Liposuction interventions are on the rise, driven by the enormous influence of social media on how we look and by the abundance of cheap clinics worldwide. While liposuction surgery removes stubborn fat deposits, the recovery period from this type of intervention is often underestimated. As a clinical myotherapist specialised in Manual Lymphatic Drainage (MLD) Vodder style, I regularly work with clients who are navigating the post-operative process, and I often get to hear clients who haven’t been fully informed about the post-surgery care needed, and the timeframe of recovery. Indeed, many patients who have undergone Liposuction surgery are surprised to learn that MLD plays a supportive role in the recovery process, and not by “boosting” healing, but by complementing your body’s natural ability to manage swelling, fluid congestion, and fibrosis. Below, I explain what liposuction involves, why MLD is recommended before and after surgery, and what you can expect during the healing timeline. What Exactly Is Liposuction? Liposuction is a surgical procedure that aims to remove excess fat from targeted areas of the body. There are different ways in which liposuction can be delivered, but what they all have in common is the usage of a cannula to break down and suction fat from beneath the skin. Once the surgery is delivered, and the fat is removed, the body experiences trauma in the form of: Swelling Fluid accumulation Tissue inflammation Disruption to lymphatic pathways Development of fibrosis (hardened or rope-like scar tissue) Superficial blood cloth Manual Lymphatic Drainage (MLD) is a manual therapy that can make a significant difference for all those presentations. How Manual Lymphatic Drainage Supports the Healing Process MLD is a non-invasive, gentle manual technique that stimulates the movement of lymphatic fluid toward functioning lymph nodes. Compared to a regular massage (Remedial Massage, Deep Tissue, Thai Massage…), it does involve the usage of oil or creams and does not aim to reproduce any pain or inflammatory response. In fact, it is the opposite; it aims at taking away excessive inflammation, as this is one of the many roles of the lymphatic system, and the technique I used is Vodder style, which is clinically recognised for its rhythmic, directional, and methodical application. Here’s how MLD supports recovery after liposuction: Reducing Post-operative Swelling As with any surgery, even Liposuction leads to significant swelling as the body implements an inflammatory response post-trauma (the physical damage of cutting the skin open and removing body tissue). MLD helps guide the fluid that builds up due to the inflammatory response back into the lymphatic circulation, easing pressure and discomfort. Minimising the Formation of Fibrosis Fibrosis is the body’s natural response to invasive body intervention and to sudden skin dilatation; indeed, it is a common presentation in Lymphoedema too. The fibrotic tissue is a common concern after liposuction, and without proper care, tissue can become firm and lumpy, affecting the final aesthetic result.Here is how MLD supports the breakdown and prevention of fibrosis: Increasing lymph flow Softening congested areas In the fibrotic area, we apply strong pressure (still pain-free) to break fibrosis down Encouraging natural tissue remodelling That’s where more frequent treatment is most helpful. To break and manage fibrosis at its best. Preparing the Body Before Surgery The reason why MLD should be considered as a pre-operative intervention too, lies in the fact that a stimulated Lymphatic System place you in an advantageous position along the recovery process, by improving lymphatic circulation, creating better conditions for tissue recovery after surgery. When Should You Start MLD After Liposuction? Once the surgery has been delivered, the ideal time to begin MLD is as soon as you have finished your course of antibiotics, as long as: All open wounds are closed, and No infection is present. The above are essential precautions to prevent the spread of infections. Also, the early start of MLD practice would ensure the best outcome post-surgery. What To Expect from MLD Treatment Post-Liposuction While many patients find out about MLD only after they receive the surgery, and this often happens when they have their surgery overseas, in countries like Turkey, Thailand, Bali, they are still not sure till the time they meet me, what MLD treatment would be about for their post-surgery recovery. In this case, I always explain in detail what the treatment is going to be about, starting with and overview of: What is the lymphatic system How we stimulated What you should expect post-treatment, and what to do and not to do Healing time frame Other topics I had to share and reassure my patients about are: MLD is not painful There is no body fluid extraction I am not going to push liquid out of your incision Yes, you need to drink plenty of water post-treatment I found that patients who undergo liposuction, especially in Turkey, come back with tough stories about acute post-surgery care, where they get their incision reopened, and liquid milked out from there. THIS IS A DANGEROUS PRACTICE AND IS NOT MLD AND IS NOT WHAT I OFFER ANYWHERE UNDER ANY CIRCUMSTANCES. How Should You Prepare Yourself for and MLD Treatment? Here is a list of things to be aware of before you go for and MLD treatment: Food and water – You can eat a light meal a few hours before your treatment and ensure you drink only water before and after the treatment. Strictly avoid alcohol – Avoid any form of intoxication before and after treatment, as this can make you really sick and unwell Medication and Clinical History – In the initial consultation form, you must declare any medication you are taking or have taken and your clinical history, to ensure no contraindications for MLD are present. Avoid cream or lotion – Application of cream or lotion on the skin would make the skin slippery and more difficult to stretch, impairing then the stimulation of the lymphatic system Post Treatment – MLD is extremely relaxing. Ensure to have some time off after your session, in case you feel like a nap or not doing […]
Tag Archives: fitzroy
When the space between the collarbone and first rib gets tight, during movement or even at complete rest, it can lead to Thoracic Outlet Syndrome (TOS). Between the two structures mentioned above, we have the passage of the thoracic plexus (nerves) and blood vessels. The compression of those structure, can result in pain, weakness and numbness radiating down the shoulder, arm, and hand. Because TOS has multiple causes and presentations, effective treatment depends heavily on accurate assessment and an individualised approach, and that’s where myotherapy can play a crucial role. What Causes Thoracic Outlet Syndrome? As there are different tissues passing by this space, the nature of TOS can be broadly categorised into three types: Neurogenic TOS: Compression of the brachial plexus (nerves). Venous TOS: Compression of the subclavian vein. Arterial TOS: Compression of the subclavian artery. But not only can different tissues be compressed, but different structures can be responsible for the compression. Indeed, the compression can be due to the scalene muscle, pectoralis minor or bone. And here are some common causes: Muscle imbalances that lead to poor posture (forward head/rounded shoulders); Repetitive overhead activities (which lead to constant compression of the tissues); Trauma (e.g. whiplash or clavicle fracture); Anatomical variations (such as a cervical rib). The Role of Myotherapy in TOS Assessment As a myotherapist, when treating someone with suspicious TOS, we go for a series of assessments that we compare to the clinical history and symptoms. The test itself would aim to reproduce the patient’s symptoms and guide us on what potential structure is compressed. If we are suspicious of TOS, we can aim to reduce tension in soft tissue and give exercises that can reinforce those structures to alleviate any compression in the area. Orthopedic Testing & Myotome Assessment Some common assessments include: Adson’s Test (for scalene involvement) – It consists of reproducing a drop of heart bit in the wrist (affected side) by asking the patient to abduct and extend the arm while rotating (same side) and extending the neck. This would add extra compression on the suspected structures. Roos/Elevated Arm Stress Test (to reproduce vascular or neural symptoms) – It is about asking the patient to lift the arm at 90°/90° and start closing and opening their hands repetitively for 30 seconds to 1 minute. A drop of strength or symptom reproduction would lead to a positive test. Costoclavicular Maneuver (to assess space between clavicle and first rib) – It is delivered by having the patient with depressed and retracted shoulders. The positivity of this test is given by the reproduction of symptoms or a reduction in the distal wrist. Wright’s Hyperabduction Test (for pectoralis minor tightness) – The patients get asked to lift their arm (affected side) above their head while the therapist stands behind and keeps count of the wrist heartbeat. Any symptoms, reproduction, or drop in bit is considered positive. In addition to those tests, we would use: Myotome testing: which assesses the motor function of specific spinal nerve roots; Clinical history: Any history of previous injury, surgeries, work and sport loads; Type and timing of symptoms: When and how those symptoms are reproduced on daily life. All this said, we always have to consider that as therapists, myo or physio as per osteo exc… we can assume that the positivity of many of those test leads to a positive or negative conclusion regarding TOS. Hands-on treatment and exercises in combination can be the easy steps to take to treat the presentation, but can not always guarantee the best outcome, due to each individual’s unique presentation. Hands-On Treatment and Exercise Prescription Once we have more understanding of what is potentially happening in terms of compression, a myotherapy treatment focuses on addressing the underlying causes: Manual Therapy Myofascial release of the scalene, pectoralis minor, and upper trapezius muscles. Trigger point therapy to reduce local and referred pain patterns. Joint mobilisation to improve scapular movement and rib mechanics. Neural gliding techniques to encourage nerve mobility and reduce irritation. Exercise Rehabilitation Postural re-education, particularly strengthening the deep neck flexors and lower trapezius. Scapular stabilisation exercises to improve shoulder mechanics. Breathing retraining is necessary if dysfunctional patterns (like apical breathing) are contributing to compression. Neurodynamic stretches are appropriate for nerve mobility. Together, these interventions help reduce symptoms, improve function, and support long-term recovery. The time frame for improvement, if not complete reduction of the symptoms, can be different per individual, but we can estimate a period of time that goes between 12 and 16 weeks. If no changes are reproduced within this time frame, that’s where we would refer the patient elsewhere for further investigations, like a scan. When Is Surgery Needed for Thoracic Outlet Syndrome? Surgical intervention is typically reserved for cases where conservative care fails or in cases of vascular TOS, where there’s a risk of thrombosis or embolism, but also where anatomical variations, like a cervical rib is present. Surgical procedures may include: Scalenectomy (removal of the scalene muscles) First rib resection Clavicle decompression or repair if there’s previous trauma These operations aim to create more space in the thoracic outlet, thus relieving the compression. Post-Surgical Recovery and the Role of Myotherapy In case of surgery, as a myotherapist, we can still help and ensure a correct recovery post-intervention. Treatment like MLD can help in flushing excess liquid out of the surgery area, but again, we would look into exercises as a form of recovery and rehabilitation of the area affected by the surgery and or affected by the lack of strength that is a consequence of a prolonged period of muscle weakness. More broadly, myotherapy treatment can help with: Pain management Scar tissue Muscle guarding or weakness Neurological symptoms that may persist or reappear Do You Need a Scan if we’re suspicious of TOS? Imaging, as discussed in other blogs, may be recommended when we are suspicious of other presentations, or if standard method are not creating any difference. For example: To rule out cervical disc herniation, tumours, or other causes of neurovascular symptoms. When […]
Cosmetic surgeries have become increasingly common, with procedures such as liposuction, tummy tucks, facelifts, and breast augmentations helping people achieve their desired aesthetic goals. However, while the surgical aspect gets most of the attention, what often goes under-discussed is the importance of post-operative care, especially Manual Lymphatic Drainage (MLD) in promoting faster, smoother recovery and reducing the risk of ending with fibrosis tissue build up underneath the skin. What Is Manual Lymphatic Drainage (MLD)? MLD is a gentle, rhythmic massage technique designed to stimulate the lymphatic system and encourage the natural drainage of lymph fluid. The lymphatic system plays a crucial role in immune function and fluid balance. After cosmetic surgery, lymphatic flow can become disrupted due to inflammation, surgical trauma, or temporary damage to lymph vessels. While the first few days post-surgery are dedicated to acute recovery and the taking of Antibiotic to reduce the risk of infection post-surgery, as soon as this risk is passed, that’s when you want to start your MLD journey. Why Is MLD Important After Cosmetic Procedures? Cosmetic surgeries often cause swelling, bruising, and fluid accumulation (known as seroma or edema). This is due to the body reacting to an invasive procedure and removing tissue beneath the skin. MLD helps: ✅ Reduce post-surgical swelling ✅ Accelerate the removal of metabolic waste and excess fluid ✅ Improve skin texture and reduce fibrosis (hardened tissue) ✅ Speed up visible results by enhancing contour definition ✅ Decrease discomfort by reducing pressure from trapped fluids As with any surgery, when lymphatic drainage massage is applied, no pain is to be experienced. While I treat someone with MLD I always pass this information up front, to ensure that if they experience any type of pain, I get told about it, so that I can go lighter with pressure. Which Procedures Benefit Most from Lymphatic Drainage? MLD is commonly recommended after: Liposuction (including 360 lipo or Brazilian Butt Lift – BBL) Tummy tucks (abdominoplasty) Facial surgeries (rhinoplasty, facelifts, blepharoplasty) Breast augmentation or reduction Body contouring procedures As a Lymphoedema therapist, I do get surgeons referring me patients to assist them with post-op management, especially when swelling or fibrosis is a concern. When Should You Start Lymphatic Drainage? As briefly explained above, the ideal time to begin MLD is as soon as you stop your antibiotic cycle, and is your surgeon or GP call to when you are safe to do so. On the other hand: Typically, MLD is started 3 to 5 days post-surgery, once acute inflammation has settled and the incision sites are closed or protected. A full course may include 6–10 sessions spaced out over a few weeks for optimal results. Always follow the advise of the surgeon about post surgery, but, when you safe to do, the more movement we add to Lymphatic Draiange, the better the recovery would go. Is MLD Safe post-cosmetic surgery? When performed by a qualified lymphatic therapist, lymphatic drainage is non-invasive, safe, and effective. It’s gentle enough for delicate post-op tissue and can significantly improve comfort and healing time. My qualification in Lymphatic Drainage was done with the Vodder Academy whicg holds the gold standards for MLD practice, and is worldwide well known for the quality of their practice. On the other hand, I also hold a qualification in Clinical Myotherapy, which allows me to help people recover from injury and stick to their fitness goals via training and exercises. When Can I Book My Appointment for Post-Cosmetic Surgery Recovery? My studio, Melbourne Massage and Treatment, is located in Fitzroy North, on the corner of St George Rd and Holden St. I work Monday to Saturday, and to book an appointment, you can just head online to the booking page and choose the best time/days that work for you. Given the number of session needed for this type of work, I always suggest to book a series of session in a raw, from to 3 session per week for the first 2 weeks. Session by session we do evaluate together the progress, and chose together what’s the next step. If you have any questions, please do not hesitate to contact me. FAQs – Cosmetic Surgery & Lymphatic Drainage
Bone fractures are a common injury, but with proper care and rehabilitation, bones can heal and regain strength. Strength exercise is a crucial component of this healing process, aiding in bone regeneration and restoring mobility and function. How can a bone fracture? Bones can fracture when placed under a load or force that they can’t tolerate. The load tolerance is subjective, person to person, and can vary based on the individual medical presentation and clinical history. Age it is only a circumstance that at the current moment in our society is seen as an increase the chance of fracture, but if we learn to age by keeping our feet via strength training, age would not be anylonger a risk component. Indeed, during the aging process, the bone can become weaker if not stimulate to positive stress, such as load active loads. The less load they received, the less the bone would keep regenerating, due to a slower metabolism. Therefor, as explained in other blogs, strength training is a key to longevity and better health. How can bone fractures heal? When a bone fractures, the body initiates a complex healing process involving several stages: Inflammation: Immediately after the fracture, blood clots form, initiating the healing process. Soft Callus Formation: Fibrocartilaginous tissue begins to bridge the fracture gap. Hard Callus Formation: The soft callus is replaced by a hard bony callus made of woven bone. Remodelling: The bone gradually remodels into its original shape and structure. This process can take several weeks to months, depending on factors like age, overall health, previous clinical history, medication intake and the severity of the fracture. Even though there is nothing that can speed up the recovery, as this is a body’s natural process, there are things that can be done to assist the recovery and ensure that the healing happens as smoothly as possible. Exercises are one of those factors that are part of the healing journey, but have to be incorporated under supervision, to ensure not to aggravate the presentation. The Role of Exercise in Bone Regeneration As mentioned above, and in other blog exercises, specifically strengthening exercises are a positive load for the body tissues, including bone, which can help stimulate the regeneration of those tissues. Obviously, different phases of healing require and can accept different types of strength exercises. So yes, you would not start with a single-leg jump on a broken tibia Stimulates Bone Formation: Mechanical stress from exercise promotes osteoblast activity, leading to new bone formation. Enhances Strength and Flexibility: Regular movement prevents joint stiffness and muscle atrophy. Improves Balance and Coordination: Reducing the risk of future falls and fractures. A systematic review by Kuijlaars et al. (2019) highlighted that physical therapy exercises, whether home-based or supervised, significantly improve functional mobility and strength post-fracture. Recommended Exercises for Recovery At Melbourne Massage and Treatment, I offer assistance with bone fracture recovery exercises throughout the Myotherapy and Fitness class treatment plan. What I would focus on, too, when aiming for recovery, would be: Weight-Bearing Exercises: Including walking or gentle jogging (if we are talking about lower limb injury), to stimulate bone growth; Resistance Training: Using bands or light weights to strengthen muscles supporting the bone, or the joint to which the bone is attached. Flexibility and Balance Exercises: Again, using weights and machinery, we aim to strengthen the muscles that control your overall equilibrium and stability to prevent further falls and reduce the risk of injury. Plyometrics which is most often towards the end of a recovery process from anytype of injury, where we focus on motion that are more close to return to daily activity, and we load your tendon as springs, as per can be doing jumping on the spot or repetitive explosive motions with arms. Clinical Evidence Supporting Exercise in Recovery from Bone Fractures Research, as already mentioned in the Kuijlaars et al. (2019) systematic review, shows the benefits of incorporating exercise into fracture rehabilitation, and below we look into more details about what exercises have to offer in terms of recovery: Improved Healing Rates: Patients engaging in structured physical therapy often experience more robust bone healing (Song, 2022). Reduced Complications: Regular movement decreases the risk of complications like deep vein thrombosis or joint stiffness (Ruan et al., 2023). Enhanced Quality of Life: Maintaining physical activity levels improves overall well-being and independence (Mahindru et al., 2023). What to consider when doing exercises post-bone fractures. While exercise is beneficial, it is always important to approach the recovery process with care: Follow Medical Advice: Always adhere to the guidelines provided by healthcare professionals. Avoid Overexertion: Pushing too hard can hinder healing or cause re-injury. Going hard or going home is not how recovery works. Monitor Pain Levels: Some discomfort is normal, but sharp or persistent pain should be addressed immediately. Pain-wise, on a scale of 0 to 10, we usually aim to get you to experience a comfortable discomfort, based on your worst pain experienced as a maximum threshold. Recovery from an injury, including a bone fracture, is a personal journey, and therefore is unique to everyone, in terms of how quickly it can be and what considerations to take into place during the exercise recovery. FAQs – Bone Fractures Recovery and Strength Training 1. How do bones fracture?Bones can fracture when exposed to forces they cannot tolerate. This tolerance varies from person to person, depending on factors like health history, bone density, and physical condition. While age is often seen as a risk factor, it’s more about reduced activity levels. With consistent strength training, the risk of fractures can be lowered significantly, regardless of age. 2. How does a fractured bone heal?Bone healing occurs in four key stages: Inflammation: Blood clots form to protect and initiate healing. Soft Callus Formation: Fibrous tissue bridges the fracture. Hard Callus Formation: New bone begins forming. Remodelling: The bone reshapes to its original form.This process varies in duration based on the severity of the fracture and individual health factors. 3. Can exercise speed […]
The Star Excursions Balance Test (SEBT) is a fabulous functional test that can tell us a lot about the mobility and stability of the ankle, knee, and hip joints. On top of being a functional test, the star excursion can also be used as an exercise, and via a series of progressions, which we will discuss in more detail later, can help you train for better running performance and injury prevention. Why is the Star Excursion Balance Test Important? The importance of the Star Excursions Balance Test lies in its ability to assess, with one motion, the capacity of your ankle to remain stable on the surface of support (the floor) and how this stability is transmitted to the knee first and, consequently, to the hip. This is possible because the transfer of vertical pressure is applied to each joint while you are aiming to get the movement done. The movement required is to keep the feet of the anchor down to the floor, from the toes to the heel, while with the other foot, you aim to reach the furthest point away within the eight cardinal directions (like a star *). Along those movements, then, we also get observational data about your: Proprioception: The ability to sense the position of the body and its parts in space. Balance: The ability to control the body’s centre of mass over a stable base of support. Functional Movement: How well the body can perform multi-directional movements, such as stepping, reaching, and stabilising. The Role of the Star Excursion Balance Test in Lower Limb Injury Recovery So, if you are someone who has sustained lower limb injuries, particularly around the ankle, knee, or hip, these capabilities are often compromised. By using the Star Excursion Balance Test, we can: Assess any deficits in these areas, which might increase the risk of re-injury or limit recovery progress. But not only that. Indeed, that information will shape the recovery program, allowing us to understand better which muscle group or joint we need to focus more on with the exercises. Help runners, as running is a dynamic activity that places high demand on the lower extremities. Even minor imbalances or weaknesses can lead to conditions such as IT band syndrome, shin splints, and knee pain. The Star Excursion Balance Test helps in identifying these early warning signs before they evolve into more serious conditions. What Does the Star Excursion Test Measure? The primary purpose of the SEBT is to evaluate a person’s capacity to control body movement while standing on one leg. In rehabilitation, the Star Excursion Balance Test trains and improves: Ankle Stability and Control: It challenges the ankle to support the body’s weight while shifting through various planes of motion. Knee and Hip Joint Function: By demanding strength and flexibility in the lower limb, it helps retrain the kinetic chain, especially after joint injury. Balance and Proprioception: The test improves your ability to sense where your body is in space, which is essential for both preventing and recovering from injuries. Postural Awareness: Training balance also trains your ability to maintain proper posture, which can reduce stress on your joints and muscles during exercise. In fact, the test consists of reaching with one leg in multiple directions (anterior, posterior, medial, and lateral and a mix of those directions) while maintaining balance on the other leg. This shows their neuromuscular control and postural stability. It mimics the demands placed on the body during dynamic activities like running, cutting, and jumping. The Progression of the Star Excursion Test The beauty of the Star Excursion Test is its flexibility. It can be adapted based on the individual’s injury level, fitness, and goals. The test itself involves several variations, which I implement depending on the stage of recovery or the individual’s needs: Softer Ground: For those in the early stages of rehabilitation, we may perform the test on a softer surface, such as a foam pad or balance disc. This reduces the stability of the base and forces the individual to engage more stabilising muscles, which aids in proprioceptive training and can be beneficial for rebuilding ankle and knee control. Weight on the Ankle: For those who have had ankle injuries, I often modify the test to place more weight on the injured ankle. This helps rebuild strength and functional control, as it forces the injured area to bear load and engage in movement patterns that may have been avoided during the healing phase. Eyes Closed: To increase the challenge, I sometimes ask my clients to perform the test with their eyes closed. This removes visual input, forcing the body to rely more on internal feedback (proprioception). This is especially important in the latter stages of rehabilitation, as it helps to refine neuromuscular control and reduce reliance on external cues. Using the Star Excursion Test with Lower Limb Injury Recovery and Runners The SEBT is a functional test that I like to use, with all its variations, to assess the progress of patient recovery. Whether you present with an injury, or you want to improve your form and body functionality throughout exercises, the SEBT allows us to look in depth at what we need to work on, too. For example, after a sprained ankle, I’ll often use the SEBT to check whether an individual is able to move without compensation, ensuring that their body has regained sufficient control and strength before returning to activities like running or sports. And this, don’t be surprised, is something that I do and has to be done whenever someone presents with complaints about knee or hip pain, too. Again, an unstable ankle would transmit that instability up the chain. On the other hand, for runners, the test helps evaluate areas of weakness that might predispose them to injuries such as Achilles tendinopathy, patellofemoral pain, or iliotibial band syndrome. Since running places repetitive stress on the lower limbs, identifying and addressing weaknesses early can prevent long-term problems and improve overall performance. Myotherapy and SEBT […]
Ankle sprains are among the most common injuries, especially for athletes, active individuals, and even those who simply trip or misstep during daily activities. Despite being a frequent injury, the importance of properly recovering from an ankle sprain is often underestimated. Proper rehabilitation is crucial not only for returning to normal activities but also for preventing long-term complications like chronic instability, arthritis, or re-injury. In this blog, we’ll take a closer look at ankle sprains, their impact on the ligaments involved, and why recovery is so vital for the health of your ankle and the joints above it. What is an Ankle Sprain? An ankle sprain is an injury that occurs to the ankle ligament, which may stretch or be torn. Most commonly, this happens on the lateral portion of the ankle, as the plantar of the feet turn internally. The role of ligaments is to connect bones to each other and provide stability to the joint. In the acute phase of injury, you may experience swelling, pain, bruising, and sometimes instability in the joint. Mechanism of action includes sudden twisting, rolling, or turning motions, like sports or walking on uneven surfaces. Not all ankle sprains are the same, indeed, we have a classification system for it, which is based on their severity: Grade I (Mild): A slight stretching or microscopic tearing of the ligament fibres, typically causing minimal swelling and pain. Grade II (Moderate): Partial tearing of the ligament, with noticeable swelling, bruising, and limited mobility. Grade III (Severe): Complete rupture of the ligament, leading to significant swelling, instability, and difficulty bearing weight. Which Ligaments Are Most Affected? The ankle joint consists of several ligaments, but sprains most commonly affect the lateral (outer) ligaments. These include: The anterior talofibular ligament (ATFL) is the most commonly sprained ligament on the front of the ankle. Calcaneofibular ligament (CFL): A ligament that connects the fibula to the heel bone. Posterior talofibular ligament (PTFL): Less frequently injured, but it can be involved in more severe sprains. Studies show that the ATFL is the most commonly injured ligament, with up to 85% of all lateral ankle sprains involving this ligament (Kerkhoffs et al., 2012). The CFL is also frequently injured, but less commonly than the ATFL. As mentioned above, most often an ankle sprain happens on the lateral portion of the ankle, but in rare cases, the deltoid ligament on the ankle’s medial (inner) side can be sprained, particularly during more forceful or traumatic incidents. Why more laterally than medially? Biomechanically, our ankle finds it easier to turn inwards than outwards. Therefore, it is easier to exceed in ankle inversion (the feet’ plantar face the medial line of the body) than the other way around. This is due to the disposition of the bond in the ankle and feet. The Risks of Not Fully Recovering from an Ankle Sprain Many people recover from an ankle sprain and return to normal activities, but this doesn’t always mean the ankle is fully healed. Incomplete recovery can lead to several risks, including: Chronic Instability: If the ligaments don’t heal properly, the ankle may feel unstable, making it prone to future sprains or injuries. This can create a cycle of repeated sprains, leading to longer-term joint instability. Re-injury: Insufficient rehabilitation increases the risk of re-injury. Returning to physical activity too soon or without proper strength can cause the ligaments to overstretch or tear again. Arthritis: Studies have shown that improper healing of the ankle joint can lead to post-traumatic osteoarthritis (PTOA). This occurs when the joint surfaces are not properly aligned during healing, leading to cartilage degradation over time. Research suggests that 5-20% of individuals who suffer from ankle sprains may develop PTOA later in life (Delco et al., 2017). Muscle Weakness and Atrophy: After a sprain, the muscles around the ankle often weaken due to disuse and immobilisation. This weakness can extend to other areas of the body, increasing the risk of compensatory injuries (e.g., knee or hip strain) as you change how you move to protect the injured ankle. The Benefits of Proper Recovery As with any injury, the recovery process is dictated by your subjective presentation, which includes your clinical history, fitness level, and more. Here are some of the key steps for a full recovery: Achieve strength and joint stabilityThanks to the therapist’s guidance and a mix of treatment and exercises focused on the muscles that cross the ankle joint, like the peroneal and calf muscles, you can regain ankle stability and strength to return to your daily activities. This process can take up to 12 weeks, and its success is based on a mix of your clinical history and effort placed in the recovery process. Reduction in the Risk of Chronic PainPast the acute phase of injury, the risk of developing chronic pain is a common problem for individuals who don’t rehabilitate properly after an ankle sprain. In fact, studies suggest that proper rehab can reduce the risk of long-term pain by improving joint function and reducing stiffness with research indicating that patients who complete a rehabilitation program are 60-70% less likely to experience chronic ankle pain compared to those who don’t (Gribble et al., 2016; Zamperetti et al., 2019). Rehabilitate the Range of MotionA key goal of rehabilitation is to restore the full range of motion (ROM) to the injured joint. Restoring normal ROM is critical for preventing compensatory movements that can strain other joints along the joint chain, like the knee, hip, or lower back. The Recovery Process: What to Expect Proper recovery from an ankle sprain typically involves several stages: Acute Phase (0-72 hours) – P.E.A.C.E: Protect: Safeguard the injured area from further harm and avoid excessive strain. Elevate: Raise the injured area to reduce swelling and improve blood flow. Avoid Anti-inflammatories: Refrain from using anti-inflammatory medications unless advised by a healthcare professional, as they can hinder the natural healing process in some cases. Compress: Apply compression (e.g., with bandages or sleeves) to reduce swelling and provide support. Educate: […]
Menopause is a natural phase in every woman’s life, but it comes with a variety of physical, emotional, and mental challenges. As hormone levels shift, particularly estrogen, progesterone, and testosterone, many women experience symptoms like hot flashes, mood swings, sleep disturbances, and weight gain. Fortunately, for managing menopause symptoms, various lifestyle changes can be put in place, such as exercise, a balanced diet, improved sleep hygiene, and stress management techniques. In this blog, we will explore how adopting a healthier lifestyle can significantly improve your menopausal experience. Exercise and Physical Activity For Managing Menopause Symptoms Exercise is again the best recommendation for health improvement that can be offered here. Of course, implementing exercises alone without following any other changes or advice (where needed) is not going to do the trick. But let’s start from here. Exercises can improve overall health and have specific benefits that help ease common issues like weight gain, mood swings, and hot flashes. But not only that. Indeed, exercises, and in particular strength training, are positive stress, which allows the body to regenerate and ensure the slowing down of bone and muscle mass, which is one of the main issues that a woman going through menopause is going to face. Here is a list of exercise routines that you could focus on. But keep in mind that if you really want to choose, I would strongly suggest Strength Training. Aerobic Exercise:Walking, swimming, cycling, or jogging would help in improving circulation, promote heart health, and relieve stress (for the last one, especially if done in open-air environment). Regular aerobic exercise has also been shown to reduce the frequency and intensity of hot flashes. Plus, it aids in weight management, especially during menopause when metabolism slows. Strength Training:Engaging in strength training exercises, such as weightlifting or resistance band workouts, helps preserve muscle mass and improve bone density, which decreases as estrogen levels decline. This is essential for reducing the risk of osteoporosis and maintaining strong bone and muscle mass. Yoga or Pilates:Both yoga and Pilates are great for improving flexibility, balance, and muscle strength while reducing stress and anxiety. These low-impact exercises help maintain your physical health and mental well-being, both of which can be affected by hormonal fluctuations during menopause. Tai Chi or Qigong:These ancient practices involve slow, deliberate movements and deep breathing. They are excellent for enhancing balance, reducing stress, and promoting relaxation—especially helpful for managing mood swings and anxiety. Eating an Anti-Inflammatory Diet A nutrient-rich diet can significantly help in managing menopause symptoms. By incorporating specific foods and avoiding certain triggers, you can reduce inflammation, balance hormones, and support your body’s needs during this transition. Phytoestrogens:Phytoestrogens are plant-based compounds that mimic estrogen in the body and can help alleviate symptoms like hot flashes and night sweats. Foods rich in phytoestrogens include soy products (tofu, tempeh, edamame), flaxseeds, lentils, chickpeas, and whole grains. Calcium and Vitamin D:As estrogen levels decline, the risk of bone loss and osteoporosis increases. To support bone health, incorporate calcium-rich foods such as leafy greens (kale, broccoli, sesame seeds), fortified plant-based milks, and dairy products. Vitamin D is crucial for calcium absorption, so get it from sun exposure or foods like fatty fish (salmon, mackerel) and fortified foods. Vitamin D is cumulative, so during the longer days of the year, ensure to spend some extra time in the sun. But of course, do so during the safest hours and not at UV light pick time. Regarding Vitamin D and Calcium supplements, there is a strong debate about whether they are good or what potential side effects they have, so you’d better talk to your GP about the specifications. Healthy Fats:Omega-3 fatty acids found in fatty fish, flaxseeds, chia seeds, and walnuts have anti-inflammatory properties that can help reduce joint pain and inflammation during menopause. These healthy fats also support heart health, which is increasingly important as estrogen levels drop. Whole Grains and Fibre:Fibre helps stabilise blood sugar levels and improves digestion, which can be helpful as metabolism slows. Incorporate fiber-rich foods like whole grains (brown rice, oats, rye), fruits, vegetables, and legumes to support digestive health and reduce bloating. In the case of beans and grain, ensure that they are soaked when needed to reduce the bloat side effect. Limit Sugary and Processed Foods:Foods high in sugar and processed carbs can cause blood sugar spikes and crashes, leading to irritability and fatigue. This is where having a variety of fresh food is a key component. So yes, no one wants you to overstress about what you eat or not, but, generally speaking, if you have never looked into a balanced anti-inflammatory diet, it is time to do so. Reducing Alcohol and Inflammatory Foods Both alcohol and inflammatory foods can exacerbate menopause symptoms, so limiting or avoiding them can provide significant relief. Limit Alcohol:While alcohol might seem like a way to unwind, it can actually trigger hot flashes, disrupt sleep, and contribute to mood swings. Moderation is key—try limiting your alcohol intake to no more than one drink per day, and if possible, reduce it further to see if it improves your symptoms. Alcohol is a substance that the body does not recognise, and it has quite a hard time breaking it down. Avoid Inflammatory Foods:Highly processed foods, refined sugars, and trans fats can increase inflammation in the body and worsen menopause symptoms like joint pain, fatigue, and mood swings. Instead, focus on anti-inflammatory foods such as berries, leafy greens, fatty fish, and nuts to support your body during this phase. Inflammatory foods are all those that contain Omega-6 fatty acids, which are long-chain fatty acids, that would get collected in your Lymphatic System at first, and attacked by the macrophages (white cells), inciting an inflammatory response. Caffeine:Excessive caffeine can disrupt sleep and worsen hot flashes. If you find that caffeine aggravates your symptoms, consider reducing your intake or cutting back on coffee and other caffeinated beverages, especially in the afternoon or evening. Here is a great podcast from ZOE podcast about […]
Bone density is a key factor in bond fracture prevention. Bone is made of cells that die and regenerate. When this process is compromised, the risk of fracture arises. During the early stages of life, we can ensure that we intake and store calcium through food to build up our bones, but after a certain age (about 30), the body stops absorbing calcium, and the storage that we created is now our reserve for the rest of life. Cell Regeneration in Bone and Other Body’s Tissues The body’s cells, like muscle cells, skin cells, tendon cells, ligament cells and even bond cells, are in constant change via a process called cell regeneration. Old cells die off and they get replaced with new cells. In the case of bone, the cells that allow this process to happen are called osteoblasts. While we age, this process slows down, meaning that cells would still die, but they don’t get replaced. A typical example is a woman going through menopause. Estrogen, which is the hormone responsible for bond metabolism, allows the activity of osteoblasts. During menopause, indeed, women have a drop in Estrogen production, and osteoblasts are not as operative as they used to be. Strength Exercises and Cell Regeneration As this meta-analysis shows, strength exercises are a positive stress stimulus for the body and can help the osteoblast work harder and maintain bone cell regeneration. When the body perceives stress as physical resistance, it does its best to establish a reparation mechanism. So whenever we pick a weight against gravity, the body would implement a regeneration of the tissue that are used to complete this action. Who Is at Risk of Losing Bone Mass? There are several factors that can contribute to decreased bone mass: Age: Bone density typically peaks in early adulthood and declines with age. Gender: Women, especially postmenopausal, are at higher risk due to hormonal changes that accelerate bone loss. Family History: A family history of osteoporosis can increase risk. Body Size: Individuals with smaller body frames may have less bone mass to draw from as they age. Hormonal Levels: Thyroid imbalances and reduced sex hormones can lead to bone loss. Dietary Factors: Low calcium and vitamin D intake contribute to diminished bone density. Lifestyle Choices: A sedentary lifestyle, excessive alcohol consumption, and smoking are linked to weaker bones. I have included factors like dietary and hormonal levels in the above list. Bear in mind that taking supplements such as calcium and vitamin D (which helps retain calcium) could have severe contraindications. So, always talk to your doctor or specialist about the intake of supplements. How to determine Bone Density? To determine bone density, there is a diagnostic test called Dual-energy X-ray Absorptiometry (DEXA or DXA). This non-invasive procedure measures the mineral content in bones, usually in areas like the spine, hip, or wrist, to assess bone density and identify potential risks of osteoporosis or fractures. The results are given as a T-score, which compares your bone density to the average peak bone mass of a healthy young adult. A T-score of -1.0 or above is considered normal, while a score between -1.0 and -2.5 indicates low bone mass (osteopenia), and a score of -2.5 or lower suggests osteoporosis. Other methods, like ultrasound or quantitative computed tomography (QCT), can also assess bone density, but DEXA remains the gold standard for bone health evaluations. Mobility before strengthening So far, we have discussed how strength exercises are a good way to maintain bond density. Still, I would not recommend that anyone who is not into strength exercise and has bone density issues go and start lifting heavily. Why (?), you may ask. Well, before we start lifting heavy, we want to ensure that the body mechanics are optimal for it, so we better start looking into your mobility and then pass on to the strength part of things. Please be aware that mobility has nothing to do with elasticity or stretching. Those are different practices. How Can We Achieve Great Mobility For people who decide to take a journey to ensure an optimal level of mobility and then strengthen the body, the first step is to assess their joint mobility with active and passive range of motion. After that, we could use a combo of Myotherapy treatment and mobility exercises to ensure they can quickly pick up the best of their mobility capacity, given their subjective presentation. And here is a list of mobility exercises which we may look into at first: Hip Openers to improve range of motion in the pelvis and lower back. Ankle Drills to support proper weight distribution in weight-bearing exercises. Thoracic Spine Mobility Exercises to prevent excessive strain on the lower back. AC Joint External rotation to ensure we can build strong rotator cuff muscles, essential for shoulder health It Is Time To Strength. How Can We Do This? Once the minimum mobility is achieved, which may take 1 to 2 weeks of training, depending on each individual and their subjective history and effort, we can start looking into more strengthening exercises. So, here is a list of different exercises that can help with strengthening, written with the progressions to follow: Calf raises with double leg, single leg and weight Hamstring and Quads Curl that gets weight added as weeks go by Standing Adduction and Abduction at cable machine or with resistance bend Glut Muscles training at cable machine or with resistance bend Deadlift for back and posterior chain muscle strength Squat with weights and explosion variations Cuff rotator-specific strength is Ideal before stepping into more complex arm weight-lifting Cervical muscle strength to prevent cervical headache and sore neck All of those exercises, except the cervical one, can then be modified to achieve plyometric drills and combined movement. But this is a process that would take months, and there is no rush to get to it, as I want you to be safe throughout the entire journey. Integrating Exercise into Myotherapy Treatment At Melbourne Massage and Treatment, I incorporate […]
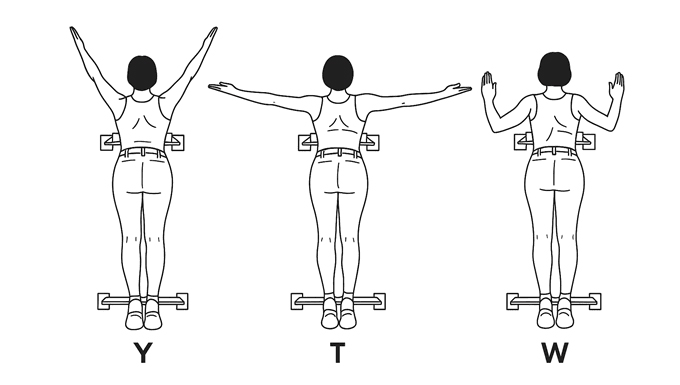
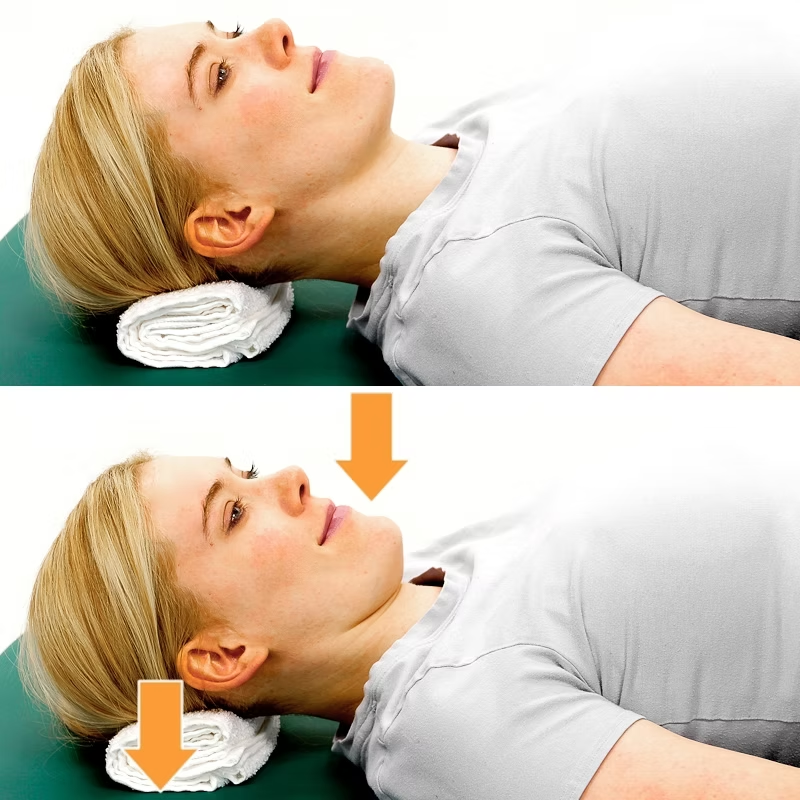
Whiplash is a common neck injury caused by a sudden and forceful back-and-forth motion of the head. We often see this in patients who go through a car accident, contact sports injuries (AFL, rugby or even Soccer), or falls. While whiplash is usually not life-threatening, we now know that it can cause persistent pain and discomfort, affecting daily activities. Therefore, it is important to understand its symptoms, causes, and the best exercises for recovery, which can help individuals manage and overcome this condition effectively. Common Causes of Whiplash Whiplash is a term used to describe a fast rocking motion of the cervical area and is most frequently caused by: Car accidents: Rear-end collisions are the leading cause, as the sudden force propels the head forward and backward. Sports injuries: Contact sports like football, boxing, or hockey but even AFL, Rugby or even Soccer increase the risk of whiplash injuries. Falls: Slipping and falling can cause the head to jerk suddenly, leading to whiplash. Physical assaults: Blows to the head or sudden jolts, such as those experienced in shaken baby syndrome, can result in whiplash. What are the consequences of Whiplash for the cervical ligaments? The consequences of whiplash for the cervical ligaments can be significant, leading to long-term instability and chronic pain. When the ligaments are overstretched or torn, they lose their ability to support the cervical spine, resulting in properly: Reduced Stability: Weakened ligaments can no longer provide adequate support to the cervical vertebrae, leading to excessive movement and an increased risk of further injury. That’s why stretching is not recommended either. Chronic Pain and Stiffness: Persistent discomfort may arise as the muscles attempt to compensate for the lack of ligament support. Increased Risk of Degeneration: Ligament damage can accelerate wear and tear on the cervical joints, potentially leading to conditions such as osteoarthritis. Neurological Symptoms: Instability in the cervical spine may irritate or compress nerves, leading to headaches, dizziness, or numbness in the arms. Symptoms of Whiplash Whiplash symptoms can range from mild discomfort to severe pain, and they often appear within hours or days of the injury. Common symptoms include: Neck pain and stiffness: One of the most prevalent symptoms, often worsening with movement. Headaches: Typically originating from the base of the skull and radiating toward the forehead. Shoulder and upper back pain: The impact can cause muscle strain in surrounding areas. Reduced range of motion: Difficulty moving the neck due to stiffness and discomfort. Dizziness and fatigue: A common reaction as the body copes with the injury. Tingling or numbness in the arms: Nerve involvement may lead to sensations of pins and needles. Cognitive issues: Some people experience memory problems, difficulty concentrating, and irritability. Those symptoms may not present all at once, and they can belong to other presentations, while whiplash did or didn’t happen anytime before. That’s why when we go through a clinical history taking, as Myotherapist, we take our time to dig into your past and your body habits, as this can give us important information about your current presentation and what we can do to improve it. Why Can Whiplash Become a Lifelong Issue? In some cases, whiplash can become a chronic condition due to the instability of cervical ligaments. Cervical vertebrae can be divided into two parts, Mobile and Stable joints. C1 to C2 are the mobile ones, whereas C3 to C7 are the stable ones. Now, if along a whiplash incident, the ligaments of either the mobile or, most luckily, the stable side get strained, the muscles surrounding that segment of the joint would have to work harder to maintain stability. This would lead to to ongoing discomfort, reduced mobility due to pain and muscle spasms, and increased vulnerability to future injuries. If left untreated or managed improperly, this is how the condition can become chronic and lead to other injuries along the way. Importance of Thoracic Mobility Thoracic mobility plays a crucial role in preventing the chain effect of mobility and stability issues between the thoracic spine, lower cervical, and upper cervical regions. If the thoracic spine is stiff or restricted, the lower and upper cervical spine must compensate, leading to increased strain and pain. Improving thoracic mobility through targeted exercises can help reduce this compensatory stress, allowing for better neck function and reducing the risk of chronic discomfort. In a case of a previous history of whiplash, maintaining good thoracic mobility would allow the cervical area to focus on its duties, so stability for the lower portion and mobility for the upper. Reducing the risk of overcompensation and muscle fatigue. Effective Exercises for Whiplash Recovery A structured exercise program is essential for whiplash recovery. This program should begin with isometric exercises to restore basic cervical movement, progress to concentric exercises to rebuild strength, and eventually include thoracic mobility drills to enhance overall spinal function. Phase 1: Isometric Exercises for Early Recovery. For the first 2 weeks post-injury, 5 to 7 days a week. Isometric exercises help activate muscles without excessive movement, providing a stable foundation for recovery. This step is essential to start driving more blood to the area irritated by the whiplash and also allow the central nervous system to feel confident in perceiving the cervical structure moving without pain. Isometric Neck Holds: Place your hand on your forehead and gently press against it without moving your head. Push only 25% of your strength, as it has to be a pain-free exercise. Hold for 5-10 seconds and repeat 5 times. These exercises can be done in any cervical movement, such as extension, lateral flexion, or rotation, by using your hand as a resistance and pushing always at 25% of your strength. The strenght of push does not ever progress, what you will progress within isometric exercises are the time fram of push, repetitions and sets. Phase 2: Concentric Strengthening Exercises. From week 3 post-injury onwards,3 to 5 times a week. Once the pain subsides, which we would expect to happen in 2 weeks about it, gradual […]
Greater Trochanteric Pain Syndrome (GTPS) is a common condition that causes persistent lateral hip pain, often making everyday activities like walking, climbing stairs, or even lying on your side difficult. GTPS primarily affects middle-aged individuals, particularly women, and is commonly linked to issues such as gluteal tendinopathy and weakness in the hip stabilizing muscles. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. GTPS Symptoms Greater Trochanteric Pain Syndrome can present with a series of symptoms that are local to the side of the hip. Here are the most common: Lateral hip pain: Persistent pain on the outer side of the hip, which may extend down the thigh. Pain when lying on the affected side: Discomfort that worsens when lying directly on the hip. Tenderness to touch: Sensitivity around the greater trochanter, which may be painful to press. Pain with movement: Aggravation of pain during walking, climbing stairs, or standing for prolonged periods. Weakness in hip muscles: Reduced strength in the gluteal muscles, leading to instability in movement. Difficulty sitting for long periods: Sitting on hard surfaces can exacerbate discomfort. Mechanism of Injury for GTPS GTPS is primarily associated with tendinopathy of the gluteus medius and/or minimus muscles, with or without accompanying bursitis. As per many tendon injuries, this condition often arises from repetitive stress or overuse, leading to microtrauma and degeneration of these tendons. On the other hand, abnormal hip biomechanics can exacerbate the issue, as compressive forces cause impingement of the gluteal tendons and bursa onto the greater trochanter by the iliotibial band during hip adduction. Contributing factors to GTPS include acute trauma, such as a fall onto the lateral hip, prolonged pressure from lying on one side, and overuse from activities like running or stair climbing. Additionally, conditions like iliotibial band disorders and gluteal muscle weakness can increase the risk of developing GTPS. Understanding these mechanisms is crucial for effective management and prevention of GTPS. Evaluation of GTPS Diagnosing GTPS typically involves a combination of clinical examination and medical history assessment. After taking your clinical history, including sports and work activity, I will perform a series of tests to validate the suspicions of GTPS. Those tests include single-leg stance and resisted hip abduction, which we would expect to show weakness in single-leg standing and pain during the abduction movement. Lastly, we would also palpate the area, which is a test that is kept for last because we want to avoid flair the presentation, which may be painful with any other test after that. In some cases, imaging techniques like ultrasound or MRI may be used to rule out other conditions and confirm gluteal tendinopathy or soft tissue abnormalities. I personally do not recommend image testing as the first way to go because the impact of seeing physical damage can also have a negative impact on self-perception, making a recovery harder. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. The difference between GTPS and Femoroacetabular Impingement (FAI) The difference between GTPS and FAI stands in the hip area involved in the injury. The GTPS is relative to the side of the hip and involves the gluteus medius and minimus tendon and the bursa that separate that tendon from the greater trochanter of the femur. On the other hand, FAI is a presentation that still involves the hip, but it does take place on the anterior portion of the hip, as is characterised by and overgrowth of tissue on the femur head or the hip socket, and it does manifest with hip flexion and external rotation. That’s why it is important to receive an evaluation of the presentation from a professional, in order not to mix the two presentation, or also, in order to evaluate if both presentation are present at the same time, which can also happen. The Role of Exercise in GTPS Treatment A recent systematic review and meta-analysis analyzing multiple randomized controlled trials found that structured exercise provides significant benefits for individuals with GTPS. The findings revealed that: Long-term pain reduction: Exercise can lead to slight but meaningful reductions in hip pain over time. Improved physical function: Patients who engage in targeted exercise programs experience better mobility and overall hip function. Increased likelihood of meaningful recovery: Compared to corticosteroid injections, exercise significantly increases the chances of noticeable improvement in symptoms. One of the most notable takeaways from this research is that exercise has a long-lasting effect, whereas treatments such as corticosteroid injections may provide only short-term relief. Additionally, no serious adverse effects were reported with exercise-based interventions, making it a safe and sustainable approach to managing GTPS. Why Choose Exercise Over Corticosteroid Injections? Corticosteroid injections have often been used for GTPS pain relief, but the research indicates that exercise leads to better long-term outcomes. While injections may offer temporary symptom relief, they do not address the underlying causes of GTPS, such as gluteal muscle weakness or tendon dysfunction. Exercise, on the other hand, strengthens the hip muscles, improves joint stability, and reduces the likelihood of recurring pain. In a previous blog post, I spoke about the key role of Gluteus Medius as a pelvis stabiliser. Effective Exercises for GTPS At Melbourne Massage and Treatment in Fitzroy North clinic, I design individualised exercise programs to help patients with GTPS regain strength and function. Some of the most effective exercises for GTPS include: Isometric exercises involve holding static positions to engage the hip muscles without excessive movement, reducing pain and improving muscle endurance, driving blood to the tendons and joints, helping with recovery. Strength training: Progressive strengthening of the gluteus medius and minimus muscles to enhance hip stability. Functional movement training: Exercises that mimic daily activities to help improve movement patterns and prevent pain triggers. Along those exercises […]
- 1
- 2