When the lymphatic system stop working, either because for a congential malfunctioning, or because of a an external intervention, which did lead to lymphatic system damage, the individual may start experiencing symptoms of Lymphoedema. At Melbourne Massage and Treatment in Fitzroy North, Giovanni understand how challenging lymphoedema can be, which is why he provide expert care through Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). These non-invasive treatments help manage the symptoms and improve your quality of life. What is Lymphoedema? Lymphoedema occurs when the lymphatic system is blocked or malfunctioning, leading to a buildup of lymphatic fluid. This fluid results in swelling in the affected areas, often in the arms, legs, or other extremities. Lymphoedema can be primary (a hereditary condition) or secondary (often caused by injury, surgery, or infection). The fluid that builds up in the body is a fluid that is naturally produced by the body and is released under the skin and between tissues by the bloodstream. It is reached in protein, bacteria, viruses, dust, and other minor substances that the body is unsure how to handle. Stages of Lymphoedema Lymphoedema progresses in stages, with each stage representing the severity of the condition. Recognizing the symptoms early on can help prevent the condition from advancing, so it’s important to be aware of the subtle changes in your body. Stage 0: Latent or Subclinical Stage In this early stage, there are no visible signs or symptoms of lymphoedema, but the lymphatic system may already be compromised. People in Stage 0 may experience a feeling of heaviness, discomfort, or mild swelling, int the limbs affected by this presentation, but these symptoms typically disappear after resting or with limb elevation. The fluid retention is still minimal and may not be noticed by the individual, but it can be detected through careful assessment. Stage 1: Reversible Stage At this stage, swelling is more noticeable, but the skin is still soft, and the swelling can still decrease with limb elevation and movement. When the swelling is present, the skin will feel puffy or tight, and there may be a sensation of heaviness in the affected area. In this relevant early stage, it i still easy to intervene for prevent further degeneration, and if you are unsure of what you are experiencing, reach out Giovanni for a 15 minutes free consultation, in which, at least thanks to the analysis of your clinical history, we can already evaluate if what you are experiencing is a Stage 1 Lymphoedema. Stage 2: Spontaneously Irreversible Stage In Stage 2, the swelling becomes more persistent and is not fully responsive to movement and limb elevation. The asking of the affected area may begin to feel firmer, and there can be noticeable thickening of the skin. This is the stage where fibrosis (scarring of the tissue) starts to develop, and it’s crucial to stop this from going any worse. While the swelling might fluctuate, it becomes more difficult to manage without intervention. At this point, manual treatments like Manual Lymphatic Drainage (MLD) can significantly help reduce swelling and improve the overall function of the lymphatic system. Stage 3: Lymphostatic Elephantiasis The final stage of lymphoedema is characterized by extreme swelling and thickened, hardened skin. The affected area may look large, disfigured, and become painful to the touch. Tissue fibrosis is advanced, and the skin may develop ulcerations or infections due to poor circulation and immune system function. Indeed, along with the swelling and the fibrosis buildup, the outer layer of the skin is placed further away from the blood capillary, which is responsible for releasing oxygen and other substances essential for skin regeneration.Therefore, as the skin breaks open, due to its poor condition, it is more subject to infections and contamination of pathogens. Stage 3 lymphoedema is debilitating and requires ongoing care and treatment to prevent complications and manage symptoms. At this stage, a combination of therapies such as Combined Decongestive Therapy (CDT) and MLD becomes vital for managing the swelling and restoring lymphatic flow. Common Symptoms of Lymphoedema Lymphoedema symptoms can vary from person to person and depend on the stage of the condition. The common symptoms include: Swelling: The most obvious sign of lymphoedema is swelling in the affected area, typically starting in the arms or legs. The swelling is often gradual and may worsen over the course of the day, especially after prolonged standing or sitting. Tightness or Heaviness: Affected limbs may feel heavy or tight, particularly after physical activity or at the end of the day. This sensation is often worse in the early stages and may become more pronounced as the condition progresses. Pain or Discomfort: Pain, tenderness, or discomfort in the swollen area is common, especially when there is fibrosis (hardening) of the tissues. The pain can range from mild to severe, depending on the stage. Reduced Range of Motion: As the swelling and fibrosis increase, it can lead to a limited range of motion, particularly in the arms and legs. This can impact daily activities and mobility. Skin Changes: In later stages of lymphoedema, the skin may appear thickened or leathery, with a shiny, tight appearance. There may also be visible folds in the skin, particularly around the knees, elbows, or ankles. Frequent Infections: Swollen tissues have a reduced ability to fight off infections, so people with lymphoedema are more susceptible to bacterial and fungal infections, which can further complicate the condition. Numbness or Tingling: As the swelling progresses, the nerves in the affected area may be compressed, leading to sensations of tingling, numbness, or even burning. Increased Skin Sensitivity: The skin in the affected area may become more sensitive, prone to rashes, or develop sores due to the increased swelling and poor circulation. Commonly Affected Areas of the Body Lymphoedema can affect different parts of the body, but the most common areas are: Arms: After surgery, particularly mastectomy (breast cancer surgery) that involves the removal of lymph nodes, the arms are a common site for lymphoedema. The swelling […]
Tag Archives: manual lymphatic drainage
Lymphoedema therapy is crucial for those dealing with this chronic condition characterized by swelling due to lymph fluid buildup. Effective management can significantly improve quality of life, making it essential to understand various approaches. The Importance of Prevention in Lymphoedema Therapy Prevention is critical in lymphoedema therapy. Early intervention is vital for those at risk, such as cancer survivors or those with this presentation running in the family genetics. Regular exercise, maintaining a healthy weight, and avoiding tight clothing, including underwear and bras, can help support lymphatic health. Other things to be aware of include being vigilant about skincare and promptly addressing any injuries, which can further prevent lymphoedema’s development or worsening. Degeneration and Fibrosis Without proper lymphoedema therapy, the condition can lead to degeneration and fibrosis, where excess fibrous tissue develops in the affected area. Thdis can cause stiffness and discomfort, making it harder for lymphatic fluid to drain. Regular therapy, including manual lymphatic drainage, can help maintain tissue health and prevent these complications. Fibrosis is the body’s response to the constant inflammation created by the accumulation of lymph liquid. Once the fibrosis hardens and starts building up, no lymph capillary can be generated through that. Still, eventually, capillaries and nerves would, making the surgical removal of this type of tissue difficult. Skin Care and Anti-inflammatory Diet as part of Lymphoedema Therapy Proper skin care is essential in lymphoedema therapy. Keeping the skin clean and moisturized helps prevent infections, which can worsen symptoms. As the lymph fluid which is accumulates under the skin is reach in protein, it is important to maintain the skin intact, or the risk of infetioncs would hires exponentially, leading to ulcers and usage of antibiotic for a prolonged period of time. On top of that, to maintain the lymphedema presentation at ease, an anti-inflammatory diet rich in fruits, vegetables, and healthy fats can also support lymphatic function and reduce swelling. Foods like turmeric and omega-3 fatty acids are particularly beneficial. More specifically about the diet, avoiding long-chain fatty acids and processed food (which most often is rich in long-chain fatty acids) is essential, too. This is because those types of fat are absorbed via the lymphatic system, as they are too big (long chain) to be absorbed by the bloodstream directly. So, once those fats are loaded in the lymphatic system, it would be extra work for this already damaged system to get rid of those components. Compression Garment Wear Wearing compression garments is a fundamental aspect of lymphoedema therapy. These specially designed garments help maintain pressure on the affected areas, promoting lymphatic drainage and reducing swelling. It’s crucial to have garments that fit properly, as the right fit maximizes their effectiveness. Indeed, Giovanni would reccomedn to get your garments wear from clinics where the do measurements, and not from the pharmacy, as those last one, they may not follow at best your presentation or limbs. Melbourne Massage and Treatment and Lymphoedema Therapy At Melbourne Massage and Treatment, Giovanni offers Lymphoedema Therapy via services like Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy. The combination of those treatments allows the reduction of severe swelling within a series of treatments. There is also to say that each presentation is unique and based on other factors, such as diet, skincare and other presentations that may coexist with Lymphoedema, someone may need more time to achieve greater results. However, MLD consists of manual therapy that stimulates the lymphatic system. CDT involves applying compression to the swollen limb, maintaining pressure and making the liquid move. To know more about Giovanni Lymphoedema Clinic services, you can now book your free 15-minute initial consultation. Based on this initial chat, would be easier to evaluate a management plan for your presentation. Conclusion about Lymphoedema Therapy Lymphoedema therapy encompasses strategies that focus on prevention, skin care, dietary choices, garment wear, and infection management. By following these guidelines, individuals can effectively manage their condition and enhance their overall quality of life. Awareness and proactive care are key in navigating the challenges of lymphoedema.
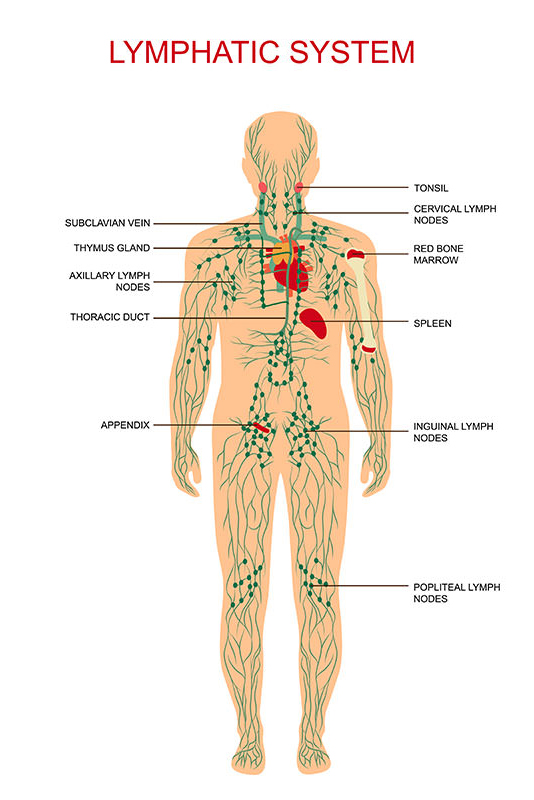
Swelling reduction in a lymphoedema presentation is the key component of successful treatment. Fluid accumulation under the skin can lead to severe swelling, skin cracks, and consequent infections. At Melbourne Massage and Treatment, Giovanni focuses on lymphoedema management using techniques like Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). The Lymphatic System: How It Works The lymphatic system plays a crucial role in maintaining our body’s fluid balance and supporting the immune system. It begins with tiny vessels called lymphatic capillaries, which are interspersed throughout the body, especially in tissues. These capillaries collect excess interstitial fluid, which surrounds cells. This fluid is made of proteins, fats, bacteria, viruses, dust, or anything that the body doesn’t recognise. The lymph then travels through progressively larger vessels called lymphatic collectors, connected by lymph nodes. Is here where the immune system clean the fluid. Once the clean is done, eventually the fluid would merge into larger ducts like the thoracic duct and the right lymphatic duct. These ducts drain lymph back into the bloodstream, ensuring that excess fluid is removed and helping maintain overall fluid balance. Muscle Movement and Its Role in Lymphatic Flow Muscle movement plays a vital role in facilitating lymphatic flow. Unlike the circulatory system, the lymphatic system doesn’t have a central pump like the heart. Instead, it relies on the contraction of surrounding muscles to push lymph through the vessels. When we move, especially during activities like walking or exercising, the rhythmic contractions of our muscles compress the lymphatic vessels, propelling lymph upward toward the ducts. This is why physical activity is essential not only for circulation but also for swelling reduction and maintaining a healthy lymphatic system. Understanding Lymphoedema: Causes and Types Lymphoedema occurs when a disruption in the lymphatic system leads to an abnormal accumulation of lymph fluid, usually in the arms or legs. There are two types of lymphoedema: primary and secondary. Primary lymphoedema is a genetic condition that results from malformations in the lymphatic system, often present at birth or developing during puberty. In contrast, secondary lymphoedema results from damage or obstruction of the lymphatic system due to factors such as surgery, radiation therapy, infection, or trauma. Understanding the differences between these types is crucial for effective management and treatment. Combined Decongestive Therapy (CDT): A Path to Swelling Reduction One effective treatment for lymphoedema is Combined Decongestive Therapy (CDT). This comprehensive approach combines manual lymphatic drainage (MLD) compression therapy, exercise, and skincare to promote lymphatic flow and support swelling reduction. The manual lymphatic drainage technique helps stimulate the lymphatic vessels and facilitates the movement of lymph fluid, while compression garments assist in maintaining the reduction achieved during therapy. By addressing both the symptoms and the underlying causes of lymphoedema, CDT provides individuals with a practical strategy for managing their condition. Combined Decongestive Therapy (CDT) and Bandaging Techniques Combined Decongestive Therapy (CDT) incorporates techniques, including specialized bandaging, to effectively manage lymphoedema. Two primary types of bandages are short-stretch and long-stretch bandages. Short-stretch Bandages These bandages have low elasticity and provide firm compression without causing excessive pressure during movement, making them ideal for managing lymphatic fluid in a stable manner. They support the natural muscle pump action, allowing the patient to move their limbs freely and promoting lymphatic drainage as the muscles contract. Long-stretch Bandages In contrast, long-stretch bandages offer elastic compression, which can create resting pressure that may be less effective during activity. This type of bandage works best when the patient is less likely to move their limb. In CDT, short-stretch bandages are generally preferred because they maintain consistent pressure on the affected limb, helping to reduce swelling more effectively while allowing for functional mobility. This strategic choice creates an optimal environment for lymphatic flow and manages the symptoms of lymphoedema. Melbourne Massage and Treatment: Promoting Health and Lymphoedema Swelling Reduction At Melbourne Massage and Treatment in Fitzroy North, Giovanni specializes in therapies that reduce swelling and enhance overall wellness. By understanding the lymphatic system and the importance of movement, you can take proactive steps to manage lymphoedema and promote better health. If you want to know more about how Giovanni can help you with your lymphoedema management plan, book a 15-minute free consultation today. FAQ: Lymphoedema and Swelling Reduction Q: What is lymphoedema? A: Lymphoedema is characterized by the abnormal accumulation of lymph fluid, usually in the arms or legs, leading to severe swelling. It occurs when the lymphatic system is disrupted or obstructed. Q: What causes lymphoedema? A: There are two types of lymphoedema. Primary lymphoedema is genetic and results from malformations in the lymphatic system. Secondary lymphoedema is caused by damage or obstruction due to surgery, radiation therapy, infection, or trauma. Q: How does the lymphatic system work? A: The lymphatic system maintains fluid balance and supports the immune system. It begins with lymphatic capillaries that collect excess interstitial fluid, which transforms into lymph and travels through larger vessels, eventually draining back into the bloodstream. Q: How can muscle movement help with lymphatic flow? A: Muscle movement aids lymphatic flow by contracting and compressing the lymphatic vessels, propelling lymph toward the ducts. This is essential for circulation and swelling reduction, as the contractions facilitate the movement of lymph fluid. Q: What is Combined Decongestive Therapy (CDT)? A: CDT is a comprehensive treatment for lymphoedema that includes manual lymphatic drainage, compression therapy, exercise, and skincare. It promotes lymphatic flow and supports swelling reduction, addressing both symptoms and underlying causes. Q: Why are short-stretch bandages preferred in CDT? A: Short-stretch bandages are preferred because they maintain consistent pressure on the affected limb, promoting effective swelling reduction while allowing for mobility. This helps create an optimal environment for lymphatic flow. Q: How can I learn more about managing lymphoedema? A: For more information on lymphoedema management, you can book a 15-minute free consultation with Giovanni at Melbourne Massage and Treatment, Lymphoedema Clinic, in Fitzroy North. Giovanni specializes in therapies designed to reduce swelling and enhance overall wellness.
Welcome to Melbourne Massage and Treatment, a Lymphoedema Clinic located in the heart of Fitzroy North. If you’re seeking effective management for lymphoedema, our specialised Clinic, led by experienced therapist Giovanni, is here to help you reclaim your comfort and quality of life. Understanding Lymphoedema Lymphoedema is a chronic degenerative condition characterised by swelling, typically in the arms or legs, but it can also occur in the abdominal, thoracic, or genital areas. A buildup of lymph fluid causes lymphoedema and can arise from various factors, including cancer surgery (mastectomy), radiation treatment, or genetic predisposition. When it is a genetic predisposition, it is categorised as Primary Lymphoedema, and when it develops post-surgery or due to external factors, it is characterised as Secondary Lymphoedema. Managing lymphoedema is crucial to preventing further complications and enhancing overall well-being. Meet Giovanni, Your Lymphoedema Specialist Giovanni is a dedicated myotherapyst trained at the prestigious Vodder Academy, renowned for its comprehensive approach to lymphatic health. With extensive experience in Manual Lymphatic Drainage (MLD) and Combined Destive Therapy (CDT), Giovanni employs proven techniques to reduce swelling, alleviate discomfort, and promote lymphatic flow. Manual Lymphatic Drainage (MLD) MLD is a gentle, non-invasive massage technique designed to stimulate the lymphatic system. Giovanni’s expert hands help to encourage the movement of lymph fluid, reducing swelling and improving circulation. This technique allows the stimulation of your lymphatic system’s parallel channels (anastomosis), which would not be active unless stimulated. This is a crucial step in Lymphoedema management as the lymph fluid would not have anywhere to go due to its damaged structure. Combined Decongestive Therapy (CDT) As Melbourne Massage and Treatment is also a Lymphoedema Clinic, the treatment that you can receive from Giovanni is not going to be focused on MLD only, but once the anastomosis has been activated, Giovanni would apply Combined Decongestive Therapy. This holistic approach focuses on the application of compression bandaging, which maintains the skin’s lymphatic fluid under pressure. Other types of care approaches to be aware of along this presentation are skin care and exercise, providing a comprehensive management plan tailored to each patient’s needs through garment wear. Giovanni will work closely with you to develop a personalised strategy that addresses your specific concerns and lifestyle. Free Initial Consultation Understanding your condition and exploring your treatment options can be overwhelming. To support you, Giovanni offers a 15-minute free phone consultation for lymphoedema patients. This initial conversation provides an opportunity to discuss your symptoms, ask questions, and learn how our clinic can assist you on your journey to better health. Why Choose Us? Expertise: Giovanni’s training at the Vodder Academy ensures you receive care rooted in the latest techniques and knowledge. Personalised Care: We understand that each patient is unique. Giovanni tailors treatment plans to fit your individual needs and lifestyle. Convenient Location: My clinic in Fitzroy North is easily accessible, making it convenient for local patients to receive ongoing care. Supportive Environment: We prioritise creating a welcoming atmosphere where you can feel comfortable discussing your health concerns. Get Started Today! If you’re ready to take the next step in managing your lymphoedema, contact the Melbourne Massage and Treatment Clinic today. Schedule your free initial phone consultation with Giovanni and discover how MLD and CDT can help you achieve a healthier, more comfortable life. Visit our website or call us to learn more about our services and how we can assist you on your path to recovery. Your well-being is our priority, and we look forward to supporting you every step of the way! FAQS – Melbourne Massage and Treatment (Lymphoedema Clinic) 1. What is lymphoedema? Lymphoedema is a chronic condition caused by a buildup of lymph fluid, leading to swelling, usually in the arms or legs. It can also affect the abdomen, chest, or genital area. It may result from cancer treatments (like mastectomy or radiation), surgery, or genetic factors (primary lymphoedema). 2. What are the differences between primary and secondary lymphoedema? Primary Lymphoedema is genetic and occurs due to an inherited malfunction in the lymphatic system. Secondary Lymphoedema develops due to external factors like surgery (e.g., mastectomy), radiation therapy, trauma, or infection. 3. How can lymphoedema be managed? Lymphoedema is a degenerative condition, meaning it worsens over time if untreated. However, proper management through Manual Lymphatic Drainage (MLD), Combined Decongestive Therapy (CDT), compression garments, skin care, and exercise can significantly reduce symptoms and improve quality of life. 4. What is Manual Lymphatic Drainage (MLD)? MLD is a gentle, specialised massage technique that stimulates the lymphatic system to improve lymph flow, reduce swelling, and activate alternative lymphatic pathways (anastomosis) when the main vessels are damaged. 5. What is Combined Decongestive Therapy (CDT)? CDT stands for Combined Decongestive Therapy and is about applying compression to the limb affected by lymphoedema to get the fluid in exceed to keep moving post MLD therapy. 6. Do you offer a free consultation? Yes! I offer lymphoedema patients a free 15-minute phone consultation to discuss symptoms, treatment options, and how I can help. 7. Where is the clinic located? Melbourne Massage and Treatment Lymphoedema clinic is conveniently located in Fitzroy North, Melbourne, making it easily accessible for local patients. 8. Can lymphoedema be cured? While lymphoedema is a chronic condition, proper management can significantly reduce swelling, discomfort, and the risk of complications. Early intervention and consistent therapy are key. 9. Is compression therapy necessary for lymphoedema? Yes, compression garments or bandages are essential in CDT to maintain pressure on tissues, prevent fluid re-accumulation, and support long-term management. 10. Can exercise help with lymphoedema? Yes! Gentle, guided exercises can promote lymphatic drainage and improve mobility. Giovanni can recommend safe exercises tailored to your condition. 11. How often should I get MLD or CDT treatments? The frequency depends on the severity of your condition. Some patients benefit from weekly sessions, while others may need maintenance treatments less often. Giovanni will create a personalised plan for you. 12. Does private health insurance cover lymphoedema treatments? Some private health funds may cover part of the […]
Lymphoedema is a condition that can affect many individuals following a mastectomy, particularly those who have undergone lymph node removal as part of their breast cancer treatment. Understanding lymphoedema, its causes, symptoms, and management can help those affected navigate this challenging aspect of recovery. What is Lymphoedema? Lymphoedema is a chronic condition characterised by tissue swelling, usually in the arms or legs, due to an accumulation of lymphatic fluid. It often occurs when lymph nodes are removed or damaged, disrupting the normal flow of lymph fluid through the body. Another reason why someone could end up going through Lymphoedema is severe skin infections that damage the lymphatic system, radiation therapy, or invasive surgeries. Why Does Lymphoedema Occur After Mastectomy? During a mastectomy, when lymph nodes are removed (as in axillary lymph node dissection), the pathway for lymph fluid drainage from the hand and the arm can be compromised as the fluid has nowhere to be discharged at the surgery area. This disruption can lead to a buildup of fluid, resulting in swelling that, if left untreated, can create severe discomfort. While not everyone who has a mastectomy will develop lymphoedema, certain risk factors may increase the likelihood, including: The extent of surgery Radiation therapy Infection Obesity Lack of physical activity Previous or current other injuries to limb/shoulder Surgery was on the side of the dominant hand Be a smoker Symptoms of Lymphoedema post mastectomy The symptoms of lymphoedema can vary in severity and may develop gradually. Common signs include: Swelling in the arm, hand, or breast area A feeling of heaviness or tightness in the affected area Restricted range of motion in the shoulder or arm Skin changes, such as thickening or hardening Swelling doesn’t reduce just by holding the arm elevated Early Detection and Diagnosis Recognizing the early signs of lymphoedema is crucial for effective management. This would help prevent degeneration of the condition and reduce the chance of fibrosis building under the skin, which would lead to longer treatment and possible complications. If you notice swelling or other symptoms, Giovanni is here to help, so don’t hesitate to get in touch. To simplify the diagnosis process, Giovanni offers a 15-minute free phone consultation appointment. During this phone call, we can evaluate whether no pathologies need to be addressed by a GP or other medical staff or if the Lymphoedema management plan can be initiated. Managing Lymphoedema While there is currently no cure for lymphoedema, various management strategies can help reduce symptoms and improve quality of life: Manual Lymphatic Drainage (MLD) is a specialized massage technique that stimulates the lymphatic system and encourages fluid movement.At Melbourne Massage and Treatment in Fitzroy North, Giovanni specialises in the management of Lymphoedema with MLD. Combined Decongestive Therapy (CDT): CDT refers to the application of bandaging that Giovanni would do after the initial MLD treatment. Garments Wear: Wearing compression garments, such as sleeves or bandages, can help prevent fluid buildup and promote lymphatic drainage. Exercise: Gentle, targeted exercises can improve circulation and lymphatic flow. Giovanni at the end of the appointment would show a series of simple exercises that can help you in managing the Lymphoedema swelling. Skin Care: Maintaining skin hygiene and moisturization can prevent infections, which may exacerbate lymphoedema. Diet and Lifestyle: Maintaining a healthy weight and staying active can reduce the risk of developing or worsening lymphoedema. Surgery: In some cases, surgical options may be considered, such as lymphovenous bypass or vascularized lymph node transfer. Support and Resources Coping with lymphoedema can be emotionally and physically challenging. Support groups and counselling can provide valuable resources and community connections. Organizations like the Lymphatic Education & Research Network (LE&RN) and local cancer support services can offer information and support tailored to your needs. Conclusion Navigating lymphoedema after a mastectomy can be daunting, but understanding the condition and implementing effective management strategies can make a significant difference. Early intervention, education, and support are key components in minimizing its impact on daily life. If you or a loved one is facing this challenge, remember you are not alone—reach out to Giovanni and ask how Melbourne Massage and Treatment services can help. FAQ
A surgery is an invasive procedure that involves cutting your skin open to intervene on your musculoskeletal system and or the organs. Surgeries are often a life-saving intervention, but even a life-changing intervention. Once you undergo surgery, your body will never be the same. MLD post-surgery can help stimulate your Lymphatic System, supporting your recovery from this type of intervention. The lymphatic system is a body system that collects, moves and cleans the excess water and substances, like bacteria, viruses, dirt, tattoos, ink and more, from below the skin and then passes it to the bloodstream. Lymphatic System and Surgery. 80% of the Lymphatic System sits below the skin, and 20% sits within the deep fascia. When going for surgery and the skin gets cut, the superficial layer of the lymphatic system gets interrupted and is damaged. Unless we intervene, the lymphatic system will have a hard time regenerating. Indeed, the lymphatic system can regenerate if stimulated. The stimulation of the lymphatic system happens through touch, like with MLD or through the movement of the body, like exercises, even as simple as muscle contraction. MLD Post-Surgery – How It Works? Before or after surgery, it is recommended to stay active. This would allow the different body systems to keep working and maintain their function at their best till the time of the surgery. On the other hand, being active post-surgery is not always an option. In fact, during the post-surgery period, being active in the area that got stitches can be a contraindication, as the stitches could break. A cast may be present in other cases, and the muscle near the surgery can’t be moved. That’s where MLD can help stimulate the lymphatic system. By doing so, we can guarantee the circulation of liquids in the body, which is essential for a great recovery. But not only that Reducing the swelling around the cutting area or below the area affected by the operation would guarantee a fast return to movement. This is because the less swelling, the easier it is to move the joint. But also, MLD comes with a deep relaxation effect, which would put you in a state of relaxation and would help you move more easily. So MLD, by boosting the lymphatic system, reduces the swelling and allows the body’s natural healing process. What to do if you have to go for surgery then? If you are up for surgery soon and you have no contraindication to MLD, what you can do to guarantee a faster recovery is, keep moving as much as you can, stay active, and book yourself in for a few MLD treatments just for the days before your surgery is due. That would help with the Lymphatic System recovery, as a more robust and healthier Lymphatic System would recover faster. And as the risk of infection and post-surgery is under control, and your blood pressure is within the acceptable range (this depends on what type of surgery you had), get moving as much as possible and come back for a few more sessions of MLD. MLD post-Surgery – Does It Work For Any Surgery? C-section (preeclampsia) bone fracture liposuction carpal tunnel knee reconstruction hip replacement day hospital intervention MLD Post-Surgery – What You Should Know As often happens with cancer surgery, lymph nodes get removed if they are contaminated by cancerous cells. After surgery, you may also be treated with chemotherapy or radiotherapy in the area affected by the surgery. Lymph node removal prevents the cancer cells from spreading throughout the rest of the body, so it is often an inevitable step in this type of intervention. The risk of developing lymph node removal, on the other hand, is represented by the development of Lymphoedema after a cancer surgery, which depends on many different factors, including lifestyle, genetics, radiation therapy and more. I dedicated a series of blogs to the Lymphoedema topic, which you can find here. On the other hand, If you are concerned about Lymphoedema presentation, get in touch now to discuss how Giovanni can assist you. Giovanni’s Training For MLD I trained for MLD on two separate occasions with the Vodder Academy, whose courses in Australia are offered by Moving Lymph. The first course I did was in 2021, and I trained to work on patients who had an intact lymphatic system. My training was already complete to work with patients who undergo surgery. It was then in 2024 that I took a course for Lymphoedema therapy. This second had a strong focus on conditions where the lymphatic system is interrupted. Either because of a congenital presentation (primary lymphoedema) or because of external intervention (secondary Lymphoedema). FAQ – MLD post-Surgery
Arthritis can be described as the swelling and tenderness of one or more joints. Arthritis symptoms and types Symptoms include: joint pain stiffness reduce Range of Motion (ROM) Major Types: Osteoarthritis Rheumatoid-Arthritis Said so, Arthritis can be a consequence of another type of disease, like: Ankylosing spondylitis Gout Juvenile idiopathic Psoriatic A. Reactive A. Septic A. Thumb A. Those types of Arthritis manifest in different body areas and can display simultaneously. Symptoms can worsen with the ageing process. What is Osteoarthritis, and what causes it? We refer to osteoarthritis when the cartilage between the bonds that form a joint does wear out. Cartilage is a hard, slippery tissue that sits between 2 bonds, like the knee cap and femur, or between the bond of your fingers and toes. When this protective layer that keeps the two bonds separate does work out, the joint starts swelling due to an inflammatory process, and pain is consequently reproduced. The cause can be joint overloading due to chronic injuries or imbalance within the musculoskeletal system. For example, wearing high heels, or having a high foot arch, can lead to wear in the cartilage of the big toes. There is no cure for this type of arthritis, and pain management, through manual therapy and or medications is what so far can be done. What is Rheumatoid Arthritis, and what causes it? Rheumatoid A. is a disease type where the immune system attacks the joints. For rheumatoid arthritis, there are fewer known reasons why it can happen, but there are some factors that can play a role, such as: Family history Gender Obesity Joint injury Age Diagnoses To diagnose arthritis, you would have to see your GP and go for further investigations such as an X-ray, blood test or other medical investigations process. Massage and Treatment for Arthritis. For this type of condition, massage can be a useful therapeutic tool to reduce the pain sensation and manage the presentation. No massage technique can cure the presentation itself, but techniques like MLD are probably the most effective in pain management and symptom relief. Thanks to the direct stimulation of the Lymphatic System, MLD can inhibit the pain signal and relieve the person. As arthritis is often present in older people, we must check for any other condition or presentation that is an absolute contraindication to this type of treatment before commencing treatment. If this post is talking to you, and you need a massage, book your next session by clicking here.
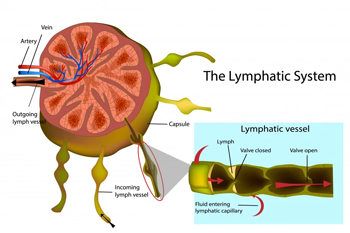
Lymph nodes (or lymph glands) are small lumps of tissue containing white blood cells that fight infection. They are part of the body’s immune system and filter lymph fluid, composed of water and waste products from body tissues. Introduction to Lymph Nodes Lymph nodes are located in different body areas. On average, we have approx 600 LN. In the neck area only, we find 160 LN itself. LN can vary in size and go from 2 to 30 mm. Lymph Nodes are connected by vessels, better known as afferent and efferent vessels. The afferent vessels carry the lymph to the lymph node, and the efferent vessels take the lymph away from the lymph nodes. So, the lymph nodes are also connected directly to the blood system, veins, and arteria. What is a lymph node made of? Despite the structures that enter and leave the lymph node, these cleaning stations are made of: Connective tissue capsule Supporting strands of connective tissue inside Below the marginal sinus, there are clusters of lymphocytes lymphoid follicles Artery, vein and nerve As for the filtering station, the lymph node is essential to ensure that no bacteria, viruses or dirt can access the blood system. Where we find no lymph nodes in the brain. Indeed, the lymph fluid around this area gets drained by the Optic and Olfactory nerve. Following then the position of the lymph nodes, we can define the watershed. MLD and Lymph Nodes. Lymph Nodes can occasionally be swollen, which happens when the body fights an infection. In my practitioner experience, I often have to refer to the lymph node concept to introduce the client to MLD treatment. Not many clients know about this technique; they are more familiar with Myotherapy or Thai Massage and Remedial Massage. Said so, the client who tried MLD are all well impressed with its benefit. During an MLD session, what happens is that with a gentle stretch and recoil of the skin, I help your lymphatic system to work faster. Consequently, that’s how swollen area gets reduced. In pushing your lymphatic system to work harder, the lymph node would receive more liquid to process. On the other hand, knowing where the lymph nodes are, is essential to ensure we push the lymph liquid in the right direction. If you haven’t booked your appointment yet and wish to set a goal for MLD, please follow this link.
When experiencing pain around the head, we talk about Headaches. Headache is a common condition, and for most cases, is not considered a serious illness. Migraine and headache. 4.9 million Australians experience migraine. Migraine is a specific type of headache, so consider that the number stated above is still a small figure. Headache and muscle. If you ever experience a headache, you may notice that the pain sensation does start from your cervical area. Or, by confronting yourself with who is around you, your headache pain pattern, is consistent, but it is different from the one of someone else. On the other hand, you may associate headaches to the result of a heavy drinking night, or of lack of water (which is why you get headaches after a heavy drinking night, by the way), but often headaches are there because of cervical muscle tightness. Wait, what? Yes, you did read right. How can we define then if the headaches come from muscle tension? So in order for this to happen, the muscle responsible for referring its pain up to the head must be tight or stretched out, and loaded with trigger points. As massage therapists, especially in the first consultation session, we would ask about headaches and if there are any, “where about do you feel the headache”? Indeed, the answer to this question is most luckily the giveaway to know which muscle is may responsible for your headaches. To confirm the suspicions, we would then assess your posture, looking for any muscular-skeletal unbalance, and then we would assess the Range of Motion (ROM). If the ROM show up to be limited on the muscle that we believe is responsible for the pain in the head, then most luckily we are halfway through the solution. I do say halfway through, a single massage session either Myotherapy, Remedial Massage, Thai Massage, or MLD is maybe not enough to release all the tension that is in needs to be alleviated to eradicate the headache. Said so, no journey starts, without doing the first step, isn’t it? When a headache is a Red Flag? For red flags, we refer to symptoms that may be present due to serious illness or condition. Some example includes clients who had a clinical history of stroke and or brain cancer, a recent car accident or recent head trauma, or blurred vision. If that’s the case, the next step is referring the client to a GP immediately for further investigation. What about the cervical muscle tension headaches type of presentation? As already mentioned in another blog post, the Occipital muscle can have headache type of pain in the lower section of the posterior side of the skull. If we then look into the area of the skull that seat above the ear, could be more tension from the Upper trap or Levator Scapulae. By keep moving more medially and above the head, Splenius cervis can refer to the medial superior side of the head and Splenius capitis to the middle top side of the head. Sternocleidomastoid, indeed, can refer to the frontal lobe of the skull. Now, all these muscles are sitting on the neck and throat and from above the shoulder. So, ensuring that those areas are free or not overloaded with tension can help in staying headache-free. Now, in this blog post, we are keeping the headache presentation type of pain to its simple aspects. On the other hand, the topic can be further discussed in person with Giovanni during your next massage appointment. Book now your next massage session, if you are trying to get to sort out your headache presentation. Other approaches to a headache-free life, out of massage therapy. There is a series of things that complimentary massage can help with to relieve headache pain. Exercises Keep yourself hydrated Good posture when seating and standing Good variety of food as diet intake Wearing glasses if needed. Meditation for stress management In conclusion, headache is a really common problem for all Australians, for both women and men. Don’t wait for your symptoms to get worse; you may not need to take medicine all the time if you have a headache, as the medicine will just numb the symptom but will not sort out the problem. If you are keen to learn more about where your headache may be coming from, book your next Massage Session today.
First Massage Appointment. At Melbourne Thai Treatment, a first massage appointment session does last a bit longer than a regular appointment. Indeed, if you go on the booking page, you may notice that the first appointment lasted 75mins. Why so?! Well, within the first appointment, as a therapist my aim is to track down your Clinical History. For doing so there is initially a form to fill in and in a second stage few subjective questions that I am going to ask. Questions are like: “What do you do for work?” “What sports activity do you do or did?” “On what side do you sleep?” “Are you Right or Left Handed?” Ext… These and other questions, relevant always to the presentation that you come in with, are for me therapist essential to understand how you end up having the pain or discomfort that I have to remove or reduce. Obviously, those questions asked during the first massage appointment can take a bit of time to be answered Occasionally an answer gives space to a new question. Said so, the more specific are the answer more I can narrow down the clinical situation. If this post is talking to you, book your next massage session by clicking here. As per result, will be easier to find a path to alleviate pain and discomfort. On the other hand, as the session last longer than a regular visit, as a therapist I charge a bit more. For a Remedial Massage and a Thai Massage a first appointment session would last 75mins. About MLD a first Massage session would last 60 minutes. Indeed, with this post, I would like to share and explain to any clients that the first appointment is not more expensive because I am greedy. Is through, the time we spend doing the massage itself is per usual the same time that we would spend during a general consultation. But, that initial time that we spend working out your Clinical History, will save time after actually treating the condition. In conclusion, I would not see the first appointment as an extra expense, but as an investment in your health. Before we find out what’s the cause of your pain, and discomfort before I can create a proper treatment for it.
- 1
- 2