, it’s essential to focus on how you feel and function rather than the appearance of your feet. In many cases, flat feet are perfectly normal and do not pose any significant health risks.
At Melbourne Massage and Treatment, we specialise in providing tailored remedial massage therapies designed to alleviate chronic pain. These therapies are meticulously designed to target the root causes of pain, fostering relief and recovery through specialised techniques. Our expert therapists are committed to assisting individuals in reclaiming their comfort and mobility, paving the way for a healthier, more active lifestyle. Key Takeaways: Tailored Approach: Each treatment is customised to address specific pain areas, enhancing effectiveness. Professional Expertise: Our therapists are highly trained in a variety of techniques to offer optimal relief. Holistic Benefits: Beyond pain relief, enjoy improved mobility and reduced stress. The Power of Remedial Massage Remedial massage is not just about relaxation; it’s a potent therapeutic tool for chronic pain management. By manipulating the soft tissues of the body, remedial massage helps in breaking down knots and improving blood circulation. This process not only alleviates pain but also enhances the healing process of the muscles and tissues. For individuals with conditions like arthritis, fibromyalgia, and back pain, a regular remedial massage can be a cornerstone of effective management. How Remedial Massage Works Pain Relief: Through techniques such as kneading and pressure, remedial massage relieves muscular tension and pain. Improves Circulation: Enhanced blood flow aids in faster recovery of sore, overworked muscles. Increases Mobility: Regular sessions help in restoring flexibility and range of motion. Addressing Chronic Pain Conditions with Remedial Massage Remedial massage not only provides immediate relief but also long-term benefits to those suffering from chronic pain conditions. By focusing on specific areas of tension and imbalance within the muscular system, remedial therapy can significantly alleviate the symptoms associated with chronic musculoskeletal conditions. For individuals dealing with repetitive strain injuries or postural problems, remedial massage provides essential relief that is both healing and preventive. By increasing tissue elasticity and fluidity, the therapy ensures less tension in the muscles, which is often the root cause of ongoing pain and stiffness. Individualised Treatment Plans Our approach at Melbourne Massage and Treatment is deeply rooted in understanding the unique conditions and needs of each client. During the initial consultation, our therapists perform a thorough assessment to determine the most effective treatment strategy. This personalised plan is aimed at not only addressing the pain but also at promoting recovery and preventing future issues. Each session is adapted to progress with the client’s recovery, ensuring the most beneficial outcome. Techniques and Therapies Remedial massage incorporates a variety of techniques, each chosen for its ability to target different issues: Deep Tissue Massage: Focuses on deeper layers of muscles and connective tissue, helpful in releasing chronic muscle tension. Myofascial Release: Targets the fascia, the connective tissue around muscles, alleviating tension and restoring mobility. Trigger Point Therapy: Aims at specific areas of tight muscles that cause pain in other parts of the body, often described as ‘knots’. Benefits Beyond Pain Relief The benefits of remedial massage extend beyond the direct treatment of pain. Regular sessions contribute to: Enhanced Recovery: Speeding up the recovery process from injuries and surgeries. Improved Posture: Regular massage helps in correcting posture and muscle imbalances. Stress Reduction: The relaxation aspect of massage helps reduce stress levels, which is often a contributor to chronic pain. Real Client Success Stories At Melbourne Massage and Treatment, we’ve seen remarkable transformations in our clients’ health. For instance, a client with chronic back pain, who had tried various treatments without significant improvement, found relief after a series of targeted remedial massage sessions. This individual story is just one of many that exemplify the healing potential of dedicated remedial massage treatment. Integrating Remedial Massage into Your Health Regimen Incorporating remedial massage into your regular health care routine can profoundly affect your overall well-being. It’s recommended for anyone suffering from chronic pain to consider setting up a routine with our skilled therapists. This not only helps in managing pain but also enhances general health and prevents the recurrence of injuries. Expert Care at Melbourne Massage and Treatment Our team of therapists at Melbourne Massage and Treatment is not only skilled in a variety of massage techniques but also in assessing the needs of our clients. They continually update their skills and knowledge to include the latest in remedial massage research and techniques. This commitment ensures that our clients receive the highest standard of care currently available in the field of massage therapy. Understanding Chronic Pain Management Chronic pain is a complex condition that affects every aspect of an individual’s life. At Melbourne Massage and Treatment, we believe in a multidisciplinary approach to pain management. Remedial massage is a cornerstone of this approach, but it is most effective when combined with other treatments and lifestyle adjustments. Our therapists often work in conjunction with physiotherapists, chiropractors, and doctors to provide a comprehensive treatment plan that addresses all aspects of the client’s health. Lifestyle and Remedial Massage Incorporating lifestyle changes alongside regular remedial massage sessions can dramatically improve outcomes for individuals with chronic pain. Simple adjustments like improving ergonomic setups at work, maintaining a balanced diet, and regular physical activity can complement the effects of massage therapy. Our therapists provide guidance on these aspects, offering a holistic approach to managing chronic pain. Education as a Tool for Empowerment Knowledge is power when it comes to managing chronic pain. Our therapists ensure that clients are educated about their conditions and the mechanics of pain, which empowers them to make informed decisions about their health. This education includes understanding how various massage techniques work to alleviate pain and how they can actively participate in their recovery process. The Role of Regular Assessment Regular assessments are crucial to the success of any treatment plan. By consistently evaluating a client’s progress, therapists can adjust treatments as needed, ensuring that each session is as effective as possible. These assessments look at pain levels, functionality, and overall mobility, adjusting the course of treatment to match the changing needs of the client. Conclusion At Melbourne Massage and Treatment, we understand the debilitating nature of chronic pain. Our remedial […]
Remedial massage offers a therapeutic approach to easing pain and hastening recovery from injuries, blending traditional techniques with tailored treatments to suit individual needs. At Melbourne Massage and Treatment, we specialise in this intricate therapy, aiming to not only alleviate pain but also to restore function and enhance overall well-being. Key Takeaways: Remedial massage provides targeted pain relief, enhancing comfort during recovery. This therapy promotes increased circulation, aiding the body’s natural healing process. Regular treatments can improve flexibility and mobility in affected areas. The therapy also supports mental well-being, helping reduce stress associated with injuries. How Remedial Massage Can Help in Recovering from Injuries Direct Impact on Injury Sites: Remedial massage techniques are adept at targeting the specific tissues affected by an injury. By applying controlled pressure to the injured area, these techniques help break down scar tissue and adhesions that can restrict movement and cause pain. As a result, the direct manipulation of these tissues stimulates healing and the restoration of healthy function. Enhancing Lymphatic Drainage: One of the lesser-known but critical benefits of remedial massage is its ability to stimulate the lymphatic system, which is pivotal in reducing swelling and inflammation often associated with injuries. Improved lymphatic drainage not only alleviates pain but also enhances immune system function, which is crucial in fighting off potential infections that can complicate the recovery process. Stimulation of Endorphin Release: The process of remedial massage helps in stimulating the body’s production of endorphins, the natural ‘feel good’ hormones. These hormones act as natural painkillers, reducing the perception of pain and promoting a sense of well-being. This psychological boost is essential, as it can significantly impact one’s motivation and enthusiasm for continuing with the rehabilitation process. Restoring Muscular Balance and Posture: Injuries often disrupt the normal muscular balance within the body, leading to compensatory movements and postures that can themselves lead to further discomfort or injury. Remedial massage helps to identify and correct these imbalances. By easing the tension in overused muscles and stimulating underactive ones, the body can return to a more natural posture and reduce the risk of recurring injuries. Preventative Measures for Future Injuries: Beyond just aiding in recovery, remedial massage serves a preventative function. Regular sessions can identify and mitigate risk factors associated with injuries, such as tightness in certain muscles or limited joint mobility. This proactive approach not only helps to prevent future injuries but also enhances overall physical performance and endurance. Integrating Remedial Massage into Recovery Plans Integrating remedial massage into an injury recovery plan should be done with consideration to the individual’s specific needs and medical history. Collaboration with healthcare professionals can ensure that massage techniques are effectively aligned with other treatment modalities, such as physical therapy or medication, for optimal recovery. Customised Treatment Approaches: Every injury is unique, and thus, every remedial massage session should be tailored to the specific needs of the individual. Experienced therapists at Melbourne Massage and Treatment assess each client’s condition and create a personalised treatment plan. Long-Term Health Benefits The benefits of remedial massage extend far beyond immediate injury recovery. Regular sessions contribute to maintaining a healthy musculoskeletal system, reducing the risk of injury by keeping muscles loose and flexible and improving joint mobility and stability. Furthermore, the relaxation benefits of massage can help manage stress, which is a common factor in many chronic health conditions. Holistic Approach to Well-being: Melbourne Massage and Treatment promotes a holistic approach to health, where remedial massage is integrated with other wellness practices. This might include guidance on nutrition, exercise, and mental health strategies to support a well-rounded recovery and maintain long-term health and well-being. Empowering Clients: Educating clients about their body and the healing process is a critical component of the service provided. By understanding the mechanics of their recovery and the role remedial massage plays, clients are better equipped to take proactive steps towards their health, further enhancing the effectiveness of their treatment. Enhancing Mental and Emotional Well-being An often overlooked aspect of remedial massage is its capacity to improve mental and emotional health. The stress of dealing with an injury can be overwhelming, leading to anxiety and depression. Remedial massage helps mitigate these issues by promoting relaxation and reducing stress levels. The soothing effect of hands-on therapy provides a therapeutic escape from the constant concern over injury and recovery, which in turn can accelerate the physical healing process. Optimal Circulatory Health Improved blood circulation is another significant benefit of remedial massage. By enhancing blood flow, more nutrients and oxygen are delivered to damaged tissues, which is crucial for repairing injuries. Additionally, better circulation helps to remove waste products and toxins from the body, which can accumulate around injury sites and slow down the healing process. This aspect of remedial massage is essential for those recovering from muscular injuries and strains, as it ensures that tissues receive the necessary components for swift recovery. Flexibility and Strength Remedial massage plays a crucial role in enhancing flexibility and strength, particularly post-injury. Techniques like stretching and kneading increase the elasticity of muscle fibers, preventing stiffness and increasing range of motion. This is particularly beneficial for individuals who are recovering from joint or muscle injuries, as it aids in gradually restoring strength without adding undue stress on the recovering tissues. Synergy with Other Therapies For comprehensive recovery, remedial massage often works best when combined with other therapeutic approaches. For instance, integrating massage with physiotherapy or chiropractic care can provide a more holistic recovery plan. Each therapy complements the other, with massage easing muscle tension and improving flexibility, while other treatments focus on alignment and functional improvement. Educating Clients on Self-Care At Melbourne Massage and Treatment, we believe in empowering our clients with knowledge about self-care techniques that complement their in-clinic massage sessions. Simple strategies, such as regular stretching, proper hydration, and stress management techniques, are shared to enhance recovery and prevent future injuries. This education is crucial, as it helps clients maintain the benefits of massage between sessions and builds a foundation for lasting health. […]
- 1
- 2