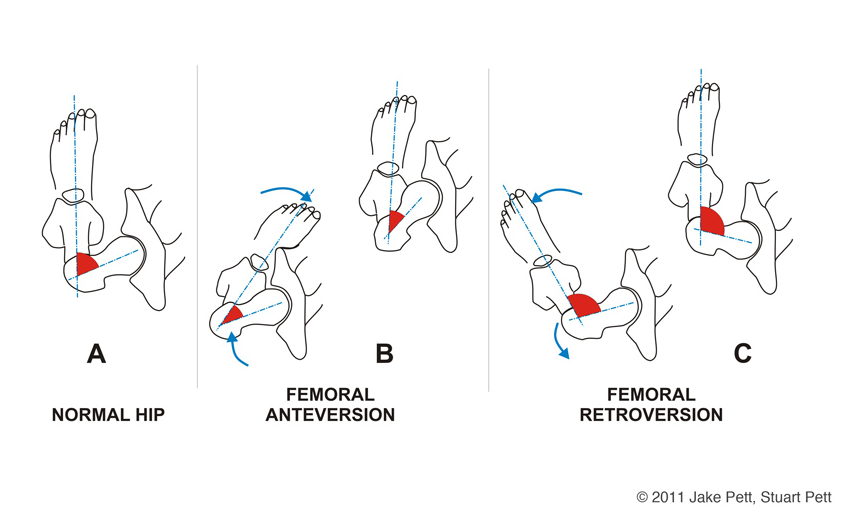
Elbow tendinopathy, whether it presents as tennis elbow (lateral elbow pain) or golfer’s elbow (medial elbow pain), is one of the most common overuse injuries in active people, desk workers, and manual labourers. At Melbourne Massage and Treatment in Fitzroy North, I frequently help patients recover from both forms of elbow tendinopathy. Elbow Tendinopathy: How Does It Manifest? “Tendinopathy” refers to irritation and degeneration within a tendon due to repeated overload. Elbow Tendinopathy, in both of its forms, tennis or golfer’s elbow, can sound like a sport-related injury, but it has little to do with the sports world. The reason why those presentations carry their name is due to the sport action, which requires that specific muscle group to work to deliver the golfer strike (medial) or tennis strike (lateral). So what can actually cause an elbow tendinopathy are: Sudden increase of tendon load – lifting heavier than usual, at the gym or at work Repetitive action – think of that constant mouse or keyboard action in the office environment Overstretching of the tendon – Poor office ergonomics can overload the elbow joint and the elbow’s tendons To be more specific, the office worker presenting with elbow tendinopathy often has repetitive mouse/keyboard use, which is often accompanied by poor ergonomic factors, such as the forearm being in a prolonged pronated position (palm facing down), which places the common extensor digitorum tendon (CEDT) under stretch. Medial and Lateral Tendinopathy of the Elbow Let’s look into the difference between the actual Tennis (lateral) and Golfer’s (medial) Elbow. Tennis Elbow (Lateral Epicondylitis) Pain in the outer elbow Irritation of the wrist extensor tendons, especially the Extensor Carpi Radialis Brevis (ECRB) Familiar with typing, lifting, racquet sports, and DIY tasks Golfer’s Elbow (Medial Epicondylitis) Pain in the inner elbow Irritation of the wrist flexor tendons Related to gripping, pulling, forearm rotation, and throwing How To Recover From a Tendinopathy? Despite different pain locations, the rehab approach is almost identical, and while rest provides temporary relief, it does not fix the underlying tendon changes. The true solution? A structured, progressive exercise rehab program that restores tendon strength and resilience. In fact, as the tendinopathy itself came to be an issue due to an overload of the elbow’s tendon, to settle the pain and discomfort, we have to: Reinforce the elbow tendon and muscle so that it can perform better. Analyse what overloaded the elbow tendons – we have to understand what can be changed in the loading process, starting from: Shoulder stability (looking up in the joint chain – Mobility and Stability) The ergonomic of your workload, that is, office or heavy repetitive work (like gardening, for example, or construction). Workout program – ensure there is a progressive load in the program that is right for your capacity. The 3-Phase Exercise Program for Elbow Tendinopathy Here at Melbourne Massage and Treatment in Fitzroy North, as a clinical myotherapist, I get to see many patients presenting with Elbow Tendinopathy, and the rehab protocol and recovery that I used is detailed below. Phase 1: Pain Reduction & Tendon Activation (Week 1–3) In this initial phase, the goal is to calm symptoms without resting the tendon completely. Tendons respond best to gentle, controlled tension, better known as isometric exercises. Isometric is ideal because: Tendons have a low blood supply compared to muscles, so in order to receive the nutrients that allow the healing process to be delivered, they need long and steady engagements. A tenodon that is inflamed presents with disorganised collagen fibres, which are not running straight, and no longer form a compact line. And there is a need for a constant load to restore new fibres that can regain the tendon’s functionality. Wrist Extension Isometric (for Tennis Elbow) You will be sitting at a desk with your forearm comfortably supported by the desk, with your hand in a prone position (palm down) Slightly extend your wrist against resistance. Pain-free movement (it could be a bend or a lightweight) Hold 20 seconds, repeat 10 reps Wrist Flexion Isometric (for Golfer’s Elbow) You will be sitting at a desk with your forearm comfortably supported by the desk, with your hand in a supine position (palm up) Deliver a slight wrist flexion against resistance. Again, it has to be a pain-free movement. Hold 20 seconds, repeat 10 reps Time of hold, repetition and pain response are subjective to each individual. That’s where we would stop and focus on each individual clinical history and presentation, and adapt the elbow tendinopathy rehab program to your needs. Gentle Mobility & Dry Needling From a point of view of massage for elbow tendinopathy, there are a few techniques that work really well, especially in the early phase of recovery: Joint Mobilisation – passive movement applied to the wrist and elbow joint, to improve the range of motion of this joint and disengage the area. Dry Needling – The usage of a needle on muscle, to create a micro-inflammation and to drive more attention from the nervous system into the targeted area. Deep Tissue Massage – When dry needling is not an option, deep tissue massage can also help in creating this targeted central nervous system response. Phase 2: Strength & Tendon Remodelling (Week 3–8) This is the most critical phase, and the one that actually restores tendon health. Eccentric Wrist Extension (Tennis Elbow Gold Standard) How to do it: Extend the wrist of the affected side with your good hand, while in the affected side, you are holding a lightweight or resistance band. Slowly lower the weight with your injured side with a tempo that last 3–5 seconds Repeat 12–15 reps, 2–3 sets – this is an endurance setup. Between each set, rest for at least 30 seconds. Eccentric Wrist Flexion (Golfer’s Elbow Gold Standard) Same method, but applied in a flexion motion. Assist the initial movement of flexion Slowly bring the wrist back to the straight position with a 3-5 second tempo. Look always at somewhere between 12-15 reps, for endurance performance. […]
Monthly Archives: December 2025
As a therapist who works with Lymphatic Massage in Fitzroy North and post-cosmetic-surgery patients, I often get asked, “What’s the difference between MLD and Brazilian lymphatic drainage?” To answer this question, I often have to give people a background of my training as a Lymphatic Drainage therapist and what is happening to their body post-liposuction. What are the differences between Vodder MLD and Brazilian Lymphatic Drainage Vodder MLD, which is the therapy I offer for post-cosmetic surgery and also Lymphoedema management, is a very light, rhythmical, skin-stretching technique. It has about 100 years of history, and it has a strong research base for lymphedema management and is useful in postoperative recovery, either in cosmetic or orthopedic surgery. Brazilian lymphatic drainage, on the other hand, tends to be firmer, more continuous, and pragmatically geared toward reducing swelling and bruising after cosmetic procedures, but it has less scientific evidence to support any benefits. For post-cosmetic surgery lymphatic massage (liposuction, abdominoplasty, facelifts, tummy tuck…) I would strongly recommend gentle Vodder-style MLD, and here is why: Any surgery, including cosmetic surgery, is highly invasive for the body, and therefore, you will present post-surgery with High skin sensitivity Swelling and bruising Pain A gentle approach, as Vodder MLD, would allow: Reduce the swelling with a pain-free approach Take away exceeds inflammation Help reinforce skin sensitivity As the healing process progresses and you move from the acute to the sub-acute healing phase (week 2 to week 3), we can start applying stronger pressure to break down fibrosis. What people call “Brazilian Lymphatic Drainage” “Brazilian lymphatic drainage” (BLD) is a manual therapy that is getting famous thanks to social media presence and some influencers talking about it. It is a practice which often refers to faster, more continuous wave-like movements and sometimes firmer pressure than Vodder MLD, and involves the usage of oil too. Those who offer Brazilian Lymphatic Drainage claim a faster recovery after aesthetic procedures (reducing bruising, local oedema, and tissue stiffness), even though clinical literature that looked into BLD in aesthetic and post-op settings, like randomised trials, describes this technique as debatable, and furthermore, the evidence of its efficacy is limited compared with Vodder studies. What does the research say? Systematic reviews on MLD (Vodder used often) show MLD is commonly used for decongestive therapy in Lymphoedema patients. The quality of the evidence varies, while effect sizes are moderate for some outcomes. Randomised trials that compare Vodder MLD with other modalities (e.g., compression, pneumatic compression) report benefit for symptoms and arm volume in breast cancer-related lymphedema and postoperative swelling in some surgical contexts. An early RCT explicitly used the Vodder technique and showed benefits in arm lymphedema management. Recent reviews and clinical articles regarding plastic-surgery literature highly support the use of postoperative lymphatic massage. The recommendations are to receive MLD one to three times a week, in the early recovery phase, for reducing swelling, pain, fibrosis and improving comfort. That said, often that information is shared by the surgery clinic staff after the surgery; therefore, it’s always better to choose a clinic that is clear and transparent about the post-surgery recovery, and not only about the surgery itself. When looking for studies about the Brazilian Lymphatic Drainage massage, it is hard to find something that is specific enough about this technique, and that doesn’t mix data and trials with other techniques, like bandaging and exercises. Therefore, it’s hard to evaluate the quality of this technique in terms of the RCT protocols. MLD – What works for what? Practical comparison For lymphedema (medical swelling after lymph node removal/cancer). When someone presents with lymphedema, the best choice is Vodder-style MLD as part of complete decongestive therapy. I don’t do this recommendation only because I offer this service, and I know its potential, but also because Most RCTs and meta-analyses have evaluated MLD (in Vodder style) as the safest and evidence-based treatment that has enough relevance for this type of presentation. For early post-operative care after cosmetic procedures (e.g., liposuction, abdominoplasty, facelifts, tummy tuck). In any given surgery, along the acute phase, the body is a high state of inflammation and the site of surgery would be delicate to touch for several weeks post surgery, indeed a gentle approach to the area is highly recommended, so Vodder-style MLD is way safer compare to Brazilian Lymphatic Drainage, because the tissues are fragile; MLD at this stage in time, it would helps reduce oedema and bruising and promotes comfort. Many plastic surgeons recommend MLD early and frequently in the first 2–6 weeks. Later phase (2–6+ weeks): While healing is progressing and you step into a sub-acute phase of recovery from the post-cosmetic surgery, firmer or more targeted techniques, which recall what Brazilian Lymphatic Drainage can be used to address residual fibrosis/stiffness, always with the surgeon’s clearance. That said When dealing with post-cosmetic surgery fibrosis, even Vodder MLD would include firm pressure. That’s how fibrosis is broken down. For general wellbeing, detox/relaxation, cellulite or fluid retention Gentle MLD (Vodder) is great for relaxation, reducing mild fluid retention, and supporting circulation without soreness. Good for regular wellness maintenance. Brazilian-style DLM is often used in aesthetic clinics for body contouring and cellulite care; people report feeling less heaviness and faster visual improvement, but the high-quality evidence is more limited, and outcomes vary with practitioner technique. MLD Safety & Contraindications – What You Need To Know In my practice, I am selective about who I offer MLD, especially after cosmetic surgery, and here is what I would look out for: Active infection Uncontrolled heart failure Acute deep vein thrombosis (DVT) Untreated cancer without clearance Fever Recent major bleeding or unstable medical conditions Liver or Kidney conditions After cosmetic surgery, you have to make sure to follow the surgeon’s recommendation about antibiotic intake, and or other medications. MLD can not start unless you are cleared of all the above. So, which do I recommend, Vodder or Brazilian Lymphatic Drainage? It is now quite clear that at Melbourne Massage and Treatment, for MLD, either […]
ACL stands for anterior cruciate ligament, and is the strongest ligament in the knee. ACL injuries can be time-consuming, depending on the severity. At Melbourne Massage and Treatment in Fitzroy North, I offer an ACL rehab program that aims to help you recover based on your clinical history, daily activities, including your sports, if any, and consider that the healing time can’t be boosted, but assisted. ACL – What It Is? ACL is the strongest ligament in your knee, and connects the femur to the tibia. Its role is to keep the knee stable, especially during activities that involve sudden stops, changes in direction, or jumping. You can then understand why so many athletes or sports lovers end up with an ACL-type injury. As with all ligaments in our body, the ACL doesn’t have an excellent blood supply, which makes its recovery longer, compared to what can be a muscle injury. What is Myotherapy and How Can It Help with ACL Rehab? Myotherapy is a hands-on treatment method that targets muscular pain, improves joint mobility, and addresses the root causes of musculoskeletal injuries. For ACL rehab, this approach is essential because an ACL injury affects not just the knee but the surrounding muscles, joints and movement patterns. Hands-on treatment can indeed be a good start for rehab and injury, as it not only creates a trust between the patient and the therapist, but can help in creating better awareness of the muscles, which in a second phase of the myotherapy appointment are going to be used for delivering tailored and injury-specific exercises. The goal is to support your ACL recovery and knee rehabilitation holistically. ACL Injury: Scan and Manual Test There are several methods of diagnosing an ACL injury. Scans: Arthroscopy – A keyhole surgery, where a camera is inserted in the knee to check the level of injury. Partial or complete ACL tear. Magnetic Resonance Imaging (MRI) – Less invasive than an Arthroscopy, but still expensive to run. Indeed, it is rare nowadays; in Australia, you can get an MRI prescribed for this presentation. More information is available here. Manual Test Lachman test Lateral Pivot Shift Test Anterior Draw Test Those together with an attemptive clinical history, range of motion and functional test would help to tailor a conclusion on a possible ACL injury. ACL and Surgery – Is Surgery Still a Thing? Surgery techniques and technologies have come a long way from what we could expect, and yes, ACL surgery is still a thing. That said, before going for surgery, you will be asked to try and recover from your injury with conservative treatment, like a rehab program. The reason behind this is: Suregey cost and pressure on the public health system Rehab gives as good results as surgery most of the time Surgery also goes by the severity of your injury – is any other knee tissue/structure injured, or is it only the ACL? Post surgery, you still have to go for rehab, and it would still take 6 to 12 months for a full recovery. Athletes may benefit the most from ACL surgery, given its longer-lasting effects on knee stability. More information about ACL rehab vs ACL surgery is available from the systematic review by Papaleontiou et al (2024). The ACL Rehab Phases: Strengthen Beyond the Knee To recover from an ACL injury, we need to look behind the mechanics of your lower limb, and set a starting and and ending point of recovery. Acute Phase In the acute phase, which is the first one to two weeks after injury, we may focus on isometric holds, gentle movement, and spend more time on hands-on treatment. In this phase, the aids of crutches is mandatory. Strength Phase Past the acute phase of the injury, you will notice how it would be easier to engage the knee joint, as the swelling would be eased, and therefore, you can achieve greater movement. There, we will start incorporating eccentric and concentric loads, with some light-weight or light-resistance bends. This phase can last somewhere between 10 and 12 weeks. All of these would be a step-by-step process. So the loads would be progressed weekly, based on the strength and mobility outcome. Sometimes, you will have to push through some mild pain, but the most important thing is that you keep that joint moving, and have good rest, good food too, to enhance the recovery at its best. Return to daily activity – RDA In the final stage, the focus would shift to plyometrics, an essential part of ligament rehab. That’s where we would re-train your knee to act pre-injury time. This can take another 12 to 24 weeks. It all depends on the severity of the injury and what your needs, in terms of sport or daily activities, are. So, the combination of myotherapy treatment with targeted rehabilitation exercises and fitness classes for recovery is what makes Melbourne Massage and Treatment service stand out. In my rehab-focused classes, we work on: Strengthening the muscles that support the ACL Improving balance and stability to prevent re-injury Gradual conditioning to safely return to sports, running, or everyday activities My Personal Approach At Melbourne Massage and Treatment, I work one-on-one with each client. I assess your movement, identify areas of weakness or tension, and design a personalised ACL rehab program. To be even more specific to your individual presentation, I do use THE MAT as an aid. A measurement tool that allows me to test your mobility and stability, giving us objective numbers and data to work on, too. Recovery from an ACL injury takes time, but with the right approach, you can regain full function and return to the activities you love. I’m here to guide you through every step of your ACL rehabilitation journey. If you’re ready to start your ACL rehabilitation in Fitzroy North or want to see how myotherapy can help, book a session with me at Melbourne Massage and Treatment today. Let’s get you moving stronger and safer than […]
Liposuction interventions are on the rise, driven by the enormous influence of social media on how we look and by the abundance of cheap clinics worldwide. While liposuction surgery removes stubborn fat deposits, the recovery period from this type of intervention is often underestimated. As a clinical myotherapist specialised in Manual Lymphatic Drainage (MLD) Vodder style, I regularly work with clients who are navigating the post-operative process, and I often get to hear clients who haven’t been fully informed about the post-surgery care needed, and the timeframe of recovery. Indeed, many patients who have undergone Liposuction surgery are surprised to learn that MLD plays a supportive role in the recovery process, and not by “boosting” healing, but by complementing your body’s natural ability to manage swelling, fluid congestion, and fibrosis. Below, I explain what liposuction involves, why MLD is recommended before and after surgery, and what you can expect during the healing timeline. What Exactly Is Liposuction? Liposuction is a surgical procedure that aims to remove excess fat from targeted areas of the body. There are different ways in which liposuction can be delivered, but what they all have in common is the usage of a cannula to break down and suction fat from beneath the skin. Once the surgery is delivered, and the fat is removed, the body experiences trauma in the form of: Swelling Fluid accumulation Tissue inflammation Disruption to lymphatic pathways Development of fibrosis (hardened or rope-like scar tissue) Superficial blood cloth Manual Lymphatic Drainage (MLD) is a manual therapy that can make a significant difference for all those presentations. How Manual Lymphatic Drainage Supports the Healing Process MLD is a non-invasive, gentle manual technique that stimulates the movement of lymphatic fluid toward functioning lymph nodes. Compared to a regular massage (Remedial Massage, Deep Tissue, Thai Massage…), it does involve the usage of oil or creams and does not aim to reproduce any pain or inflammatory response. In fact, it is the opposite; it aims at taking away excessive inflammation, as this is one of the many roles of the lymphatic system, and the technique I used is Vodder style, which is clinically recognised for its rhythmic, directional, and methodical application. Here’s how MLD supports recovery after liposuction: Reducing Post-operative Swelling As with any surgery, even Liposuction leads to significant swelling as the body implements an inflammatory response post-trauma (the physical damage of cutting the skin open and removing body tissue). MLD helps guide the fluid that builds up due to the inflammatory response back into the lymphatic circulation, easing pressure and discomfort. Minimising the Formation of Fibrosis Fibrosis is the body’s natural response to invasive body intervention and to sudden skin dilatation; indeed, it is a common presentation in Lymphoedema too. The fibrotic tissue is a common concern after liposuction, and without proper care, tissue can become firm and lumpy, affecting the final aesthetic result.Here is how MLD supports the breakdown and prevention of fibrosis: Increasing lymph flow Softening congested areas In the fibrotic area, we apply strong pressure (still pain-free) to break fibrosis down Encouraging natural tissue remodelling That’s where more frequent treatment is most helpful. To break and manage fibrosis at its best. Preparing the Body Before Surgery The reason why MLD should be considered as a pre-operative intervention too, lies in the fact that a stimulated Lymphatic System place you in an advantageous position along the recovery process, by improving lymphatic circulation, creating better conditions for tissue recovery after surgery. When Should You Start MLD After Liposuction? Once the surgery has been delivered, the ideal time to begin MLD is as soon as you have finished your course of antibiotics, as long as: All open wounds are closed, and No infection is present. The above are essential precautions to prevent the spread of infections. Also, the early start of MLD practice would ensure the best outcome post-surgery. What To Expect from MLD Treatment Post-Liposuction While many patients find out about MLD only after they receive the surgery, and this often happens when they have their surgery overseas, in countries like Turkey, Thailand, Bali, they are still not sure till the time they meet me, what MLD treatment would be about for their post-surgery recovery. In this case, I always explain in detail what the treatment is going to be about, starting with and overview of: What is the lymphatic system How we stimulated What you should expect post-treatment, and what to do and not to do Healing time frame Other topics I had to share and reassure my patients about are: MLD is not painful There is no body fluid extraction I am not going to push liquid out of your incision Yes, you need to drink plenty of water post-treatment I found that patients who undergo liposuction, especially in Turkey, come back with tough stories about acute post-surgery care, where they get their incision reopened, and liquid milked out from there. THIS IS A DANGEROUS PRACTICE AND IS NOT MLD AND IS NOT WHAT I OFFER ANYWHERE UNDER ANY CIRCUMSTANCES. How Should You Prepare Yourself for and MLD Treatment? Here is a list of things to be aware of before you go for and MLD treatment: Food and water – You can eat a light meal a few hours before your treatment and ensure you drink only water before and after the treatment. Strictly avoid alcohol – Avoid any form of intoxication before and after treatment, as this can make you really sick and unwell Medication and Clinical History – In the initial consultation form, you must declare any medication you are taking or have taken and your clinical history, to ensure no contraindications for MLD are present. Avoid cream or lotion – Application of cream or lotion on the skin would make the skin slippery and more difficult to stretch, impairing then the stimulation of the lymphatic system Post Treatment – MLD is extremely relaxing. Ensure to have some time off after your session, in case you feel like a nap or not doing […]
Joint hypermobility is often seen as an advantage or as a healthier status. How often have you heard someone say, “Oh, I can’t do that! I am stiff as!” while looking at someone else who can easily bend over and touch their toes. In this blog, we are going to take a look at the risk related to hypermobility and the lower-limb risk of injury. What is Joint Hypermobility? Joint hypermobility refers to the ability of a joint to move beyond the normal range of motion. A joint is a structure made of ligaments that connect two or more bones, and when it is hypermobile, it is due to the connective tissue being looser or to variations in collagen. It is hard to estimate the total number of people who are hypermobile, and there are also certain health conditions that are related to this presentation, but overall, the majority of people who are hypermobile do not suffer from any direct pain because of this presentation. On the other hand, if doing specific sports activities, the risk of injury may increase. We will see why later. How Do We Test for Joint Hypermobility? – The Beighton Score During a Myotherapy or Remedial Massage initial consultation, a hypermobility test is something that we commonly look at at the start of the session. The Beighton Score allow us to determine the excessive hypermobility a patient may present with and helps us understand what range of motion we are expecting from specific movements. The test consists of 9 passive movements that test the flexibility of the: Elbows; Knees; Fingers; Thumbs; Pelvis Each side of the body is tested (for a total of 9 possible joints), and the higher the score, the more hypermobile the person is considered to be. The passive movement is delivered by the therapist, which moves the patient’s joint. Beighton Score Tests: Bending the index or middle finger backward beyond 90° (one point each side) Bending the thumb back to touch the forearm (one point on each side) Hyperextension of the elbows beyond 10° (one point each side) Hyperextension of the knees beyond 10° (one point each side) Bending forward with straight knees and placing palms flat on the floor (one point) Scores: 0 to 2 points – Hypomobile 3 to 4 points – Norms 5 to 9 points – Hypermobile What the Research Says About Injury Risk A systematic review from Pacey et al. (2010) found that: Knee injuries are significantly more common in hypermobile athletes, especially in contact sports such as football, rugby, and basketball. The risk of knee injury was up to 4.7 times higher in hypermobile individuals compared to their non-hypermobile peers. Interestingly, ankle injuries did not show the same increased risk. This systematic review concluded that yes, hypermobility may increase the risk of injury, but only for specific joints. Why Are Hypermobile Joints at Risk? Now, let’s try to understand why hypermobile joints are at risk. Joint instability: Looser ligaments provide less support and lack stability. Muscle overcompensation: Muscles around the joint may have to work harder to stabilise movement. Delayed proprioception: Hypermobile individuals may have reduced awareness of joint positioning, making them more susceptible to awkward landings or twists. These factors combine to place increased strain on the knees, particularly during high-impact and contact activities. Managing Joint Hypermobility with Strength Training Joints’ hypermobility is not something that can be changed to the extent of the ligament’s lack of stiffness, at least to any significant level (when looking at adults), but it can be managed via strengthening the muscles that cross the hypermobile joint. Benefits of Strength Exercises for Joint Hypermobility: Improved joint stability: Stronger muscles support the joints and reduce reliance on ligaments. Better proprioception and control: Resistance training helps improve coordination and joint-position awareness. Injury prevention: By creating balanced strength around vulnerable joints (like the knee), you can reduce the likelihood of strains, sprains, and dislocations. Practical Exercise Tips: Focus on controlled movements over heavy lifts – Lifting heavy helps you build hypertrophy in the muscle. Incorporate closed-chain functional exercises (like squats, lunges, and leg presses) that mimic real-life movements. Train the stabiliser muscle of the body: Calf muscles for the ankles Quads, hamstrings for the knee Abdominal muscles for the lumbar area Cuff rotator muscles for the shoulders Biceps and triceps for the elbows This is a breakdown and a simplification of what can be done. But when going for strength training, you can be sure that all those muscles would be included in any generic workout. Final Thoughts Hypermobility is not a limitation; it’s simply a characteristic of how your body moves. However, when combined with physical activity, especially in contact sports, it is associated with a higher risk of knee injuries. The good news is that strength training and targeted rehabilitation can help protect hypermobile joints, improve performance, and keep athletes active for longer. If you suspect you have hypermobility, book a Fitness Class here at Melbourne Massage and Treatment, Fitzroy North, and let’s start working on your presentation by choosing your goals and achieving them step by step. FAQs: