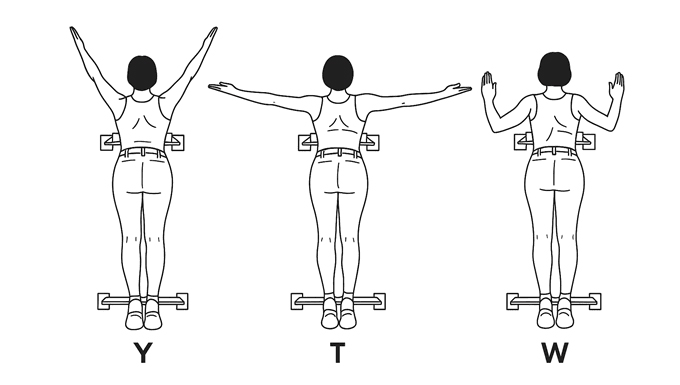
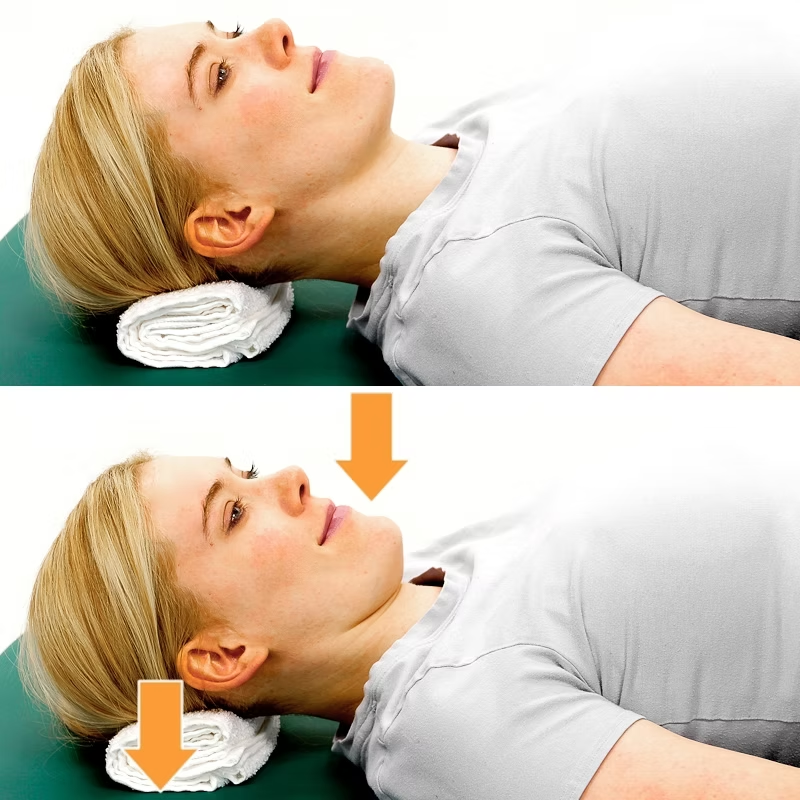
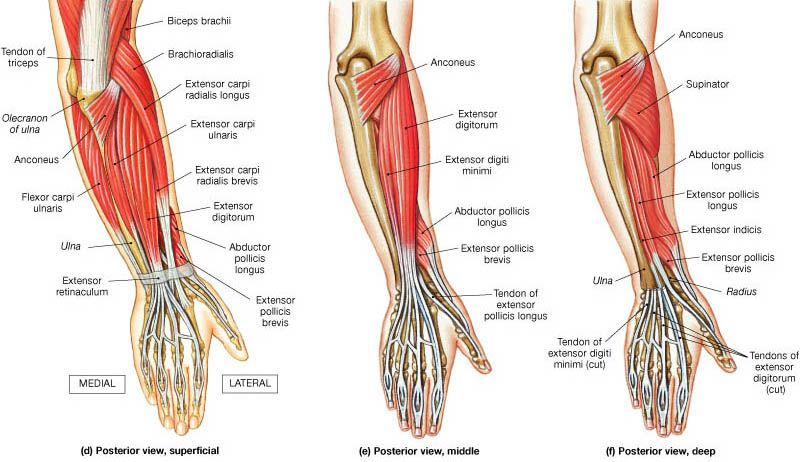
Neck pain and or upper back pain often originates from a disbalance of mobility and stability joints along the spine, including poor scapula-thoracic joint stability and thoracic mobility. Indeed, a hypermobile scapula can lead to instability, muscular imbalances, and chronic tension in either the shoulder joints or the cervical. Therefore, assuming that neck pain is only a neck issue is a bit limiting. We need to look at the bigger picture and target the right reason why you are in pain. In this blog, we are going to look at how scapular stabilisation exercises can restore balance, enhance posture, and reduce neck pain. Understanding Scapular Stability and Hypermobility The scapula, or shoulder blade, plays a vital role in upper-body movement and stability. It acts as the foundation for arm motion, connecting the humerus to the thorax through the scapulothoracic joint. When control is compromised, which is common for those with general hypermobility or for those who have scapular hypermobility, the result can be excessive movement and discomfort. Consequences of having a hypermobile scapula are: Neck and shoulder pain Reduced athletic performance Increased injury risk Muscle fatigue and tension As is often recommended, we need to look at strengthening as a way to improve muscular control of the joint, and in this case, we would look at: rhomboids, trapezius (upper, middle and lower), and latissimus dorsi, which is essential for restoring balance and function. Mobility Comes First: The Foundation of Stability As already mentioned in so many other blogs, and as I educate my clients all the time, before introducing strengthening exercises, mobility must be addressed. A stiff thoracic spine forces the scapula to compensate for many shoulder movements, leading to muscles originating and or inserting in the scapula to be overused, leading to pain and discomfort. Essential Thoracic Mobility Exercises There are some really easy exercises that you can do to pick up on thoracic mobility. Here is a short list: Foam Roller Thoracic Extensions Open Book Rotations Thread-the-Needle Cat-Cow Mobility Drill Diaphragmatic Breathing Exercises Those exercises would help in restoring thoracic mobility, preparing the groundwork for effective scapulothoracic stability exercises. Key Muscles for Scapular Stabilisation Now we can look at the muscle that we would need to strengthen to create a better scapular stabilisation. Rhomboids Function: Scapular retraction and stabilisation. Importance: Provide postural support and control during pulling movements. Recommended Exercises: Resistance Band Rows Prone T Raises Seated Cable Rows All those exercises can be easily delivered at home, with some decent resistance bands, or with light weights. But don’t let the simplicity of these rhomboid exercises fool you, as prone T raises, to start with, are enough even with no weights, as the weight of your arm is already enough. Trapezius (Upper, Middle, and Lower) Function: Elevation, retraction, and upward rotation of the scapula. Each fibre group has a different role regarding the scapula movement.Importance: The lower trapezius is essential for shoulder stability and posture. Recommended Exercises: Prone Y Raises Wall Angels Face Pulls Shoulder Shrugs Again, those exercises don’t require a full gym set-up, but some strong resistance bands and light weights would do. Latissimus Dorsi Function: Shoulder extension, adduction, and thoracic stability.Importance: Connects the upper limbs to the trunk and supports efficient movement. Recommended Exercises: Straight-Arm Pulldowns Lat Pulldowns Assisted Pull-Ups Resistance Band Pulldowns Scapular Stabilisation Exercises for a Hypermobile Scapula Now that we have looked at which exercises are ideal for what muscle or muscle group, we can look at a combination of those based on generic fitness levels. Those exercise lists are obviously a generic recommendation, and unless we have already done some work and assessment, I would not suggest picking and choosing an exercise routine and trying your best to sort out your pain. Beginner Level Scapular Setting Exercises Wall Slides Isometric Holds Against a Wall Serratus Anterior Punches Intermediate Level Prone Y and T Raises Resistance Band Pull-Aparts Face Pulls Incline Dumbbell Rows Advanced Level Landmine Presses Farmer’s Carries Overhead Carries Pull-Ups with Controlled Scapular Movement Furthermore, these exercises for scapular stability enhance neuromuscular coordination and are particularly beneficial for individuals with hypermobility. How Scapular Stability Reduces Neck Pain While we can’t directly associate hypermobility of the scapula with neck pain, we also know that poor scapular control often leads to overactivation of the upper trapezius and cervical muscles, contributing to neck pain. By strengthening the stabilisers of the scapulothoracic joint, mechanical stress on the neck is reduced. Therefore, here is a list of the benefits of scapular stabilisation exercises: Improved posture Reduced neck and shoulder pain Enhanced thoracic control Increased muscular endurance Better movement efficiency Lower risk of injury How We Support Scapular Stabilisation at Melbourne Massage and Treatment At Melbourne Massage and Treatment, in Fitzroy North, the treatment of scapular stabilisation starts from a tailored assessment of your presentation, looking at: Overall hypermobility Your clinical history Past and present sports activities Site of pain Pain time frame That and more information are essential to understand what your experience is, and what we can do about it. Hands-on treatment, like remedial massage or myotherapy, would be the first step to relax the body and allow you to feel and move better. The next step from that would be guiding you throughout exercises that you can deliver at home or at the gym, at your own time, so that you can take control of your pain and your presentation. All of this can be easily delivered along a treatment plan. And to simplify the whole process, I also offer a FREE 15-minute Online Consultation, where we can start looking into your presentation and understand what has been done till now and what needs to be done at this stage.
Tag Archives: mobility
Neck pain is such a common presentation, and often I have to hear from my clients that it is due to them storing stress in their neck or shoulder. I can’t think of how many times I heard this, and how many times I than have to ask questions like: “When was the last time you did some neck-strengthening exercises or movement for your neck?” “If you work in an office, how many screens do you have in front of you, and which one do you look at more often?” “Have you ever had a whiplash? And if yes, have you done anything about it?” As you would imagine, the answers are anticipated by a moment of silence, thinking and then in order of question: “I never do neck strengthening exercises, at best I do some stretching”. “2 or 3 screens and I look at the one on one side most of the time”. “Yes, but it was xx years ago, and I haven’t done anything about it, as I was too young to care about it”. Now, I believe that those answers are already going to give you an idea of where that pain may come from. In fact, the neck isn’t just tight, it’s often weak and poorly controlled. To fix that, we need to understand how the neck actually works and how we can strengthen it. Why Neck Strengthening Matters (Mobility vs Stability) Each cervical spine is unique, and we can all present with different needs and capacities for movement. Indeed, a hypermobile person may find their neck to be really mobile and easy to twist and turn. Hypermobility, as discussed many times, is an advantage for flexibility, but it comes with the cons of joint weakness and a higher risk of joint injuries. So, when looking at the cervical area, we may notice that it sits at the top of the joint chain, meaning everything from your shoulders to your lower back influences it. Specifically, the cervical is made of 2 joint sessions: The upper neck (C1-C2) is built for mobility (turning, nodding) The lower neck (C2-C3) is built for stability (supporting your head) When that balance is off, you’ll often notice: Neck stiffness Headaches “Poor posture” (forward head position) Ongoing discomfort Fortunately, those statements are backed up by recent research that shows how strengthening deep neck muscles improves pain, posture, and neuromuscular control, especially when mobility and stability training are combined. Chin Tucks (Deep Neck Flexor Strengthening) Chin Tucks are simple and effective neck strengthening exercises that I often prescribe for neck pain. Let’s then look at a series of progressions for this type of exercise: Chin-Tuck in all four: Position yourself in all four, with hands under the shoulder, and knees under the hips You will be looking at the floor where you have placed an object, right between your hands. Now retract the chin, while you keep looking at the object between your hands. Release the chin and repeat. This version of chin tuck is ideal for: Early rehab. People with pain or poor control. Learning correct movement without compensation. Chin-Tuck in sitting or standing position: Sit or stand upright (standing is the ultimate progression). Gently pull your chin straight back (like making a double chin). Keep your eyes level. Anyhow, you are going to do these exercises, ensure to do them slowly, and take your time doing them. 4 to 5 second tempo. Why Chin Tuck Works for Your Neck Strengthening This exercise activates your deep cervical flexors, which are the stabilising muscles that support your neck. Those muscles can be defined as stabilisers as they go from the thoracic vertebrae to the upper cervical vertebrae, for the longus capitis, which originates in the lower portion of the cervical (C3-C6) and inserts at the basilar portion of the occipital bone. When these muscles are weak: Your head shifts forward Larger muscles overcompensate (SCM) Pain builds over time Isometric Neck Exercises (Build Stability in All Directions) Isometric exercises are an optimal exercise that places major focus on tendons and ligaments, and are ideal for acute symptoms and warm-up pre-training. How to do it: Place your hand on your forehead and gently push into it (no movement) Repeat on: Back of your head Left side Right side Hold each for 5–10 seconds Perform 5 reps per direction This form of exercise can be applied in any direction of movement, such as flexion, extension, lateral flexion, rotation and mixed movement, like flexion on the diagonal side. Why it works: Isometric exercises are applied to pain-free range of motions, so while you move and contract the tissues, you are not experiencing pain, your brain gets triggered to be safe while the body moves, and your musculoskeletal tissues get looked after as they get activated and contract. This would help in improving joint stability and control. Shoulder Shrugs – Let’s Make Those Muscles Work Shoulder shrugs are a simple but effective way to build neck stability through the upper trapezius, which plays a key role in supporting the cervical spine as part of the broader joint chain. How to do it: Take in your hands a pair of weights, or an elastic band, which would you make pass under your feet. Gently lift your shoulders up toward your ears, pause briefly, then lower them with control. Why it works: Shoulder shrugs exercise does work by placing shared-load capacity between the neck and shoulders, reducing the strain on the cervical spine. On the other hand, when working on the cervical joints, it is ideal to intervene also on joints that are muscle-connected to the cervical itself, by adding global muscular support, which is essential for everyday loads. How These Exercises Fit Into the Joint Chain Your neck doesn’t work alone. As mentioned in many other blogs, all the body’s joints are part of a bigger system, the joint chain of mobility and stability. Therefore, if you present with: Tight shoulders A stiff thoracic spine Lack of movement […]
While I guide my client during a 1:1 fitness class at Melbourne Massage and Treatment, a Myotherapy clinic in Fitzroy North, on how to learn using bands or a single-column pulley machine to practice KLT (Kinetic Link Training), I often get asked how someone should or shouldn’t do a lunge. “Should my knee go ahead of my toes?” “Should my knee stay on top of my ankle?” “What about my back? Should I hinge or stay straight?” The answer to those questions lies in a simple fact: what part of the body are you trying to train? Are you aiming to build more glut (posterior chain) or quads (anterior chain)? No, because there is no perfect lunge, as either right or wrong. As per the squat, there is the lunge that works for you, for your presentation and for your goal. The Two Main Lunge Strategies (And Why They Matter) So, when we talk about lunges, most people are really debating between two variations: Knee Travels Forward (Past the Ankle Line) When going for this variation, we have to conceptualise that the knee is going into a deep flexion, right? Now, if the knee has to come out of flexion, the quads are the muscle that needs to be engaged. (Quads are the knee extensors). The deeper the knee flexion, the more quads fibres are engaged to do the reverse to get the extension done. In fact, what this type of lunge does is: Increases knee flexion Increases quadriceps demand Places more load through the patellar tendon Furthermore, research shows that when the knee moves forward, quadriceps force and knee joint stress increase significantly. In a super summary: This is a quad-dominant lunge. Vertical Shin (Knee Stays Over the Ankle) On the other hand, when delivering a lunge movement and the knee stays on top of the ankle, within a vertical shin line, there is a max of 90° knee flexion; therefore, the amount of fibre engaged for the quads is less, and what is than the primary mover for the ascending action, is the gluteus maximum, the biggest glut, which is going to help with the hip extension. So, in this variation, what we are going to achieve is: Shifting the load away from the knee Increases contribution from the hip extensors Encourages more posterior chain involvement Therefore, this will be a glute-focused lunge. What Biomechanics Actually Tell Us About The Lunge Exercise While we look at this movement, we may get triggered into thinking that the lunge exercise is knee-dominant because the knee does a lot of movement, right? Well, if we break it down a bit more, as Riemann et al. (2012) did, we find that yes, the knee moves a lot, but what really takes the load during the lunge movement is the hip. So this is how we can break it down: The knee moves more (kinematics). But the hip produces more force (kinetics). Why this is a thing, then(?) you may ask. Well is tru that the knee move a lot, it can flex up to 90° and still this can be a hip dominant exercises, but, we have to think that the knee, while it is moving that far, is not placing much load on the lower fibers of the quads, and the joint that has to push against gravity, in the ascending phase, are indeed the hip. That’s where all the load actually is. The weight of the upper body. The Lunge Game-Changer: Add a Hip Hinge And here is where we can add a twist to the lunge, by going into hip hinging. What happens if we do so? The glutes are placed under greater stretch at their origin. This increases mechanical tension. You get better glute recruitment and carryover in strength. In fact, this is not just theory, but it’s basic muscle physiology: Muscles produce more force when stretched under load. Therefore, by hinging at the hip, you are not only going to feel more burning sensation in the glutes, but you are going to train them even more effectively. Why Toe Mobility Is the Missing Piece Now let’s talk about something almost no one considers: Your toes. As often happens, the toes and feet are not taken into consideration when looking at functional movement. Even though every leg movement starts from there. In a proper lunge, especially for the rear leg, your toes need enough mobility (extension) to: Accept vertical load Stabilise the movement Prevent your body from shifting forward Indeed, if you lack toe mobility: The movement gets projected forward Load shifts into the front knee and quads You lose posterior chain contribution To support those statements, a study by Harato et al. (2019) examined how foot and toe positioning directly affects knee mechanics and load distribution. So to clarify, the mobility-stability joint chain must always be taken into consideration when we look at functional movement. In this case, your toes aren’t just along for the ride; they’re controlling where the force goes. So… Which Lunge Is Best? I hope that by now, you have an idea of what answer is coming up: Neither. There is no best lunge, as there is no best squat. The forward knee lunge is not “bad”; it’s a tool for quads. The vertical shin lunge is not “safer”; it’s a tool for glutes. The mistakes are thinking that: One can replace the other one. Having an injury in the knee, and thinking that lunges are not your thing anymore. That’s why, at my clinic, Melbourne Massage and Treatment, here in Fitzroy North, I always emphasise to my clients to understand that: “Don’t chase perfect technique — chase the right stimulus.” And to get to a better technique, better than what your body can deliver for now, is a step-by-step journey. And when there is an injury, we have to be confident in the tissue’s healing timeline, and exercises with load are the best tools to help with that. How I Use This With My […]
At Melbourne Massage and Treatment in Fitzroy North, as a clinical Myotherapist, I am enthusiastic to offer 1:1 fitness class that aim to improve your wellbeing and body strength. And one thing that I will never stop surprising my clients with is that it is never too late to start working on their strengths, no matter their age, gender, and capacity. Whether you’re recovering from injury, managing persistent pain, navigating age-related changes, or simply want more energy and confidence, personalised fitness is transformative. Why Starting Now A 1:1 Fitness Class Matters? Strength Training Improves Physical Health at Any Age Have you ever heard an older person wishing to be weaker? No, don’t you? That’s why strength and resistance training aren’t just for elite athletes or bodybuilders; they’re essential for everyone. As we age, our body’s natural capacity to regenerate, including regenerating muscle mass and strength, bone density, and other body tissues, naturally declines, which can affect balance, mobility, fall risk, and independence. Resistance training reverses this decline and improves functional outcomes. A systematic review by Kashi K. S. et al. (2023) found that resistance training significantly improved muscle strength, physical function, and reduced symptoms of depression in older adults. Exercise Matters for Mental Health Too Exercises are not only the best way to maintain physical health but also have an immense impact on our mental health. And that is a 1:1 fitness class or a group class, regular exercises can really change how you feel within your head. Infact, we have plenty of evidence from Recent Research that looks into this: A review by Ayaz A. et al. (2026) highlights how aerobic, resistance, and mind-body exercise modalities have psychological benefits, from improved mood to reduced stress and anxiety. Study by Ma Y. and Mumtaz S. (2025) finds that structured exercise programs improve mental well-being by activating neurobiological and psychosocial pathways. Meta-analysis by Rossi E. (2024) showed that strength training has moderate and significant antidepressant effects in adults with depressive symptoms. So yes, your workouts aren’t just changing your body, but they’re changing your brain. Why 1:1 Fitness Classes Are Especially Effective While training is beneficial for everyone, for physical and mental health, personalised training, like a 1:1 fitness class, makes a huge difference, and here’s why: Training Tailored to You Everyone has different goals when starting a fitness journey, or while they are training, and everyone has different needs and capacities, on which the goal is shaped. Therefore, a 1:1 fitness class session allows for customised programming that matches your goals, health history, injury status, and movement patterns, which generic videos or crowded group classes rarely provide. Expert Guidance Prevents Injury At Melbourne Massage and Treatment, I am proud of the studies I done (a Bachelor in health science clinical myotherapy, and following courses like the KLT training) and the effort I put in place to improve my fitness and communication skills, which led me to offer a tailored program for any of my clients. For people with pain, past injuries, or chronic conditions, this is crucial. Motivation and Accountability I often come across clients who don’t feel confident enough in themselves, who don’t like the gym and think that strength training for them is not a thing. And that’s when I can’t stop thinking about how powerful it is to change their mind by showing them how a few minutes of well-done movement, either with or without load, can change everything. That’s when I get them in for Fitness Class here in Fitzroy North, and I help them achieve their goals. Personalised Follow-up On top of a tailored 1:1 fitness class in person, what makes the difference in terms of service here at Melbourne Massage and Treatment, when I show some exercises, I will send you a PDF file with the picture and the description of the exercises, to ensure you will be bale to replicate those exercises anywhere you are ay your own time and comfort. Fitness Class Comes With An Added Bonus — Better Bone and Cardiovascular Health The action of lifting weights and lifting heavy is seen from your body as a positive stress, which creates a concatenation of benefits. Along those we find: Bone regeneration – increase of bone density Maintaining metabolic health Improving markers related to heart disease and diabetes Improve or maintain optimal equilibrium – poor equilibrium is the major cause of falls. And more… All the benefits a fitness class can deliver are crucial as we age. No one, as they age, wishes that their health gets more and more compromised, isn’t it? Start Where You Are — It’s Not About Perfection Whether you’ve never stepped foot in a gym before, you’re returning after an injury, or you’re trying to break a cycle of inactivity, the best time to start was yesterday. The next best time is now. It is never too late to start working on your strength, and this is the most important message I find myself passing on to my clients. The body can always adapt to load. And no matter if you have just started or you are a pro, you will always have to face some challenges. Therefore, start working on your mobility, improve the way your body can move, let’s than load it a little at the time, and build your own journey into wellbeing day by day, fitness class after fitness class. Final Thoughts You don’t need to be “fit enough” to start a 1:1 fitness class, and it’s absolutely never too late. Here’s the truth I’ve seen in across many clients: People in their 40s, 50s, 60s, and beyond see meaningful gains, both physically and mentally. Individualised guidance accelerates progress safely. Strength and structured exercise improve both quality of life and mental well-being. If you’ve been thinking about starting a fitness journey, come and talk to us at Melbourne Massage and Treatment, Fitzroy North. For those who decide to commit to a change, a positive change, for their well-being, there are 5 or […]
Shoulder pain is one of those presentations that can stop you from enjoying your day. Rolling in bed becomes difficult; carrying shopping or even sitting there and doing nothing can be frustrating. At Melbourne Massage and Treatment, I got to see many clients who complained of shoulder pain for a variety of reasons. Although one thing that is common with those different types of pain is the imbalance in the mobility stability joint chain, especially in people who do physical labour, repetitive overhead work, or intense gym training. Therefore, while many people expect me to focus only on the sore spot in the shoulder, my myotherapy approach is always broader and more thorough. Yes, I treat the shoulder as the primary concern, but effective, long-term relief comes from understanding why your shoulder is overloaded in the first place. That means looking beyond the glenohumeral joint and assessing thoracic mobility, scapular control, and thoraco-scapular stability, which are key components that are often overlooked but critical for shoulder health and to help you fix the shoulder pain. Why Shoulder Pain Often Persists The Shoulder is a joint characterised by a great amount of mobility and not much stability, which puts it at high risk of injury and so pain. When your shoulder hurts, it’s rarely because the shoulder itself is “weak” or “damaged” in isolation. Indeed, to arrive to the pain response, either you had a severe trauma, like a fall on the shoulder or more commonly, the shoulder is compensating for: Poor thoracic spine mobility Weak or poorly coordinated scapular stabilisers Faulty movement patterns under load Repetitive strain from work or training And let’s be clear, we are all different, so two individuals who do the exact same job or sport may end up having different pain and presentation due to basic anatomical differences in the shoulder. That said, here are some common presentations that can lead to shoulder pain: If the thoracic spine doesn’t move well, the shoulder is forced to work harder. If the scapula doesn’t stabilise properly, the ac joint gets overloaded Genetically, the space between bonds (Humerus and Acromioclavicle joint) is narrower than the norm My Clinical Assessment Process For Shoulder Pain When you come to my Myotherapy Clinic in Fitzroy North for shoulder pain, I don’t just ask where it hurts, but I would assess: Thoracic spine mobility (especially rotation and extension) Cervical movement in active and passive motion Scapular positioning and control Shoulder range of motion under load Training or work-related movement demands Previous injuries or recurring pain patterns This is particularly important if you: Work in trades or manual labour Train heavily in the gym or sport Perform repetitive overhead movements Have had recurring or long-term shoulder pain A tailored assessment, such as the above one, allows me to not only pinpoint why the shoulder is in pain and what further investigation may be needed to confirm the findings but also address these factors, allowing us to understand the underlying drivers of your pain. The Role of Thoracic Mobility in Shoulder Pain The thoracic spine (mid-back) plays a massive role in how your shoulder functions. This is because the thoracic section of the spine is the mobile portion that anticipates the stable scapula-thoracic joint in the mobility, stability chain. Limited thoracic mobility can lead to: Reduced the overhead range Increased strain on the rotator cuff Poor scapular mechanics Neck and shoulder tension As part of the myotherapy treatment protocol for shoulder pain, I often combine manual therapy, joint mobilisation, and movement-based rehab to restore thoracic movement.When the thoracic spine moves better, the shoulder doesn’t have to overwork, pain reduces, and then we can increase the strength by increasing the load. A classic example of the thoracic shoulder relation is a cricket player. The thoracic rotation along the throwing action is essential to optimise the force imprinted during the throwing action. In fact, imagine the thrower in a cricket game, using only the shoulder, and not rotating that thoracic joint chain. The shoulder load would be excessive, and in a short time, it would cause overload injury and so shoulder pain. Scapular Stability: The Missing Link Your scapula (shoulder blade) is the foundation for shoulder movement. Indeed, the scapula-thoracic joint is the stable joint between the thoracic and the glenohumeral mobile joints. But not only that, indeed, the scapula is the origin point of the rotator cuff muscles, a group of muscles that control the positioning of your humeral head in the glenoid fossa. If it lacks stability or control: The shoulder joint becomes vulnerable Tendons are placed under excessive stress Pain persists despite “strengthening” exercises As a Clinical Myotherapist, I focus on improving thoraco-scapular stability, ensuring the shoulder blade moves smoothly and supports the arm during load, lifting, and rotation. This is especially crucial for people involved in: Weightlifting Cross-training Construction or trade work Sports requiring throwing or overhead movement To strengthen the stability of the scapula, we then have to work on the rhomboid muscles and the trapezius (upper, mid, and lower), but even the levator scapulae. So yes, it is not a quick fix to restore shoulder functionality and remove shoulder pain, but there is a step-by-step journey that can be taken, and it is your choice to start walking along this path. I am here only to help you understand what the right path is for your presentation and ensure we take the right route. Hypermobility and Shoulder Pain One often overlooked factor in shoulder pain is hypermobility. Hypermobility means your joints move more than the norms which isn’t always a bad thing, but it significantly increases injury risk when stability is lacking, particularly in the shoulder. For hypermobile individuals: Ligaments provide less passive support Muscles must work harder to stabilise joints Poor scapular stability leads to shoulder overload When hypermobility exists alongside poor thoraco-scapular stability, shoulder pain becomes far more likely. In these cases, treatment isn’t about increasing flexibility; instead would be the opposite: Improving neuromuscular control Enhancing scapular […]
Here in Fitzroy North, at my Myotherapy Clinic and 1:1 fitness class studio, I get to work with a wide range of clients, and what I notice is that there is a lack of knowledge and awareness on how to deliver a Glutes Strengthening. And why I believe that a squat is important is simply because squatting is an action that we do so often throughout the day that we all should be good at it, and it is the best functional movement that allows you to reinforce the full body structure. Therefore, when I come across those presentations, I ensure to educate my patients about the basic mechanics of a squat, including mobility, stability, and glutes strengthing. Are You Looking Into Glutes Strengthening? Let’s Check Your Joint Mobility and Stability First In order to deliver effective training for your glutes, including delivering an efficient squat, you will look at: Adequate ankle mobility A well-coordinated hip hinge Stability in fee tarsals and knee joints Those are regular things I would look at during a myotherapy treatment and 1:1 fitness class in Fitzroy North, to improve glute activation, movement efficiency, and injury resilience. Ankle Mobility Exercise to Improve Squat Depth and Lower Limb Mechanics As discussed in greater depth in the mobility and stability blog, before we start looking at strength and start working on functional movement, like the squat, we want to ensure that the mobile joints are mobile enough to deliver the right mechanics. In fact, limited ankle mobility often results in compensatory strategies such as: Excessive forward trunk lean during squats Early heel lift Increased stress on the knees or lumbar spine Clinical Importance of Ankle Mobility Adequate ankle dorsiflexion allows improved tibial progression during squatting movements, enabling more effective hip and glute loading. Exercise: Knee-to-Wall Ankle Dorsiflexion Drill Position the foot flat on the ground, facing a wall Aim for a 10 cm distance between the big toes and the wall Maintain heel contact with the floor Drive the knee forward toward the wall under control Perform slow, controlled repetitions Your aim is to teach the wall with the kneem, with a big toe-wall distance of min. 10 to 12 cm Clinical application:This exercise is commonly prescribed in myotherapy sessions to improve squat mechanics, reduce compensatory loading, and support long-term joint health. Hip Hinge Drill for Posterior Chain Activation and Spinal Control The hip hinge is a fundamental movement pattern required for safe and effective loading of the gluteal muscles, but not only that, indeed, poor hip hinge mechanics often present as excessive lumbar flexion or extension during deadlift-based movements. Why Hip Hinge Mechanics Matter Efficient hip hinging can help with: Increases glute and hamstring activation Reduces lumbar spine strain Improves RDL and deadlift performance Exercise: Wall-Assisted Hip Hinge Drill Stand approximately 20–30 cm from a wall Push the hips posteriorly to make contact with the wall Maintain a neutral spine and rib position Return to standing using glute contraction (squeeze those glutes) Clinical focus:This drill is a key component of both rehabilitation and performance-based programming at Melbourne Massage and Treatment. It is also a fundamental movement pattern taught in my glute-focused fitness classes, ensuring clients build strength safely and efficiently. Stability Starts From Your Feet Foot stability is a crucial part of delivering a good squat, especially during a low-bar squat, when feet are flat on the ground. Imagine your feet unable to give a stable direction to whatever is above, like the ankle, knee and hip. This would lead to knee shaking during squatting, and once the squat load increases, the risk of injury rises. So for foot stability, we look at: Even weight distribution of your load along the plantar of the feet, not only on your toes or on the heel. All toes, grabbing the floor, throughout the squat performance Lower-bar squat, feet flat on the floor (be barefoot or use gambaletto type of shoes) and feet wider than hip, stand in slight external rotation High-bar squat, feet open wide as hip stand (so a narrow stand) and heel well elevated. In both my clinical work and my strength-based fitness classes, foot stability is always assessed first. On the other hand, more about the high and low bar squat is available from this blog. Squats for Functional Glutes Strengthening In my glute-strengthening fitness class sessions, the squat is one of the primary movements we refine. Keep in mind that when we talk about squat for glut strength, we always refer to the lower-bar squat. Therefore, when performed with appropriate technique, this exercise is the most effective exercise for developing functional glutes strenghtening and improving lower-limb coordination. Below, you will find the most common Clinical Faults in Squatting Limited ankle mobility restricting depth Poor hip control resulting in lumbar compensation Reduced gluteus contribution due to motor control deficits So this is what you need to focus on to for a Optimal Glute Engagement while squatting: Maintain even foot pressure throughout the movement Maintain spinal alignment and controlled descent Drive upward through the heels and mid-foot Clinical note:Squat depth should be dictated by movement quality rather than arbitrary range targets. Romanian Deadlifts (RDLs) Another Glutes strengthening Exercise The Romanian deadlift, in comparison to the conventional deadlift, is a partial movement, where the load never touch the ground throughout the exercise (once it gets picked off the ground). This type of lift is ideal for exercising the posterior chain, particularly in the gluteal and hamstring musculature. Benefits of RDLs in Myotherapy and Strength Training Enhances glute and hamstring load tolerance Improves hip-dominant movement capacity Reduces injury risk through controlled eccentric loading RDL Execution Guidelines Maintain close bar or weight proximity to the body Initiate movement via hip hinge, not knee flexion Maintain spinal neutrality throughout the range Terminate the movement when pelvic control is lost Clinical relevance:RDLs are regularly integrated into rehabilitation and strength programs for clients with lower back pain or who are returning to lifting after injury. But are also ideal to build […]
Functional movement is all those types of movement that you may have been training at the gym, like a squat, but really, those movements are what we are designed to deliver daily. Per the squat, think about sitting. Now, if you are young and fit, you may not need a great deal of mobility to sit on a chair, but as we get older, if we don’t train to maintain this form of mobility, things can really get difficult, and the risk of injury would increase. That’s where Myotherapy can really help you to understand which joints need more work in terms of mobility, but also which muscle groups you need to train to keep your stability at doc, so that your functional movement, especially when done under load, is going to be safe and with less risk of injury. What Is Myotherapy? Myotherapy is a form of manual therapy that focuses on assessing, treating, and managing musculoskeletal pain and dysfunction. At Melbourne Massage and Treatment in Fitzroy North, I use techniques such as deep tissue massage, joint mobilisation, myofascial release, dry needling, and corrective exercise to restore normal movement and prevent pain from returning. What I love about being a Clinical Myotherapist is that when working with my clients, I have to deliver a tailored treatment plan, as everyone is different and everyone presents with a unique body, which may need a different approach to reach the same goal. All this, starting from joint mobility and stability. Why Joint Mobility and Stability Matter Let’s start by defining what mobility and stability are: Mobility: the ability to move through a full range of motion Stability: the control that keeps your joints aligned to the body plane and supported To move well under load and deliver safe exercises, you must have good mobility and stability where needed. For example, if your hips lack mobility, your lumbar spine might compensate, creating discomfort and increasing the injury. Furthermore, a lack of mobility, it means you can not fully engage your muscle fibres, as less movement means less contraction or elongation of the muscle fibres involved in that movement, so less power and less growth. On the other hand, lack of stability is given from your lumbar area, which is not able to support a heavy load, and that’s how you can hurt your back. How Myotherapy Enhances Functional Movement Here at my clinic in Fitzroy North, as a clinical myotherapist I focus on helping you restoring balance through a whole-body approach. Here’s how Myotherapy helps: Comprehensive Movement AssessmentLet’s start with assessing posture, joint range of motion, and functional movement patterns to identify restrictions or weaknesses. Addressing the Root Cause of PainPain is central nervous system response to something that doesn’t work at is best. It may be an injury, or it may be a sensitization of the area. As a clinical myotherapist I help you break the cycle of compensation and discomfort, allowing more efficient, pain-free movement. Improving Joint MobilityUsing targeted soft tissue therapy, myofascial release, and gentle joint mobilisation, we help reduce tightness and restore freedom of movement across affected joints and muscles. Building Joint StabilityOnce mobility is restored, we focus on improving control and strength. Personalised exercises activate stabilising muscles, enhancing balance and coordination to prevent re-injury. Long-Term Support and EducationAfter every appointment I ensure to leave a detailed PDF file with the exercises we look into, so that you are able to reproduce our work at home or at your gym. But for every question, and for your progressions, I am always here ready to help. Who Can Benefit From A Myotherapy Session? Myotherapy is suitable for people of all activity levels. At our Fitzroy North practice, I regularly help clients dealing with: Muscle tightness or restricted joint movement Neck, shoulder, or lower back pain Postural strain from office work Sports or exercise-related injuries Limited flexibility affecting daily performance The Takeaway on Myotherapy and Functional Movement To improve your functional movement starts working on the right balance between joint mobility and stability. Myotherapy offers a targeted, evidence-based way to achieve that balance, and I am here helping you move better, feel stronger, and prevent future injuries. If you’re ready to enhance your movement and reduce pain, book a Myotherapy session at Melbourne Massage and Treatment, Fitzroy North today. Let’s get your body moving the way it’s meant to. And if you have any question, please use the form below to reach me out:
Bone density is a key factor in bond fracture prevention. Bone is made of cells that die and regenerate. When this process is compromised, the risk of fracture arises. During the early stages of life, we can ensure that we intake and store calcium through food to build up our bones, but after a certain age (about 30), the body stops absorbing calcium, and the storage that we created is now our reserve for the rest of life. Cell Regeneration in Bone and Other Body’s Tissues The body’s cells, like muscle cells, skin cells, tendon cells, ligament cells and even bond cells, are in constant change via a process called cell regeneration. Old cells die off and they get replaced with new cells. In the case of bone, the cells that allow this process to happen are called osteoblasts. While we age, this process slows down, meaning that cells would still die, but they don’t get replaced. A typical example is a woman going through menopause. Estrogen, which is the hormone responsible for bond metabolism, allows the activity of osteoblasts. During menopause, indeed, women have a drop in Estrogen production, and osteoblasts are not as operative as they used to be. Strength Exercises and Cell Regeneration As this meta-analysis shows, strength exercises are a positive stress stimulus for the body and can help the osteoblast work harder and maintain bone cell regeneration. When the body perceives stress as physical resistance, it does its best to establish a reparation mechanism. So whenever we pick a weight against gravity, the body would implement a regeneration of the tissue that are used to complete this action. Who Is at Risk of Losing Bone Mass? There are several factors that can contribute to decreased bone mass: Age: Bone density typically peaks in early adulthood and declines with age. Gender: Women, especially postmenopausal, are at higher risk due to hormonal changes that accelerate bone loss. Family History: A family history of osteoporosis can increase risk. Body Size: Individuals with smaller body frames may have less bone mass to draw from as they age. Hormonal Levels: Thyroid imbalances and reduced sex hormones can lead to bone loss. Dietary Factors: Low calcium and vitamin D intake contribute to diminished bone density. Lifestyle Choices: A sedentary lifestyle, excessive alcohol consumption, and smoking are linked to weaker bones. I have included factors like dietary and hormonal levels in the above list. Bear in mind that taking supplements such as calcium and vitamin D (which helps retain calcium) could have severe contraindications. So, always talk to your doctor or specialist about the intake of supplements. How to determine Bone Density? To determine bone density, there is a diagnostic test called Dual-energy X-ray Absorptiometry (DEXA or DXA). This non-invasive procedure measures the mineral content in bones, usually in areas like the spine, hip, or wrist, to assess bone density and identify potential risks of osteoporosis or fractures. The results are given as a T-score, which compares your bone density to the average peak bone mass of a healthy young adult. A T-score of -1.0 or above is considered normal, while a score between -1.0 and -2.5 indicates low bone mass (osteopenia), and a score of -2.5 or lower suggests osteoporosis. Other methods, like ultrasound or quantitative computed tomography (QCT), can also assess bone density, but DEXA remains the gold standard for bone health evaluations. Mobility before strengthening So far, we have discussed how strength exercises are a good way to maintain bond density. Still, I would not recommend that anyone who is not into strength exercise and has bone density issues go and start lifting heavily. Why (?), you may ask. Well, before we start lifting heavy, we want to ensure that the body mechanics are optimal for it, so we better start looking into your mobility and then pass on to the strength part of things. Please be aware that mobility has nothing to do with elasticity or stretching. Those are different practices. How Can We Achieve Great Mobility For people who decide to take a journey to ensure an optimal level of mobility and then strengthen the body, the first step is to assess their joint mobility with active and passive range of motion. After that, we could use a combo of Myotherapy treatment and mobility exercises to ensure they can quickly pick up the best of their mobility capacity, given their subjective presentation. And here is a list of mobility exercises which we may look into at first: Hip Openers to improve range of motion in the pelvis and lower back. Ankle Drills to support proper weight distribution in weight-bearing exercises. Thoracic Spine Mobility Exercises to prevent excessive strain on the lower back. AC Joint External rotation to ensure we can build strong rotator cuff muscles, essential for shoulder health It Is Time To Strength. How Can We Do This? Once the minimum mobility is achieved, which may take 1 to 2 weeks of training, depending on each individual and their subjective history and effort, we can start looking into more strengthening exercises. So, here is a list of different exercises that can help with strengthening, written with the progressions to follow: Calf raises with double leg, single leg and weight Hamstring and Quads Curl that gets weight added as weeks go by Standing Adduction and Abduction at cable machine or with resistance bend Glut Muscles training at cable machine or with resistance bend Deadlift for back and posterior chain muscle strength Squat with weights and explosion variations Cuff rotator-specific strength is Ideal before stepping into more complex arm weight-lifting Cervical muscle strength to prevent cervical headache and sore neck All of those exercises, except the cervical one, can then be modified to achieve plyometric drills and combined movement. But this is a process that would take months, and there is no rush to get to it, as I want you to be safe throughout the entire journey. Integrating Exercise into Myotherapy Treatment At Melbourne Massage and Treatment, I incorporate […]
Whiplash is a common neck injury caused by a sudden and forceful back-and-forth motion of the head. We often see this in patients who go through a car accident, contact sports injuries (AFL, rugby or even Soccer), or falls. While whiplash is usually not life-threatening, we now know that it can cause persistent pain and discomfort, affecting daily activities. Therefore, it is important to understand its symptoms, causes, and the best exercises for recovery, which can help individuals manage and overcome this condition effectively. Common Causes of Whiplash Whiplash is a term used to describe a fast rocking motion of the cervical area and is most frequently caused by: Car accidents: Rear-end collisions are the leading cause, as the sudden force propels the head forward and backward. Sports injuries: Contact sports like football, boxing, or hockey but even AFL, Rugby or even Soccer increase the risk of whiplash injuries. Falls: Slipping and falling can cause the head to jerk suddenly, leading to whiplash. Physical assaults: Blows to the head or sudden jolts, such as those experienced in shaken baby syndrome, can result in whiplash. What are the consequences of Whiplash for the cervical ligaments? The consequences of whiplash for the cervical ligaments can be significant, leading to long-term instability and chronic pain. When the ligaments are overstretched or torn, they lose their ability to support the cervical spine, resulting in properly: Reduced Stability: Weakened ligaments can no longer provide adequate support to the cervical vertebrae, leading to excessive movement and an increased risk of further injury. That’s why stretching is not recommended either. Chronic Pain and Stiffness: Persistent discomfort may arise as the muscles attempt to compensate for the lack of ligament support. Increased Risk of Degeneration: Ligament damage can accelerate wear and tear on the cervical joints, potentially leading to conditions such as osteoarthritis. Neurological Symptoms: Instability in the cervical spine may irritate or compress nerves, leading to headaches, dizziness, or numbness in the arms. Symptoms of Whiplash Whiplash symptoms can range from mild discomfort to severe pain, and they often appear within hours or days of the injury. Common symptoms include: Neck pain and stiffness: One of the most prevalent symptoms, often worsening with movement. Headaches: Typically originating from the base of the skull and radiating toward the forehead. Shoulder and upper back pain: The impact can cause muscle strain in surrounding areas. Reduced range of motion: Difficulty moving the neck due to stiffness and discomfort. Dizziness and fatigue: A common reaction as the body copes with the injury. Tingling or numbness in the arms: Nerve involvement may lead to sensations of pins and needles. Cognitive issues: Some people experience memory problems, difficulty concentrating, and irritability. Those symptoms may not present all at once, and they can belong to other presentations, while whiplash did or didn’t happen anytime before. That’s why when we go through a clinical history taking, as Myotherapist, we take our time to dig into your past and your body habits, as this can give us important information about your current presentation and what we can do to improve it. Why Can Whiplash Become a Lifelong Issue? In some cases, whiplash can become a chronic condition due to the instability of cervical ligaments. Cervical vertebrae can be divided into two parts, Mobile and Stable joints. C1 to C2 are the mobile ones, whereas C3 to C7 are the stable ones. Now, if along a whiplash incident, the ligaments of either the mobile or, most luckily, the stable side get strained, the muscles surrounding that segment of the joint would have to work harder to maintain stability. This would lead to to ongoing discomfort, reduced mobility due to pain and muscle spasms, and increased vulnerability to future injuries. If left untreated or managed improperly, this is how the condition can become chronic and lead to other injuries along the way. Importance of Thoracic Mobility Thoracic mobility plays a crucial role in preventing the chain effect of mobility and stability issues between the thoracic spine, lower cervical, and upper cervical regions. If the thoracic spine is stiff or restricted, the lower and upper cervical spine must compensate, leading to increased strain and pain. Improving thoracic mobility through targeted exercises can help reduce this compensatory stress, allowing for better neck function and reducing the risk of chronic discomfort. In a case of a previous history of whiplash, maintaining good thoracic mobility would allow the cervical area to focus on its duties, so stability for the lower portion and mobility for the upper. Reducing the risk of overcompensation and muscle fatigue. Effective Exercises for Whiplash Recovery A structured exercise program is essential for whiplash recovery. This program should begin with isometric exercises to restore basic cervical movement, progress to concentric exercises to rebuild strength, and eventually include thoracic mobility drills to enhance overall spinal function. Phase 1: Isometric Exercises for Early Recovery. For the first 2 weeks post-injury, 5 to 7 days a week. Isometric exercises help activate muscles without excessive movement, providing a stable foundation for recovery. This step is essential to start driving more blood to the area irritated by the whiplash and also allow the central nervous system to feel confident in perceiving the cervical structure moving without pain. Isometric Neck Holds: Place your hand on your forehead and gently press against it without moving your head. Push only 25% of your strength, as it has to be a pain-free exercise. Hold for 5-10 seconds and repeat 5 times. These exercises can be done in any cervical movement, such as extension, lateral flexion, or rotation, by using your hand as a resistance and pushing always at 25% of your strength. The strenght of push does not ever progress, what you will progress within isometric exercises are the time fram of push, repetitions and sets. Phase 2: Concentric Strengthening Exercises. From week 3 post-injury onwards,3 to 5 times a week. Once the pain subsides, which we would expect to happen in 2 weeks about it, gradual […]
At Melbourne Massage and Treatment in Fitzroy North, we frequently encounter clients dealing with tennis elbow (lateral epicondylitis) and golfer’s elbow (medial epicondylitis). These conditions can cause significant discomfort and limit your ability to enjoy sports and everyday activities. While they are often associated with repetitive arm and wrist movements, it’s essential to consider how poor shoulder mobility and stability can contribute to these issues. What Are Tennis and Golfer’s Elbow? Tennis Elbow Tennis elbow affects the outer part of the elbow, causing pain and tenderness on the outside. This condition typically arises from overuse of the forearm muscles, especially those responsible for wrist extension. Activities such as painting, or even prolonged computer use, or overstreching of extensor muscles can trigger this condition. Golfer’s Elbow Conversely, a golfer’s elbow affects the inner part of the elbow, leading to pain on the inside. This condition is commonly associated with activities that require gripping, flexing the wrist, or repetitive forearm movements, such as golfing, throwing, or lifting. In this presentation is the common flexor tendon that get’s irritated, and refer with pain. The Connection to Shoulder Mobility and Stability While tennis and golfer’s elbow are localized conditions, they often stem from dysfunctions higher up in the kinetic chain, particularly in the shoulder. Poor shoulder mobility and stability can lead to compensatory patterns that place undue stress on the forearm and elbow joints. Shoulder Mobility Limited shoulder mobility can restrict the natural range of motion for various activities. For instance, if your shoulders lack mobility, you may overcompensate with your forearm muscles during tasks that require reaching, lifting, or throwing. This overcompensation can lead to strain, resulting in conditions like tennis or golfer’s elbow. To maintain proper shoulder mobility, you want to ensure the use of the glenohumeral joint along your exercises and move it with specific drills, as this would stimulate the joint synovial fluid and maintain the joint lubricated. On the other hand, if the joint is hypermobile, we should look into how to stabilize it better. Shoulder Stability Shoulder stability is crucial for maintaining proper alignment during movement. Weakness in the shoulder stabilizers can cause the shoulder joint to become unstable, leading to altered movement patterns. When the shoulder isn’t stable, the body often compensates by engaging the forearm and elbow excessively, increasing the risk of injury. As mentioned in the paragraph above, this is what would occur when someone presents with a hypermobility body. In the hypermobility presentation, the ligaments are more lax and don’t hold back the joint movement as expected. Assessing and Addressing the Issue At Melbourne Massage and Treatment, we recommend a comprehensive approach to address tennis and golfer’s elbow effectively: Assessment of elbow epicondylitis Understanding the root cause of your pain is vital. During an initial consultation, we still mainly focused on your elbow presentation and addressed what movement reproduced the discomfort. But not only that. Throughout a tailored investigation, we will address what could be the root cause of the problem. This way, it would be easier to develop a tailored treatment plan. Treatment for elbow epicondylitis Massage Therapy: Targeted massage can alleviate tension in the forearm and improve blood flow, promoting healing. MDN: Myofascial Dry Needling plays a really effective role in tendinitis management. It focuses on targeting the underactive muscles, restoring the neural connection between the central nervous system and muscle, and desensitizing the painful area. Mobilisation: Mobilisation is an ideal technique to address mobility issue, and improve the range of motion of a joint. For epicondylitis presentations, the mobilisation could focus on wrist, elbow or shoulder. This would be based on the finding along the assessment. Strengthening Exercises: In the exercise program, we will initially focus on exercises that can desitentize the elbow area, such as isometric holds, and then move to eccentric and concentric exercises. In this second step, we would already focus on specific shoulder mobility or stability exercises, as needed. Education Understanding proper biomechanics can empower you to make lifestyle changes that prevent future injuries. Giovanni will guide you through exercises and techniques to maintain shoulder health and prevent elbow pain. Conclusion Tennis and golfer’s elbow can be debilitating, but addressing shoulder mobility and stability is key to recovery and prevention. At Melbourne Massage and Treatment in Fitzroy North, Giovanni is dedicated to helping you achieve optimal function and well-being. If you’re experiencing symptoms of tennis or golfer’s elbow, don’t hesitate to contact Giovanni or Book Now your 15-minute free phone consultation to learn more about a personalized assessment and treatment plan. Together, we can work towards getting you back to the activities you love, pain-free. FAQ Q: What are tennis elbow and golfer’s elbow? A: Lateral epicondylitis, affects the outer part of the elbow, causing pain due to overuse of the forearm muscles, particularly those responsible for wrist extension. Common activities that can trigger it include painting and prolonged computer use. Medial epicondylitis, impacts the inner part of the elbow, leading to pain often associated with gripping, flexing the wrist, or repetitive movements like golfing or throwing. Q: How are shoulder mobility and stability related to these conditions? A: Poor shoulder mobility can lead to overcompensation by the forearm muscles during activities requiring reaching, lifting, or throwing. Similarly, weak shoulder stabilizers can cause the shoulder joint to become unstable, forcing the forearm and elbow to work harder, which increases the risk of injury. Both factors contribute to the development of tennis and golfer’s elbow. Q: What are the signs of limited shoulder mobility? A: Signs include restricted movement during overhead activities, difficulty reaching behind your back, and discomfort during routine tasks that involve lifting or throwing. These limitations can lead to compensatory movements that stress the elbow. Q: How do you assess tennis or golfer’s elbow at Melbourne Massage and Treatment? A: We conduct a thorough assessment that focuses on your elbow presentation, identifying movements that reproduce discomfort. This investigation also explores potential underlying issues related to shoulder mobility and stability, helping us understand the root […]
- 1
- 2