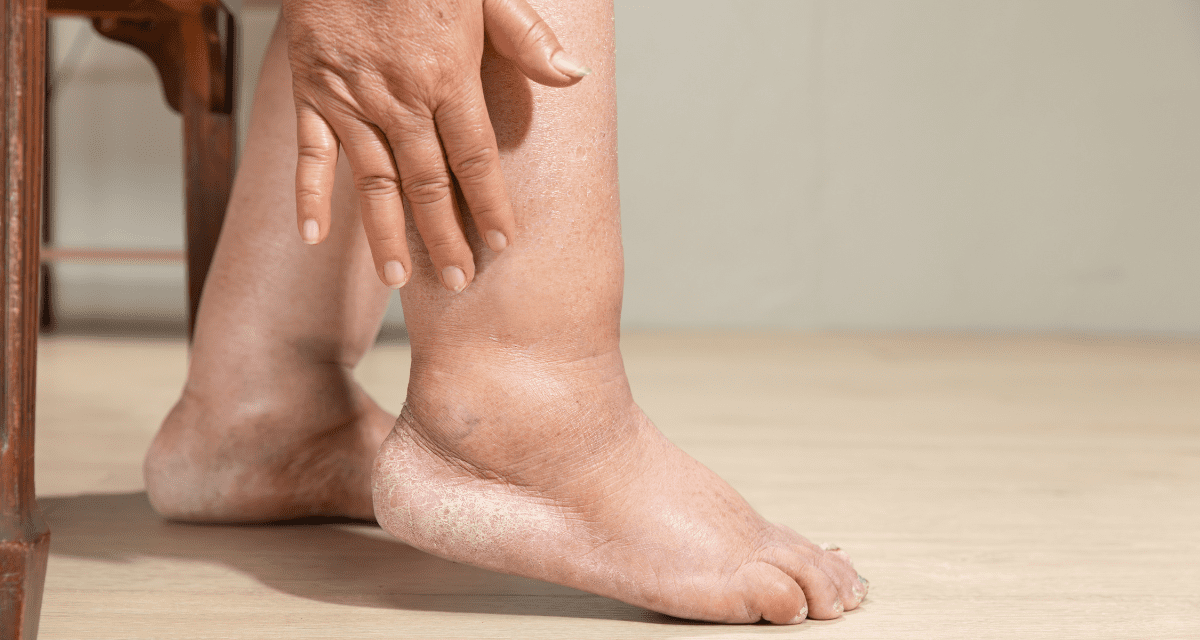
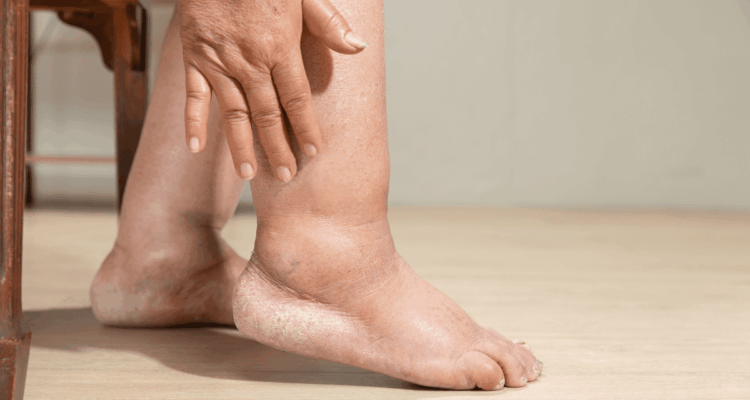
If you’ve noticed swelling in one or both of your legs, it’s natural to feel concerned. Leg swelling, or severe oedema, can have many causes, and understanding the difference between them is key to getting the proper treatment. In this blog, we are going to discuss the different reasons why legs may swell, and how to recognise the key factors of Lymphoedema, and when you’d better consult a GP to address the other issues
Is the Leg Swelling in One or Both Legs?
To start, we want to observe whether the swelling is monolateral or bilateral —i.e., on one leg or both.
Unilateral (one leg):
In this case, we may look at a lymphoedema, but we also have to consider a possible vascular-related cause such as deep vein thrombosis (DVT), venous or arterial insufficiency, or trauma.If DVT is suspected, urgent referral is essential. DVT symptoms include:
- Redness
- Heat
- Pain
- Possible post-flight or prolonged period of immobilisation
If it’s venous or arterial insufficiency or injury-related, compression therapy may be started once it’s safe.
- A specific scan of the vascular system can assist with diagnosis. Your GPs should be able to refer you to a vein specialist to further investigate the presentation.
Bilateral (both legs):
This may indicate a more systemic or internal cause, such as:- Heart, liver, or kidney disease
- Low protein levels (hypoalbuminaemia)
- Thyroid issues
- Medications or reduced mobility
Lymphoedema is unlikely to be bilateral, unless severe damage happens to both limbs or the abdominal area, where the lymphatic system is completely damaged. In this case, we still want to rule out any other conditions and dive deep into your medical history.
Symmetrical vs Asymmetrical Leg Swelling
Symmetrical swelling often suggests internal illness or lipodema, which is a chronic fat distribution disorder that can mimic lymphoedema but is not caused by lymphatic failure.
Asymmetrical swelling, where one leg is noticeably more swollen, could point toward lymphatic or venous problems.
Understanding the Type of Oedema
Once vascular or systemic causes are ruled out, the swelling is classified into types:
Venous Oedema
Usually linked to chronic venous insufficiency, and the treatment include:
Managing weight and mobility
For any MLD treatment and/or intense exercise activity, a safety disclosure from the GP or specialist may be recommended.
Lymphatic Oedema (Lymphoedema)
Lymphoedema can be primary (congenital or inherited) or secondary (caused by surgery, infection, trauma, or cancer treatment). Either way, if left untreated, it can lead to skin thickening and fibrosis. Furthermore, if the skin suffers a cut or a crack, it can get infected. Therefore, the earlier the intervention, the better.
Treatment:
Skin care and gentle exercise
Multidisciplinary management
I wrote a specific blog about the characteristics of Lymphoedema and explored the possibility of excluding other conditions. Read it here.
Mixed Oedema
When a mixed oedema is the presentation, a referral from a GP is essential to ensure there are no contraindications to MLD or compression therapy for treatment.
When both venous and lymphatic systems are involved.
Needs a combined approach of compression, skin care, exercise, and lifestyle support.
Getting the Right Diagnosis and Support
If you suspect lymphoedema, it’s essential to get a clinical assessment. At Melbourne Massage and Treatment in Fitzroy North I can help you with that.
Things that we will look into are:
The pattern and duration of swelling
- Does the swelling worsen in the heat?
- Where does the swelling start from?
Skin condition
- Is the skin intact?
- Does the skin have any elasticity?
Medical history and possible triggers
- Family history of Lymphoedema
- Any history of cancer or general surgery?
Response to elevation and compression
- Does elevating the leg make a difference in swelling reduction?
- Does adding compression to it help?
Early diagnosis helps prevent complications such as infections or long-term tissue changes.
Bokk Now A 15 minutes FREE Online Consultation
Final Thoughts
Swelling in your leg doesn’t always mean lymphedema, but it’s something worth checking out. Things to look into, to narrow down the possibility of having lymphoedema are:
- Swelling in one leg or both
- Symmetrical or asymmetrical
- Attemptive Medical history check
Remember: Lymphoedema is manageable with the proper care — and early action makes all the difference.
FAQ — Leg Swelling: Lymphoedema or Something Else?
What causes leg swelling? A: Leg swelling (oedema) can result from vascular issues like venous insufficiency or DVT, internal illnesses such as heart, liver, or kidney disease, or lymphatic disorders like lymphoedema.
Is swelling in one leg more concerning than in both? A: Yes, swelling in one leg (unilateral) often points to DVT, venous disease, or lymphoedema. It should always be checked by a healthcare professional.
What does bilateral leg swelling mean? A: Bilateral swelling (in both legs) may suggest systemic issues such as heart failure, kidney disease, low protein levels, or thyroid imbalance.
How can I tell if it’s lymphoedema? A: Lymphoedema typically causes persistent, asymmetrical swelling that doesn’t go down with elevation, along with a heavy or tight feeling and possible skin thickening.
What is the difference between lymphoedema and lipodema? A: Lipodema is a symmetrical fat distribution disorder causing tenderness and bruising, while lymphoedema results from lymphatic dysfunction and usually affects one limb more.
How is venous oedema treated? A: Venous oedema is managed through compression therapy, leg elevation, exercise, and addressing any underlying venous insufficiency.
What treatments help with lymphoedema? A: Lymphoedema is managed with Manual Lymphatic Drainage (MLD), compression garments, skin care, and gentle exercise. Early intervention prevents infection and fibrosis.
Can I have both venous and lymphatic oedema? A: Yes — this is called mixed oedema. It needs a combined treatment plan and GP referral to ensure compression or MLD therapy is safe.
When should I see a GP about leg swelling? A: If you notice sudden swelling, redness, pain, or heat (especially after long travel), seek medical attention immediately to rule out DVT. Persistent or unexplained swelling should also be assessed by your GP.
Can Melbourne Massage and Treatment help diagnose lymphoedema? A: Yes, at Melbourne Massage and Treatment in Fitzroy North, I can assist you to determine if you are presenting with lymphoedema or if you may need to see the GP for further investigations regarding other presentations.

Giovanni La Rocca
Giovanni moved to Melbourne, Australia, from Italy in 2008 and became a citizen in 2017. He started studying massage therapy in 2016, then completed a Bachelor of Health Science in Clinical Myotherapy in August 2024. During those years, he also specialised in Thai Massage and Manual Lymphatic Drainage for presentations like Lipoedema and Lymphoedema. Nowadays, he runs his clinic in Fitzroy North, Melbourne, where he integrates movement therapy into his practice to enhance overall well-being. He also values meditation, having completed several Vipassana courses. Committed to continuous learning, he aims to share his expertise in integrated therapies to help others achieve balance and resilience.