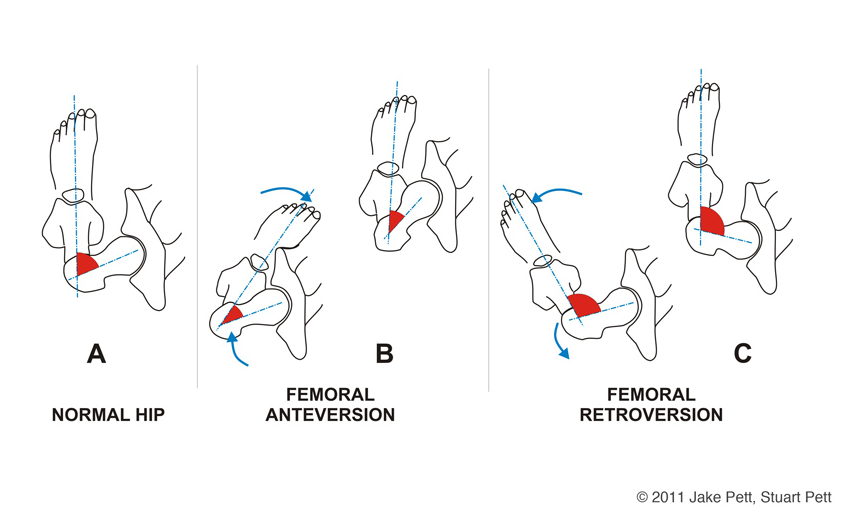
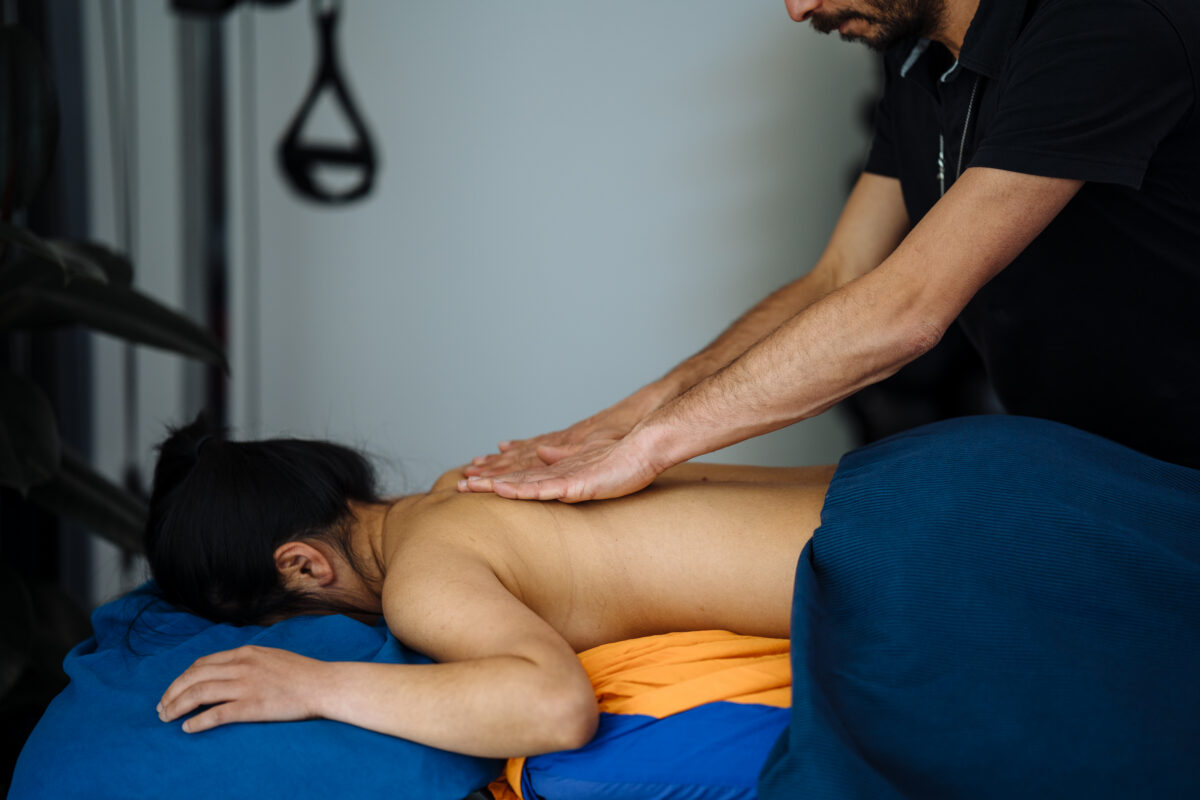
As a Myotherapist and Lymphoedema Therapist here in Fitzroy North, I’ve always believed that movement is one of the most powerful tools for health. Exercise isn’t just about getting fit; it’s about feeling stronger, moving with ease, and living life without pain. Recently, I completed professional training in Kinetic Link Training (KLT), and it gave me the opportunity to see fitness classes and rehabilitation programs under a new light. I’m now offering KLT sessions in Fitzroy North as part of my fitness class at Melbourne Massage and Treatment, in order to help clients move better, recover well, and build long-term strength. Why Exercise Is Good for Everyone The benefits of regular exercise are many, including: Improves muscle tone; Boosts energy Supports joint health; Improves posture; Reduces stress So it doesn’t matter what your goal is, whether you are recovering from an injury, working a desk job, or simply wanting to feel stronger, functional movement training is one of the best investments you can make in your health. That’s why we said that movement is medicine. And Kinetic Link Training is ideal for any fitness level, given the simplified structure of its exercises, and the fact that its setup can be easily replicated at home with some resistance bands and some light dumbbells. How Kinetic Link Training Is Different from Conventional Training More traditional gym workouts often aim to work one group of muscles at a time, with a primary focus on agonist muscles, agonist to a certain movement, such as bicep curls, leg presses, and shoulder raises. Nothing wrong with those exercises, they definitely help you build strength, yes, but not always functional strength. That’s where Kinetic Link Training is different, as KLT is built around integrated, full-body movement patterns that connect the upper and lower body through controlled, coordinated actions. Instead of training one movement at a time, you train the body as a connected system. This style of training improves: Core stability and posture Joint mobility and balance Real-world strength and coordination To simplify it, KLT helps you move better, not just lift more. Therefore, having a goal in mind when choosing to start training can help you define the type of training you may need and want to go for. Kinetic Link Training Is Also Ideal for Post-Surgery and Injury Recovery Rehab KLT is an excellent option for rehabilitation and post-surgery recovery. A few keys component that makes KLT so safe are: Low-impact exercises Controlled movement Entirely adjustable for your needs You can train easily at home What then makes KLT effective for rehabilitation is the fact that you will be asked to do natural movement patterns that can help in regaining body strength safely. In fact, KTL is ideal for anyone looking to rebuild function, improve range of motion, and return to daily activity with confidence. Perfect for Beginners and Those New to Strength Training If you’ve never done strength training before, KLT is a gentle and intelligent place to start. “Why so?” you may ask. Well, the beauty of KLT is that it allows you to perform any exercise to your capacity, and from there, you can not only increase the load or resistance, but you can also increase the degree of movement. Let’s take, for example, a posterior pull with a double leg squat: In this exercise, you are going to start in a squat position (max depth is quads parallel to the ground), facing the machine or the cable direction, while your arms are fully extended. To deliver the exercises, you will be asked to stand while pulling the cable towards yourself, with the elbows running alongside the ribcage. Now, let’s consider a person who may have difficulty squatting. They are not required to go as deep to start with, but still, they can apply a full upper body range of motion, which is basically like a lat. raw exercise. The depth of the squat would come with time and practice. This is only an example of how exercises can be adapted You don’t need to be strong, flexible, or experienced. The movements are easy to learn and can be scaled to any fitness level. Kinetic Link Training: A Balanced Full-Body Workout Now, another great advantage of KLT is the engagement of the upper and lower body in all its exercises. As explained in the example above, along with the KLT exercises, you are required to engage in: Upper body movement: Push Pull Arch Double or Single arm. Different directions, “from where” and “to where” the cable may run: Very Low Low Mid High Very High With or without crossover. Lower body movement between: Squat – Double Leg, Single Leg, Wide Stand Lunge – Anterior, Posterior, Lateral Calf Raises (as a progression of the end/start of squat movement) Which can also be subcategorised as alternated, Split, Reciprocal, and Partial Standing direction: 0° – Facing the cable 45° – To the cable 60° – To the cable 90° – Your L/R side is facing the cable direction 180° – You are giving your back to the cable direction Now, combine all of those options, and you easily end up with thousands of exercises that engage the upper and lower body with an incredible variety of regression and progression. Indeed, this is why every KLT session integrates upper and lower body movements, creating balanced, total-body strength. This ensures you don’t overwork one area while neglecting another. KLT and Lymphoedema Lymphoedema is a chronic condition characterised by severe swelling of the limb due to failure of the Lymphatic System. It can occur due to a congenital presentation (primary Lymphoedema) or post-surgery (secondary Lymphoedema), as often happens after cancer surgery. To manage a Lymphoedema presentation, exercises are essential, as the lymphatic system is stimulated by muscle contraction. Based on the severity of your lymphedema, we can use KLT to help you boost lymphatic fluid circulation and build resistance in the joints and limbs affected by lymphedema. Functional Fitness Fitzroy North Bringing Kinetic Link Training into my practice […]
Monthly Archives: November 2025
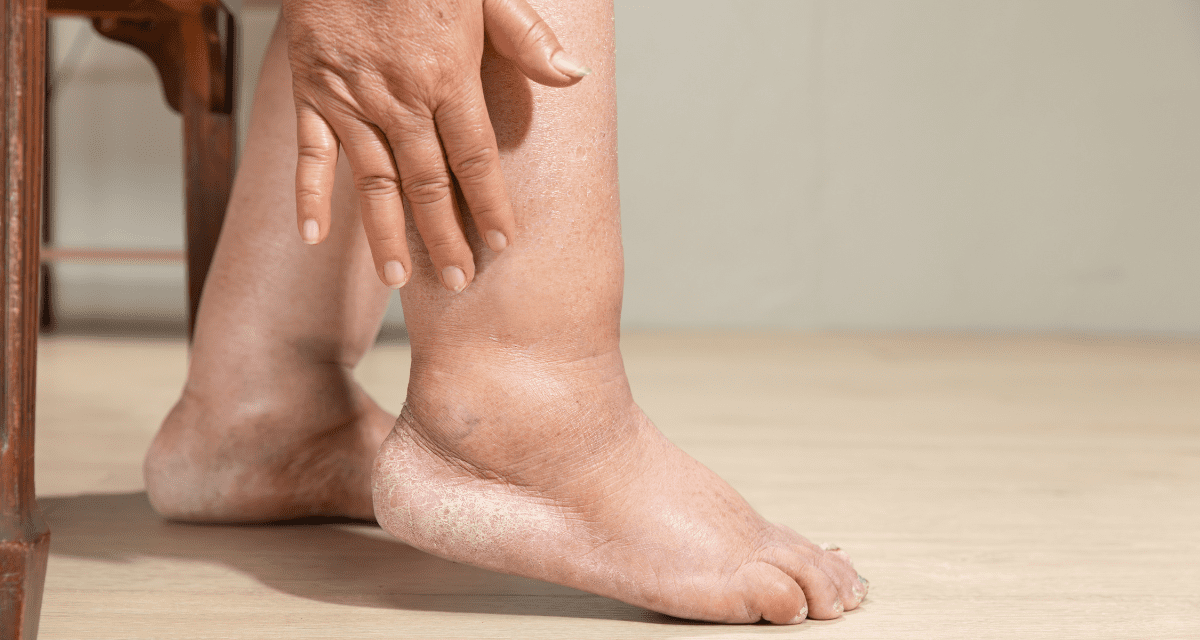
If you’ve noticed swelling in one or both of your legs, it’s natural to feel concerned. Leg swelling, or severe oedema, can have many causes, and understanding the difference between them is key to getting the proper treatment. In this blog, we are going to discuss the different reasons why legs may swell, and how to recognise the key factors of Lymphoedema, and when you’d better consult a GP to address the other issues Is the Leg Swelling in One or Both Legs? To start, we want to observe whether the swelling is monolateral or bilateral —i.e., on one leg or both. Unilateral (one leg):In this case, we may look at a lymphoedema, but we also have to consider a possible vascular-related cause such as deep vein thrombosis (DVT), venous or arterial insufficiency, or trauma. If DVT is suspected, urgent referral is essential. DVT symptoms include: Redness Heat Pain Possible post-flight or prolonged period of immobilisation If it’s venous or arterial insufficiency or injury-related, compression therapy may be started once it’s safe. A specific scan of the vascular system can assist with diagnosis. Your GPs should be able to refer you to a vein specialist to further investigate the presentation. Bilateral (both legs):This may indicate a more systemic or internal cause, such as: Heart, liver, or kidney disease Low protein levels (hypoalbuminaemia) Thyroid issues Medications or reduced mobility Lymphoedema is unlikely to be bilateral, unless severe damage happens to both limbs or the abdominal area, where the lymphatic system is completely damaged. In this case, we still want to rule out any other conditions and dive deep into your medical history. Symmetrical vs Asymmetrical Leg Swelling Symmetrical swelling often suggests internal illness or lipodema, which is a chronic fat distribution disorder that can mimic lymphoedema but is not caused by lymphatic failure. Asymmetrical swelling, where one leg is noticeably more swollen, could point toward lymphatic or venous problems. Understanding the Type of Oedema Once vascular or systemic causes are ruled out, the swelling is classified into types: Venous Oedema Usually linked to chronic venous insufficiency, and the treatment include: Compression bandaging or stockings Exercise and elevation Managing weight and mobility For any MLD treatment and/or intense exercise activity, a safety disclosure from the GP or specialist may be recommended. Lymphatic Oedema (Lymphoedema) Lymphoedema can be primary (congenital or inherited) or secondary (caused by surgery, infection, trauma, or cancer treatment). Either way, if left untreated, it can lead to skin thickening and fibrosis. Furthermore, if the skin suffers a cut or a crack, it can get infected. Therefore, the earlier the intervention, the better. Treatment: Manual lymphatic drainage (MLD) Compression garments or bandaging Skin care and gentle exercise Multidisciplinary management I wrote a specific blog about the characteristics of Lymphoedema and explored the possibility of excluding other conditions. Read it here. Mixed Oedema When a mixed oedema is the presentation, a referral from a GP is essential to ensure there are no contraindications to MLD or compression therapy for treatment. When both venous and lymphatic systems are involved. Needs a combined approach of compression, skin care, exercise, and lifestyle support. Getting the Right Diagnosis and Support If you suspect lymphoedema, it’s essential to get a clinical assessment. At Melbourne Massage and Treatment in Fitzroy North I can help you with that. Things that we will look into are: The pattern and duration of swelling Does the swelling worsen in the heat? Where does the swelling start from? Skin condition Is the skin intact? Does the skin have any elasticity? Medical history and possible triggers Family history of Lymphoedema Any history of cancer or general surgery? Response to elevation and compression Does elevating the leg make a difference in swelling reduction? Does adding compression to it help? Early diagnosis helps prevent complications such as infections or long-term tissue changes. Final Thoughts Swelling in your leg doesn’t always mean lymphedema, but it’s something worth checking out. Things to look into, to narrow down the possibility of having lymphoedema are: Swelling in one leg or both Symmetrical or asymmetrical Attemptive Medical history check Remember: Lymphoedema is manageable with the proper care — and early action makes all the difference.
Lymphoedema is a chronic condition that affects men and women worldwide and is categorised into primary and secondary forms. The primary is a congenital type of Lymphoedema, which would present with swelling starting at the end of the limb and propagating upwards. Where the secondary is due to an external cause, which can potentially damage the lymphatic system, such as post-cancer surgery or radiation therapy, but it can also happen post-severe injury or major surgeries, and the swelling would start at the area of damage and spread away from it. So let’s look now into some self-assessment you can do at home to help you understand if you are presenting with Lymphoedema. Signs and Symptoms of Lymphoedema Lymphoedema presents as severe swelling in an individual body part, which can be a leg, an arm, the thoracic area, or even the genital area. Most common signs of Lymphoedema are: Swelling Tight skin Lack of mobility in the limb involved Dry skin Skin that cracks easily Redness Feeling of tightness and heaviness in the limb The aspect of tight skin and cracks on the skin when experiencing lymphoedema has to be taken seriously and needs immediate attention. The risk is of encountering severe infections if the skin cracks are not kept clean and sanitised. Consequences include infections, like cellulitis. Who is at Lymphoedema Risk? As mentioned in the introduction of this blog, there are several reasons why someone can suffer from Lymphoedema. Now let’s try to get some clarity about it, by analysing in more detail what primary and secondary lymphoedema are. Primary Lymphoedema A primary lymphoedema is a congenital condition, which means the subject suffering from lymphoedema was born with a damaged, missing, or malfunctioning lymphatic system. Here is a further breakdown of this presentation based on the age at which the Primary Lymphoedema manifest: Congenital lymphedema – birth to age 2 Lymphedema praecox – puberty to age 35 Lymphedema tarda – after age 35 A specific characteristic of primary lymphoedema is that the swelling starts at the extremity of the limb. Secondary Lymphoedema A secondary Lymphoedema manifests itself after an external cause has damaged the Lymphatic System. An example of an external course is a cancer surgery, where, along with the cancer removal, there are lymph nodes removed, leaving the lymphatic system interrupted. Other causes of secondary lymphoedema include radiotherapy, which may damage the lymphatic system, but even a severe injury like a car crash or other types of surgery. Indeed, if someone already experiences a weak lymphatic system, an external intervention, like a surgery, can further damage the structure, leading to lymphoedema as a consequence. In comparison to the primary lymphoedema, the swelling in a secondary lymphoedema would start at the site of damage (surgery or radiated area) and travel down the limb. Lymphoedema self-assessment As a lymphoedema therapist in Fitzroy North, I help people who present with this symptom determine whether the swelling they are experiencing is related to lymphoedema. But there is a series of Lymphoedema self-assessments that you can also do at home to start helping you understand what’s going on. Stemmer’s Sign The Stemmer’s sign is one of those Lymphoedema self-assessments that you can do on your feet or hands, and consists of the ability to pinch off the skin above your fingers or toes (based on which limb the lymphoedema is) just where the metatarsal (hand) or tarsal (feet). If the swelling is severe enough to stretch the skin tight, you would not be able to pick the skin off that area. For more accuracy, it is suggested to do this test on both limbs to notice any difference. Pitting Oedema A pitting oedema is a mark left in the skin after pressure is applied. Similar to the sox mark, which we all may get after wearing sox for a prolonged period of time. The difference is that for a pitting oedema to be positive, it is enough to apply pressure for about 30 to 60 seconds. What you are looking for, for a positive test, is: Is any mark left behind? How fast does the skin recoil? How fast does the skin’s colour return to normal? A positive pitting oedema is a sign of protein-rich fluid accumulating beneath the skin. Online questionnaire – Lymphoedema Self-Assessment Below, I provide two online questionnaires available to anyone to self-assess their risk of developing secondary lymphedema from post-cancer treatment. Arm Lymphoedema Questionnaire Leg Lymphoedema Questionnaire These guides are designed as educational aids based on experience, with no supporting evidence in the literature, so do not take the result of this test as a diagnosis. What’s After Lymphoedema Self-Assessment? If the results of the questionnaire and the lymphoedema self-assessment above give you a hint of suffering from lymphoedema, I personally suggest to: Keep your skin clean and moist. Avoid skin cuts, so if you work in the garden or outdoors, wear protective clothing and take any precautions needed to maintain your skin integrity. Book a 15-minute free online consultation so that we can discuss what treatment plan may work best for you, and how we can manage your Lymphoedema. Keep yourself in motion. Any movement is better than no movement. Walking is great, go swimming, just don’t spend a prolonged period of time still.