Bone density is a key factor in bond fracture prevention. Bone is made of cells that die and regenerate. When this process is compromised, the risk of fracture arises. During the early stages of life, we can ensure that we intake and store calcium through food to build up our bones, but after a certain age (about 30), the body stops absorbing calcium, and the storage that we created is now our reserve for the rest of life. Cell Regeneration in Bone and Other Body’s Tissues The body’s cells, like muscle cells, skin cells, tendon cells, ligament cells and even bond cells, are in constant change via a process called cell regeneration. Old cells die off and they get replaced with new cells. In the case of bone, the cells that allow this process to happen are called osteoblasts. While we age, this process slows down, meaning that cells would still die, but they don’t get replaced. A typical example is a woman going through menopause. Estrogen, which is the hormone responsible for bond metabolism, allows the activity of osteoblasts. During menopause, indeed, women have a drop in Estrogen production, and osteoblasts are not as operative as they used to be. Strength Exercises and Cell Regeneration As this meta-analysis shows, strength exercises are a positive stress stimulus for the body and can help the osteoblast work harder and maintain bone cell regeneration. When the body perceives stress as physical resistance, it does its best to establish a reparation mechanism. So whenever we pick a weight against gravity, the body would implement a regeneration of the tissue that are used to complete this action. Who Is at Risk of Losing Bone Mass? There are several factors that can contribute to decreased bone mass: Age: Bone density typically peaks in early adulthood and declines with age. Gender: Women, especially postmenopausal, are at higher risk due to hormonal changes that accelerate bone loss. Family History: A family history of osteoporosis can increase risk. Body Size: Individuals with smaller body frames may have less bone mass to draw from as they age. Hormonal Levels: Thyroid imbalances and reduced sex hormones can lead to bone loss. Dietary Factors: Low calcium and vitamin D intake contribute to diminished bone density. Lifestyle Choices: A sedentary lifestyle, excessive alcohol consumption, and smoking are linked to weaker bones. I have included factors like dietary and hormonal levels in the above list. Bear in mind that taking supplements such as calcium and vitamin D (which helps retain calcium) could have severe contraindications. So, always talk to your doctor or specialist about the intake of supplements. How to determine Bone Density? To determine bone density, there is a diagnostic test called Dual-energy X-ray Absorptiometry (DEXA or DXA). This non-invasive procedure measures the mineral content in bones, usually in areas like the spine, hip, or wrist, to assess bone density and identify potential risks of osteoporosis or fractures. The results are given as a T-score, which compares your bone density to the average peak bone mass of a healthy young adult. A T-score of -1.0 or above is considered normal, while a score between -1.0 and -2.5 indicates low bone mass (osteopenia), and a score of -2.5 or lower suggests osteoporosis. Other methods, like ultrasound or quantitative computed tomography (QCT), can also assess bone density, but DEXA remains the gold standard for bone health evaluations. Mobility before strengthening So far, we have discussed how strength exercises are a good way to maintain bond density. Still, I would not recommend that anyone who is not into strength exercise and has bone density issues go and start lifting heavily. Why (?), you may ask. Well, before we start lifting heavy, we want to ensure that the body mechanics are optimal for it, so we better start looking into your mobility and then pass on to the strength part of things. Please be aware that mobility has nothing to do with elasticity or stretching. Those are different practices. How Can We Achieve Great Mobility For people who decide to take a journey to ensure an optimal level of mobility and then strengthen the body, the first step is to assess their joint mobility with active and passive range of motion. After that, we could use a combo of Myotherapy treatment and mobility exercises to ensure they can quickly pick up the best of their mobility capacity, given their subjective presentation. And here is a list of mobility exercises which we may look into at first: Hip Openers to improve range of motion in the pelvis and lower back. Ankle Drills to support proper weight distribution in weight-bearing exercises. Thoracic Spine Mobility Exercises to prevent excessive strain on the lower back. AC Joint External rotation to ensure we can build strong rotator cuff muscles, essential for shoulder health It Is Time To Strength. How Can We Do This? Once the minimum mobility is achieved, which may take 1 to 2 weeks of training, depending on each individual and their subjective history and effort, we can start looking into more strengthening exercises. So, here is a list of different exercises that can help with strengthening, written with the progressions to follow: Calf raises with double leg, single leg and weight Hamstring and Quads Curl that gets weight added as weeks go by Standing Adduction and Abduction at cable machine or with resistance bend Glut Muscles training at cable machine or with resistance bend Deadlift for back and posterior chain muscle strength Squat with weights and explosion variations Cuff rotator-specific strength is Ideal before stepping into more complex arm weight-lifting Cervical muscle strength to prevent cervical headache and sore neck All of those exercises, except the cervical one, can then be modified to achieve plyometric drills and combined movement. But this is a process that would take months, and there is no rush to get to it, as I want you to be safe throughout the entire journey. Integrating Exercise into Myotherapy Treatment At Melbourne Massage and Treatment, I incorporate […]
Tag Archives: exercises
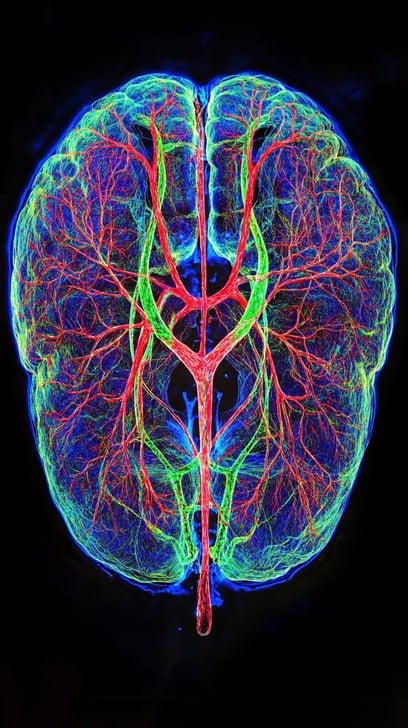
Alzheimer’s is a growing concern worldwide, affecting millions of individuals and their families. As we age, cognitive decline becomes a reality for many, but research has shown that regular exercise can play a significant role in reducing the risk of developing Alzheimer’s. Incorporating physical activity into daily routines can improve brain health, enhance memory, and support overall mental well-being. But how is this possible? And what do exercises have to do with brain health? What are the main factors that lead to Alzheimer’s disease? Even before starting to look into how exercises are beneficial for reducing the chance of developing Alzheimer’s, we have to understand what conditions can lead to Alzheimer’s in the first place. Indeed, there is a combination of factors that would increase your chance of developing this form of Dementia. Here is the list: low education level, midlife hypertension, midlife obesity, hearing loss, later-life depression, diabetes, smoking, social isolation, and, of course, low physical activity. Now, once you read this list, you can easily imagine how exercises can be beneficial for many of these presentations and how already acting directly on reducing these factors can lead to reducing your future chance of developing Alzheimer’s. How Exercise Benefits Brain Health Engaging in regular physical activity helps maintain cognitive function by improving blood flow to the brain. Indeed, the brain, as shown in the picture here, is a bundle of veins and arteries and has the most blood supply of any organ. As we now know, blood helps reduce inflammation and promotes the release of brain-derived neurotrophic factor (BDNF). BDNF is a protein that supports neuron growth and connectivity, which is crucial for memory retention and learning. On the other hand, exercise also helps reduce stress and anxiety, which are known contributors to cognitive decline. Additionally, studies like the London taxi driver study demonstrate how mental and physical engagement can grow the brain. The study found that taxi drivers who undergo rigorous memorization training developed larger hippocampi compared to bus drivers who followed set routes. This supports the idea that both physical activity and cognitive challenges contribute to brain resilience. Types of Exercises for Brain Health Different types of exercises offer unique benefits for brain function. Here are some of the best activities to help prevent Alzheimer’s: Aerobic Exercise: Activities like walking, running, cycling, and swimming increase heart rate and improve circulation, ensuring that the brain receives adequate oxygen and nutrients. Strength Training: Lifting weights or using resistance bands helps build muscle mass, which has been linked to better cognitive function and reduced risk of Alzheimer. Balance and Flexibility Exercises: Yoga, Tai Chi, and stretching improve coordination and reduce the risk of falls, which can contribute to brain injuries and cognitive impairment. Mental Engagement through Exercise: Activities such as dancing, martial arts, or playing sports require learning new movements and strategies, stimulating brain activity and improving neural connections. Metabolic and Lifestyle Factors Moving forward on the prevention side of things, there is to say that exercise alone is not the only factor influencing Alzheimer’s risks. Chronic conditions like pre-diabetes, diabetes, high LDL cholesterol, and chronic inflammation are significant contributors to cognitive decline. Studies show that individuals with uncontrolled pre-diabetes and high cholesterol in midlife face a greater risk of developing Alzheimer’s later on. A holistic approach to brain health should also address these metabolic pathways through a combination of exercise, a balanced diet, and proper medical management. How to Incorporate Exercise into Daily Life Nowadays I often hear patients saying that they have no time for exercise. But is that true? Or is it more about knowing how to optimise the time and apply some changes to our lifestyle? Then, here are some practical ways to integrate exercise into your routine: Take a brisk 30-minute walk daily. This can be easily accomplished by leaving the tram one stop earlier than your work’s stop and walking one stop back and forth, or parking the car a bit further away than the work location and walking your way down and back (15 mins each way). Join a local exercise class or sports group. If you give yourself a time and day that you have to attend a regular appointment, you are more luckily to make it a routine. Use stairs instead of elevators. If you work in a building with an elevator, opt for the stairs as many time as you can. Engage in gardening or household chores that require movement. Indeed gardening is not only a great way to spent time outdoor but it also a good way to move your body. Practice mobility drills before and after bedtime. Start and end yoyr day with a 10 minutes mobility self time, where you focus on get the spine moving and get your joint some selflove. How Melbourne Massage and Treatment can help with exercises for Alzheimer’s prevention? At Melbourne Massage and Treatment, I do my best to teach my patients exercises and guide them through a better lifestyle. Alzheimer’s disease is something that I experienced myself with my family throughout my mother’s journey. As I lived this in the first place, I want to make sure that no others have to go through the same journey. So not only do I regularly practice exercises myself, but I ensure to pass these skills and knowledge to others. If you are keen to learn more about how exercises can help your wellness journey, book now your next appointment for Exercises Prescription. Or if you have any questions, reach out via the contact page. FAQ about Exercises and Alzheimer’s prevention. Q: What are the main risk factors for developing Alzheimer’s disease? A: Several factors increase the likelihood of developing Alzheimer’s, including low education level, midlife hypertension, obesity, hearing loss, depression, diabetes, smoking, social isolation, and low physical activity. Addressing these risk factors through lifestyle changes can help reduce the chances of cognitive decline. Q: How does exercise benefit brain health? A: Regular physical activity improves blood flow to the brain, reduces inflammation, […]
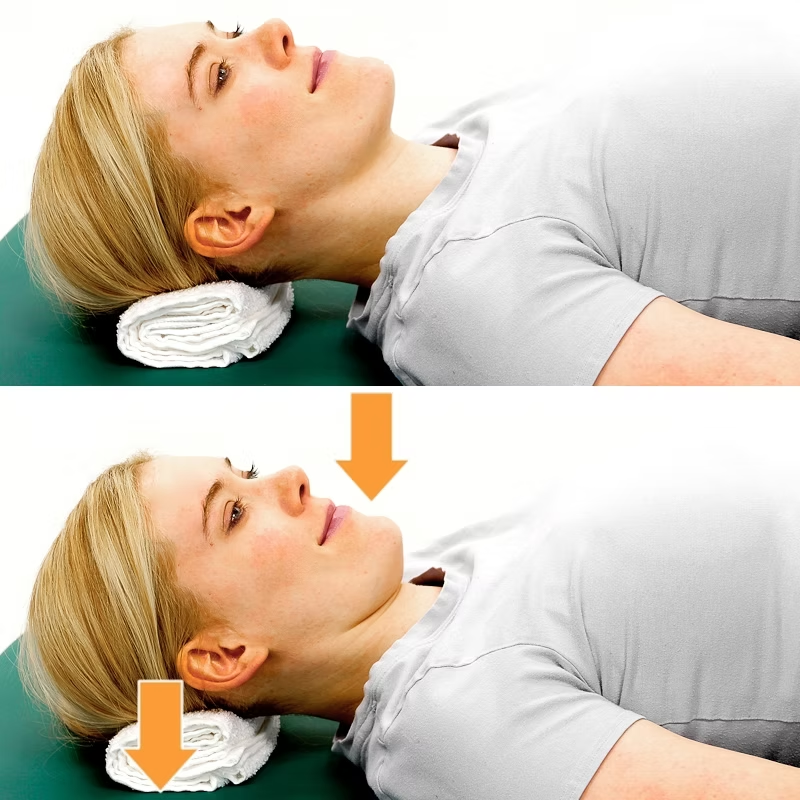
Whiplash is a common neck injury caused by a sudden and forceful back-and-forth motion of the head. We often see this in patients who go through a car accident, contact sports injuries (AFL, rugby or even Soccer), or falls. While whiplash is usually not life-threatening, we now know that it can cause persistent pain and discomfort, affecting daily activities. Therefore, it is important to understand its symptoms, causes, and the best exercises for recovery, which can help individuals manage and overcome this condition effectively. Common Causes of Whiplash Whiplash is a term used to describe a fast rocking motion of the cervical area and is most frequently caused by: Car accidents: Rear-end collisions are the leading cause, as the sudden force propels the head forward and backward. Sports injuries: Contact sports like football, boxing, or hockey but even AFL, Rugby or even Soccer increase the risk of whiplash injuries. Falls: Slipping and falling can cause the head to jerk suddenly, leading to whiplash. Physical assaults: Blows to the head or sudden jolts, such as those experienced in shaken baby syndrome, can result in whiplash. What are the consequences of Whiplash for the cervical ligaments? The consequences of whiplash for the cervical ligaments can be significant, leading to long-term instability and chronic pain. When the ligaments are overstretched or torn, they lose their ability to support the cervical spine, resulting in properly: Reduced Stability: Weakened ligaments can no longer provide adequate support to the cervical vertebrae, leading to excessive movement and an increased risk of further injury. That’s why stretching is not recommended either. Chronic Pain and Stiffness: Persistent discomfort may arise as the muscles attempt to compensate for the lack of ligament support. Increased Risk of Degeneration: Ligament damage can accelerate wear and tear on the cervical joints, potentially leading to conditions such as osteoarthritis. Neurological Symptoms: Instability in the cervical spine may irritate or compress nerves, leading to headaches, dizziness, or numbness in the arms. Symptoms of Whiplash Whiplash symptoms can range from mild discomfort to severe pain, and they often appear within hours or days of the injury. Common symptoms include: Neck pain and stiffness: One of the most prevalent symptoms, often worsening with movement. Headaches: Typically originating from the base of the skull and radiating toward the forehead. Shoulder and upper back pain: The impact can cause muscle strain in surrounding areas. Reduced range of motion: Difficulty moving the neck due to stiffness and discomfort. Dizziness and fatigue: A common reaction as the body copes with the injury. Tingling or numbness in the arms: Nerve involvement may lead to sensations of pins and needles. Cognitive issues: Some people experience memory problems, difficulty concentrating, and irritability. Those symptoms may not present all at once, and they can belong to other presentations, while whiplash did or didn’t happen anytime before. That’s why when we go through a clinical history taking, as Myotherapist, we take our time to dig into your past and your body habits, as this can give us important information about your current presentation and what we can do to improve it. Why Can Whiplash Become a Lifelong Issue? In some cases, whiplash can become a chronic condition due to the instability of cervical ligaments. Cervical vertebrae can be divided into two parts, Mobile and Stable joints. C1 to C2 are the mobile ones, whereas C3 to C7 are the stable ones. Now, if along a whiplash incident, the ligaments of either the mobile or, most luckily, the stable side get strained, the muscles surrounding that segment of the joint would have to work harder to maintain stability. This would lead to to ongoing discomfort, reduced mobility due to pain and muscle spasms, and increased vulnerability to future injuries. If left untreated or managed improperly, this is how the condition can become chronic and lead to other injuries along the way. Importance of Thoracic Mobility Thoracic mobility plays a crucial role in preventing the chain effect of mobility and stability issues between the thoracic spine, lower cervical, and upper cervical regions. If the thoracic spine is stiff or restricted, the lower and upper cervical spine must compensate, leading to increased strain and pain. Improving thoracic mobility through targeted exercises can help reduce this compensatory stress, allowing for better neck function and reducing the risk of chronic discomfort. In a case of a previous history of whiplash, maintaining good thoracic mobility would allow the cervical area to focus on its duties, so stability for the lower portion and mobility for the upper. Reducing the risk of overcompensation and muscle fatigue. Effective Exercises for Whiplash Recovery A structured exercise program is essential for whiplash recovery. This program should begin with isometric exercises to restore basic cervical movement, progress to concentric exercises to rebuild strength, and eventually include thoracic mobility drills to enhance overall spinal function. Phase 1: Isometric Exercises for Early Recovery. For the first 2 weeks post-injury, 5 to 7 days a week. Isometric exercises help activate muscles without excessive movement, providing a stable foundation for recovery. This step is essential to start driving more blood to the area irritated by the whiplash and also allow the central nervous system to feel confident in perceiving the cervical structure moving without pain. Isometric Neck Holds: Place your hand on your forehead and gently press against it without moving your head. Push only 25% of your strength, as it has to be a pain-free exercise. Hold for 5-10 seconds and repeat 5 times. These exercises can be done in any cervical movement, such as extension, lateral flexion, or rotation, by using your hand as a resistance and pushing always at 25% of your strength. The strenght of push does not ever progress, what you will progress within isometric exercises are the time fram of push, repetitions and sets. Phase 2: Concentric Strengthening Exercises. From week 3 post-injury onwards,3 to 5 times a week. Once the pain subsides, which we would expect to happen in 2 weeks about it, gradual […]
Greater Trochanteric Pain Syndrome (GTPS) is a common condition that causes persistent lateral hip pain, often making everyday activities like walking, climbing stairs, or even lying on your side difficult. GTPS primarily affects middle-aged individuals, particularly women, and is commonly linked to issues such as gluteal tendinopathy and weakness in the hip stabilizing muscles. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. GTPS Symptoms Greater Trochanteric Pain Syndrome can present with a series of symptoms that are local to the side of the hip. Here are the most common: Lateral hip pain: Persistent pain on the outer side of the hip, which may extend down the thigh. Pain when lying on the affected side: Discomfort that worsens when lying directly on the hip. Tenderness to touch: Sensitivity around the greater trochanter, which may be painful to press. Pain with movement: Aggravation of pain during walking, climbing stairs, or standing for prolonged periods. Weakness in hip muscles: Reduced strength in the gluteal muscles, leading to instability in movement. Difficulty sitting for long periods: Sitting on hard surfaces can exacerbate discomfort. Mechanism of Injury for GTPS GTPS is primarily associated with tendinopathy of the gluteus medius and/or minimus muscles, with or without accompanying bursitis. As per many tendon injuries, this condition often arises from repetitive stress or overuse, leading to microtrauma and degeneration of these tendons. On the other hand, abnormal hip biomechanics can exacerbate the issue, as compressive forces cause impingement of the gluteal tendons and bursa onto the greater trochanter by the iliotibial band during hip adduction. Contributing factors to GTPS include acute trauma, such as a fall onto the lateral hip, prolonged pressure from lying on one side, and overuse from activities like running or stair climbing. Additionally, conditions like iliotibial band disorders and gluteal muscle weakness can increase the risk of developing GTPS. Understanding these mechanisms is crucial for effective management and prevention of GTPS. Evaluation of GTPS Diagnosing GTPS typically involves a combination of clinical examination and medical history assessment. After taking your clinical history, including sports and work activity, I will perform a series of tests to validate the suspicions of GTPS. Those tests include single-leg stance and resisted hip abduction, which we would expect to show weakness in single-leg standing and pain during the abduction movement. Lastly, we would also palpate the area, which is a test that is kept for last because we want to avoid flair the presentation, which may be painful with any other test after that. In some cases, imaging techniques like ultrasound or MRI may be used to rule out other conditions and confirm gluteal tendinopathy or soft tissue abnormalities. I personally do not recommend image testing as the first way to go because the impact of seeing physical damage can also have a negative impact on self-perception, making a recovery harder. At Melbourne Massage and Treatment, our focus is on evidence-based approaches to managing GTPS, and the latest research strongly supports the role of exercise as the first line of treatment for this condition. The difference between GTPS and Femoroacetabular Impingement (FAI) The difference between GTPS and FAI stands in the hip area involved in the injury. The GTPS is relative to the side of the hip and involves the gluteus medius and minimus tendon and the bursa that separate that tendon from the greater trochanter of the femur. On the other hand, FAI is a presentation that still involves the hip, but it does take place on the anterior portion of the hip, as is characterised by and overgrowth of tissue on the femur head or the hip socket, and it does manifest with hip flexion and external rotation. That’s why it is important to receive an evaluation of the presentation from a professional, in order not to mix the two presentation, or also, in order to evaluate if both presentation are present at the same time, which can also happen. The Role of Exercise in GTPS Treatment A recent systematic review and meta-analysis analyzing multiple randomized controlled trials found that structured exercise provides significant benefits for individuals with GTPS. The findings revealed that: Long-term pain reduction: Exercise can lead to slight but meaningful reductions in hip pain over time. Improved physical function: Patients who engage in targeted exercise programs experience better mobility and overall hip function. Increased likelihood of meaningful recovery: Compared to corticosteroid injections, exercise significantly increases the chances of noticeable improvement in symptoms. One of the most notable takeaways from this research is that exercise has a long-lasting effect, whereas treatments such as corticosteroid injections may provide only short-term relief. Additionally, no serious adverse effects were reported with exercise-based interventions, making it a safe and sustainable approach to managing GTPS. Why Choose Exercise Over Corticosteroid Injections? Corticosteroid injections have often been used for GTPS pain relief, but the research indicates that exercise leads to better long-term outcomes. While injections may offer temporary symptom relief, they do not address the underlying causes of GTPS, such as gluteal muscle weakness or tendon dysfunction. Exercise, on the other hand, strengthens the hip muscles, improves joint stability, and reduces the likelihood of recurring pain. In a previous blog post, I spoke about the key role of Gluteus Medius as a pelvis stabiliser. Effective Exercises for GTPS At Melbourne Massage and Treatment in Fitzroy North clinic, I design individualised exercise programs to help patients with GTPS regain strength and function. Some of the most effective exercises for GTPS include: Isometric exercises involve holding static positions to engage the hip muscles without excessive movement, reducing pain and improving muscle endurance, driving blood to the tendons and joints, helping with recovery. Strength training: Progressive strengthening of the gluteus medius and minimus muscles to enhance hip stability. Functional movement training: Exercises that mimic daily activities to help improve movement patterns and prevent pain triggers. Along those exercises […]
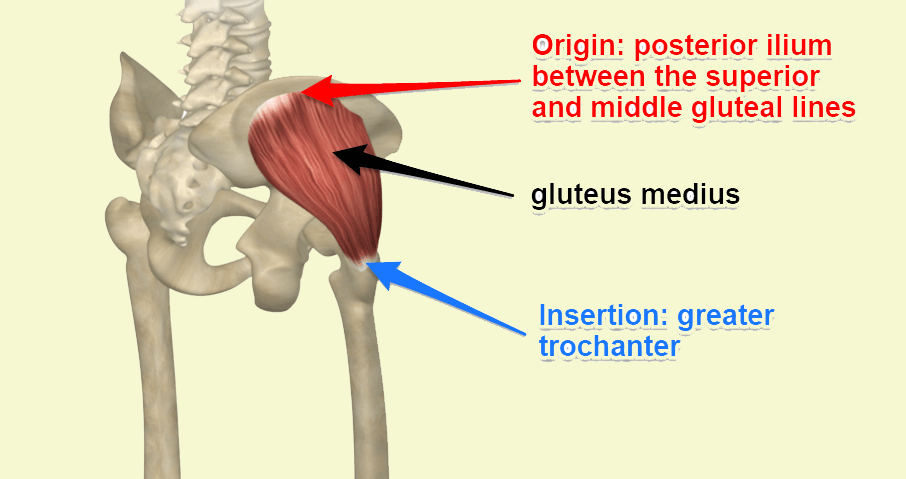
When it comes to maintaining a healthy, functional body, it’s easy to overlook the pivotal role of certain muscles in everyday movement and long-term stability. One such muscle is the gluteus medius. At Melbourne Massage and Treatment, located in Fitzroy North, I see many patients who either love running or love to hit the gym but are not aware of the importance of this muscle for their activity. What is the Gluteus Medius? The gluteus medius (GM) is one of the three primary muscles of the gluteal group, located in the upper part of the buttock. Here is a breakdown of its anatomy: Origin: the gluteal surface of the ilium Insertion: lateral surface of the greater trochanter Innervation: dorsal branches of the L4, L5, and S1 Actions: Abduction and medial rotation of the lower limb. It stabilises the pelvis. Thanks to its positioning, the GM plays a vital role in controlling pelvic movement, specifically in the stabilization of the pelvis during various motions like walking, running, or standing on one leg. More Information About Gluteus Medius actions The GM serves several essential functions that directly affect the stability of the hip and lower body: Pelvic Stabilization: One of its primary roles is preventing the pelvis from tilting excessively to one side when you move, especially when you’re walking or running. If the gluteus medius isn’t working properly, the opposite side of your pelvis may dip downward, leading to an imbalance and compensatory movements that strain other parts of the body. Hip Abduction: The gluteus medius helps to move the leg out to the side, away from the body. This movement, known as hip abduction, is crucial for activities that require lateral movement, such as stepping sideways or maintaining balance while performing physical tasks. Internal and External Rotation: The gluteus medius also assists with the rotation of the hip joint. Depending on which fibers are activated, it helps with both internal and external rotation of the thigh. This is essential for maintaining control and precision in movements. Postural Support: The gluteus medius muscle helps keep the pelvis level when you’re standing on one leg. Without proper activation of this muscle, one hip might drop, affecting posture and causing misalignments in the spine and lower back. The Role of the Gluteus Medius in Hip Stability Why is the GM so important for hip stability? Simply put, this muscle acts as the stabilizer of the pelvis. Without a properly functioning gluteus medius, other muscles and joints are forced to compensate for the lack of stability, leading to overuse and strain. For example, improper GM function can result in excessive stress on the knees, lower back, and even the ankles, which can lead to pain, discomfort, and injury. Clinical implications are vast, especially for athletes and individuals who regularly engage in physical activities. Hip instability can result in difficulty performing simple tasks like walking or climbing stairs, and over time, it may contribute to chronic conditions such as hip osteoarthritis. A common painful presentation that we see in athletes but also the everyday patients is Greater Throcanta Pain Syndrome (GTPS), which is characterised by the side hip pain. This presentation results from a GM tendon irritation. Signs of Weak or Dysfunctional Gluteus Medius Here are some common signs that your gluteus medius may need attention: Pain in the hip or lower back: Since this muscle is integral to proper alignment, dysfunction often manifests as discomfort in the hips or lower back. Difficulty balancing on one leg: Struggling with stability when standing on one leg may indicate weak gluteus medius muscles. Shifting or limping while walking: A noticeable shift or limp while walking can point to weakness in the gluteus medius, causing the body to compensate and disrupt your gait. How can Gluteus Medius impact your run? The gluteus medius is crucial for runners as it stabilizes the pelvis, controls hip movement, and ensures proper alignment during running. This muscle prevents excessive pelvic tilting, reduces side-to-side sway, and helps maintain efficient running form, thereby lowering the risk of injuries such as knee pain, IT band syndrome, and lower back discomfort. A weak or dysfunctional gluteus medius can lead to compensatory movements, affecting performance and causing imbalances. How Melbourne Massage and Treatment Can Help At Melbourne Massage and Treatment, as a clinical myotherapist, I focus on treatment designed to address muscle pain and dysfunction through a variety of techniques. One of the key areas of focus is to create a treatment plan that works for your presentation based on your clinical history. Here is a breakdown: 1. Assessment and Diagnosis: I would conducts a thorough assessment to identify if the gluteus medius is underperforming, weak, or compensating due to other musculoskeletal issues. This involves a combination of posture analysis, movement patterns, and targeted strength tests. 2. Myotherapy Treatment Techniques: I will use various techniques, including trigger point therapy, Dry Needling, myofascial release, and deep tissue massage, to release tension in the gluteus medius and surrounding muscles. This helps to restore proper function, reduce pain, and improve mobility. 3. Rehabilitation and Strengthening: After addressing any issues, we will work to develop rehabilitation strategies, including targeted strengthening exercises for the gluteus medius and other muscles that surround the pelvic, lower back and leg area. These exercises aim to restore proper muscle activation and prevent future imbalances. 4. Injury Prevention: In order to prevent further injury, we will set a target of strength that you want to achieve with your sports activity, and we will do our best to hit that target. Be mindful that based on your presentation, the target could extend from a few weeks to several months. The Takeaway The gluteus medius muscle is far more important for hip stability than many people realize. Its role in maintaining pelvic alignment and controlling movement is essential for pain-free mobility, proper posture, and long-term musculoskeletal health. Whether you’re dealing with hip pain, experiencing difficulty with balance, or want to prevent future issues, understanding and caring for […]
A deadlift (conventional deadlift) is a popular exercise that aims to strengthen your posterior chain muscle, including the erector spinae muscle, glutes, and hamstring. It is considered a really top list of important exercises to do, and it can be fun and rewarding, but when the weight you move starts increasing, it can lead to severe injuries if you are not using the right technique. Let’s then look into what we need to do to get a good deadlift by starting to analyse from bottom to top how the body should be placed. Centre of mass and biomechanics in deadlift To start with, let’s talk about the biomechanics and the centre of mass for a deadlift. When doing exercises, biomechanics plays a crucial role in safety and optimal exercise execution, and there is no exception for the deadlift. Furthermore, along with all exercises, the lifting and the descending part, the weight has to be in line with the centre of mass. These two components are strictly interconnected to the other one, which means if I don’t use the right biomechanics, I am not going to have the weight aligned with the centre of mass, or if the weight is not aligned with the centre of mass, I am not using my biomechanics at its full potential. So, what’s the centre of mass in the deadlift? The centre of mass in a deadlift is that imaginary line that runs right from the mid-portion of your feet up right in front of your shins, and as you lift the weight up, it passes right in front of your pelvis. That’s where the bar is going to end once you complete the lifting motion. What happens if I don’t keep the bar along the centre of mass? At any stage, during the lifting or the descending motion, if you move the bar further away from the centre of the mass line, there is a great danger of injury. This is because, as the weight travels away from the centre of mass, there is an increase in momentum, which means that your muscles and ligaments that are working hard to move the weight are suddenly placed under a greater load. What are then the proper biomechanics to observe along a deadlift? Ankle and Knee To execute a good deadlift, we want to ensure we have good ankle dorsiflexion, which is not as important as when we squat, but still, we better ensure it is working right. This would allow a straight forward movement of the knee, which would not need to find its way medially or laterally along the initial bending for when we go to grab the bar. Moving up the chain, as we said, the knee have to point straight ahead, following the toes direction. Hip and lower back Next is the hip. This is an important joint, and here is where we need to make sure that we tilt the pelvis forward (bring the teil bone upwards) and as we hinge the hip, we have to have enough movement in there that the greater trochanter (bone landmark that represents the side of the femur’s head) is posterior to the malleolus (the bone landmark that make the side and medial portion of the ankle). Now, if we managed to have tailbone project far back and up, and hip hinged with a slightly bent knee, our back up to cervical area would be alrady quiet flat. Thoracic and head If we keep going upwards, we get to the upper thoracic area, right between the scapula. Here, we want to keep the scapula protracted and have the rhomboids and serratus anterior muscles active and strong so that the arms can hang down straight towards the bar and sit right next to the knee. Regarding the head, use your eyesight to look down at the floor at 45° in front of you and feel the ears pulling away from the shoulder. That would keep your neck nice and long and place the head in the right position. Arms and hands Arms hang down from the shoulder in a straight line, from the AC Joint down to the wrist. The arm has to feel heavy and prolonged, and the hands must sit right next to the shin. Indeed, your arms must stay as wide as your shoulders. That would ensure that your arms are at 90° with the bar, and from a vertical pool point of view, they can take the maximum load ever. Lastly, regarding the hands, there are different grip types that can be used for the deadlift. What is most important is that the wrist is straight following the armline. For exercise purposes, you can have a regular grip where your thumb is gripping around the bar. For heavier weights, you may want to do a mixed grip, where one hand (the dominant one) has the palm facing forward, and the other hand has the palm facing you. In conclusion, the biomechanics of the deadlift, if used correctly, will allow you to always weight in a safe spot, in line with the centre of mass. Your back has to be flat at all times, and along the exercise execution, you want to grasp air in, engage the core to flat out the lower back and then you can lift off. Benefits of Deadlifting Now, let’s look into the benefits of deadlifting. Full-body workout: Deadlifts engage multiple muscle groups—glutes, hamstrings, quads, lower back, core, traps, and forearms—providing a full-body workout in a single movement. Improved strength: Deadlifts are among the best exercises for building overall strength, especially in the posterior chain (back, glutes, and hamstrings). Better posture: Deadlifts can improve posture and reduce the risk of slouching by strengthening your back and core muscles. Core stability: The movement requires significant core activation, helping to enhance core strength and stability. Increased athletic performance: Deadlifts translate well to other athletic movements, as they improve explosiveness, agility, and endurance. Fat loss: The intensity and demand on […]
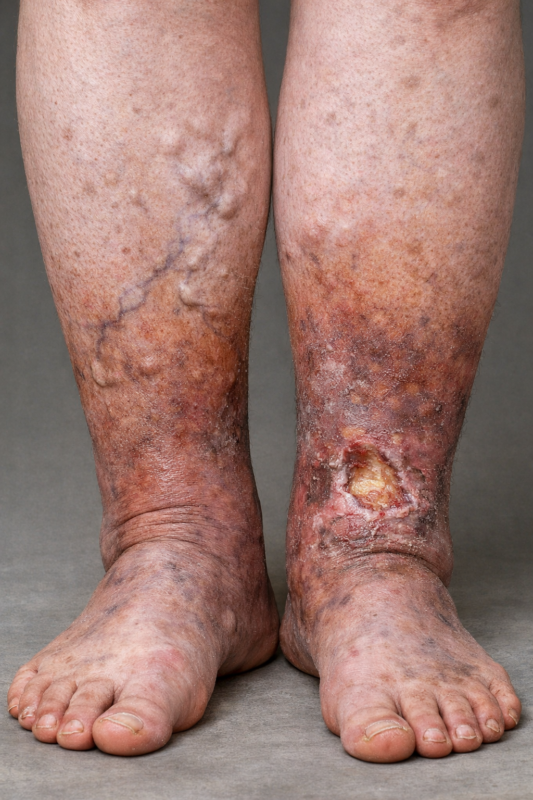
Lymphoedema therapy is crucial for those dealing with this chronic condition characterized by swelling due to lymph fluid buildup. Effective management can significantly improve quality of life, making it essential to understand various approaches. The Importance of Prevention in Lymphoedema Therapy Prevention is critical in lymphoedema therapy. Early intervention is vital for those at risk, such as cancer survivors or those with this presentation running in the family genetics. Regular exercise, maintaining a healthy weight, and avoiding tight clothing, including underwear and bras, can help support lymphatic health. Other things to be aware of include being vigilant about skincare and promptly addressing any injuries, which can further prevent lymphoedema’s development or worsening. Degeneration and Fibrosis Without proper lymphoedema therapy, the condition can lead to degeneration and fibrosis, where excess fibrous tissue develops in the affected area. Thdis can cause stiffness and discomfort, making it harder for lymphatic fluid to drain. Regular therapy, including manual lymphatic drainage, can help maintain tissue health and prevent these complications. Fibrosis is the body’s response to the constant inflammation created by the accumulation of lymph liquid. Once the fibrosis hardens and starts building up, no lymph capillary can be generated through that. Still, eventually, capillaries and nerves would, making the surgical removal of this type of tissue difficult. Skin Care and Anti-inflammatory Diet as part of Lymphoedema Therapy Proper skin care is essential in lymphoedema therapy. Keeping the skin clean and moisturized helps prevent infections, which can worsen symptoms. As the lymph fluid which is accumulates under the skin is reach in protein, it is important to maintain the skin intact, or the risk of infetioncs would hires exponentially, leading to ulcers and usage of antibiotic for a prolonged period of time. On top of that, to maintain the lymphedema presentation at ease, an anti-inflammatory diet rich in fruits, vegetables, and healthy fats can also support lymphatic function and reduce swelling. Foods like turmeric and omega-3 fatty acids are particularly beneficial. More specifically about the diet, avoiding long-chain fatty acids and processed food (which most often is rich in long-chain fatty acids) is essential, too. This is because those types of fat are absorbed via the lymphatic system, as they are too big (long chain) to be absorbed by the bloodstream directly. So, once those fats are loaded in the lymphatic system, it would be extra work for this already damaged system to get rid of those components. Compression Garment Wear Wearing compression garments is a fundamental aspect of lymphoedema therapy. These specially designed garments help maintain pressure on the affected areas, promoting lymphatic drainage and reducing swelling. It’s crucial to have garments that fit properly, as the right fit maximizes their effectiveness. Indeed, Giovanni would reccomedn to get your garments wear from clinics where the do measurements, and not from the pharmacy, as those last one, they may not follow at best your presentation or limbs. Melbourne Massage and Treatment and Lymphoedema Therapy At Melbourne Massage and Treatment, Giovanni offers Lymphoedema Therapy via services like Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy. The combination of those treatments allows the reduction of severe swelling within a series of treatments. There is also to say that each presentation is unique and based on other factors, such as diet, skincare and other presentations that may coexist with Lymphoedema, someone may need more time to achieve greater results. However, MLD consists of manual therapy that stimulates the lymphatic system. CDT involves applying compression to the swollen limb, maintaining pressure and making the liquid move. To know more about Giovanni Lymphoedema Clinic services, you can now book your free 15-minute initial consultation. Based on this initial chat, would be easier to evaluate a management plan for your presentation. Conclusion about Lymphoedema Therapy Lymphoedema therapy encompasses strategies that focus on prevention, skin care, dietary choices, garment wear, and infection management. By following these guidelines, individuals can effectively manage their condition and enhance their overall quality of life. Awareness and proactive care are key in navigating the challenges of lymphoedema.
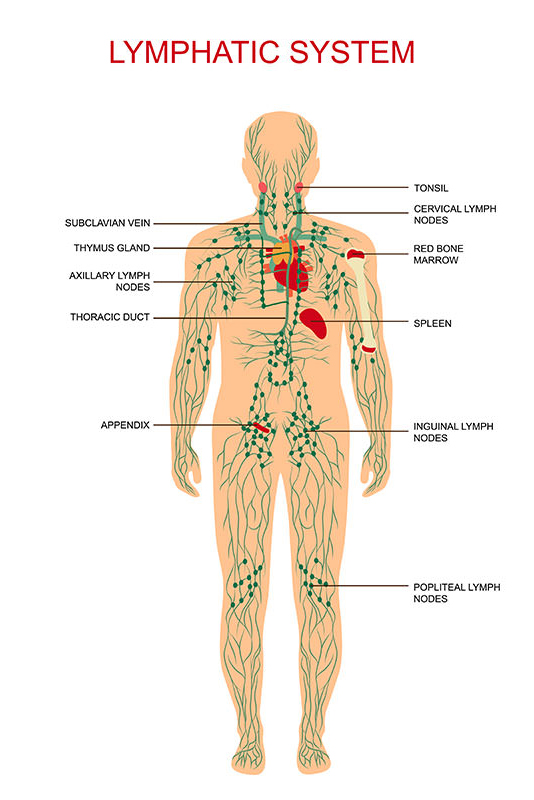
Swelling reduction in a lymphoedema presentation is the key component of successful treatment. Fluid accumulation under the skin can lead to severe swelling, skin cracks, and consequent infections. At Melbourne Massage and Treatment, Giovanni focuses on lymphoedema management using techniques like Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). The Lymphatic System: How It Works The lymphatic system plays a crucial role in maintaining our body’s fluid balance and supporting the immune system. It begins with tiny vessels called lymphatic capillaries, which are interspersed throughout the body, especially in tissues. These capillaries collect excess interstitial fluid, which surrounds cells. This fluid is made of proteins, fats, bacteria, viruses, dust, or anything that the body doesn’t recognise. The lymph then travels through progressively larger vessels called lymphatic collectors, connected by lymph nodes. Is here where the immune system clean the fluid. Once the clean is done, eventually the fluid would merge into larger ducts like the thoracic duct and the right lymphatic duct. These ducts drain lymph back into the bloodstream, ensuring that excess fluid is removed and helping maintain overall fluid balance. Muscle Movement and Its Role in Lymphatic Flow Muscle movement plays a vital role in facilitating lymphatic flow. Unlike the circulatory system, the lymphatic system doesn’t have a central pump like the heart. Instead, it relies on the contraction of surrounding muscles to push lymph through the vessels. When we move, especially during activities like walking or exercising, the rhythmic contractions of our muscles compress the lymphatic vessels, propelling lymph upward toward the ducts. This is why physical activity is essential not only for circulation but also for swelling reduction and maintaining a healthy lymphatic system. Understanding Lymphoedema: Causes and Types Lymphoedema occurs when a disruption in the lymphatic system leads to an abnormal accumulation of lymph fluid, usually in the arms or legs. There are two types of lymphoedema: primary and secondary. Primary lymphoedema is a genetic condition that results from malformations in the lymphatic system, often present at birth or developing during puberty. In contrast, secondary lymphoedema results from damage or obstruction of the lymphatic system due to factors such as surgery, radiation therapy, infection, or trauma. Understanding the differences between these types is crucial for effective management and treatment. Combined Decongestive Therapy (CDT): A Path to Swelling Reduction One effective treatment for lymphoedema is Combined Decongestive Therapy (CDT). This comprehensive approach combines manual lymphatic drainage (MLD) compression therapy, exercise, and skincare to promote lymphatic flow and support swelling reduction. The manual lymphatic drainage technique helps stimulate the lymphatic vessels and facilitates the movement of lymph fluid, while compression garments assist in maintaining the reduction achieved during therapy. By addressing both the symptoms and the underlying causes of lymphoedema, CDT provides individuals with a practical strategy for managing their condition. Combined Decongestive Therapy (CDT) and Bandaging Techniques Combined Decongestive Therapy (CDT) incorporates techniques, including specialized bandaging, to effectively manage lymphoedema. Two primary types of bandages are short-stretch and long-stretch bandages. Short-stretch Bandages These bandages have low elasticity and provide firm compression without causing excessive pressure during movement, making them ideal for managing lymphatic fluid in a stable manner. They support the natural muscle pump action, allowing the patient to move their limbs freely and promoting lymphatic drainage as the muscles contract. Long-stretch Bandages In contrast, long-stretch bandages offer elastic compression, which can create resting pressure that may be less effective during activity. This type of bandage works best when the patient is less likely to move their limb. In CDT, short-stretch bandages are generally preferred because they maintain consistent pressure on the affected limb, helping to reduce swelling more effectively while allowing for functional mobility. This strategic choice creates an optimal environment for lymphatic flow and manages the symptoms of lymphoedema. Melbourne Massage and Treatment: Promoting Health and Lymphoedema Swelling Reduction At Melbourne Massage and Treatment in Fitzroy North, Giovanni specializes in therapies that reduce swelling and enhance overall wellness. By understanding the lymphatic system and the importance of movement, you can take proactive steps to manage lymphoedema and promote better health. If you want to know more about how Giovanni can help you with your lymphoedema management plan, book a 15-minute free consultation today. FAQ: Lymphoedema and Swelling Reduction Q: What is lymphoedema? A: Lymphoedema is characterized by the abnormal accumulation of lymph fluid, usually in the arms or legs, leading to severe swelling. It occurs when the lymphatic system is disrupted or obstructed. Q: What causes lymphoedema? A: There are two types of lymphoedema. Primary lymphoedema is genetic and results from malformations in the lymphatic system. Secondary lymphoedema is caused by damage or obstruction due to surgery, radiation therapy, infection, or trauma. Q: How does the lymphatic system work? A: The lymphatic system maintains fluid balance and supports the immune system. It begins with lymphatic capillaries that collect excess interstitial fluid, which transforms into lymph and travels through larger vessels, eventually draining back into the bloodstream. Q: How can muscle movement help with lymphatic flow? A: Muscle movement aids lymphatic flow by contracting and compressing the lymphatic vessels, propelling lymph toward the ducts. This is essential for circulation and swelling reduction, as the contractions facilitate the movement of lymph fluid. Q: What is Combined Decongestive Therapy (CDT)? A: CDT is a comprehensive treatment for lymphoedema that includes manual lymphatic drainage, compression therapy, exercise, and skincare. It promotes lymphatic flow and supports swelling reduction, addressing both symptoms and underlying causes. Q: Why are short-stretch bandages preferred in CDT? A: Short-stretch bandages are preferred because they maintain consistent pressure on the affected limb, promoting effective swelling reduction while allowing for mobility. This helps create an optimal environment for lymphatic flow. Q: How can I learn more about managing lymphoedema? A: For more information on lymphoedema management, you can book a 15-minute free consultation with Giovanni at Melbourne Massage and Treatment, Lymphoedema Clinic, in Fitzroy North. Giovanni specializes in therapies designed to reduce swelling and enhance overall wellness.
Welcome to Melbourne Massage and Treatment, a Lymphoedema Clinic located in the heart of Fitzroy North. If you’re seeking effective management for lymphoedema, our specialised Clinic, led by experienced therapist Giovanni, is here to help you reclaim your comfort and quality of life. Understanding Lymphoedema Lymphoedema is a chronic degenerative condition characterised by swelling, typically in the arms or legs, but it can also occur in the abdominal, thoracic, or genital areas. A buildup of lymph fluid causes lymphoedema and can arise from various factors, including cancer surgery (mastectomy), radiation treatment, or genetic predisposition. When it is a genetic predisposition, it is categorised as Primary Lymphoedema, and when it develops post-surgery or due to external factors, it is characterised as Secondary Lymphoedema. Managing lymphoedema is crucial to preventing further complications and enhancing overall well-being. Meet Giovanni, Your Lymphoedema Specialist Giovanni is a dedicated myotherapyst trained at the prestigious Vodder Academy, renowned for its comprehensive approach to lymphatic health. With extensive experience in Manual Lymphatic Drainage (MLD) and Combined Destive Therapy (CDT), Giovanni employs proven techniques to reduce swelling, alleviate discomfort, and promote lymphatic flow. Manual Lymphatic Drainage (MLD) MLD is a gentle, non-invasive massage technique designed to stimulate the lymphatic system. Giovanni’s expert hands help to encourage the movement of lymph fluid, reducing swelling and improving circulation. This technique allows the stimulation of your lymphatic system’s parallel channels (anastomosis), which would not be active unless stimulated. This is a crucial step in Lymphoedema management as the lymph fluid would not have anywhere to go due to its damaged structure. Combined Decongestive Therapy (CDT) As Melbourne Massage and Treatment is also a Lymphoedema Clinic, the treatment that you can receive from Giovanni is not going to be focused on MLD only, but once the anastomosis has been activated, Giovanni would apply Combined Decongestive Therapy. This holistic approach focuses on the application of compression bandaging, which maintains the skin’s lymphatic fluid under pressure. Other types of care approaches to be aware of along this presentation are skin care and exercise, providing a comprehensive management plan tailored to each patient’s needs through garment wear. Giovanni will work closely with you to develop a personalised strategy that addresses your specific concerns and lifestyle. Free Initial Consultation Understanding your condition and exploring your treatment options can be overwhelming. To support you, Giovanni offers a 15-minute free phone consultation for lymphoedema patients. This initial conversation provides an opportunity to discuss your symptoms, ask questions, and learn how our clinic can assist you on your journey to better health. Why Choose Us? Expertise: Giovanni’s training at the Vodder Academy ensures you receive care rooted in the latest techniques and knowledge. Personalised Care: We understand that each patient is unique. Giovanni tailors treatment plans to fit your individual needs and lifestyle. Convenient Location: My clinic in Fitzroy North is easily accessible, making it convenient for local patients to receive ongoing care. Supportive Environment: We prioritise creating a welcoming atmosphere where you can feel comfortable discussing your health concerns. Get Started Today! If you’re ready to take the next step in managing your lymphoedema, contact the Melbourne Massage and Treatment Clinic today. Schedule your free initial phone consultation with Giovanni and discover how MLD and CDT can help you achieve a healthier, more comfortable life. Visit our website or call us to learn more about our services and how we can assist you on your path to recovery. Your well-being is our priority, and we look forward to supporting you every step of the way! FAQS – Melbourne Massage and Treatment (Lymphoedema Clinic) 1. What is lymphoedema? Lymphoedema is a chronic condition caused by a buildup of lymph fluid, leading to swelling, usually in the arms or legs. It can also affect the abdomen, chest, or genital area. It may result from cancer treatments (like mastectomy or radiation), surgery, or genetic factors (primary lymphoedema). 2. What are the differences between primary and secondary lymphoedema? Primary Lymphoedema is genetic and occurs due to an inherited malfunction in the lymphatic system. Secondary Lymphoedema develops due to external factors like surgery (e.g., mastectomy), radiation therapy, trauma, or infection. 3. How can lymphoedema be managed? Lymphoedema is a degenerative condition, meaning it worsens over time if untreated. However, proper management through Manual Lymphatic Drainage (MLD), Combined Decongestive Therapy (CDT), compression garments, skin care, and exercise can significantly reduce symptoms and improve quality of life. 4. What is Manual Lymphatic Drainage (MLD)? MLD is a gentle, specialised massage technique that stimulates the lymphatic system to improve lymph flow, reduce swelling, and activate alternative lymphatic pathways (anastomosis) when the main vessels are damaged. 5. What is Combined Decongestive Therapy (CDT)? CDT stands for Combined Decongestive Therapy and is about applying compression to the limb affected by lymphoedema to get the fluid in exceed to keep moving post MLD therapy. 6. Do you offer a free consultation? Yes! I offer lymphoedema patients a free 15-minute phone consultation to discuss symptoms, treatment options, and how I can help. 7. Where is the clinic located? Melbourne Massage and Treatment Lymphoedema clinic is conveniently located in Fitzroy North, Melbourne, making it easily accessible for local patients. 8. Can lymphoedema be cured? While lymphoedema is a chronic condition, proper management can significantly reduce swelling, discomfort, and the risk of complications. Early intervention and consistent therapy are key. 9. Is compression therapy necessary for lymphoedema? Yes, compression garments or bandages are essential in CDT to maintain pressure on tissues, prevent fluid re-accumulation, and support long-term management. 10. Can exercise help with lymphoedema? Yes! Gentle, guided exercises can promote lymphatic drainage and improve mobility. Giovanni can recommend safe exercises tailored to your condition. 11. How often should I get MLD or CDT treatments? The frequency depends on the severity of your condition. Some patients benefit from weekly sessions, while others may need maintenance treatments less often. Giovanni will create a personalised plan for you. 12. Does private health insurance cover lymphoedema treatments? Some private health funds may cover part of the […]
Lymphoedema is a condition that can affect many individuals following a mastectomy, particularly those who have undergone lymph node removal as part of their breast cancer treatment. Understanding lymphoedema, its causes, symptoms, and management can help those affected navigate this challenging aspect of recovery. What is Lymphoedema? Lymphoedema is a chronic condition characterised by tissue swelling, usually in the arms or legs, due to an accumulation of lymphatic fluid. It often occurs when lymph nodes are removed or damaged, disrupting the normal flow of lymph fluid through the body. Another reason why someone could end up going through Lymphoedema is severe skin infections that damage the lymphatic system, radiation therapy, or invasive surgeries. Why Does Lymphoedema Occur After Mastectomy? During a mastectomy, when lymph nodes are removed (as in axillary lymph node dissection), the pathway for lymph fluid drainage from the hand and the arm can be compromised as the fluid has nowhere to be discharged at the surgery area. This disruption can lead to a buildup of fluid, resulting in swelling that, if left untreated, can create severe discomfort. While not everyone who has a mastectomy will develop lymphoedema, certain risk factors may increase the likelihood, including: The extent of surgery Radiation therapy Infection Obesity Lack of physical activity Previous or current other injuries to limb/shoulder Surgery was on the side of the dominant hand Be a smoker Symptoms of Lymphoedema post mastectomy The symptoms of lymphoedema can vary in severity and may develop gradually. Common signs include: Swelling in the arm, hand, or breast area A feeling of heaviness or tightness in the affected area Restricted range of motion in the shoulder or arm Skin changes, such as thickening or hardening Swelling doesn’t reduce just by holding the arm elevated Early Detection and Diagnosis Recognizing the early signs of lymphoedema is crucial for effective management. This would help prevent degeneration of the condition and reduce the chance of fibrosis building under the skin, which would lead to longer treatment and possible complications. If you notice swelling or other symptoms, Giovanni is here to help, so don’t hesitate to get in touch. To simplify the diagnosis process, Giovanni offers a 15-minute free phone consultation appointment. During this phone call, we can evaluate whether no pathologies need to be addressed by a GP or other medical staff or if the Lymphoedema management plan can be initiated. Managing Lymphoedema While there is currently no cure for lymphoedema, various management strategies can help reduce symptoms and improve quality of life: Manual Lymphatic Drainage (MLD) is a specialized massage technique that stimulates the lymphatic system and encourages fluid movement.At Melbourne Massage and Treatment in Fitzroy North, Giovanni specialises in the management of Lymphoedema with MLD. Combined Decongestive Therapy (CDT): CDT refers to the application of bandaging that Giovanni would do after the initial MLD treatment. Garments Wear: Wearing compression garments, such as sleeves or bandages, can help prevent fluid buildup and promote lymphatic drainage. Exercise: Gentle, targeted exercises can improve circulation and lymphatic flow. Giovanni at the end of the appointment would show a series of simple exercises that can help you in managing the Lymphoedema swelling. Skin Care: Maintaining skin hygiene and moisturization can prevent infections, which may exacerbate lymphoedema. Diet and Lifestyle: Maintaining a healthy weight and staying active can reduce the risk of developing or worsening lymphoedema. Surgery: In some cases, surgical options may be considered, such as lymphovenous bypass or vascularized lymph node transfer. Support and Resources Coping with lymphoedema can be emotionally and physically challenging. Support groups and counselling can provide valuable resources and community connections. Organizations like the Lymphatic Education & Research Network (LE&RN) and local cancer support services can offer information and support tailored to your needs. Conclusion Navigating lymphoedema after a mastectomy can be daunting, but understanding the condition and implementing effective management strategies can make a significant difference. Early intervention, education, and support are key components in minimizing its impact on daily life. If you or a loved one is facing this challenge, remember you are not alone—reach out to Giovanni and ask how Melbourne Massage and Treatment services can help. FAQ