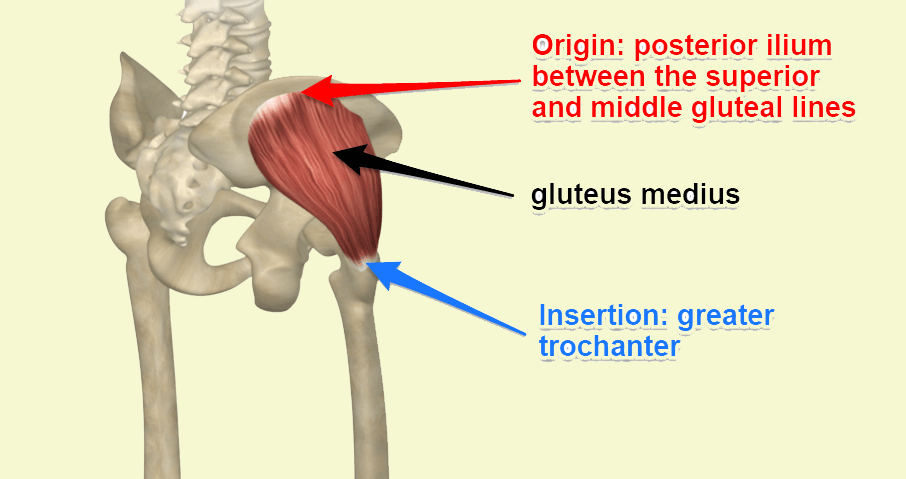
When it comes to maintaining a healthy, functional body, it’s easy to overlook the pivotal role of certain muscles in everyday movement and long-term stability. One such muscle is the gluteus medius. At Melbourne Massage and Treatment, located in Fitzroy North, I see many patients who either love running or love to hit the gym but are not aware of the importance of this muscle for their activity. What is the Gluteus Medius? The gluteus medius (GM) is one of the three primary muscles of the gluteal group, located in the upper part of the buttock. Here is a breakdown of its anatomy: Origin: the gluteal surface of the ilium Insertion: lateral surface of the greater trochanter Innervation: dorsal branches of the L4, L5, and S1 Actions: Abduction and medial rotation of the lower limb. It stabilises the pelvis. Thanks to its positioning, the GM plays a vital role in controlling pelvic movement, specifically in the stabilization of the pelvis during various motions like walking, running, or standing on one leg. More Information About Gluteus Medius actions The GM serves several essential functions that directly affect the stability of the hip and lower body: Pelvic Stabilization: One of its primary roles is preventing the pelvis from tilting excessively to one side when you move, especially when you’re walking or running. If the gluteus medius isn’t working properly, the opposite side of your pelvis may dip downward, leading to an imbalance and compensatory movements that strain other parts of the body. Hip Abduction: The gluteus medius helps to move the leg out to the side, away from the body. This movement, known as hip abduction, is crucial for activities that require lateral movement, such as stepping sideways or maintaining balance while performing physical tasks. Internal and External Rotation: The gluteus medius also assists with the rotation of the hip joint. Depending on which fibers are activated, it helps with both internal and external rotation of the thigh. This is essential for maintaining control and precision in movements. Postural Support: The gluteus medius muscle helps keep the pelvis level when you’re standing on one leg. Without proper activation of this muscle, one hip might drop, affecting posture and causing misalignments in the spine and lower back. The Role of the Gluteus Medius in Hip Stability Why is the GM so important for hip stability? Simply put, this muscle acts as the stabilizer of the pelvis. Without a properly functioning gluteus medius, other muscles and joints are forced to compensate for the lack of stability, leading to overuse and strain. For example, improper GM function can result in excessive stress on the knees, lower back, and even the ankles, which can lead to pain, discomfort, and injury. Clinical implications are vast, especially for athletes and individuals who regularly engage in physical activities. Hip instability can result in difficulty performing simple tasks like walking or climbing stairs, and over time, it may contribute to chronic conditions such as hip osteoarthritis. A common painful presentation that we see in athletes but also the everyday patients is Greater Throcanta Pain Syndrome (GTPS), which is characterised by the side hip pain. This presentation results from a GM tendon irritation. Signs of Weak or Dysfunctional Gluteus Medius Here are some common signs that your gluteus medius may need attention: Pain in the hip or lower back: Since this muscle is integral to proper alignment, dysfunction often manifests as discomfort in the hips or lower back. Difficulty balancing on one leg: Struggling with stability when standing on one leg may indicate weak gluteus medius muscles. Shifting or limping while walking: A noticeable shift or limp while walking can point to weakness in the gluteus medius, causing the body to compensate and disrupt your gait. How can Gluteus Medius impact your run? The gluteus medius is crucial for runners as it stabilizes the pelvis, controls hip movement, and ensures proper alignment during running. This muscle prevents excessive pelvic tilting, reduces side-to-side sway, and helps maintain efficient running form, thereby lowering the risk of injuries such as knee pain, IT band syndrome, and lower back discomfort. A weak or dysfunctional gluteus medius can lead to compensatory movements, affecting performance and causing imbalances. How Melbourne Massage and Treatment Can Help At Melbourne Massage and Treatment, as a clinical myotherapist, I focus on treatment designed to address muscle pain and dysfunction through a variety of techniques. One of the key areas of focus is to create a treatment plan that works for your presentation based on your clinical history. Here is a breakdown: 1. Assessment and Diagnosis: I would conducts a thorough assessment to identify if the gluteus medius is underperforming, weak, or compensating due to other musculoskeletal issues. This involves a combination of posture analysis, movement patterns, and targeted strength tests. 2. Myotherapy Treatment Techniques: I will use various techniques, including trigger point therapy, Dry Needling, myofascial release, and deep tissue massage, to release tension in the gluteus medius and surrounding muscles. This helps to restore proper function, reduce pain, and improve mobility. 3. Rehabilitation and Strengthening: After addressing any issues, we will work to develop rehabilitation strategies, including targeted strengthening exercises for the gluteus medius and other muscles that surround the pelvic, lower back and leg area. These exercises aim to restore proper muscle activation and prevent future imbalances. 4. Injury Prevention: In order to prevent further injury, we will set a target of strength that you want to achieve with your sports activity, and we will do our best to hit that target. Be mindful that based on your presentation, the target could extend from a few weeks to several months. The Takeaway The gluteus medius muscle is far more important for hip stability than many people realize. Its role in maintaining pelvic alignment and controlling movement is essential for pain-free mobility, proper posture, and long-term musculoskeletal health. Whether you’re dealing with hip pain, experiencing difficulty with balance, or want to prevent future issues, understanding and caring for […]
Tag Archives: massage
A deadlift (conventional deadlift) is a popular exercise that aims to strengthen your posterior chain muscle, including the erector spinae muscle, glutes, and hamstring. It is considered a really top list of important exercises to do, and it can be fun and rewarding, but when the weight you move starts increasing, it can lead to severe injuries if you are not using the right technique. Let’s then look into what we need to do to get a good deadlift by starting to analyse from bottom to top how the body should be placed. Centre of mass and biomechanics in deadlift To start with, let’s talk about the biomechanics and the centre of mass for a deadlift. When doing exercises, biomechanics plays a crucial role in safety and optimal exercise execution, and there is no exception for the deadlift. Furthermore, along with all exercises, the lifting and the descending part, the weight has to be in line with the centre of mass. These two components are strictly interconnected to the other one, which means if I don’t use the right biomechanics, I am not going to have the weight aligned with the centre of mass, or if the weight is not aligned with the centre of mass, I am not using my biomechanics at its full potential. So, what’s the centre of mass in the deadlift? The centre of mass in a deadlift is that imaginary line that runs right from the mid-portion of your feet up right in front of your shins, and as you lift the weight up, it passes right in front of your pelvis. That’s where the bar is going to end once you complete the lifting motion. What happens if I don’t keep the bar along the centre of mass? At any stage, during the lifting or the descending motion, if you move the bar further away from the centre of the mass line, there is a great danger of injury. This is because, as the weight travels away from the centre of mass, there is an increase in momentum, which means that your muscles and ligaments that are working hard to move the weight are suddenly placed under a greater load. What are then the proper biomechanics to observe along a deadlift? Ankle and Knee To execute a good deadlift, we want to ensure we have good ankle dorsiflexion, which is not as important as when we squat, but still, we better ensure it is working right. This would allow a straight forward movement of the knee, which would not need to find its way medially or laterally along the initial bending for when we go to grab the bar. Moving up the chain, as we said, the knee have to point straight ahead, following the toes direction. Hip and lower back Next is the hip. This is an important joint, and here is where we need to make sure that we tilt the pelvis forward (bring the teil bone upwards) and as we hinge the hip, we have to have enough movement in there that the greater trochanter (bone landmark that represents the side of the femur’s head) is posterior to the malleolus (the bone landmark that make the side and medial portion of the ankle). Now, if we managed to have tailbone project far back and up, and hip hinged with a slightly bent knee, our back up to cervical area would be alrady quiet flat. Thoracic and head If we keep going upwards, we get to the upper thoracic area, right between the scapula. Here, we want to keep the scapula protracted and have the rhomboids and serratus anterior muscles active and strong so that the arms can hang down straight towards the bar and sit right next to the knee. Regarding the head, use your eyesight to look down at the floor at 45° in front of you and feel the ears pulling away from the shoulder. That would keep your neck nice and long and place the head in the right position. Arms and hands Arms hang down from the shoulder in a straight line, from the AC Joint down to the wrist. The arm has to feel heavy and prolonged, and the hands must sit right next to the shin. Indeed, your arms must stay as wide as your shoulders. That would ensure that your arms are at 90° with the bar, and from a vertical pool point of view, they can take the maximum load ever. Lastly, regarding the hands, there are different grip types that can be used for the deadlift. What is most important is that the wrist is straight following the armline. For exercise purposes, you can have a regular grip where your thumb is gripping around the bar. For heavier weights, you may want to do a mixed grip, where one hand (the dominant one) has the palm facing forward, and the other hand has the palm facing you. In conclusion, the biomechanics of the deadlift, if used correctly, will allow you to always weight in a safe spot, in line with the centre of mass. Your back has to be flat at all times, and along the exercise execution, you want to grasp air in, engage the core to flat out the lower back and then you can lift off. Benefits of Deadlifting Now, let’s look into the benefits of deadlifting. Full-body workout: Deadlifts engage multiple muscle groups—glutes, hamstrings, quads, lower back, core, traps, and forearms—providing a full-body workout in a single movement. Improved strength: Deadlifts are among the best exercises for building overall strength, especially in the posterior chain (back, glutes, and hamstrings). Better posture: Deadlifts can improve posture and reduce the risk of slouching by strengthening your back and core muscles. Core stability: The movement requires significant core activation, helping to enhance core strength and stability. Increased athletic performance: Deadlifts translate well to other athletic movements, as they improve explosiveness, agility, and endurance. Fat loss: The intensity and demand on […]
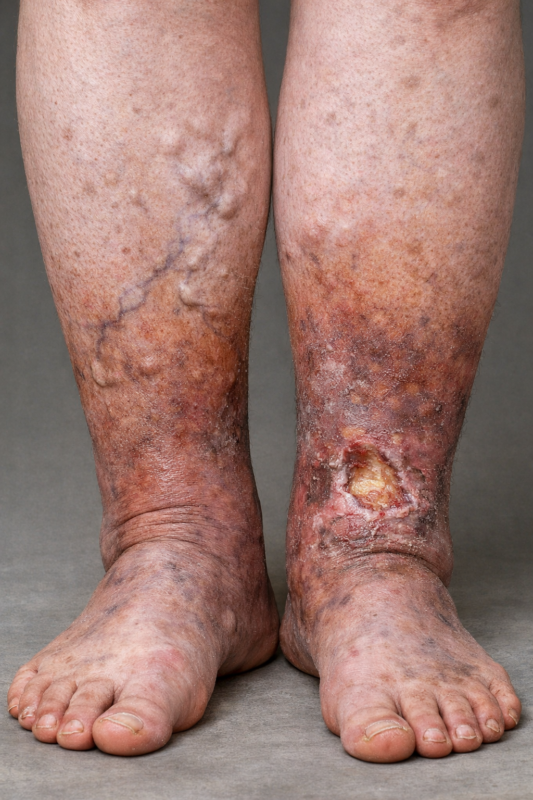
When the lymphatic system stop working, either because for a congential malfunctioning, or because of a an external intervention, which did lead to lymphatic system damage, the individual may start experiencing symptoms of Lymphoedema. At Melbourne Massage and Treatment in Fitzroy North, Giovanni understand how challenging lymphoedema can be, which is why he provide expert care through Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). These non-invasive treatments help manage the symptoms and improve your quality of life. What is Lymphoedema? Lymphoedema occurs when the lymphatic system is blocked or malfunctioning, leading to a buildup of lymphatic fluid. This fluid results in swelling in the affected areas, often in the arms, legs, or other extremities. Lymphoedema can be primary (a hereditary condition) or secondary (often caused by injury, surgery, or infection). The fluid that builds up in the body is a fluid that is naturally produced by the body and is released under the skin and between tissues by the bloodstream. It is reached in protein, bacteria, viruses, dust, and other minor substances that the body is unsure how to handle. Stages of Lymphoedema Lymphoedema progresses in stages, with each stage representing the severity of the condition. Recognizing the symptoms early on can help prevent the condition from advancing, so it’s important to be aware of the subtle changes in your body. Stage 0: Latent or Subclinical Stage In this early stage, there are no visible signs or symptoms of lymphoedema, but the lymphatic system may already be compromised. People in Stage 0 may experience a feeling of heaviness, discomfort, or mild swelling, int the limbs affected by this presentation, but these symptoms typically disappear after resting or with limb elevation. The fluid retention is still minimal and may not be noticed by the individual, but it can be detected through careful assessment. Stage 1: Reversible Stage At this stage, swelling is more noticeable, but the skin is still soft, and the swelling can still decrease with limb elevation and movement. When the swelling is present, the skin will feel puffy or tight, and there may be a sensation of heaviness in the affected area. In this relevant early stage, it i still easy to intervene for prevent further degeneration, and if you are unsure of what you are experiencing, reach out Giovanni for a 15 minutes free consultation, in which, at least thanks to the analysis of your clinical history, we can already evaluate if what you are experiencing is a Stage 1 Lymphoedema. Stage 2: Spontaneously Irreversible Stage In Stage 2, the swelling becomes more persistent and is not fully responsive to movement and limb elevation. The asking of the affected area may begin to feel firmer, and there can be noticeable thickening of the skin. This is the stage where fibrosis (scarring of the tissue) starts to develop, and it’s crucial to stop this from going any worse. While the swelling might fluctuate, it becomes more difficult to manage without intervention. At this point, manual treatments like Manual Lymphatic Drainage (MLD) can significantly help reduce swelling and improve the overall function of the lymphatic system. Stage 3: Lymphostatic Elephantiasis The final stage of lymphoedema is characterized by extreme swelling and thickened, hardened skin. The affected area may look large, disfigured, and become painful to the touch. Tissue fibrosis is advanced, and the skin may develop ulcerations or infections due to poor circulation and immune system function. Indeed, along with the swelling and the fibrosis buildup, the outer layer of the skin is placed further away from the blood capillary, which is responsible for releasing oxygen and other substances essential for skin regeneration.Therefore, as the skin breaks open, due to its poor condition, it is more subject to infections and contamination of pathogens. Stage 3 lymphoedema is debilitating and requires ongoing care and treatment to prevent complications and manage symptoms. At this stage, a combination of therapies such as Combined Decongestive Therapy (CDT) and MLD becomes vital for managing the swelling and restoring lymphatic flow. Common Symptoms of Lymphoedema Lymphoedema symptoms can vary from person to person and depend on the stage of the condition. The common symptoms include: Swelling: The most obvious sign of lymphoedema is swelling in the affected area, typically starting in the arms or legs. The swelling is often gradual and may worsen over the course of the day, especially after prolonged standing or sitting. Tightness or Heaviness: Affected limbs may feel heavy or tight, particularly after physical activity or at the end of the day. This sensation is often worse in the early stages and may become more pronounced as the condition progresses. Pain or Discomfort: Pain, tenderness, or discomfort in the swollen area is common, especially when there is fibrosis (hardening) of the tissues. The pain can range from mild to severe, depending on the stage. Reduced Range of Motion: As the swelling and fibrosis increase, it can lead to a limited range of motion, particularly in the arms and legs. This can impact daily activities and mobility. Skin Changes: In later stages of lymphoedema, the skin may appear thickened or leathery, with a shiny, tight appearance. There may also be visible folds in the skin, particularly around the knees, elbows, or ankles. Frequent Infections: Swollen tissues have a reduced ability to fight off infections, so people with lymphoedema are more susceptible to bacterial and fungal infections, which can further complicate the condition. Numbness or Tingling: As the swelling progresses, the nerves in the affected area may be compressed, leading to sensations of tingling, numbness, or even burning. Increased Skin Sensitivity: The skin in the affected area may become more sensitive, prone to rashes, or develop sores due to the increased swelling and poor circulation. Commonly Affected Areas of the Body Lymphoedema can affect different parts of the body, but the most common areas are: Arms: After surgery, particularly mastectomy (breast cancer surgery) that involves the removal of lymph nodes, the arms are a common site for lymphoedema. The swelling […]
Lymphoedema is a condition often associated with cancer survivors, particularly those who have undergone surgery or radiation therapy, but it can also occur due to other chronic conditions or injuries. Characterized by the swelling of limbs due to the accumulation of lymphatic fluid, lymphoedema can significantly impact a person’s mobility, emotional well-being, and overall quality of life. Early diagnosis of lymphedema and management are key to preventing long-term complications, and at Melbourne Massage and Treatment in Fitzroy North, Giovanni, a skilled Myotherapist and Lymphoedema therapist, specializes in identifying and managing this condition using a combination of manual techniques and physical assessments. In this blog, we’ll explore how lymphoedema is diagnosed, the challenges of identifying it early, and Giovanni’s approaches to detecting and managing the condition. What is Lymphoedema? Lymphoedema occurs when there is a disruption in the lymphatic system, leading to the accumulation of lymph fluid, a protein-rich fluid that sits beneath the skin and between the body’s tissue, which often causes swelling in the limbs or other areas of the body. This condition can develop due to a variety of factors, such as lymph node removal during surgery, radiation treatments, injury, or genetic predisposition. Early detection of lymphoedema is crucial to prevent the condition from worsening and causing complications like tissue fibrosis, infections, or reduced mobility. Challenges in the Diagnosis of Lymphoedema Lymphoedema can be difficult to diagnose, especially in its early stages. In its initial phase, symptoms such as heaviness, tightness, or mild swelling may seem subtle and easy to overlook. Patients might attribute these sensations to muscle strain or arthritis, delaying the diagnosis. Furthermore, swelling can fluctuate, making it even harder to identify at the outset. By the time noticeable swelling occurs, the condition may have already advanced, complicating treatment and requiring more intensive management. This is why early detection is so important, as it allows for less invasive treatments and better long-term outcomes. Giovanni’s Approach to Diagnosis of Lymphoedema As a Myotherapist and Lymphoedema therapist at Melbourne Massage and Treatment Lymphoedema Clinic, Giovanni uses manual techniques and physical assessments to diagnose lymphoedema. Although he does not use imaging technology or machines to detect the condition, Giovanni’s training and experience enable him to identify the signs and symptoms through careful observation, palpation, and physical examination. That said, if it is needed, Giovanni can write a referral doctor for your GP to indicate why he believes it is important for you to undertake a specific scan or some medical test. 1. History taking The earlier approach to Lymphoedema diagnosis is an extended look at the medical history, where any past surgery, injury, accident or medications need to be outlined and taken into consideration. 2. Clinical Assessment Following the history taken to diagnose lymphoedema is the clinical assessment. Giovanni conducts a thorough physical examination of the affected limb or area, paying close attention to key signs of lymphoedema, such as: Persistent swelling that doesn’t subside with rest Feeling of heaviness or tightness in the limb Changes in skin texture, such as hardening or thickening Reduced range of motion in the affected area Along with your booking confirmation, you would also receive a form to fill in online, which would start paving the road to your diagnosis. 3. Tape Measurement Method One of the simplest, yet effective, ways Giovanni diagnoses lymphoedema is by using tape measurements. This involves measuring the circumference of the affected limb at various points (e.g., wrist, forearm, upper arm) and comparing these measurements to the unaffected side. Over time, consistent and progressive changes in limb circumference can indicate the development of lymphoedema. While this method is cost-effective and easy to perform, it may not detect early, subtle changes in limb volume. However, when paired with other assessments, it offers valuable information about the progression of the condition. 4. The Pitting Test Giovanni often performs the pitting test, a hands-on method to assess fluid accumulation in the affected area. This simple test involves pressing down on the swollen area with his fingers. If an indentation (or “pit”) remains for several seconds after the pressure is released, it indicates the presence of excess fluid in the tissue, which is a hallmark of lymphoedema. The pitting test helps Giovanni evaluate the severity of fluid retention, but it is more subjective than advanced diagnostic tools. 5. Stemmer’s Sign – Tissue assessment Giovanni also uses palpation (manual examination through touch) to assess the affected area’s tissue texture and consistency. In the early stages of lymphoedema, the tissue may feel soft and puffy, but as the condition progresses, it can become firmer, and in some cases, the skin may develop a thicker, fibrous texture. These changes are essential indicators of lymphoedema and are crucial for determining the stage of the condition. In addition to this, the Stemmer’s Sign is a test that consists of picking what we would expect to be wrinkled skin, like the one just before the toe/tarsal joint. A positive test would result in the impossibility of pinching any skin due to the swelling in the area. 6. Lymphoscintigraphy A lymphoscintigraphy is a scan that is part of nuclear medicine tests, and it is specifically used to detect any interruption within the lymphatic system. The test is done in the specific clinic, and no recovery is needed for it. The procedure consists of injecting a radioactive liquid either in the feet or hands and with a specific camera, detecting the movement of the liquid within the body. We would expect the liquid to move within a certain timing and pathway along the lymphatic system. If that doesn’t happen, this test can give a good understanding if anything is not functioning with the lymphatic system. Why is Early Detection Crucial? The earlier lymphoedema is detected, the easier it is to manage. Early-stage lymphoedema is often easier to treat with less invasive interventions, such as manual lymphatic drainage (MLD), compression therapy (CDT), specific exercises, and skin care. These treatments can help reduce swelling, prevent the condition from worsening, and improve […]
When it comes to nurturing our health and well-being, many of us tend to overlook one of the body’s most vital systems—the lymphatic system. This system plays a key role in immune function, detoxification, and overall fluid balance. If you’re looking to manage a condition like lymphoedema, Lymphatic Drainage Massage can be a powerful treatment. At Melbourne Massage and Treatment in Fitzroy North, we offer expert Lymphatic Drainage Massage to support your body’s natural detox processes and help manage lymphatic health. Understanding Lymphatic Drainage Massage Lymphatic Drainage Massage is a specialized technique designed to stimulate the lymphatic system, encouraging the natural flow of lymph—the fluid that helps remove toxins and waste from your body. Using gentle, rhythmic strokes, the therapist focuses on areas where lymph nodes are most concentrated, such as the neck, armpits, and groin. The massage promotes the movement of lymph fluid, which can enhance detoxification, improve circulation, and reduce swelling. While traditional massage focuses on muscle relaxation and tension relief, Lymphatic Drainage Massage works primarily on the lymphatic system only. It helps the body to flush out toxins, support the immune system, and restore fluid balance. Whether you’re seeking general wellness benefits or a specific treatment for lymphatic concerns, lymphatic drainage massage effectively supports your body’s natural detox process. Lymphoedema: A Condition That Benefits from Lymphatic Drainage Lymphoedema occurs when the lymphatic system is unable to properly drain fluid, leading to swelling, often in the arms or legs. This can result from a variety of causes, including surgery, injury, cancer treatments, or even a congenital condition. The swelling is not always painful, but may lead to mobility issues and skin problems if not properly managed. Lymphatic Drainage Massage is a highly effective treatment for individuals suffering from lymphoedema. By gently stimulating the lymphatic system, LDM can assist in moving excess fluid away from the affected areas, reduce swelling, and alleviate the discomfort associated with the condition. In addition, LDM can help prevent the worsening of symptoms and improve the quality of life for those managing chronic lymphoedema. How Lymphatic Drainage Works Lymphatic Drainage Massage targets specific areas of the body where lymph nodes are concentrated, using light pressure and rhythmic movements to help move stagnant lymph fluid. The techniques used in LDM include: Pumping Motions: Gentle, rhythmic movements help stimulate the flow of lymph fluid through the vessels and nodes. Circular Strokes: Circular, light strokes are applied to areas where lymph is likely to stagnate. Pressure Application: Gentle, controlled pressure is used to help the lymphatic system move fluid without causing discomfort. These techniques are designed to work with your body’s natural processes, enhancing lymphatic flow and reducing fluid retention. Benefits of Lymphatic Drainage Massage Lymphatic Drainage Massage offers a range of benefits, including: Reduced Swelling (Oedema): LDM is particularly beneficial for those with lymphoedema, helping reduce swelling and discomfort. Detoxification: Encourages the body to eliminate waste products more efficiently, leaving you feeling refreshed and revitalized. Pain Relief: It reduces pain associated with chronic swelling and fluid retention, particularly in conditions like lymphoedema. This is possible because constant mechanical stimulation of the skin stimulates the parasympathetic nervous system, enhancing a relaxation effect. Enhanced Circulation: LDM stimulates the blood and lymphatic flow, helping to improve circulation and reduce the risk of fluid buildup. Conditions for which LDM is Good For Lymphoedema and or Lipedema Post-Surgery Recovery Assists with reducing swelling and speeding up recovery after surgeries, particularly those involving lymph node removal (e.g., cancer surgery). Post-Operative Swelling Helps reduce inflammation and fluid retention following any surgical procedure, such as cosmetic surgery or dental surgery. Swelling reduction would come with improvement in joint mobility. Cellulite Reduction While not a cure for cellulite, LDM can help reduce the appearance of cellulite by improving circulation and promoting lymphatic flow, which aids in the breakdown of toxins and fatty deposits. Detoxification Stimulates the lymphatic system to remove waste products, toxins, and metabolic by-products, enhancing overall detoxification. Fibromyalgia Alleviates some symptoms of fibromyalgia, such as pain and fatigue, by enhancing circulation and promoting lymphatic drainage. Sinusitis and Nasal Congestion LDM can help reduce sinus congestion and improve drainage in the sinuses, alleviating discomfort associated with sinus infections or chronic sinusitis. Migraines and Tension Headaches Promotes relaxation, reduces muscle tension, and supports lymphatic flow, which can help reduce the frequency and intensity of headaches. Skin Conditions (e.g., Acne, Psoriasis, Eczema) Improves circulation and supports the elimination of toxins, which can contribute to healthier skin and help with inflammatory skin conditions. Pregnancy-Related Swelling (Edema) Reduces fluid retention and alleviates swelling in the legs, ankles, and feet during pregnancy, offering comfort to expectant mothers. Improved Immune Function Supports the immune system by promoting lymphatic circulation and toxin removal, reducing the likelihood of illness. Stress and Anxiety While not a direct treatment for anxiety, LDM can promote relaxation, ease tension, and reduce stress, benefiting overall emotional and mental health. Improved Circulation Stimulates blood and lymphatic flow, helping to maintain healthy fluid balance in the body and reducing the risk of fluid buildup and stagnation. Sore or Aching Muscles Can aid in muscle recovery by improving circulation, reducing inflammation, and enhancing fluid drainage. Chronic Inflammation Helps reduce inflammation caused by conditions like arthritis, reducing discomfort and promoting healing. Why Choose Melbourne Massage and Treatment for Your Lymphatic Drainage Needs? At Melbourne Massage and Treatment in Fitzroy North, Giovanni understands the importance of tailored care for each individual. On top of his bachelor’s in Health Science Clinical Myotherapy, Giovanni trained in Lymphatic Drainage Massage techniques and took a holistic approach to health and well-being. Whether you are recovering from surgery, managing a condition like lymphoedema, or simply seeking to enhance your overall health, we’ll work with you to create a personalized treatment plan that meets your specific needs. Booking Your Lymphatic Drainage Massage If you’re in Fitzroy North or the surrounding Melbourne areas and are looking for a Lymphoedema Clinic that can help improve your lymphatic health, alleviate swelling, or manage lymphoedema, Lymphatic Drainage Massage can make a […]
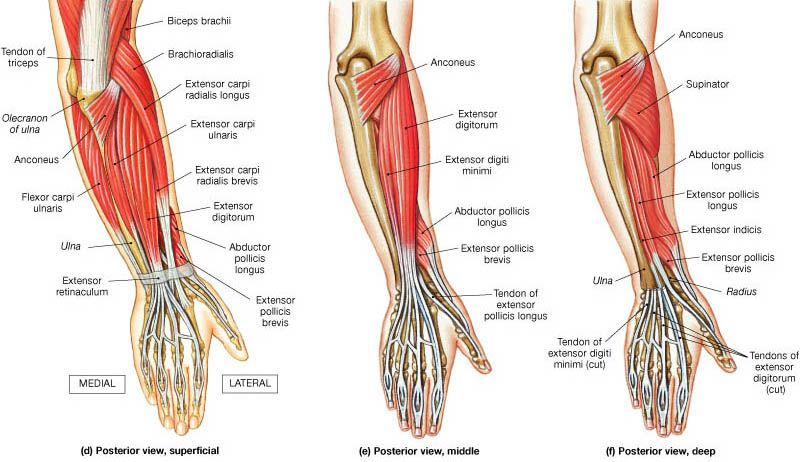
At Melbourne Massage and Treatment in Fitzroy North, we frequently encounter clients dealing with tennis elbow (lateral epicondylitis) and golfer’s elbow (medial epicondylitis). These conditions can cause significant discomfort and limit your ability to enjoy sports and everyday activities. While they are often associated with repetitive arm and wrist movements, it’s essential to consider how poor shoulder mobility and stability can contribute to these issues. What Are Tennis and Golfer’s Elbow? Tennis Elbow Tennis elbow affects the outer part of the elbow, causing pain and tenderness on the outside. This condition typically arises from overuse of the forearm muscles, especially those responsible for wrist extension. Activities such as painting, or even prolonged computer use, or overstreching of extensor muscles can trigger this condition. Golfer’s Elbow Conversely, a golfer’s elbow affects the inner part of the elbow, leading to pain on the inside. This condition is commonly associated with activities that require gripping, flexing the wrist, or repetitive forearm movements, such as golfing, throwing, or lifting. In this presentation is the common flexor tendon that get’s irritated, and refer with pain. The Connection to Shoulder Mobility and Stability While tennis and golfer’s elbow are localized conditions, they often stem from dysfunctions higher up in the kinetic chain, particularly in the shoulder. Poor shoulder mobility and stability can lead to compensatory patterns that place undue stress on the forearm and elbow joints. Shoulder Mobility Limited shoulder mobility can restrict the natural range of motion for various activities. For instance, if your shoulders lack mobility, you may overcompensate with your forearm muscles during tasks that require reaching, lifting, or throwing. This overcompensation can lead to strain, resulting in conditions like tennis or golfer’s elbow. To maintain proper shoulder mobility, you want to ensure the use of the glenohumeral joint along your exercises and move it with specific drills, as this would stimulate the joint synovial fluid and maintain the joint lubricated. On the other hand, if the joint is hypermobile, we should look into how to stabilize it better. Shoulder Stability Shoulder stability is crucial for maintaining proper alignment during movement. Weakness in the shoulder stabilizers can cause the shoulder joint to become unstable, leading to altered movement patterns. When the shoulder isn’t stable, the body often compensates by engaging the forearm and elbow excessively, increasing the risk of injury. As mentioned in the paragraph above, this is what would occur when someone presents with a hypermobility body. In the hypermobility presentation, the ligaments are more lax and don’t hold back the joint movement as expected. Assessing and Addressing the Issue At Melbourne Massage and Treatment, we recommend a comprehensive approach to address tennis and golfer’s elbow effectively: Assessment of elbow epicondylitis Understanding the root cause of your pain is vital. During an initial consultation, we still mainly focused on your elbow presentation and addressed what movement reproduced the discomfort. But not only that. Throughout a tailored investigation, we will address what could be the root cause of the problem. This way, it would be easier to develop a tailored treatment plan. Treatment for elbow epicondylitis Massage Therapy: Targeted massage can alleviate tension in the forearm and improve blood flow, promoting healing. MDN: Myofascial Dry Needling plays a really effective role in tendinitis management. It focuses on targeting the underactive muscles, restoring the neural connection between the central nervous system and muscle, and desensitizing the painful area. Mobilisation: Mobilisation is an ideal technique to address mobility issue, and improve the range of motion of a joint. For epicondylitis presentations, the mobilisation could focus on wrist, elbow or shoulder. This would be based on the finding along the assessment. Strengthening Exercises: In the exercise program, we will initially focus on exercises that can desitentize the elbow area, such as isometric holds, and then move to eccentric and concentric exercises. In this second step, we would already focus on specific shoulder mobility or stability exercises, as needed. Education Understanding proper biomechanics can empower you to make lifestyle changes that prevent future injuries. Giovanni will guide you through exercises and techniques to maintain shoulder health and prevent elbow pain. Conclusion Tennis and golfer’s elbow can be debilitating, but addressing shoulder mobility and stability is key to recovery and prevention. At Melbourne Massage and Treatment in Fitzroy North, Giovanni is dedicated to helping you achieve optimal function and well-being. If you’re experiencing symptoms of tennis or golfer’s elbow, don’t hesitate to contact Giovanni or Book Now your 15-minute free phone consultation to learn more about a personalized assessment and treatment plan. Together, we can work towards getting you back to the activities you love, pain-free. FAQ Q: What are tennis elbow and golfer’s elbow? A: Lateral epicondylitis, affects the outer part of the elbow, causing pain due to overuse of the forearm muscles, particularly those responsible for wrist extension. Common activities that can trigger it include painting and prolonged computer use. Medial epicondylitis, impacts the inner part of the elbow, leading to pain often associated with gripping, flexing the wrist, or repetitive movements like golfing or throwing. Q: How are shoulder mobility and stability related to these conditions? A: Poor shoulder mobility can lead to overcompensation by the forearm muscles during activities requiring reaching, lifting, or throwing. Similarly, weak shoulder stabilizers can cause the shoulder joint to become unstable, forcing the forearm and elbow to work harder, which increases the risk of injury. Both factors contribute to the development of tennis and golfer’s elbow. Q: What are the signs of limited shoulder mobility? A: Signs include restricted movement during overhead activities, difficulty reaching behind your back, and discomfort during routine tasks that involve lifting or throwing. These limitations can lead to compensatory movements that stress the elbow. Q: How do you assess tennis or golfer’s elbow at Melbourne Massage and Treatment? A: We conduct a thorough assessment that focuses on your elbow presentation, identifying movements that reproduce discomfort. This investigation also explores potential underlying issues related to shoulder mobility and stability, helping us understand the root […]
Exercise is the cure for pain, and it is an underestimated medicine that could sort out many of our bodies’ aches. Strengthening exercise, such as exercising under load or resistance, can be done at home or the gym, and it should be part of our weekly routine. It is never too late to start exercising; everyone can benefit from it. At Melbourne Massage and Treatment, we always encourage our patients to make a treasure of the exercises we show, and if you have any questions about it, do not hesitate to ask. Exercises as Medicine. Exercise can be considered a potent medicine, offering many benefits beyond physical fitness. Regular physical activity has been scientifically proven to reduce the risk of chronic diseases such as heart disease, type 2 diabetes, and certain cancers. It also helps manage weight, improve mood, and enhance mental well-being by reducing symptoms of anxiety and depression. Additionally, exercise strengthens muscles and bones, improves sleep quality, and boosts overall energy levels. Its ability to promote longevity and quality of life underscores its role as an indispensable component of preventive healthcare, highlighting the transformative power of exercise as medicine (Ruegsegger & Booth, 2018). How Exercises can help: Mechanotherapy. Mechanotherapy is the therapeutic application of mechanical forces to tissues and cells to promote healing and enhance physiological function. This approach harnesses the body’s innate response to physical stimuli, such as exercise, massage, and physical therapy, to stimulate tissue repair, reduce inflammation, and improve overall tissue resilience. By strategically applying mechanical forces, mechanotherapy aims to optimize biomechanical properties, restore normal tissue function, and alleviate symptoms associated with musculoskeletal injuries or chronic conditions. This therapeutic modality underscores the importance of tailored physical interventions in healthcare, offering a holistic approach to rehabilitation and wellness that complements traditional medical treatments. How many days a week? Ideally, you would like to exercise 3 to 5 times a week for 45 minutes to 1 hour daily, with 1 to 2 days of rest. The reason behind this is covered by the scientific research and data that we have in hand nowadays, which reveal the importance of loading the body with resistance and weights to grow and regenerate the body components, like muscle, tendons, ligaments, etc… and also the fact that, once the body has been put under load, it also needs time to rest and repair itself, which is crucial for maintaining optimal physical and mental health (Lee et al., 2017). Indeed, if we look at the effect of exercises on muscles, the muscles present with micro tears and micro damage post-exercise, which, the day after the training, reproduce pain, better known as DOMS ( Delayed Onset Muscle Soreness ). Time is needed to allow those microtears to recover. How long should DOMS last? As per all the inflammatory responses, DOMS can last between 24 to 72 hours. During this time frame, the body supplies extra blood to the muscles in order to implement a recovery process. During this time frame, to reduce discomfort and aches, you can use a heat pack (remember, no longer than 15 minutes), massage the area with oil, and do gentle movement. Avoid taking anti-inflammatories, as those would slow down the inflammatory response put in place by your body to heal. If pain persists longer than 72 hours, you can book a consultation or refer to a GP for advice on meds or scans. Can exercises be DOMS-free? Yes, exercises don’t have to reproduce pain every time. When you don’t feel that your muscles have been working that hard, it means that you haven’t pushed them to their limits, and therefore, they are not developing new fibres. Is this a bad thing? No, not necessarily. It is all about what you are aiming for. Indeed, if you are aiming to recover from an injury or you are training for a competition, then yes, you would aim to feel the DOMS the day after, especially if you are at the start of your training journey. On the other hand, if you are happy with the level of strength achieved, you can keep the current presentation by doing general training, without pushing your body close to its limit, by exercising twice a week only and by not increasing the load of resistance/weights as weeks pass by. Exercises and muscle bulk. Doing regular exercise is not going to make you bulky unless you are keen to be hyper-disciplined about the type of exercise, timing, and nutrition. But let’s see in more detail what happens to the muscle cells during exercise. Firstly, we have to understand that hypertrophy. Hypertrophy refers to the increase in the size of muscle cells due to the rise in their component proteins. There are two primary types of hypertrophy: myofibrillar hypertrophy and sarcoplasmic hypertrophy. Myofibrillar Hypertrophy: This type of hypertrophy involves increased size and number of myofibrils within muscle fibres. Myofibrils are the contractile units responsible for muscle contraction. Training focusing on heavy resistance and lower repetitions (e.g., weightlifting) typically induces myofibrillar hypertrophy, increasing muscle strength and density. Sarcoplasmic Hypertrophy: Sarcoplasm is muscle cells’ fluid and energy storage area. Sarcoplasmic hypertrophy involves an increase in the volume of sarcoplasm within the muscle fibres. This type of hypertrophy is often associated with higher repetition ranges and moderate resistance (e.g., bodybuilding workouts). It results in larger, more visually noticeable muscles but with less emphasis on maximal strength gains compared to myofibrillar hypertrophy. Mechanism of Muscle Growth: During exercise, particularly resistance training, muscle fibers experience microscopic tears. In response to these tears, the body initiates a repair process that involves synthesising new proteins to rebuild and strengthen the muscle fibers. Over time, with consistent exercise and adequate nutrition, this repair process leads to an increase in muscle size and strength. Importance of Nutrition: Proper nutrition is crucial for supporting muscle growth. Adequate protein intake is essential as proteins are the building blocks of muscle tissue. Carbohydrates provide energy for workouts, while fats contribute to overall health and hormone regulation. Additionally, sufficient […]
The NDIS (National Disability Insurance Scheme) stands as a transformative initiative in Australia, particularly significant in Melbourne, Victoria’s vibrant capital. Designed to provide support and services to Australians with disabilities, NDIS embodies a commitment to inclusivity, empowerment, and improved quality of life for participants across the country. NDIS and Massage Therapy Understanding the NDIS Established in 2013, NDIS represents a shift towards individualised support plans tailored to meet the specific needs and goals of people with disabilities. In Melbourne, this framework ensures that individuals have access to necessary supports that enhance their independence and participation in the community. How It Works At its core, NDIS operates by providing eligible individuals with funding for a range of supports and services. These can include personal care, access to therapies, assistive technology, and modifications to homes or vehicles, all aimed at fostering greater autonomy and well-being. Impact on Melbourne Communities Melbourne, renowned for its diversity and inclusivity, has embraced the principles of NDIS wholeheartedly. The scheme not only supports participants directly but also fosters a network of providers and community organizations dedicated to delivering high-quality services. This collaborative approach ensures that Melburnians with disabilities have access to a wide array of support options, tailored to their unique circumstances. NDSI services at Melbourne Massage and Treatment Giovanni, a dedicated Myotherapist based in North Fitzroy, plays a crucial role in the local implementation of NDIS services. His practice extends its services to surrounding suburbs, providing essential musculoskeletal therapies that enhance the physical well-being and quality of life for NDIS participants. Giovanni’s personalized treatment plans are designed to meet the unique needs of each individual, contributing to their overall health and independence. Services covered by the NDIS scheme include Remedial Massage, Myotherapy, and Manual Lymphatic Drainage (MLD). NDIS and Myotherapy In the vibrant landscape of Melbourne’s National Disability Insurance Scheme (NDIS), Myotherapy stands out as a pivotal therapy for enhancing participant well-being. Myotherapy focuses on assessing and treating musculoskeletal conditions through advanced techniques such as dry needling, joint mobilization, and tailored corrective exercises. For individuals with disabilities, this specialized approach targets pain management and improves physical function, empowering them to navigate daily life with greater comfort and mobility. NDIS and Remedial Massage Remedial Massage therapy plays a complementary role within the NDIS framework, offering participants relaxation, stress reduction, and relief from muscle tension. This therapeutic modality is essential for promoting overall physical and mental well-being. By addressing muscular discomfort and enhancing circulation, remedial massage supports participants in achieving a sense of relaxation and renewed vitality. NDIS and Manual lymphatic Drainage Manual Lymphatic Drainage (MLD) emerges as a vital service under the NDIS, particularly beneficial for individuals managing conditions such as lymphedema. This gentle, specialized massage technique promotes lymph flow, reduces swelling, and supports immune function. MLD not only helps in managing symptoms but also contributes to enhancing participants’ quality of life by improving lymphatic circulation and overall wellness. In Melbourne, practitioners like Giovanni integrate these therapies into NDIS plans with a personalized approach, ensuring participants receive comprehensive care tailored to their specific needs and goals. Through Myotherapy, Remedial Massage, and Manual Lymphatic Drainage, NDIS participants in Melbourne are empowered to achieve greater independence, alleviate discomfort, and enhance their overall well-being. Challenges and Opportunities While NDIS has been instrumental in improving the lives of many, challenges such as navigating the application process or understanding available supports can arise. In Melbourne, organizations and advocacy groups play a crucial role in assisting individuals and families through these complexities, ensuring that every participant maximizes the benefits of the scheme. Looking Ahead As NDIS continues to evolve, Melbourne remains at the forefront of innovation and advocacy in disability support. The city’s commitment to accessibility and inclusivity is reflected in its ongoing efforts to improve service delivery and expand opportunities for those with disabilities. That said, if you need treatment, do not hesitate to book now an initial consultation with Giovanni. During the first session, Giovanni would be able to draft a personal treatment plan that works best for your presentation. If you are in doubt about what treatment works best for you, just get in touch with Giovanni, by clicking here. Conclusion In conclusion, the NDIS has had a profound impact on Melbourne, empowering individuals with disabilities to live more independently and participate fully in society. Through its person-centred approach and collaborative spirit, NDIS exemplifies Australia’s commitment to equity and dignity for all. As Melbourne continues to grow and evolve, so too will the opportunities for individuals with disabilities to thrive, supported by a framework that values their unique strengths and aspirations. Whether you’re a participant, a provider like Giovanni in North Fitzroy, or an advocate, NDIS in Melbourne represents a beacon of hope and progress towards a more inclusive future.
Here is a list of services available at Melbourne Massage and Treatment: Myotherapy Exercises Rehabilitation Remedial Massage Thai Massage MLD Thai Yoga What are these services about? First, any of those services are holistic services, so they can’t be official diagnoses for medical conditions, and Giovanni can’t prescribe any medications. What to expect is guidance on how muscularscaletol conditions, such as plantar fasciitis, tight muscle, muscle tear and more…can be looked after and overcome with manual therapy and exercises. As Myotherapist, Giovanni can guide you on how possibly the pain manifests and how with massage and specific exercises, the pain can be placed at ease. Part of the process of pain management is the change in habits. This can include posture at the workstation, but not only, but other changes can also include your training program, which maybe is too intense for your body and needs to be adjusted. How is the massage delivered? Any massage is delivered in total respect of the patient and the therapist. No nudity or sensual massage are available. Only the body area that needs attention would be exposed. The rest of the body is covered in a towel. Undress level is down to bra and underwear when need it. If we are working on your shoulder, there is no need to remove the pants. Regarding individual massage sessions, like myotherapy treatment, remedial massage, and/or Thai massage, an assessment of the muscular scale of the system would be delivered before the treatment. This assessment included a series of ROM. These assessments would help Giovanni understand what muscle or groups of muscles needs more attention during the treatment. What should I do before the massage session? Treatments such as myotherapy, remedial massage, and MLD include exposing the body parts that need to be worked on. Said so, having a shower before the treatment would be much appreciated. You don’t need to wear any perfume, a deodorant is enough. Should I shave? No, you don’t need to shave. If rock tape needs to be used, the rock tape can be placed over body hair. When you have to remove it, make sure to roll it downwards. Do not pull it off like it is a wax treatment. That could lead to ripping hair and skin off. Where does Giovanni work? Melbourne Massage and Treatment services are available at the Fitzroy North studio on Holden St. Book now your next appointment. If this post didn’t answer all your questions, don’t hesitate to message Giovanni through the Contact Page.
Fibromyalgia is a health condition that causes widespread pain and sensitivity to touch. This type of condition is more common in women than in men, and it is still unknown to science why some people may suffer from Fibromyalgia, even though it is known that stress can play a significant role. On the other hand, genetics can also be the reason why someone can suffer from Fibromyalgia. Fibromyalgia signs and symptoms Symptoms of fibromyalgia may include: headaches sleep disturbances numbness and tingling of the hands and feet muscle and joint stiffness after a period of rest (after sleeping) restlesconditionsndrome Diagnosis of fibromyalgia To be diagnosed with Fibromyalgia, you have to visit your GP first, who may refer you to a specialist. The most widely used clinical criteria for diagnosing fibromyalgia are sourced from the American College of Rheumatology: pain and symptoms over the past week, based on the total of: number of painful areas out of 18 parts of the body The severity of these symptoms: fatigue waking unrefreshed cognitive problems (that can be memory or thought) Plus other general physical symptoms Symptoms lasting at least 3 months, with unchanged Exclusion of other health problems that could reproduce the pain and other symptoms. Treatment and management So, currently, there is no direct cure for fibromyalgia, but there are many treatments that can help manage this condition, like: improving your sleep routine more of a balanced diet relaxation meditation exercise MLD You can also talk to your GP to see what medications can reduce or manage the pain. How MLD can help with Fibromyalgia? Manual Lymphatic Drainage (MLD) is a gentle, non-invasive manual therapy that aims at boosting the Lymphatic System. Along with the delivery of MLD, the therapist would gently stretch your skin and let the skin recoil, with a pain-free touch. This constant repetitive skin stimulation has a positive impact on the parasympathetic nervous system, which is the portion of the nervous system responsible for what we call “rest and digest” mode. Other benefits delivered from MLD are: Oedema reduction Deep relaxation Inflammation reduction Body’s fluid stimulation Skin health improvement Chronic pain management