Cosmetic surgeries have become increasingly common, with procedures such as liposuction, tummy tucks, facelifts, and breast augmentations helping people achieve their desired aesthetic goals. However, while the surgical aspect gets most of the attention, what often goes under-discussed is the importance of post-operative care, especially Manual Lymphatic Drainage (MLD) in promoting faster, smoother recovery and reducing the risk of ending with fibrosis tissue build up underneath the skin. What Is Manual Lymphatic Drainage (MLD)? MLD is a gentle, rhythmic massage technique designed to stimulate the lymphatic system and encourage the natural drainage of lymph fluid. The lymphatic system plays a crucial role in immune function and fluid balance. After cosmetic surgery, lymphatic flow can become disrupted due to inflammation, surgical trauma, or temporary damage to lymph vessels. While the first few days post-surgery are dedicated to acute recovery and the taking of Antibiotic to reduce the risk of infection post-surgery, as soon as this risk is passed, that’s when you want to start your MLD journey. Why Is MLD Important After Cosmetic Procedures? Cosmetic surgeries often cause swelling, bruising, and fluid accumulation (known as seroma or edema). This is due to the body reacting to an invasive procedure and removing tissue beneath the skin. MLD helps: ✅ Reduce post-surgical swelling ✅ Accelerate the removal of metabolic waste and excess fluid ✅ Improve skin texture and reduce fibrosis (hardened tissue) ✅ Speed up visible results by enhancing contour definition ✅ Decrease discomfort by reducing pressure from trapped fluids As with any surgery, when lymphatic drainage massage is applied, no pain is to be experienced. While I treat someone with MLD I always pass this information up front, to ensure that if they experience any type of pain, I get told about it, so that I can go lighter with pressure. Which Procedures Benefit Most from Lymphatic Drainage? MLD is commonly recommended after: Liposuction (including 360 lipo or Brazilian Butt Lift – BBL) Tummy tucks (abdominoplasty) Facial surgeries (rhinoplasty, facelifts, blepharoplasty) Breast augmentation or reduction Body contouring procedures As a Lymphoedema therapist, I do get surgeons referring me patients to assist them with post-op management, especially when swelling or fibrosis is a concern. When Should You Start Lymphatic Drainage? As briefly explained above, the ideal time to begin MLD is as soon as you stop your antibiotic cycle, and is your surgeon or GP call to when you are safe to do so. On the other hand: Typically, MLD is started 3 to 5 days post-surgery, once acute inflammation has settled and the incision sites are closed or protected. A full course may include 6–10 sessions spaced out over a few weeks for optimal results. Always follow the advise of the surgeon about post surgery, but, when you safe to do, the more movement we add to Lymphatic Draiange, the better the recovery would go. Is MLD Safe post-cosmetic surgery? When performed by a qualified lymphatic therapist, lymphatic drainage is non-invasive, safe, and effective. It’s gentle enough for delicate post-op tissue and can significantly improve comfort and healing time. My qualification in Lymphatic Drainage was done with the Vodder Academy whicg holds the gold standards for MLD practice, and is worldwide well known for the quality of their practice. On the other hand, I also hold a qualification in Clinical Myotherapy, which allows me to help people recover from injury and stick to their fitness goals via training and exercises. When Can I Book My Appointment for Post-Cosmetic Surgery Recovery? My studio, Melbourne Massage and Treatment, is located in Fitzroy North, on the corner of St George Rd and Holden St. I work Monday to Saturday, and to book an appointment, you can just head online to the booking page and choose the best time/days that work for you. Given the number of session needed for this type of work, I always suggest to book a series of session in a raw, from to 3 session per week for the first 2 weeks. Session by session we do evaluate together the progress, and chose together what’s the next step. If you have any questions, please do not hesitate to contact me. FAQs – Cosmetic Surgery & Lymphatic Drainage
Tag Archives: massage
Temporomandibular Joint (TMJ) disorders are a common source of jaw pain, clicking, and discomfort that can impact anyone at any age. At Melbourne Massage and Treatment in Fitzroy North, I see many clients presenting with TMJ clicking and associated symptoms. One of the key factors behind the painful symptoms is retrodiscal tissue compression, a condition that not only causes joint noises but may also lead to chronic jaw pain. What Causes TMJ Clicking? Let’s start understanding why TMJ clicks. When looking at the TMJ, we can see that between the two bones that make up the joint, there is a disk, called the articular disc, which is made of cartilage and is meant to keep the bones apart (the temporal bone and the mandibular condyle). In a healthy joint, the disc moves smoothly with the jaw during opening and closing. But when the disc is out of alignment, the condyle may snap over it, creating that characteristic “click.” For reference, a condyle is a rounded protuberance at the end of a bone, which in this case, fits into a cavity. The Role of Retrodiscal Tissue Compression in TMJ Clicking and Pain Right behind the disc lies a tissue known as the retrodiscal tissue, which contains blood vessels, nerves, and connective tissue. When the disc is displaced anteriorly, the condyle may compress this sensitive area during jaw movements. This compression can lead to: Inflammation Persistent pain Increased joint stiffness Neurovascular irritation This is possible because the tissue, as mentioned earlier, is innervated, where the disk, is not. Therefor, the disk compression on its own, is not going to replicate any pain, as there is no nerve to pick up any stimulus in there. Forward Head Posture Would Not Help. Forward head posture is a common presentation linked to TMJ clicking. Forward head posture is characterised by the head sitting forwards compared to the midline of the body, and is often due to a lack of strength in deeper neck flexor muscles. This presentation can make the TMJ presentation worse because of the excessive load placed on the muscle that surround the TMJ (masseter and temporalis muscles). Other reasons include the misalignment of the teeth, which can make the chewing action more difficult and over time, create strain along the TMJ tissues (muscles, ligaments and tendons), but also referral pain from the cervical joint tension can lead to manifest stress in the jaw and face muscle due to constant pain and disconfort. How Myotherapy Can Help At Melbourne Massage and Treatment, I offer a combination of evidence-based manual techniques and exercise therapy to address the root causes of TMJ dysfunction, aiming not just to manage symptoms but to promote long-term recovery. 1. Joint Mobilisation Gentle mobilisation techniques to the jaw, cervical spine, and upper neck can reduce joint restriction, improve mobility, and relieve the pressure on retrodiscal tissue. Mobilisation helps restore normal disc-condyle mechanics, reducing clicking and improving range of motion. 2. Dry Needling Dry needling of trigger points in the masseter, temporalis, and lateral pterygoid muscles can reduce hypertonicity and relieve pain referred to the jaw and head. Targeting myofascial restrictions can also indirectly reduce stress on the TMJ itself. 3. Targeted Exercise Therapy Specific exercises for jaw control and cervical strength are crucial for maintaining results between sessions. Jaw isometric exercises are ideal for pain management and quick relief. Resistance bend exercises for jaw opening. Relaxation techniques for parafunctional habits like clenching Over time, these exercises can enhance joint stability, reduce overloading, and in some cases improve mild degenerative changes by promoting better joint mechanics and tissue resilience. 4. Deep Tissue Massage Massaging the muscles surrounding TMJ and the cervical muscles can help reduce tension, stimulate the nervous system to relax and give a break from pain and discomfort, while improving mobility. As always, there is not one solution for the common presentation of many. Each individual is different, and the treatment results can be different. But what we can expect is that, if we balance the usage of hands-on treatment and exercises, we can create some real change with some great benefits. TMJ Clicking and Menopause Menopause is a topic I have already spoken about in my blogs. Briefly, we can refer to menopause as the day past 12 months of missing menstrual periods in a woman’s life cycle. Before that is called perimenopause, after that day, we talk about post-menopause. This step is achieved when a woman has no more eggs to release, and her menstruation has stopped. While it is not the same journey for each woman and there are many changes that women can go through, a common one is stiffness of ligaments. Again, this is not happening in one day, but is a change that comes with time and is different person to person. This is possible because of the lack of estrogen. Indeed, estrogen, along with controlling many other aspects of the biological life of a woman, is also responsible for the elasticity of the ligament. Put: less estrogen, less elasticity. This can explain why, during this phase, women start experiencing more TMJ pain and potentially TMJ clicking. On the other hand, we have no yet enough evidence to say that Hormonal Replacement Therapy is effective for establishing this presentation (Robinson et al., 2019). FAQ – TMJ Clicking 1. What causes the clicking sound in the TMJ?The clicking occurs when the articular disc in the jaw joint becomes displaced, and the mandibular condyle snaps over it during jaw movement. This is often due to disc misalignment. 2. Why does retrodiscal tissue compression cause TMJ pain?The retrodiscal tissue contains nerves and blood vessels. When compressed due to disc displacement, it can lead to inflammation, pain, and stiffness in the TMJ area. 3. Can TMJ clicking happen without pain?Yes. If the articular disc is displaced but the retrodiscal tissue isn’t compressed or irritated, the joint may click without producing pain. 4. How does forward head posture affect TMJ?Forward head posture strains neck muscles and can […]
Bone fractures are a common injury, but with proper care and rehabilitation, bones can heal and regain strength. Strength exercise is a crucial component of this healing process, aiding in bone regeneration and restoring mobility and function. How can a bone fracture? Bones can fracture when placed under a load or force that they can’t tolerate. The load tolerance is subjective, person to person, and can vary based on the individual medical presentation and clinical history. Age it is only a circumstance that at the current moment in our society is seen as an increase the chance of fracture, but if we learn to age by keeping our feet via strength training, age would not be anylonger a risk component. Indeed, during the aging process, the bone can become weaker if not stimulate to positive stress, such as load active loads. The less load they received, the less the bone would keep regenerating, due to a slower metabolism. Therefor, as explained in other blogs, strength training is a key to longevity and better health. How can bone fractures heal? When a bone fractures, the body initiates a complex healing process involving several stages: Inflammation: Immediately after the fracture, blood clots form, initiating the healing process. Soft Callus Formation: Fibrocartilaginous tissue begins to bridge the fracture gap. Hard Callus Formation: The soft callus is replaced by a hard bony callus made of woven bone. Remodelling: The bone gradually remodels into its original shape and structure. This process can take several weeks to months, depending on factors like age, overall health, previous clinical history, medication intake and the severity of the fracture. Even thought there is nothing that can speed up the recovery, as this is a body natural process, there are things that can be done to assist the recovery and ensure that the healing happens as smooth as possible. Exercises is one of those factors, which are part of the healing journey, but have to be incorporated under supervision, to ensure not to aggravate the presentation. The Role of Exercise in Bone Regeneration As mentioned above, and in other blog exercises, specifically strengthening exercises, are a positive load for the body tissues, including bone, which can help stimulate the regeneration of those tissues. Obviously, different phases of healing require and can accept different types of strength exercises. So yes, you would not start with a single-leg jump on a broken tibia Stimulates Bone Formation: Mechanical stress from exercise promotes osteoblast activity, leading to new bone formation. Enhances Strength and Flexibility: Regular movement prevents joint stiffness and muscle atrophy; Improves Balance and Coordination: Reducing the risk of future falls and fractures. A systematic review by Kuijlaars et al. (2019) highlighted that physical therapy exercises, whether home-based or supervised, significantly improve functional mobility and strength post-fracture. Recommended Exercises for Recovery At Melbourne Massage and Treatment, I offer assistance with bone fracture recovery exercises throughout the Myotherapy and Fitness class treatment plan. What I would focus on, too, when aiming for recovery, would be: Weight-Bearing Exercises: Including walking or gentle jogging (if we are talking about lower limb injury), to stimulate bone growth; Resistance Training: Using bands or light weights to strengthen muscles supporting the bone, or the joint to which the bone is attached. Flexibility and Balance Exercises: Again, using weights and machinery, we aim to strengthen the muscles that control your overall equilibrium and stability to prevent further falls and reduce the risk of injury; Plyometrics which is most often towards the end of a recovery process from anytype of injury, where we focus on motion that are more close to return to daily activity, and we load your tendon as springs, as per can be doing jumping on the spot or repetitive explosive motions with arms. Clinical Evidence Supporting Exercise in Recovery from Bone Fractures Research, as already mentioned in the Kuijlaars et al. (2019) systematic review, shows the benefits of incorporating exercise into fracture rehabilitation, and below we look into more details about what exercises have to offer in terms of recovery: Improved Healing Rates: Patients engaging in structured physical therapy often experience more robust bone healing (Song, 2022). Reduced Complications: Regular movement decreases the risk of complications like deep vein thrombosis or joint stiffness (Ruan et al., 2023). Enhanced Quality of Life: Maintaining physical activity levels improves overall well-being and independence (Mahindru et al., 2023). What to consider when doing exercises post-bone fractures. While exercise is beneficial, it is always important to approach the recovery process with care: Follow Medical Advice: Always adhere to the guidelines provided by healthcare professionals. Avoid Overexertion: Pushing too hard can hinder healing or cause re-injury. Going hard or going home is not how recovery works. Monitor Pain Levels: Some discomfort is normal, but sharp or persistent pain should be addressed immediately. Pain-wise, on a scale of 0 to 10, we usually aim to get you to experience a comfortable discomfort, based on your worst pain experienced as max treshold. Recovery from an injury, including bone fracture, is a personal journey, and therefore is unique to everyone how quick it can be and what are the consideration to take in place during the exercises recocery. FAQs – Bone Fractures Recovery and Strength Training 1. How do bones fracture?Bones can fracture when exposed to forces they cannot tolerate. This tolerance varies from person to person, depending on factors like health history, bone density, and physical condition. While age is often seen as a risk factor, it’s more about reduced activity levels. With consistent strength training, the risk of fractures can be lowered significantly, regardless of age. 2. How does a fractured bone heal?Bone healing occurs in four key stages: Inflammation: Blood clots form to protect and initiate healing. Soft Callus Formation: Fibrous tissue bridges the fracture. Hard Callus Formation: New bone begins forming. Remodelling: The bone reshapes to its original form.This process varies in duration based on the severity of the fracture and individual health factors. 3. Can exercise speed up bone healing?While […]
As a Clinical Myotherapist, I often work with patients who perform back squats as part of their exercise routine, and at the question: “What’s your goal with a back squat?” the answer is often vague and not specific to what this exercise is for. The reason why the answer is not specific, is simply because they don’t know what’s the difference between high and lower bar squat, and don’t know that the back squat, as long as it is an amazing functional movement, it doesn’t train at the same level all the lower body muscles. That’s where, to prevent injury, to perform better squats, and to strengthen more evenly all the lower body muscles, I would suggest them to do exercises like: Quods curl, Hamstirng Curl, Cable Machine Adduction and Diagonal Extension (Glut Medius). Back Squat: The Foundation of Strength The back squat is such a great form of exercise because it does train multiple joints and multiple muscles all at once, but also it does allow us to use our innate capacity of squatting, which is a functional movement, to move high loads, therefore achieving more strength gains. However, this leaves us with more responsibility to train smartly. So let’s start to break down the two main different types of back squat: High-Bar Back Squat (Upper Bar Position) The bar rests on the upper traps The torso remains more upright Greater emphasis on the quadriceps muscles Ideal if your goal is quad strength and knee-dominant movement patterns The fact that the bar is sitting on the upper traps, and that the torso sits straighter, would lead to a descending movement where your thigh would reach a parallel degree with the floor, and from there you will stand back up. This is how you put more force throughout the quads. Indeed, the combination of a higher bar, straighter torso, and reduced descending position allows the weight to sit in the middle of the centre of gravity, which is placed more posteriorly compared to a lower-bar back squat. Low-Bar Back Squat (Lower Bar Position) Bar rests lower on the rear deltoids Torso leans forward slightly more Greater load on the glutes and posterior chain Favoured by powerlifters Best for developing hip strength and glute activation On the other hand, the lower-bar back squat, as anticipated, is more for the posterior chain muscles, like the gluteus max. This is possible because the bending forward of the trunk stretches more muscle fibres in their origin point (the posterior aspect of the ilium (the pelvic bone), the sacrum, and the coccyx), allowing more fibre contraction in the ascending movement. Also, the lower position of the bar and the bending of the torso maintain the weight in the middle of the centre of mass, which is pushed forward at this time. How about if I cannot squat deep? The depth of a squat is the distance that you can cover from a standing position to the lowest point you can reach. How deep you can squat, it would definetely change what muscle group you can activate, but, not everyone can squat deep, and that’s absolutely ok. Each of us has biomechanics that are different, due to differences in how the skeleton is shaped. Without going into many details in this blog, we can definitely say that those who have a longer femur would have a harder time going for a deep squat, compared to those who have a shorter femur. The femur’s length is compared to that of the torso. But this is not all, indeed, there are also other femur and hip characteristics that can limit how deep you can squat, such as anteverted or retroverted femur head. Accessory Work for a Complete Lower Leg Program So, knowing when and why to use each back squat variation can help tailor your program toward specific goals or help rehab muscle imbalances through focused intent. No squat is right, no squat is wrong; it is all about your goal. However, we need to add work more specifically with other exercises for strength symmetry, muscle activation, and injury prevention. Quad Curl (Leg Extension) Isolates the quadriceps Improves knee tracking and squat depth Essential in rehab for knee pain or quad weakness Quads curl can be done in many ways, with a cable machine or on a bench with quads curl attachment, but even with kettlebell or resistance bend. It all depends on your setup. As per all the exercise, be consistent with your set up and progressions. What I prefer most for my training, and what I offer to my patient during the fitness class, is to do quad curls on a bench with the attachment for quad curls. The advantages of this set-up are: Confort Easy progressions Easy set-up Inclination of the back at about 45° to 65° and slight elevation of the quads. The last point is essential to ensure we engage both ends of the quadriceps femoris, which is one of the four quads, that crosses both the hip and knee joints. Hamstring Curl Focuses on the hamstrings, which during a squat are often undertrained Strengthens the back of the thigh and supports knee stability A must-have for runners and athletes prone to hamstring strains As per the quad curl, even the hamstring curl can be done with different variations; there is never one way to train those muscles, but again, it is all about the efficiency and the amount of load that we can put through the muscle, which makes a difference. And again, what I can offer at Melbourne Massage and Treatment, in Fitzroy North, is to do these exercises on a bench, using this time a lower inclination for the upper body (which is now in a prone position) so that the origin of the hamstring is put under greater load, allowing more movement and greater load. Cable Glute Medius Diagonal Extension Targets the glute medius, a key hip stabiliser Performed by extending the leg diagonally behind and outward Crucial […]
Pregnancy brings many wonderful changes, but it can also bring some discomforts, especially as the body adapts to the growing baby. Common complaints include swelling, water retention, and aching joints. An effective and non-invasive treatment for these issues is lymphatic drainage massage (MLD), which can offer relief, promote wellness, and help pregnant individuals feel their best. In this blog, we’ll explore the safety, benefits, and potential contraindications of lymphatic drainage massage during pregnancy, as well as how this therapy can be customised to suit each individual’s needs. The Benefits of Lymphatic Drainage Massage During Pregnancy Lymphatic drainage massage focus in boosting the work of the lymphatic system. By increasing the functionality of this body system, we promote the flow of lymph liquids and help the body to move unwanted substances, as well as reduce fluid retention. This type of massage has been shown to have specific benefits for pregnant individuals (Cataldo Oportus et al., 2013), particularly when it comes to managing swelling and improving overall circulation. The benefits of include: Reduction of Swelling (Oedema): One of the most common pregnancy-related discomforts is swelling in the feet, ankles, and legs. Lymphatic drainage helps to enhance the flow of lymph, which can reduce fluid buildup in the tissues and alleviate discomfort caused by oedema. Relief from Pregnancy-Related Back Pain: Lymphatic drainage massage can reduce tension in the back and promote better posture, helping to relieve pain caused by the increased weight and pressure on the spine during pregnancy. In this case, the treatment is delivered in a side position. Improved Circulation: Pregnancy can lead to changes in blood flow and circulation. Lymphatic drainage promotes circulation and can improve oxygen and nutrient delivery to both the mother and baby. Mental and Emotional Wellbeing: Lymphatic drainage massage is extremely relaxing, and this positive side effect of the treatment can help you in having a better sleep which obviously can overcome stress and body ache. Per standard and comfort, at Melbourne Massage and Treatment, I tend to deliver lymphatic drainage massage in a seated position for pregnant women. This is possible thanks to the reclined hydraulic table, which can be converted from a flat table into a comfortable and big chair. How Compression Stockings Can Help Reduce Swelling Another effective way to manage swelling during pregnancy is the use of compression stockings. I recommend and provide to my patient stockings from Sigvaris, which is one of the world’s leading stocking manufacturers. The idea of using stocking, is to maintain pressure and liquid moving along the day, while sitting or walking, or doing your daily activities. How the stocking works is by adding a constant compression, which still leave you with a comfortable feeling and does help in pushing the liquid towards the upper body, reducing the chances of fluid accumulation in the lower limbs. For pregnancy, the grade recommended is grade 2, which is a clinical grade stocking. Consider that grade 3 is what is recommended for presentation like Lymphoedema. In terms of measurements, I can easily take mesuraments on site for the best fitting compression, and have the leggings with in 2 to 3 business days. For any enquire about the product or the services please do not hesistate to contact me now. What to Consider When Delivering a Massage During Pregnancy Now we are going to talk about what to consider when we deliver a massage to a pregnant patient, and as you will read, often light pressure is a must in this type of treatment, which gives lymphatic drainage massage an advantage compared to traditional relaxation pregnancy massage. So, there are certain areas of the body that we tend to avoid working on during a massage treatment for pregnancy, or where we may work on, but with a really light pressure and a full verbal or sometimes written consent. Here is a brief summary: 1. Abdominal Area: Deep or direct pressure on the abdominal area is a big NO. Instead, we can do gentle, light strokes if the patient is comfortable with it and they request it. Explicit consent here is a must. 2. Lower Back (Spine and Sacral Area): This is another big NO for heavy pressure. The reason lies behind the fact that strong pressure can lead to strain of the ligaments that hold the joints together, which, as the pregnancy progresses to a later stage, become more and more relaxed, allowing the birth to happen. So again, gentle massage techniques such as effleurage (long, sweeping strokes) or light kneading can be beneficial, but light touch. 3. Legs: Inner thighs another area where we avoid strong pressure, due to the presence of pressure points that could potentially stimulate uterine contractions if over-stimulated (e.g., peroneal or acupressure points). 4. Ankles and Feet: Ankles and feet, as there are acupressure points (like those related to the reproductive system) that may lead to unwanted effects if stimulated too forcefully. That said, a gentle foot massage can help relieve swelling and discomfort. 5. Hand and wrist The area of your hand, between thumb and index, and the pulsing point on the wrist, are other areas where massage is not recommended as it can cause contractions. Always remember that this is a brief summary, and everyone can react differently to the work received in that area. Therefore, there is no need to be scared of making contact with other people, and you should feel comfortable with your body. Trimesters and Positioning The position to be in during a massage, including lymphatic drainage massage, also depends on the trimester in which you are. First Trimester (0–12 Weeks): Lying on the back or side is generally fine during the first trimester, as long as the client is comfortable. A reclining position with support (e.g., pillows or bolsters) is often preferred for comfort. Lying prone (on the stomach) can be done during the first trimester if the client feels comfortable. However, lying flat on the stomach will become uncomfortable and impractical as pregnancy progresses. Second and Third […]
The Star Excursions Balance Test (SEBT) is a fabulous functional test that can tell us a lot about the mobility and stability of the ankle, knee, and hip joints. On top of being a functional test, the star excursion can also be used as an exercise, and via a series of progressions, which we will discuss in more detail later, can help you train for better running performance and injury prevention. Why is the Star Excursion Balance Test Important? The importance of Star Excursions Balance Test’s lying behind the fact that this test allows for testing with one motion the capacity of your ankle to stay stable on the surface of support (the floor) and how this stability is transmitted to the knee first and consequently to the hip. This is possible because the transfer of vertical pressure that is appllied to each joint while you are aiming to get the movement done. The movement required is to keep the feet of the anchor down to the floor, from the toes to the heel, while with the other foot, you aim to reach the furthest point away within the eight cardinal directions (like a star *). Along those movements, then, we also get observational data about your: Proprioception: The ability to sense the position of the body and its parts in space. Balance: The ability to control the body’s centre of mass over a stable base of support. Functional Movement: How well the body can perform multi-directional movements, such as stepping, reaching, and stabilising. So, if you are someone who has sustained lower limb injuries, particularly around the ankle, knee, or hip, these capabilities are often compromised. By using the Star Excursion Balance Test, we can assess any deficits in these areas, which might increase the risk of re-injury or limit recovery progress. But not only that. Indeed, that information will shape the recovery program, allowing us to understand better which muscle group or joint we need to focus more on with the exercises. That said, runners also benefit significantly from the SEBT. Running is a dynamic activity that places high demand on the lower extremities. Even minor imbalances or weaknesses can lead to issues like IT band syndrome, shin splints, and knee pain. The Star Excursion Balance Test helps in identifying these early warning signs before they evolve into more serious conditions. What Does the Star Excursion Test Measure? The primary purpose of the SEBT is to evaluate a person’s capacity to control body movement while standing on one leg. In fact, the test consists of reaching with one leg in multiple directions (anterior, posterior, medial, and lateral and a mix of those directions) while maintaining balance on the other leg. This shows their neuromuscular control and postural stability. It mimics the demands placed on the body during dynamic activities like running, cutting, and jumping. In rehabilitation, the Star Excursion Balance Test trains and improves: Ankle Stability and Control: It challenges the ankle to support the body’s weight while shifting through various planes of motion. Knee and Hip Joint Function: By demanding strength and flexibility in the lower limb, it helps retrain the kinetic chain, especially after joint injury. Balance and Proprioception: The test improves your ability to sense where your body is in space, which is essential for both preventing and recovering from injuries. Postural Awareness: Training balance also trains your ability to maintain proper posture, which can reduce stress on your joints and muscles during exercise. The Progression of the Star Excursion Test The beauty of the Star Excursion Test is its flexibility. It can be adapted based on the individual’s injury level, fitness, and goals. The test itself involves several variations, which I implement depending on the stage of recovery or the individual’s needs: Softer Ground: For those in the early stages of rehabilitation, we may perform the test on a softer surface, such as a foam pad or balance disc. This reduces the stability of the base and forces the individual to engage more stabilizing muscles, which aids in proprioceptive training and can be beneficial for rebuilding ankle and knee control. Weight on the Ankle: For those who have had ankle injuries, I often modify the test to place more weight on the injured ankle. This helps rebuild strength and functional control, as it forces the injured area to bear load and engage in movement patterns that may have been avoided during the healing phase. Eyes Closed: To increase the challenge, I sometimes ask my clients to perform the test with their eyes closed. This removes visual input, forcing the body to rely more on internal feedback (proprioception). This is especially important in the latter stages of rehabilitation, as it helps to refine neuromuscular control and reduce reliance on external cues. Using the Star Excursion Test with Lower Limb Injury Recovery and Runners The SEBT is a functional test that I like to use, with all its variations, to assess the progress of patient recovery. Either that you present with an injury, or either that you want to improve your form and body functionality through out exercises, the SEBT allows us to look in depth in what we need to work on too. For example, after a sprained ankle, I’ll often use the SEBT to check whether an individual is able to move without compensation, ensuring that their body has regained sufficient control and strength before returning to activities like running or sports. And this, don’t be surprised, is something that I do and has to be done whenever someone presents with complaints about knee or hip pain too. Again, an unstable ankle would transmit that instability up the chain. On the other hands for runners, the test helps evaluate areas of weakness that might predispose them to injuries such as Achilles tendinopathy, patellofemoral pain, or iliotibial band syndrome. Since running places repetitive stress on the lower limbs, identifying and addressing weaknesses early can prevent long-term problems and improve overall performance. Myotherapy and SEBT […]
Muscle tension headache and migraine are two different types of presentation that have in common a pain, which can also be debilitating, in the head area. Back in 2019, in Australia, 3 million people were estimated to suffer from migraine (Wijeratne et al., 2023), where, define how many people are suffering from muscular tension head-ache is a bit more tricky, as is not a presentation that can be easily tracked, due to self managed protocols, and other miss data counting. That said, they have different origins, symptoms, and treatment options. In this blog post, we will explore the key differences between muscle tension headaches and migraines, helping you understand how to identify and manage them. What Are Muscle Tension Headaches? Muscle tension headaches, or tension-type headaches, are the most common. This type of headache originates from cervical or facial muscle tensions, which recreates a pattern of pain on the head of facial area. As with all muscles, but even joints, the pain that we can experience can be local or in an area around the tense spot. These headaches are often linked to stress, lack of good posture, anxiety, and even sleep disturbances. They can be chronic or occasional, but compared to migraine, they lack neurological symptoms. Symptoms of Muscle Tension Headaches: Dull, aching pain or pressure around the head, especially in the forehead, temples, and back of the head. A sensation of tightness or “band-like” pressure around the head. Mild to moderate intensity (usually not as severe as a migraine). Pain can last from 30 minutes to several hours, sometimes even days. Tenderness or tightness in the neck, shoulders, and scalp. Causes of Muscle Tension Headaches: Stress: Emotional and mental stress is one of the primary causes of muscle tension in the neck and scalp muscles. Lack of good posture: Sitting or standing with poor posture and lack of strength in the musculoskeletal system, especially for long work, can strain muscles and trigger headaches. Sleep issues: Sleep deprivation or poor-quality sleep can exacerbate muscle tension and lead to headaches. The body recovers from the fatigue of the day before during sleep, especially in the early morning hours. Sleep deprivation would increase the chance of a headache. Dehydration: Not drinking enough water can lead to tension and headache symptoms. The body withdraws water from the brain to keep the organ functioning, causing physical brain shrinkage, which leads to headaches. Recent studies have indicated that chronic tension-type headaches (CTTH) are often exacerbated by environmental stressors, and poor posture in daily activities can cause muscle imbalance and contribute to the frequency of these headaches (Bendtsen et al., 2018; Grazzi et al., 2016). Treatment Options: Pain relief: Over-the-counter pain relievers, like ibuprofen or acetaminophen, can help ease the discomfort. Heat pack: Applying a warm compress to the neck and shoulders can help relax tense muscles. Keep always in mind that heat application should be limited to 10-15 minutes, once or twice a day. Massage: Gentle massage of the neck and shoulder muscles can reduce tightness and alleviate headache symptoms. Stress management: Practising relaxation techniques such as deep breathing, thai yoga, and meditation can reduce stress and prevent muscle tension headaches. Strengthen muscles: Strengthening the muscles around your cervical and shoulder area can help reduce the chance of suffering a headache by reducing the inflammatory response that the muscle would activate due to a lack of strength. What Are Migraines? As I mentioned above, the significant difference between headaches and migraines is due to neurological symptoms, a unique characteristic of migraines. Migraines are neurological events that involve complex brain activity. They are characterised by intense, throbbing pain, usually on one side of the head. They are often accompanied by other symptoms such as nausea, vomiting, and sensitivity to light and sound. Migraines are more debilitating than muscle tension headaches and can last a few hours to several days. The intensity of the headache doesn’t have to be severe. Symptoms of Migraines: Although many people experience nausea, vomiting, and light sensitivity, migraine symptoms can vary, with some individuals experiencing dizziness or visual disturbances without significant head pain. Throbbing or pulsing pain, usually on one side of the head. Nausea and vomiting. Sensitivity to light, sound, and sometimes smells (aura). Visual disturbances such as flashing lights or blind spots (this is known as an aura, which can occur before or during the headache). Dizziness or feeling lightheaded. Migraines are understood to be primarily driven by neurovascular changes and neuronal hyperexcitability (Feng et al., 2021). A review by Wagner et al. (2021) found that the pathophysiology of migraines involves alterations in neurotransmitter systems, notably serotonin and CGRP (calcitonin gene-related peptide), which contribute to the vasodilation and pain signaling pathways. Causes of Migraines: Genetics: Migraines tend to run in families, suggesting a genetic component. Hormonal changes: For many women, changes in estrogen levels, such as during menstruation, pregnancy, or menopause, can trigger migraines. Environmental triggers: Bright lights, strong smells, certain foods (like chocolate, cheese, or caffeine), weather changes, lack of sleep, and allergies that cause sinus issues are common migraine triggers. Neurological factors: Migraines may involve changes in the brain’s nerve pathways, chemicals, and blood vessels, which cause inflammation and pain. Treatment Options for Migraines: Prescription medications: Triptans and anti-nausea medications are commonly prescribed to treat the acute pain of migraines. Preventive medications: For frequent migraine sufferers, medications such as beta-blockers, antidepressants, or anti-seizure drugs may be prescribed to reduce the frequency and severity of attacks. Lifestyle changes: Regular sleep, a healthy diet, and consistent exercise can help reduce the frequency of migraines. Cognitive-behavioural therapy (CBT): Managing stress through therapy can help alleviate migraine triggers. Alternative therapies: Acupuncture, biofeedback, and massage therapy are sometimes used as complementary treatments for migraine management. Recent studies support preventive treatments for chronic migraines, such as CGRP antagonists (Kundera et al., 2020) and neuromodulation techniques like transcranial magnetic stimulation (Lefaucheur et al., 2017). Key Differences Between Muscle Tension Headaches and Migraines Although muscle tension headaches and migraines involve head pain, they differ […]
Ankle sprains are among the most common injuries, especially for athletes, active individuals, and even those who simply trip or misstep during daily activities. Despite being a frequent injury, the importance of properly recovering from an ankle sprain is often underestimated. Proper rehabilitation is crucial not only for returning to normal activities but also for preventing long-term complications like chronic instability, arthritis, or re-injury. In this blog, we’ll take a closer look at ankle sprains, their impact on the ligaments involved, and why recovery is so vital for the health of your ankle and the joints above it. What is an Ankle Sprain? An ankle sprain is an injury that occurs to the ankle ligament, which may stretch or be torn. Most commonly, this happens on the lateral portion of the ankle, as the plantar of the feet turn internally. The role of ligaments is to connect bones to each other and provide stability to the joint. In the acute phase of injury, you may experience swelling, pain, bruising, and sometimes instability in the joint. Mechanism of action includes sudden twisting, rolling, or turning motions, like sports or walking on uneven surfaces. Not all ankle sprains are the same, indeed, we have a classification system for it, which is based on their severity: Grade I (Mild): A slight stretching or microscopic tearing of the ligament fibres, typically causing minimal swelling and pain. Grade II (Moderate): Partial tearing of the ligament, with noticeable swelling, bruising, and limited mobility. Grade III (Severe): Complete rupture of the ligament, leading to significant swelling, instability, and difficulty bearing weight. Which Ligaments Are Most Affected? The ankle joint consists of several ligaments, but sprains most commonly affect the lateral (outer) ligaments. These include: The anterior talofibular ligament (ATFL) is the most commonly sprained ligament on the front of the ankle. Calcaneofibular ligament (CFL): A ligament that connects the fibula to the heel bone. Posterior talofibular ligament (PTFL): Less frequently injured, but it can be involved in more severe sprains. Studies show that the ATFL is the most commonly injured ligament, with up to 85% of all lateral ankle sprains involving this ligament (Kerkhoffs et al., 2012). The CFL is also frequently injured, but less commonly than the ATFL. As mentioned above, most often an ankle sprain happens on the lateral portion of the ankle, but in rare cases, the deltoid ligament on the ankle’s medial (inner) side can be sprained, particularly during more forceful or traumatic incidents. Why more laterally than medially? Biomechanically, our ankle finds it easier to turn inwards than outwards. Therefore, it is easier to exceed in ankle inversion (the feet’ plantar face the medial line of the body) than the other way around. This is due to the disposition of the bond in the ankle and feet. The Risks of Not Fully Recovering from an Ankle Sprain Many people recover from an ankle sprain and return to normal activities, but this doesn’t always mean the ankle is fully healed. Incomplete recovery can lead to several risks, including: Chronic Instability: If the ligaments don’t heal properly, the ankle may feel unstable, making it prone to future sprains or injuries. This can create a cycle of repeated sprains, leading to longer-term joint instability. Re-injury: Insufficient rehabilitation increases the risk of re-injury. Returning to physical activity too soon or without proper strength can cause the ligaments to overstretch or tear again. Arthritis: Studies have shown that improper healing of the ankle joint can lead to post-traumatic osteoarthritis (PTOA). This occurs when the joint surfaces are not properly aligned during healing, leading to cartilage degradation over time. Research suggests that 5-20% of individuals who suffer from ankle sprains may develop PTOA later in life (Delco et al., 2017). Muscle Weakness and Atrophy: After a sprain, the muscles around the ankle often weaken due to disuse and immobilisation. This weakness can extend to other areas of the body, increasing the risk of compensatory injuries (e.g., knee or hip strain) as you change how you move to protect the injured ankle. The Benefits of Proper Recovery As with any injury, the recovery process is dictated by your subjective presentation, which includes your clinical history, fitness level, and more. Here are some of the key steps for a full recovery: Achieve strength and joint stabilityThanks to the therapist’s guidance and a mix of treatment and exercises focused on the muscles that cross the ankle joint, like the peroneal and calf muscles, you can regain ankle stability and strength to return to your daily activities. This process can take up to 12 weeks, and its success is based on a mix of your clinical history and effort placed in the recovery process. Reduction in the Risk of Chronic PainPast the acute phase of injury, the risk of developing chronic pain is a common problem for individuals who don’t rehabilitate properly after an ankle sprain. In fact, studies suggest that proper rehab can reduce the risk of long-term pain by improving joint function and reducing stiffness with research indicating that patients who complete a rehabilitation program are 60-70% less likely to experience chronic ankle pain compared to those who don’t (Gribble et al., 2016; Zamperetti et al., 2019). Rehabilitate the Range of MotionA key goal of rehabilitation is to restore the full range of motion (ROM) to the injured joint. Restoring normal ROM is critical for preventing compensatory movements that can strain other joints along the joint chain, like the knee, hip, or lower back. The Recovery Process: What to Expect Proper recovery from an ankle sprain typically involves several stages: Acute Phase (0-72 hours) – P.E.A.C.E: Protect: Safeguard the injured area from further harm and avoid excessive strain. Elevate: Raise the injured area to reduce swelling and improve blood flow. Avoid Anti-inflammatories: Refrain from using anti-inflammatory medications unless advised by a healthcare professional, as they can hinder the natural healing process in some cases. Compress: Apply compression (e.g., with bandages or sleeves) to reduce swelling and provide support. Educate: […]
Strengthening exercises are an important way to improve our overall health by improving muscular endurance and stability around the joints. Unlike isometric exercises, which are performed with static muscle contractions, strengthening exercises involve dynamic movements that are capable of creating contractions and lengthening of muscles. This type of training is relevant not only for sportsmen but also for everyone who wants to raise their physical condition. Why Strengthening Exercises? Recent studies have focused on the role that strengthening exercises play in the maintenance and enhancement of musculoskeletal health. Strength exercises play a key role in preventing injuries, rehabilitation, and the enhancement of daily functional activities. Why this is possible is because this type of training consists of applying resistance to your body that will challenge your muscles, bones, ligaments and tendons, helping build strength, endurance, and overall physical function. Strengthening exercises stimulate muscular hypertrophy, which is defined by an increase in muscle size and strength. This is very important for preventing and even delaying the onset of sarcopenia, a major factor in declining health with natural aging. Strengthening for Injury Prevention and Recovery Imagine having a shoulder injury and undertaking rehabilitation: It would start with light movement and isometric exercises. After the initial healing phase, strengthening integration is essential. Strengthening exercises rebuild the muscle’s strength, provide joint stability, and regain total function. For example, with a shoulder injury, performing resistance exercises such as rotations with a resistance band and or weights, along different planes and directions, can help regain the strength of the rotator cuff muscles. These exercises will enhance not only the muscles around the shoulder but also the overall stability of the joint and consequently reduce the chance of future injuries. Without going through the exercises phase, you may experience a decrease in pain over the weeks after the initial injury (it depends on the severity of the injury), but that doesn’t mean that you are out of danger or re-injury. Indeed, as soon as you place extra force in the joint or on the soft tissue of the shoulder, the risk of re-injury would skyrocket, as the shoulder complex it may not be ready or strong enough to permorm such actions. Body tissues and Exercise Strengthening. What’s the deal? Throughout our lifespan, our metabolism slows down. During this process, not only will we process energy intake differently, but how our body recovers and regenerates will also change. So, all the body’s soft and hard tissues will have difficulty recovering and staying strong. That’s where the strength exercises come through. Applying a resistance to those tissues, a positive stress resistance, would allow those tissues to regenerate and grow stronger. These are valid for both soft and hard body tissues. We define positive stress as something that does not put the body in danger but is a stress that the body can handle and take advantage of, like a few kg of a dumbbell or a resistance band. Then, the stronger we get, the more weight we can handle, and that’s how we progress in the exercises. How Do Strengthening Exercises Benefit Tendons? Probably the most essential rehabilitation of connective tissues besides bones would have to be the tendons, which connect muscles to bones. When you do resistance training, tendons encounter controlled stress that stimulates the building of collagen. Collagen is vital in repairing and strengthening tendons; thus, the substance is one of the priorities in any rehabilitation program for tendons. For instance, in the rehabilitation from Achilles tendinopathy, there are such eccentric calf raises- you gradually lower the heel below the level of the step, which are particularly effective. The exercise improves resilience and strength of the tendon through progressive loading and stimulating collagen synthesis. Examples of Effective Strengthening Exercises Squats: Excellent for overall strength of the lower body. First, try squats with your own weight, then add weights as you progress. Deadlifts: So good for exercising the posterior chain, such as hamstrings, glutes, and lower back. Go with lighter weights to perfect the form before adding any resistance. Push-Ups: A great exercise for your upper body since it targets the chest, shoulders, and triceps very well. Variants such as decline or incline push-ups can be done to increase/decrease the intensity level. Progressing the Strengthening Exercises Exercise progression is necessary if improvement is to be continually achieved; otherwise, this often leads to a level where no significant further improvements are made. Start with exercises that match your current fitness level and gradually increase the intensity by adding more weight, increasing repetitions, or incorporating more complex movements. For example, one can perfect squats with one’s own body weight and then subsequently move on to the next level by adding dumbbells or even a barbell. Or, for instance, when one masters regular push-ups, they can always try modifications, such as adding weights to the push-up or doing one-arm push-ups to make their muscles work harder. Incorporating Strengthening Exercises into Your Routine It is easy to incorporate a routine where another routine already exists. Indeed, strength exercises don’t have to be associated with hours and hours in the gym. You can have a dumbbell or a kettlebell or a resistance band, sitting in your kitchen, and while you wait for your morning coffee to come up, you can do a few squats. A few minutes of well-practised exercise here and there are better than nothing. Start with little, learn how to experience the pleasure of movement and the benefit of exercising and from there you can build a stronger and longer routine of self-care. And as you learn more and more, you can start looking into balancing a comprehensive program that blends strengthening exercises with cardiovascular activities and flexibility training to promote overall health and functionality. How often should we exercise? I often get asked this question when I give exercises to my patients. We now know that the frequency of strength exercises is strictly related to our goals. So to increase your strength, you look for 3 to 5 […]
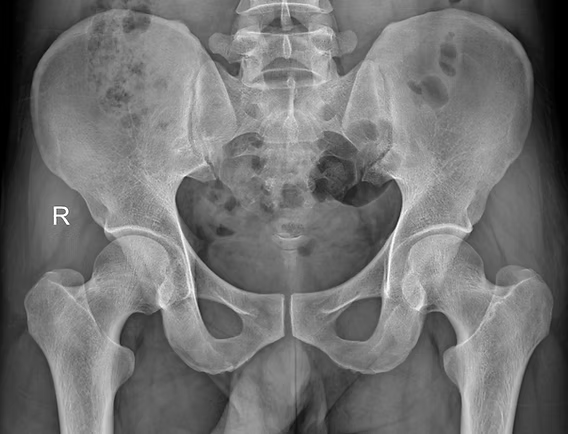
Musculoskeletal pain can be complex, and orthopedic tests and hands-on treatment, sometimes, can be a limited tool to individualise what is happening with the body’s internal structure. Indeed, there are times when a deeper look is required to ensure we are on the right path. This is where body scans imaging comes into play to identify presentations like tendinopathy, bursitis, ligament tear or other underlying conditions. The Role of Body’s Scan in Diagnosing Pathology Body scans include a series of imaging technologies, such as ultrasound, x-ray, MRI, to name a few. Ultrasound is a highly effective imaging tool used to assess soft tissue structures in real-time. Unlike X-rays, which primarily show bone, ultrasound provides detailed images of muscles, tendons, bursae, and ligaments. This makes it an excellent tool for diagnosing conditions such as: Tendinopathy – A chronic condition involving tendon degeneration due to overuse or injury. Bursitis – Inflammation of the bursae, the small fluid-filled sacs that reduce friction between tissues. Those tissue types are found along different body joints, like the shoulder and the hip. Ligament Tears – Partial or complete tears of ligaments, often occurring after trauma or excessive stress. Baker’s cyst – is a fluid-filled swelling that forms behind the knee, often resulting from knee joint conditions like arthritis or meniscal tears, causing discomfort and limited mobility. When we are suspicious of one of those presentations, due to positive results obtained by orthopedic test and medical history, including mechanism of injury, we attempt a recovery process, based on the type of injury, symptoms, and other relevant information. Along this recovery process, we may start with isometric exercises. If, with the first 6 weeks, and a series of sessions, 3 to 4 sessions with this time frame, we still don’t see a major recovery, then we may want to get extra investigation ongoing via an ultrasound scan, which can clarify the underlying pathology. It allows us to confirm or rule out certain conditions, ensuring that treatment strategies are aligned with the actual tissue damage (if any is present). On the other hand, based always on the individual case, we could also require X-rays, which are often more helpful in diagnosing conditions related to the bones, such as arthritis or fractures, as they provide a clear view of bone structure and joint spaces. MRI is a scan that is used for Brain imaging, and when the investigation needs higher details, like when looking at the spine or a joint that via ultrasound was not giving any sign of issue. Ultrasound is also comparable to MRI, as it is faster, easier to deliver, and has fewer complications. How can myotherapy treatment help recovery from what a body scans would show? As we already discussed in another blog, Myotherapy is a practice that looks into the well-being of the skeletal muscle structure. To understand what can be done about a painful presentation, we would initially take a detailed clinical history, then look into objective measurements, such as your movement and body presentation. Given the result we can obtain, we would build up a treatment plan which includes: Hands-on Treatment – Techniques such as deep tissue massage, myofascial release, and dry needling can help reduce pain and improve mobility. Exercise Prescription – Strengthening and mobility exercises help restore function and prevent future injuries. Load Management Strategies – Proper guidance on activity levels ensures tissues heal without excessive strain. That management technique would then be combined and adjusted around the scan’s results. Here are a few examples: Bursitis: If a bursitis is confirmed, medications may be given to reduce the inflammation of the bursa, for that, we concentrate on MLD treatment to further reduce the inflammation and exercises to build strength on the structure that needs support. Ligament tear: When talking of ligament tear, the healing time can dilagate to months if not also a year, so we know now why the 6 weeks program may was not as responsive. We will keep focusing on the strength of the muscle that surrounds the specific joint, and use hands-on treatment to boost blood to the area affected. Arthritis: Medication or dietary change may be put in consideration for pain management and inflammatory reduction. Also in this case, MLD can be used to manage the pain response, and exercises for mantain movement in the affected joint/s. When Should You Consider an Ultrasound or other body scans? If you experience ongoing pain, swelling, or restricted movement that is not improving with therapy, an ultrasound or other scan helps identify the cause. This can prevent prolonged discomfort and allow for a more targeted treatment approach. At Melbourne Massage and Treatment, in Fitzroy North, we aim to provide the most effective care possible. If you’re dealing with persistent musculoskeletal pain, book a consultation with Giovanni today. Together, we’ll determine the best action to get you back to optimal function. Frequently Asked Questions (FAQs) About Musculoskeletal Pain and Body Scans Imaging 1. What are body scans, and how do they help diagnose musculoskeletal pain?Body scans include imaging technologies such as ultrasound, X-ray, and MRI. These scans help diagnose soft tissue injuries (like tendinopathy, bursitis, and ligament tears) or bone-related conditions (such as fractures or arthritis). They provide a clearer picture of what might be causing pain, inflammation, or restricted movement. 2. Why is ultrasound commonly used in diagnosing soft tissue injuries?Ultrasound is highly effective for real-time imaging of soft tissues like muscles, tendons, bursae, and ligaments. It helps diagnose conditions such as tendinopathy, bursitis, and ligament tears, providing a dynamic view of the area being studied without the need for invasive procedures. 3. When should I consider getting an ultrasound or other scans for my injury?If you’re experiencing persistent pain, swelling, or limited mobility that isn’t improving with initial therapy (such as exercises or hands-on treatment), it might be time to consider an ultrasound or other scans. These can help identify the underlying cause of your symptoms and allow for a more targeted treatment approach. 4. How do orthopedic […]