As a therapist who offers Manual Lymphatic Drainage in Melbourne, I am blown away by how many people come and seek MLD for general wellbeing, and ask me questions like: “What about tapping my body?” “Should I do guasha?” “I have been told my Lymphatic System is sluggish” Indeed, if you’ve spent any time on social media lately, you’ve probably seen endless content about the lymphatic system, and of course, the more time you spend watching them, the more you will be offered. Dry brushing. Guasha. Detox teas. Essential oils. I call those “Social Media, Lymphatic hacks.” They belong only to social media, not to reality and/or science. As someone who practises Manual Lymphatic Drainage in Melbourne (MLD), I think it’s important to explain what the lymphatic system actually does, what MLD is really useful for, and why people often overcomplicate something that the body already does naturally. And honestly, for many healthy people, one of the best things you can do for your lymphatic system is simply go for a walk. What Is the Lymphatic System? To start with, the lymphatic system is part of your body’s immune and fluid regulation system. Its job is to: Help manage fluid balance Support immune function Transport waste products Assist with inflammation and healing It consists of: Lymph vessels Lymph nodes Lymphatic organs Lymph fluid Unlike the blood circulation, the lymphatic system does not have a pump like the heart, and another difference is that the lymphatic system is capable of absorbing substances that are, molecularly speaking, bigger than what the blood stream can do, simply because the capillaries of the lymphatic system have a bigger aperture than those of the blood stream. Then, regarding how the lymphatic system pumps fluid around the body, it is based on the fact that the internal vessel contraction occurs. The more the vessel contracts, the more liquid moves. And those vessels are sensitive to their surroundings, in fact: Muscle contractions Breathing Changes in pressure Everyday movement Those are all factors that stimulate the lymphatic system to work faster. That’s why movement is so important. And consider that in the human Lymphatic System, contraction rates are typically around 1 to 2 times per minute, at rest, where when doing intense visceral activity, it can jump up to 15 contractions per minute. Why Walking Helps Your Lymphatic System Now, we can than easily understand that every time we walk, our muscles gently contract and relax, and specifically, the calf muscles are the ones that work the most, and are the ones responsible for assisting both the lymphatic and blood systems to push liquid upwards, against gravity. So, walking acts like a natural pump for lymphatic flow, and it can help with: Encourage fluid movement Support circulation Reduce stiffness Improve breathing mechanics Support general recovery and wellbeing Reduce stress Your body evolved to move lymph through normal human movement. Not through expensive “detox” products. Not through aggressive scraping tools. Not through viral wellness trends. Simple movement works remarkably well. What About Dry Brushing and Guasha? Ok, I will be honest on this one: this is where social media often exaggerates things. There is currently no strong scientific evidence showing that dry brushing or guasha creates a special lymphatic drainage effect in healthy individuals. And I want this message to be clear: we are talking about healthy individuals, who are the vast majority of us. That doesn’t mean people cannot enjoy those practices, because they still have a meaning and a use. Indeed, any skin gentle stimulation would still have a major impact on the nervous system, specifically the parasympathetic (rest and digest one), which means it can still have a relaxation effect. Therefore, dry brushing may: Exfoliate the skin Increase temporary circulation at the surface Feel relaxing Guasha may: Feel relieved of muscle tension – and again, this is a nervous system response Temporarily increase local blood flow But neither appears to “detox” the body or dramatically improve lymphatic drainage in the way social media often claims, and most importantly, none of the effects mentioned above last for a long time, nothing like or in comparison to a good walk or exercise time. So let’s be clear about what does what, and let’s remember that the human body already has highly sophisticated systems for managing waste and fluid balance: The lymphatic system The liver The kidneys The lungs The digestive system And again, most healthy people do not have a “blocked” lymphatic system. What science says about those tools? Interestingly, even some of the more positive research around guasha comes with important limitations that are often ignored on social media. Indeed, a study published by Sun‐hee A. et al (2025) that looked at facial roller massage and guasha found some short-term improvements in facial contour measurements, muscle tone, and skin elasticity. However, the researchers themselves acknowledged several limitations, including: The small sample size – only 34 participants The short 8-week duration – already longer than other studies They only looked at temporary aesthetic outcomes rather than meaningful health changes to the lymphatic system itself In fact, the study did not demonstrate that guasha “detoxifies” the body or improves lymphatic drainage in healthy individuals. In other words, while these techniques may temporarily affect appearance, circulation, tissue tension, or relaxation, that is very different from the dramatic claims often made online about “flushing toxins” or “resetting” the lymphatic system. Where Manual Lymphatic Drainage (MLD) Can Be Helpful Ok, if you got this far in the blog, it means you are actually serious about your wellbeing. Great! As a Clinical Myotherapist and Vodder MLD therapist, I am with you. Now, it is important to separate evidence-based treatment from wellness marketing. Manual Lymphatic Drainage (MLD) is a gentle, specialised treatment approach designed to support lymphatic flow and fluid movement. MLD can be beneficial for people experiencing: Lymphoedema Lipoedema Chronic venous insufficiency Post-surgical swelling Scar recovery Chronic inflammation Swelling after injury Sunburn recovery MLD may also support general well-being because it is deeply […]
Tag Archives: melbourne
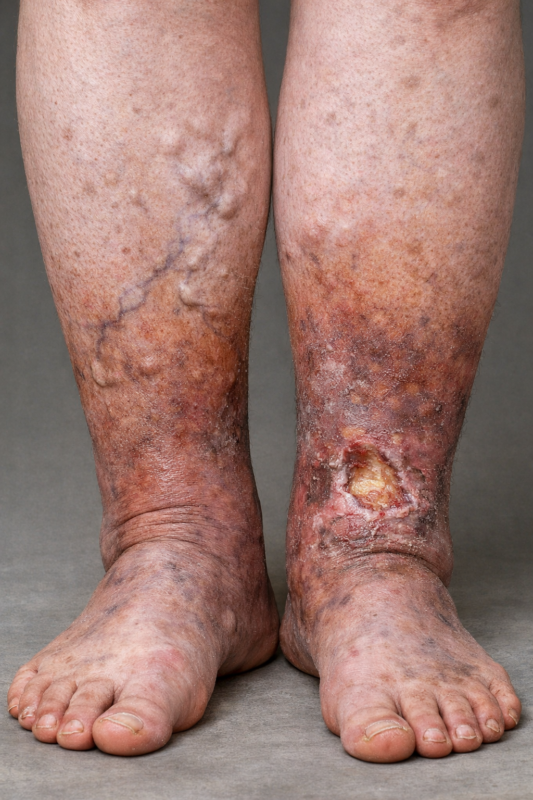
In Australia, Chronic Venous Insufficiency (CVI) affect more women than men, with a ratio of 25%–40% in women and 10%–20% in men (Al Shammeri et al., 2014). As a consequence of this condition, swollen legs are a common concern. CVI occurs when the veins in the legs struggle to return blood efficiently back to the heart, often leading to leg swelling, heaviness, aching, and visible varicose veins. At Melbourne Massage and Treatment in Fitzroy North, since I specialised in Lymphoedema therapy, I regularly support clients experiencing leg swelling related to venous conditions too. Understanding how to manage the condition can significantly improve comfort, mobility and long-term leg health. What Is Chronic Venous Insufficiency? Chronic venous insufficiency is a condition defined as chronic when lasting for more than 3 months. CVI develops when the valves inside the leg veins become weakened or damaged and stop acting as they should, which is why blood finds difficulty in flowing back to the heart. This results in swelling in the lower legs. Common symptoms include: Persistent swelling in the lower legs or ankles Aching, heaviness or fatigue in the legs Skin changes such as dryness or discolouration Varicose veins Tightness or discomfort after prolonged sitting or standing Without appropriate management, CVI can progress and increase the risk of skin complications or infection. The Different Levels of Chronic Venous Insufficiency Find below a table that describes how Clinical, Etiological, Anatomical, and Pathophysiological (CEAP) classify chronic venous insufficiency. Stage Description C0 No visible/palpable signs of venous disease C1 Telangiectasias or reticular veins C2 Varicose veins C3 Oedema C4 Skin changes secondary to chronic venous disease (haemosiderin, lipodermatosclerosis, atrophie blanche) C5 Healed ulcer C6 Recurrent active venous ulcer The more advanced the stage, the more likely the hospitalisation of the patient for infections. This is not only a cost to the public health system, but to the Australia popolation too. Compression Therapy: A Key Part of Managing Swollen Legs The most effective way to manage swelling related to Chronic Vein Insufficiency is compression therapy. Compression garments are helpful as they apply controlled pressure to the legs, which supports the veins and encourages blood and fluid to move back toward the heart. Unfortunately, there is no quick fix for swollen limbs, and for many people with chronic swelling, compression becomes an essential part of daily management. But, you have to be aware that compression should always be prescribed and fitted appropriately. Indeed, the compression has to have the right gradient pressure, so stronger pressure at the bottom and weaker at the top; otherwise, we risk getting the liquid stuck in the leg and not moving. On the other hand, with certain arterial conditions, compression may not be suitable; therefore, it is important that you talk to your GP about getting a referral to a vein specialist to know what’s the best approach for your swollen legs. When Varicose Veins Are Present If varicose veins are present, low-level compression is often recommended initially. This provides gentle support to the venous system while remaining comfortable for everyday use. The goal is to: Support vein function Reduce fluid build-up Improve comfort during daily activities Help prevent worsening swelling In fact, each individual may require a different compression level depending on their condition and tolerance, but also the integrity of the skin. Compressions indeed are tight to put on, and for those with weak and fragile skin, it can be difficult to maintain skin integrity while wearing compression. Why Flat-Knit Compression Garments Are Often Recommended For clients with persistent swelling or changes in limb shape, flat-knit compression garments are frequently recommended. Flat-knit garments offer several advantages: They provide stronger containment for swelling They can be custom-fitted for better comfort and effectiveness – class 3 and 4 They help prevent fluid from accumulating in specific areas They are often more suitable for long-term management Because every leg shape and swelling pattern is different, proper measurement and fitting are essential. At Melbourne Massage and Treatment, Lymphoedema clinic in Fitzroy North, I provide assessments and measurements for your swollen legs, so that I can provide garments that fit you for your specific presentation. Accessing Compression Garments Through the SWEP Program (Victoria) If you live in Victoria, you may be eligible to access compression garments through the SWEP program (State Wide Equipment Program). SWEP helps eligible residents obtain essential medical equipment, including compression garments used in the management of venous conditions and lymphatic swelling. As a SWEP-registered therapist, I can guide clients through the process, including: Clinical assessment Measurement for appropriate compression garments Assistance with the SWEP application process Ongoing monitoring and adjustments The SWEP is free to access and does provide funding for 4 garments a year, specifically: $150 per garment if off the shelf $300 per garment if made on measurements For Chronic Vein Insufficiency, most often the off-the-shelf garments are the ones to go for. But still, you have to know what class would best work for you, and what size would best work for you. Movement: An Often Overlooked Therapy Movement, as per my favourite medicine, is another important component in managing swollen legs. In fact, blood flow, but even lymph flow, happens better when muscles contract and work. For the legs, the calf muscles act as a natural pump, helping push blood and fluid upward when we walk or move. When we remain seated or standing for long periods, this pump becomes less effective. Simple strategies include: Regular walking Gentle ankle movements during long periods of sitting Light leg exercises Avoiding prolonged immobility when possible Even small amounts of regular movement can make a noticeable difference in managing swelling. Protecting the Skin: A Crucial Step in Preventing Infection People with chronic leg swelling are more vulnerable to skin breakdown and infection, and this is due to a series of reasons, such as: Increased venous pressure damages small blood vessels Reduced oxygen and nutrient delivery to the skin Chronic swelling stretches and weakens the skin Inflammation causes skin changes Keeping the skin […]
At Melbourne Massage and Treatment in Fitzroy North, as a clinical Myotherapist, I am enthusiastic to offer 1:1 fitness class that aim to improve your wellbeing and body strength. And one thing that I will never stop surprising my clients with is that it is never too late to start working on their strengths, no matter their age, gender, and capacity. Whether you’re recovering from injury, managing persistent pain, navigating age-related changes, or simply want more energy and confidence, personalised fitness is transformative. Why Starting Now A 1:1 Fitness Class Matters? Strength Training Improves Physical Health at Any Age Have you ever heard an older person wishing to be weaker? No, don’t you? That’s why strength and resistance training aren’t just for elite athletes or bodybuilders; they’re essential for everyone. As we age, our body’s natural capacity to regenerate, including regenerating muscle mass and strength, bone density, and other body tissues, naturally declines, which can affect balance, mobility, fall risk, and independence. Resistance training reverses this decline and improves functional outcomes. A systematic review by Kashi K. S. et al. (2023) found that resistance training significantly improved muscle strength, physical function, and reduced symptoms of depression in older adults. Exercise Matters for Mental Health Too Exercises are not only the best way to maintain physical health but also have an immense impact on our mental health. And that is a 1:1 fitness class or a group class, regular exercises can really change how you feel within your head. Infact, we have plenty of evidence from Recent Research that looks into this: A review by Ayaz A. et al. (2026) highlights how aerobic, resistance, and mind-body exercise modalities have psychological benefits, from improved mood to reduced stress and anxiety. Study by Ma Y. and Mumtaz S. (2025) finds that structured exercise programs improve mental well-being by activating neurobiological and psychosocial pathways. Meta-analysis by Rossi E. (2024) showed that strength training has moderate and significant antidepressant effects in adults with depressive symptoms. So yes, your workouts aren’t just changing your body, but they’re changing your brain. Why 1:1 Fitness Classes Are Especially Effective While training is beneficial for everyone, for physical and mental health, personalised training, like a 1:1 fitness class, makes a huge difference, and here’s why: Training Tailored to You Everyone has different goals when starting a fitness journey, or while they are training, and everyone has different needs and capacities, on which the goal is shaped. Therefore, a 1:1 fitness class session allows for customised programming that matches your goals, health history, injury status, and movement patterns, which generic videos or crowded group classes rarely provide. Expert Guidance Prevents Injury At Melbourne Massage and Treatment, I am proud of the studies I done (a Bachelor in health science clinical myotherapy, and following courses like the KLT training) and the effort I put in place to improve my fitness and communication skills, which led me to offer a tailored program for any of my clients. For people with pain, past injuries, or chronic conditions, this is crucial. Motivation and Accountability I often come across clients who don’t feel confident enough in themselves, who don’t like the gym and think that strength training for them is not a thing. And that’s when I can’t stop thinking about how powerful it is to change their mind by showing them how a few minutes of well-done movement, either with or without load, can change everything. That’s when I get them in for Fitness Class here in Fitzroy North, and I help them achieve their goals. Personalised Follow-up On top of a tailored 1:1 fitness class in person, what makes the difference in terms of service here at Melbourne Massage and Treatment, when I show some exercises, I will send you a PDF file with the picture and the description of the exercises, to ensure you will be bale to replicate those exercises anywhere you are ay your own time and comfort. Fitness Class Comes With An Added Bonus — Better Bone and Cardiovascular Health The action of lifting weights and lifting heavy is seen from your body as a positive stress, which creates a concatenation of benefits. Along those we find: Bone regeneration – increase of bone density Maintaining metabolic health Improving markers related to heart disease and diabetes Improve or maintain optimal equilibrium – poor equilibrium is the major cause of falls. And more… All the benefits a fitness class can deliver are crucial as we age. No one, as they age, wishes that their health gets more and more compromised, isn’t it? Start Where You Are — It’s Not About Perfection Whether you’ve never stepped foot in a gym before, you’re returning after an injury, or you’re trying to break a cycle of inactivity, the best time to start was yesterday. The next best time is now. It is never too late to start working on your strength, and this is the most important message I find myself passing on to my clients. The body can always adapt to load. And no matter if you have just started or you are a pro, you will always have to face some challenges. Therefore, start working on your mobility, improve the way your body can move, let’s than load it a little at the time, and build your own journey into wellbeing day by day, fitness class after fitness class. Final Thoughts You don’t need to be “fit enough” to start a 1:1 fitness class, and it’s absolutely never too late. Here’s the truth I’ve seen in across many clients: People in their 40s, 50s, 60s, and beyond see meaningful gains, both physically and mentally. Individualised guidance accelerates progress safely. Strength and structured exercise improve both quality of life and mental well-being. If you’ve been thinking about starting a fitness journey, come and talk to us at Melbourne Massage and Treatment, Fitzroy North. For those who decide to commit to a change, a positive change, for their well-being, there are 5 or […]
If you’re searching for lymphatic therapy in Fitzroy North, it’s common to see terms like Manual Lymphatic Drainage (MLD) and Lymphatic Massage used interchangeably. As a clinical myotherapist with specialised training in lymphoedema management (MLD since Nov 2021; lymphoedema therapy since Oct 2024, trained with the Vodder Academy), I am here to clarify exactly what these treatments are and why one is clinically recommended over the other — especially for conditions like lymphoedema or post-surgical swelling. In fact, the importance of understanding the difference between MLD and Lymphatic Massage is vital when you want results that matter, and not just temporary relaxation. What Is Manual Lymphatic Drainage (Vodder Method)? Manual Lymphatic Drainage (MLD) is a specialised technique developed by Emil and Estrid Vodder in the early 20th century, and it is characterised by gentle, rhythmic hand movements to stimulate the lymphatic system. The reason behind the gentle and light movement is to ensure that during the treatment, we can stretch the skin and let it recoil naturally; therefore, we stimulate the lymphatic system at its full potential. Therefore, MLD is not a “massage” in the spa sense, it’s intentionally structured to follow physiological lymphatic pathways to support lymph flow. Key points about MLD: Trained practitioners follow evidence-based protocols. Movements are light, rhythmic, and intentional, not vigorous. The “Vodder method” is internationally recognised and taught with strict standards. It is often integrated into Complete Decongestive Therapy for lymphoedema. One recent article explains the theoretical physiology and clinical context of MLD in lymphoedema management. Manual lymphatic drainage: the evidence behind the efficacy (PubMed) What Is Lymphatic Massage? “Lymphatic Massage”, on the other hand, is more of a broad term used in wellness settings, like a SPA or massage parlour. The wordling is really similar to Manual Lymphatic Drainage, and is often followed by promises of “encourage fluid movement” or “before and after photos” but: Technique quality varies widely by practitioner. Some methods use deeper pressure and general strokes. It’s largely relaxation-focused, not always aligned with lymphatic anatomy. It isn’t generally part of evidence-based protocols for clinical conditions. In short, MLD is a clinically structured intervention; lymphatic massage is not. Indeed, who promotes Lymphatic massage as a service, often don’t know the pathway of the lymphatic system, and can’t tell you the difference between a Lymphoedema or a Lipoedema, and it may try to sell the fact that Lymphatic massage would detox your body (I will write a blog soon about this detox topic, as it is one of the biggest scam in the health and beauty industry). Side-by-Side: MLD vs Lymphatic Massage In the table below is a summary and a comparison between MLD and Lymphatic Massage features. Feature Manual Lymphatic Drainage (Vodder) MLD Lymphatic Massage Based on lymphatic anatomy ✔ ✖ Evidence-aligned technique ✔ ✖ Suitable for lymphoedema management ✔ ✖ Commonly used post-surgery ✔ ✖/varies Practised by trained therapists ✔ ✖ (wide variation) Relaxation / general wellness ✔ ✔ Clinical Evidence: What Research Shows About MLD and Lymphatic Massage As with any form of therapy, even in the case of MLD, the clinical research on MLD isn’t perfect, but the PubMed literature supports its role when used correctly within clinical programs. Lymphoedema Management A randomised controlled trial (RCT) reported that women with breast cancer–related lymphoedema experienced significant limb volume reduction and improved symptoms with MLD as part of therapy. A comprehensive systematic review found mixed outcomes but noted MLD’s accepted role in conservative lymphoedema treatment and generally positive effects on swelling and quality of life when integrated with other therapies. Inflammation & Post-Surgery Support MLD is also used, and clinical studies provide evidence in the setting of postoperative swelling and pain with orthopedic and cosmetic surgery. Indeed, post-surgery, the body responds with inflammation and swelling, which passes the acute phase, and the clearance of infections is better when moved to ensure the best recovery. Why MLD Is Clinically Preferred for Lymphoedema When lymphatic transport is impaired, as in lymphoedema or after surgery, the goal is not just temporary fluid “movement,” but supporting lymphatic drainage physiology. Here’s what clinical practice guidelines emphasise: Targeted Stimulation MLD uses gentle but precise hand movements that align with superficial lymphatic pathways and node groups. These are designed to: reduce interstitial fluid accumulation, activate lymphangiomotoricity, and facilitate fluid transport without trauma. This principle comes directly from the Vodder methodology as taught by the Vodder Academy. Part of a Larger Management Strategy Especially in lymphoedema, MLD is one component of a broader therapeutic approach that includes: ✔ compression therapy✔ movement and exercise✔ skin care and infection prevention This integrated strategy has been shown to improve outcomes more than any single therapy on its own. Post-Surgical Considerations As discussed in more depth in another blog, when heading for cosmetic and orthopaedic surgery, the recovery process is caractherised by an acute phase of swelling. That’s just teh body dping its thing. But, as we move away from the acute phase, it is essential to ensure that the oedema is reduced. That’s where MLD and compression therapy are essential. In fact, unlike a typical deep massage: MLD supports lymphatic flow without stressing fragile tissues. Studies show gentler lymphatic stimulation improves swelling and trismus after surgery. That’s why many rehabilitation specialists recommend structured MLD over general “lymphatic massage” in this context. So, What Should You Choose? As per everything, I reckon that your choice has to be aligned with your goal. Therefore: If you need clinical-grade lymphatic support for lymphoedema, post-surgical swelling, or ongoing fluid dysfunction, choose Manual Lymphatic Drainage (Vodder method) delivered by a trained clinician. If you want general relaxation and mild fluid support, a lymphatic massage in a wellness setting might feel nice — but it’s not a clinical substitute for MLD in these conditions. Conclusion From A Clinical Practitioner At Melbourne Massage and Treatment, Fitzroy North, I integrate MLD with evidence-based clinical reasoning, and not just as a “feel-good massage.” My approach is rooted in training with the Vodder Academy and ongoing lymphoedema therapy practice. If you’re concerned […]
Along with many types of post-cosmetic surgery presentations I get to work with, Rhinoplasty can also present with facial swelling, which is one of the most common (and often most frustrating) parts of post-surgery recovery. While you may find many therapists claiming to work with lymphatic massage, as a therapist trained in Manual Lymphatic Drainage (MLD) through the Vodder Academy, I can help you achieve great results post surgery and help your body deal with excessive swelling, bruising, and, where it happens, even fibrosis. I So in this article, I want to explain why swelling can last longer than expected after rhinoplasty, what the science tells us, and how MLD may help reduce swelling and limit the development of fibrosis during the healing process. Why Does Swelling Persist After Rhinoplasty? Rhinoplasty is a surgery that can be done for cosmetic or functional reasons, like improving nasal breathing, and is a surgical procedure that involves deliberate trauma to bone, cartilage, and soft tissue. This trauma triggers inflammation and a temporary disruption of the lymphatic system, the network responsible for clearing excess fluid from tissues. Scientific research published in the Plastic and Reconstructive Surgery Journal shows that: Approximately two-thirds of post-rhinoplasty swelling resolves within the first month Up to 95% resolves by 6 months Residual swelling can still be present 12 months or longer, particularly in the nasal tip. Now, two things about those data: Those numbers are the results of a study done on 40 patients, so still, even if they are quite promising, more evidence is welcome for further comparison. On the other hand, this prolonged swelling is a normal physiological response, but it can be uncomfortable and visually concerning. The Role of the Lymphatic System in Facial Swelling The swelling that you may present with post-rhynoplasty surgery is due to a temporary impairment of the lymphatic system, which acts as the body’s drainage mechanism. After surgery, lymphatic vessels can become overloaded or temporarily impaired, leading to fluid stagnation in facial tissues. In another paper by Meade R et al. (2012), published in the Oxford Academic Journal, it is shown that postoperative facial surgery disrupts lymphatic flow, leading to prolonged edema in the head and neck region. In more chronic cases, where lymphatic fluid stagnates for prolonged periods, patients may also experience tissue hardening and early fibrosis. What Is Manual Lymphatic Drainage (MLD)? Manual Lymphatic Drainage is a gentle, non-invasive manual therapy designed to stimulate lymphatic vessels and redirect fluid toward functioning lymph nodes. Unlike remedial massage or deep tissue techniques, MLD is a post-surgical lymphatic massage characterised by: Light Pressure Slow and rhythmic Movements MLD aims to stimulate superficial and deep lymph vessels, not muscle tissue MLD is internationally recognised as part of Complete Decongestive Therapy (CDT), the gold-standard conservative treatment for lymphatic swelling. Lasinski B.B. et al. (2012). How MLD May Help Reduce Swelling After Rhinoplasty As mentioned above, the number of patients who undergone clinical trials for post-rhinoplasty swelling treatment is limited, but along with other studies available on PubMed, the physiological principles of MLD are well supported, and here is a breakdown of what you can come across while doing some research: Supporting Fluid Reabsorption By stimulating lymphatic flow, MLD helps the body clear excess interstitial fluid more efficiently, which may assist in reducing facial puffiness and pressure. Marxen T. et al. (2023). Improving Tissue Mobility Reduced fluid stagnation helps tissues remain softer and more pliable during healing, an essential factor for aesthetic outcomes. Masson I. et al. (2014). Encouraging Symmetrical Healing MLD techniques can be adapted to address asymmetrical swelling, which is very common after rhinoplasty. Ulu M. et al. (2025) MLD and the Prevention of Fibrosis When the body goes through severe trauma, like a surgery, as part of its natural reaction, it may build tissue under the skin. This tissue is called: Fibrosis. Fibrosis may feel firm to the touch and leave you with a feeling of tightness under the skin. When swelling is unattended, can leads to fibrotic formation and changes. In this clinical study by Masson I. et al. (2014), they looked into post-liposuction and body contouring surgery, and how Manual Lymphatic Drainage, particularly when combined with other conservative therapies, can reduce both swelling and tissue fibrosis. While facial tissues differ, the underlying biological mechanism is shared: improved lymph flow supports healthier tissue remodelling. When Can MLD Begin After Rhinoplasty? Timing is crucial, but MLD post- rhinoplasty should only begin: With surgeon approval Once acute inflammation has stabilised Using facial lymphatic drainage massage protocols appropriate for post-surgical tissue Once the antibiotic cycle is finished, and the risk of infections is no longer there anymore At Melbourne Massage and Treatment in Fitzroy North, I tailor each session based on: Surgical date Healing stage Tissue sensitivity Presence of swelling or firmness MLD is not a painful treatment, and it doesn’t matter how sensitive your skin is, or how good you are at tolerating pain, still, throughout the treatment, pain should not be experienced, as this would lead to increased inflammation, which is not what we need, when clearing off exceed lymph liquid to reduce oedema post-surgery. My Approach With MLD at Melbourne Massage and Treatment – Fitzroy North As a Vodder-trained MLD therapist, my focus is on precision, safety, and evidence-informed care. Each session is: Gentle and non-invasive Individualised to your healing phase Focused on supporting natural lymphatic recovery Most clients benefit from a short series of treatments over several weeks or months, depending on swelling persistence. Nothing can boost your healing, whether you went through a cosmetic surgery or just had a severe incident, but there are certain practices, like MLD or exercises, and even good food and plenty of rest, that can help in assisting your healing process and not make it worse or longer. <div class=”faq-accordion”> FAQs: </div>
As a therapist who works with Lymphatic Massage in Fitzroy North and post-cosmetic-surgery patients, I often get asked, “What’s the difference between MLD and Brazilian lymphatic drainage?” To answer this question, I often have to give people a background of my training as a Lymphatic Drainage therapist and what is happening to their body post-liposuction. What are the differences between Vodder MLD and Brazilian Lymphatic Drainage Vodder MLD, which is the therapy I offer for post-cosmetic surgery and also Lymphoedema management, is a very light, rhythmical, skin-stretching technique. It has about 100 years of history, and it has a strong research base for lymphedema management and is useful in postoperative recovery, either in cosmetic or orthopedic surgery. Brazilian lymphatic drainage, on the other hand, tends to be firmer, more continuous, and pragmatically geared toward reducing swelling and bruising after cosmetic procedures, but it has less scientific evidence to support any benefits. For post-cosmetic surgery lymphatic massage (liposuction, abdominoplasty, facelifts, tummy tuck…) I would strongly recommend gentle Vodder-style MLD, and here is why: Any surgery, including cosmetic surgery, is highly invasive for the body, and therefore, you will present post-surgery with High skin sensitivity Swelling and bruising Pain A gentle approach, as Vodder MLD, would allow: Reduce the swelling with a pain-free approach Take away exceeds inflammation Help reinforce skin sensitivity As the healing process progresses and you move from the acute to the sub-acute healing phase (week 2 to week 3), we can start applying stronger pressure to break down fibrosis. What people call “Brazilian Lymphatic Drainage” “Brazilian lymphatic drainage” (BLD) is a manual therapy that is getting famous thanks to social media presence and some influencers talking about it. It is a practice which often refers to faster, more continuous wave-like movements and sometimes firmer pressure than Vodder MLD, and involves the usage of oil too. Those who offer Brazilian Lymphatic Drainage claim a faster recovery after aesthetic procedures (reducing bruising, local oedema, and tissue stiffness), even though clinical literature that looked into BLD in aesthetic and post-op settings, like randomised trials, describes this technique as debatable, and furthermore, the evidence of its efficacy is limited compared with Vodder studies. What does the research say? Systematic reviews on MLD (Vodder used often) show MLD is commonly used for decongestive therapy in Lymphoedema patients. The quality of the evidence varies, while effect sizes are moderate for some outcomes. Randomised trials that compare Vodder MLD with other modalities (e.g., compression, pneumatic compression) report benefit for symptoms and arm volume in breast cancer-related lymphedema and postoperative swelling in some surgical contexts. An early RCT explicitly used the Vodder technique and showed benefits in arm lymphedema management. Recent reviews and clinical articles regarding plastic-surgery literature highly support the use of postoperative lymphatic massage. The recommendations are to receive MLD one to three times a week, in the early recovery phase, for reducing swelling, pain, fibrosis and improving comfort. That said, often that information is shared by the surgery clinic staff after the surgery; therefore, it’s always better to choose a clinic that is clear and transparent about the post-surgery recovery, and not only about the surgery itself. When looking for studies about the Brazilian Lymphatic Drainage massage, it is hard to find something that is specific enough about this technique, and that doesn’t mix data and trials with other techniques, like bandaging and exercises. Therefore, it’s hard to evaluate the quality of this technique in terms of the RCT protocols. MLD – What works for what? Practical comparison For lymphedema (medical swelling after lymph node removal/cancer). When someone presents with lymphedema, the best choice is Vodder-style MLD as part of complete decongestive therapy. I don’t do this recommendation only because I offer this service, and I know its potential, but also because Most RCTs and meta-analyses have evaluated MLD (in Vodder style) as the safest and evidence-based treatment that has enough relevance for this type of presentation. For early post-operative care after cosmetic procedures (e.g., liposuction, abdominoplasty, facelifts, tummy tuck). In any given surgery, along the acute phase, the body is a high state of inflammation and the site of surgery would be delicate to touch for several weeks post surgery, indeed a gentle approach to the area is highly recommended, so Vodder-style MLD is way safer compare to Brazilian Lymphatic Drainage, because the tissues are fragile; MLD at this stage in time, it would helps reduce oedema and bruising and promotes comfort. Many plastic surgeons recommend MLD early and frequently in the first 2–6 weeks. Later phase (2–6+ weeks): While healing is progressing and you step into a sub-acute phase of recovery from the post-cosmetic surgery, firmer or more targeted techniques, which recall what Brazilian Lymphatic Drainage can be used to address residual fibrosis/stiffness, always with the surgeon’s clearance. That said When dealing with post-cosmetic surgery fibrosis, even Vodder MLD would include firm pressure. That’s how fibrosis is broken down. For general wellbeing, detox/relaxation, cellulite or fluid retention Gentle MLD (Vodder) is great for relaxation, reducing mild fluid retention, and supporting circulation without soreness. Good for regular wellness maintenance. Brazilian-style DLM is often used in aesthetic clinics for body contouring and cellulite care; people report feeling less heaviness and faster visual improvement, but the high-quality evidence is more limited, and outcomes vary with practitioner technique. MLD Safety & Contraindications – What You Need To Know In my practice, I am selective about who I offer MLD, especially after cosmetic surgery, and here is what I would look out for: Active infection Uncontrolled heart failure Acute deep vein thrombosis (DVT) Untreated cancer without clearance Fever Recent major bleeding or unstable medical conditions Liver or Kidney conditions After cosmetic surgery, you have to make sure to follow the surgeon’s recommendation about antibiotic intake, and or other medications. MLD can not start unless you are cleared of all the above. So, which do I recommend, Vodder or Brazilian Lymphatic Drainage? It is now quite clear that at Melbourne Massage and Treatment, for MLD, either […]
Functional movement is all those types of movement that you may have been training at the gym, like a squat, but really, those movements are what we are designed to deliver daily. Per the squat, think about sitting. Now, if you are young and fit, you may not need a great deal of mobility to sit on a chair, but as we get older, if we don’t train to maintain this form of mobility, things can really get difficult, and the risk of injury would increase. That’s where Myotherapy can really help you to understand which joints need more work in terms of mobility, but also which muscle groups you need to train to keep your stability at doc, so that your functional movement, especially when done under load, is going to be safe and with less risk of injury. What Is Myotherapy? Myotherapy is a form of manual therapy that focuses on assessing, treating, and managing musculoskeletal pain and dysfunction. At Melbourne Massage and Treatment in Fitzroy North, I use techniques such as deep tissue massage, joint mobilisation, myofascial release, dry needling, and corrective exercise to restore normal movement and prevent pain from returning. What I love about being a Clinical Myotherapist is that when working with my clients, I have to deliver a tailored treatment plan, as everyone is different and everyone presents with a unique body, which may need a different approach to reach the same goal. All this, starting from joint mobility and stability. Why Joint Mobility and Stability Matter Let’s start by defining what mobility and stability are: Mobility: the ability to move through a full range of motion Stability: the control that keeps your joints aligned to the body plane and supported To move well under load and deliver safe exercises, you must have good mobility and stability where needed. For example, if your hips lack mobility, your lumbar spine might compensate, creating discomfort and increasing the injury. Furthermore, a lack of mobility, it means you can not fully engage your muscle fibres, as less movement means less contraction or elongation of the muscle fibres involved in that movement, so less power and less growth. On the other hand, lack of stability is given from your lumbar area, which is not able to support a heavy load, and that’s how you can hurt your back. How Myotherapy Enhances Functional Movement Here at my clinic in Fitzroy North, as a clinical myotherapist I focus on helping you restoring balance through a whole-body approach. Here’s how Myotherapy helps: Comprehensive Movement AssessmentLet’s start with assessing posture, joint range of motion, and functional movement patterns to identify restrictions or weaknesses. Addressing the Root Cause of PainPain is central nervous system response to something that doesn’t work at is best. It may be an injury, or it may be a sensitization of the area. As a clinical myotherapist I help you break the cycle of compensation and discomfort, allowing more efficient, pain-free movement. Improving Joint MobilityUsing targeted soft tissue therapy, myofascial release, and gentle joint mobilisation, we help reduce tightness and restore freedom of movement across affected joints and muscles. Building Joint StabilityOnce mobility is restored, we focus on improving control and strength. Personalised exercises activate stabilising muscles, enhancing balance and coordination to prevent re-injury. Long-Term Support and EducationAfter every appointment I ensure to leave a detailed PDF file with the exercises we look into, so that you are able to reproduce our work at home or at your gym. But for every question, and for your progressions, I am always here ready to help. Who Can Benefit From A Myotherapy Session? Myotherapy is suitable for people of all activity levels. At our Fitzroy North practice, I regularly help clients dealing with: Muscle tightness or restricted joint movement Neck, shoulder, or lower back pain Postural strain from office work Sports or exercise-related injuries Limited flexibility affecting daily performance The Takeaway on Myotherapy and Functional Movement To improve your functional movement starts working on the right balance between joint mobility and stability. Myotherapy offers a targeted, evidence-based way to achieve that balance, and I am here helping you move better, feel stronger, and prevent future injuries. If you’re ready to enhance your movement and reduce pain, book a Myotherapy session at Melbourne Massage and Treatment, Fitzroy North today. Let’s get your body moving the way it’s meant to. And if you have any question, please use the form below to reach me out:
Exercise is the ultimate medicine for longevity and well-being. That said, there are different ways to exercise, and you should choose which one based on your goals and needs. Ultimately, even if you will prioritise one type of exercise over others, training in different ways, it is the best option to build resilience, strength and obtain the best results. But what are these main ways of training? Well, in this blog, we are talking about Strength Training and Hypertrophy. At Melbourne Massage and Treatment in Fitzroy North, I help people achieve this goal, with tailored injury recovery Myotherapy plans that may start with hands-on treatment but aim to get the person moving and moving under load. What Is Strength Training? Strength training, in its pure form, is a type of training that aims to improve the body’s ability to produce maximal force. This is possible by optimising the nervous system’s capacity to communicate to the muscles what action has to be delivered when placed under load. In fact, the goal isn’t necessarily to make muscles bigger, but to make them stronger. Here is a breakdown of what a strength training session would be like: Typical rep range: 1–6 repetitions per set Load: Heavy (80–100% of your one-rep max) Rest periods: Longer (2–5 minutes) Primary outcome: Improved neural efficiency — your brain and muscles learn to work together more effectively. This type of training benefits everyone, from athletes to everyday movers, by: Enhancing joint stability Improving bone density Increasing functional power for daily tasks. What Is Hypertrophy Training? Now, we will examine another form of training that aims to increase muscle size. Indeed, hypertrophy focuses on creating controlled muscular fatigue that stimulates growth in the muscle fibres. Here’s how it works: Typical rep range: 6–12 repetitions per set Load: Moderate (60–80% of your one-rep max) Rest periods: Shorter (30–90 seconds) Primary outcome: Increased muscle cross-sectional area (growth). Hypertrophy is popular for aesthetic goals, but it also has significant benefits for: Joint support Posture Injury prevention, especially when paired with proper mobility and recovery practices like myotherapy. Who Would Benefit from Strength and Hypertrophy Training? Let’s be clear that both styles of resistance training can benefit a wide range of people — not just athletes or bodybuilders. But here is a clearer breakdown of which training belongs to which goals: You’ll benefit from strength training if you: Want to improve performance in sports or daily activities that require lifting, pushing, or pulling. You are seeking to increase bone density and joint stability, especially as you age. This is a big one for menopausal women. Need to enhance posture and core control to reduce the risk of back or shoulder pain. Are recovering from injury and looking to restore functional movement patterns safely under guidance. You’ll benefit from hypertrophy training if you: Want to build muscle mass for aesthetics, strength, or body composition. You are addressing muscle imbalances or weaknesses identified during myotherapy assessments. Need more joint support and stability through improved muscular structure. Aim to boost metabolism and energy expenditure through increased muscle tissue. At Melbourne Massage and Treatment, I often integrate tailored exercise advice with fitness class sessions, helping clients find the right balance between strength, mobility, and recovery for their individual goals. Massage Therapy, Dry Needling, and the Role of Passive Treatment Massage therapy, dry needling, and other forms of passive therapy are valuable tools during the recovery phase of an injury or when pain and tension are high. They help by: Reducing muscle tension and spasm Improving blood flow and assisting with tissue healing Calming the nervous system and reducing protective muscle guarding Restoring short-term mobility to prepare the body for movement At my Fitzroy North clinic, these treatments are often used early in a client’s recovery journey to reduce pain and restore comfort. However, while these therapies are excellent for short-term relief and acute recovery, they must eventually be paired with movement under load to create lasting change. Why Movement Under Load Is Essential for Long-Term Wellness Passive treatments can help you feel better, but loaded movement enables you to function better. When you progressively load muscles, tendons, and joints, your body adapts and becomes stronger and more resilient. This is what keeps pain away in the long term. Here is a practical and simplified explanation: “You have to think that the body, while it does age, it does slow down in any form of its metabolism, including the regeneration of tissues, which gets worn down, and finds it difficult to be regenerated. This is where movement under load plays a crucial role. Movement under load indeed, it is the stimulus that the central nervous system needs to maintain the body’s regeneration active and effective”. A further breakdown of why movement under load matters beyond recovery: Builds tissue resilience: Strengthens muscles and connective tissue to handle daily demands. Supports nervous system retraining: Teaches your body to move efficiently and safely. Improves joint health and posture: Strengthens stabilising muscles that protect joints. Reduces recurrence of pain: Prevents the same issues from returning by addressing root causes, not just symptoms. Another way I would express the difference between passive therapy and exercises (under load) to my patient is: “Massage and needling help you feel good now, but movement under load helps you stay good later.” That’s why our approach combines hands-on therapy to relieve pain with movement education and strengthening to keep you moving well long after your treatment. How Myotherapy Complements Strength and Hypertrophy Training Myotherapy is a form of manual therapy that aims to improve the performance of any individual who has gone through an injury or someone who wants to maintain functionality and wellbeing. In a Myotherapy session, we would start with some form of testing to evaluate the person’s capacity in mobility and strength and from there we create a treatment plan that aims to improve the current presentation. A treatment plan may include: Soft tissue therapy Corrective exercise Movement assessment Goals of myotherapy: Address muscular imbalances […]
Experiencing a vertebral fracture can be an overwhelming and challenging experience to recover from, but this doesn’t mean there is no safe protocol and successful treatment pathway out there. At Melbourne Massage and Treatment, I am here to assist you in this complex journey, which could be by offering MLD treatment, Myotherapy or Fitness Class. But let’s first understand what fractured vertebrae mean, and what we have to be aware of when working with this type of injury. Spinal Damage vs. No Spinal Damage Let’s start to look into what difference makes to have a spinal fracture where the spinal cord was injured and where it was not. With spinal cord damage, a fracture may injure the spinal cord or nerves, leading to severe symptoms such as numbness, weakness, or paralysis. These cases are medical emergencies requiring hospital care. The rehabilitation process for someone who encounters spinal damage varies based on the severity of the injury. Surgery may be necessary to repair the nerve, but there is also the fact to consider that there may not be a recovery option and life paralysis (quadriplegic or paraplegic) as an outcome. Without spinal cord damage, it is a result of a bone fracture only, without affecting the cord. These are painful but often managed with an initial period of rest and bracing and gradual rehabilitation. At our Fitzroy North clinic, Giovanni carefully assesses your needs and works alongside your medical team to provide safe and effective rehabilitation. Cervical, Thoracic, and Lumbar Vertebrae Your spine has three main regions, and fractures behave differently depending on location: Cervical (neck): Mobile but delicate; fractures here can have severe consequences. Thoracic (mid-back): Stabilised by the rib cage, but injuries here often come from higher-energy impacts. Lumbar (lower back): These vertebrae carry the body’s weight, so fractures here cause significant pain and restricted movement. Based on where the fracture is, the treatment and recovery options and plans differ. Scans for Diagnosis To properly understand the type of fracture and the severity of the fracture itself, scans are essential. Here is a short list of what diagnostic scans are available and which are most commonly used, and why: X-ray: The first step to confirm a fracture. This type of test is good to see the fracture at the bond level; it is quick, but as a downside, it exposes you to radiation. CT scan: Provides detailed 3D imaging to assess the fracture’s stability. The downside of a CT scan is that, as it is based on X-Ray technology, it can still expose you to radiation, and it can take longer to be delivered, and it is essential to be lying down while receiving the scan. MRI scan: Compared to X-Ray technology, MRI scan would not expose you to radiation, and is used to detect any involvement of nerves, discs, or the spinal cord along the fracture, as this type of scan is used for water-based tissue in the body, and not bones. These scans help guide safe rehabilitation, ensuring the right treatment approach from day one. Something else to keep in mind from the result of the scan is that not everything that a scan shows must impact your life. Indeed, a building disk may show in your scan, but that doesn’t mean that that specific pathology is something related to your spine fracture (it may have been there already before), and that doesn’t mean the body would not look after it while you are recovering from the spine injury. Types of Vertebral Fracture Common fracture types include: Compression fracture – vertebra collapses, often linked to osteoporosis (also called a wedging fracture). Burst fracture – bone shatters outward, sometimes threatening the spinal cord. Flexion-distraction fracture – usually from high-speed accidents where the spine bends suddenly. Fracture-dislocation – bone and soft tissues are displaced, often requiring surgery. Avulsion – It is a type of stress fracture, characterised by a small piece of bone pulled away from the main bone by a muscle or ligament (typical along the transverse process). Mechanism of Injury Fractures can occur from: High-energy trauma – car accidents, falls, sports collisions. Low-energy stress – in osteoporosis, even coughing or bending can trigger a fracture. Scheuermann’s disease – in this specific condition, the vertebrae may grow at different heights compared to the sagittal plane. A meticulous clinical history intake can help in figuring out he chance of you suffering from a vertebral fracture. Healing Time and Recovery As per all non-complex bone fractures, most vertebral fractures take 8–12 weeks to heal, even if recovery varies depending on age, bone health, and whether surgery was required. What we know is that nothing can actually boost the healing, but different therapies, active and passive, can help in assisting the healing process, ensuring a positive outcome. What then can be done during the recovery time is: Early phase: Pain management and protection of the fracture. Rehabilitation phase: Gentle guided movement, strengthening, and improving mobility. With myotherapy support, clients can return to safe daily activities while minimising the risk of re-injury. What to Avoid in the Early Stages of a Vertebral Fracture As mentioned earlier, in the early stage of vertebral fracture, it is important to prevent further damage to the spine and wear a corset that helps in stabilising the spine, while the body is starting the calcification of the bone. Even though you may wear a support, you will want to avoid: Heavy lifting, twisting, or bending movements. Prolonged sitting without support. High-impact exercise or activities. Movement is still recommended, as it can still promote fluid movement and relaxation. Therefore, it is possible to go for walks, move your arms, and move your legs even if in a seated position. Manual Lymphatic Drainage Massage in the Early Phase of a Vertebral Fracture At Melbourne Massage and Treatment, I got to offer MLD as a form of treatment for relaxation, which can have a positive impact on pain perception and tension relief from the spine area. MLD is a gentle […]
Within the last few years, cosmetic surgeries have been on the rise in Australia. These types of interventions can be helpful for quick body changes. Still, the recovery process post-surgery is often under-estimated and misinterpreted, especially when, past a couple of days or just a few weeks, the body’s response to surgery leaves behind hard lumps, thick skin, and reduced sensitivity. The thought skin and lumps are simply fibrosis, and the reduced sensitivity results from damaged nervous system endings. At Melbourne Massage and Treatment in Fitzroy North, I specialise in Manual Lymphatic Drainage (MLD) using the Vodder technique, helping clients reduce swelling, assisting the recovery, and breaking down fibrosis post cosmetic surgery, safely and effectively. If you’re looking for post-surgery care in Fitzroy North or Melbourne, here’s how MLD can support your recovery and improve your results. What is Fibrosis After Cosmetic Surgery? Fibrosis formation post cosmetic surgery is the result of tissue damage that occurred during the surgery. When going for an intervention like liposuction, where fat is removed from the body (either at the abdominal level, arms or legs or elsewhere), the body, to replace the void left by the fat removal, builds up fibrotic tissue. The fibrotic tissue is mainly made of collagen. While this reaction is natural, it can often cause: Hard lumps or nodules under the skin; Uneven skin contour or texture; Tightness or restricted mobility; Tenderness or discomfort. There is no real way around those types of side effects post-liposuction, at least in the short term, and the body would take weeks to recover fully (up to 3 months). That said, everybody reacts differently to this type of intervention, and based on the type of intervention received, the recovery process can vary. Who Benefits Most From Lymphatic Drainage Massage After Cosmetic Surgery? Here is a short list of cosmetic surgery interventions that are going to leave you with fibrosis in the post-surgery time, and that would benefit from Lymphatic Drainage Massage intervention: Liposuction (abdomen, thighs, arms, chin) – This includes liposuction for Lipoedema management too. Tummy tuck – Either due to post-liposuction or from severe weight loss. Breast surgery (augmentation, reduction, reconstruction) – If this is due to breast cancer, one should be aware of any risk of Lymphoedema development. Facelifts and neck lifts Brazilian Butt Lift (BBL) – This type of intervention requires fat to be removed from other body parts, as the abdomen, and that’s where fibrosis would build up. How MLD Helps Reduce Fibrosis Manual Lymphatic Drainage (MLD) is a gentle, specialised technique that stimulates the lymphatic system to clear excess fluid, reduce swelling, and assist with the healing process. After surgery, your lymphatic system could be damaged and can struggle to keep up with its work, and that’s where MLD makes a big difference. Indeed, the stimulation of the Lymphatic System, via MLD therapy, can help in assisting your recovery and ensure that the fibrotic tissue gets absorbed and dismissed, restoring freedom of movement and leaving you soon after treatment in a deep relaxation state. I trained in the MLD with the Vodder style, therefore I can provide precise, tailored treatments that are safe for sensitive post-operative tissue. Book your post-surgery lymphatic drainage in Fitzroy North today to safely reduce fibrosis. When Can I Start MLD Treatment Post Cosmetic Surgery? Generally, MLD is safe to start as soon as the antibiotic cycle is ended post-cosmetic surgery. Given the light touch of this type of therapy, we aim to produce no pain during the treatment, so we can work close to the surgical side, without affecting the recovery process. On the other hand, I found myself occasionally referring patients to the local nurse or GP here at Fitzroy North Doctors, as their recovery immediately post-surgery was compromised by misleading suggestions and procedures offered by overseas cosmetic clinic surgery. If you are not sure about what’s going on with your recovery, please, before placing a booking for an MLD treatment, talk to your GP about your recovery state, and if you have any questions regarding MLD treatment, you can always reach out to me via the contact page. How Many MLD Sessions Do I Need To Reduce The Fibrosis? As mentioned earlier, everyone responds differently to cosmetic surgery, but in my experience, it would take at least 4 to 6 weeks to start seeing a significant difference in fibrous tissue presence. That said, the number of sessions and the time length of the sessions can vary, based on the area where you received the surgery. Abdominal surgery only: I will recommend 2 to 3 treatment per week, for the first 3 weeks. Within the first week, we may spend 1 hour per session, and from the 2nd week onwards, we reduce the treatment to 45 minutes. Multiple liposuction sites: as there are multiple areas where you received a surgery, we may need to extend the time of treatment up to 1 and a half hours initially, or go for multiple sessions, each for a different area. The first few treatment may take longer as we want to spend some extra time trying to break down the fibrosis with a gentler touch, due to the high sensitivity of the body, which is high due to post-surgery. As the sensitivity decreases, and we can apply further pressure, we can achieve the same result in fibrosis reduction with less time. If you are not sure what works best for you, you can book a 15-minute free online consultation, so we can discuss your needs and work out a treatment plan in accordance with them. MLD Prices in Fitzroy North All my services are offered at the same rate and are as follows: 90 mins – $175 1 hour – $125 45 mins – $ 115 30 mins – $90 All those prices are inclusive of GST. The 90-minute option is available only if required, and not via the booking system. Why Choose MLD at Melbourne Massage and Treatment in Fitzroy North? Not all lymphatic […]