A surgery is an invasive procedure that involves cutting your skin open to intervene on your musculoskeletal system and or the organs. Surgeries are often a life-saving intervention, but even a life-changing intervention. Once you undergo surgery, your body will never be the same. MLD post-surgery can help stimulate your Lymphatic System, supporting your recovery from this type of intervention. The lymphatic system is a body system that collects, moves and cleans the excess water and substances, like bacteria, viruses, dirt, tattoos, ink and more, from below the skin and then passes it to the bloodstream. Lymphatic System and Surgery. 80% of the Lymphatic System sits below the skin, and 20% sits within the deep fascia. When going for surgery and the skin gets cut, the superficial layer of the lymphatic system gets interrupted and is damaged. Unless we intervene, the lymphatic system will have a hard time regenerating. Indeed, the lymphatic system can regenerate if stimulated. The stimulation of the lymphatic system happens through touch, like with MLD or through the movement of the body, like exercises, even as simple as muscle contraction. MLD Post-Surgery – How It Works? Before or after surgery, it is recommended to stay active. This would allow the different body systems to keep working and maintain their function at their best till the time of the surgery. On the other hand, being active post-surgery is not always an option. In fact, during the post-surgery period, being active in the area that got stitches can be a contraindication, as the stitches could break. A cast may be present in other cases, and the muscle near the surgery can’t be moved. That’s where MLD can help stimulate the lymphatic system. By doing so, we can guarantee the circulation of liquids in the body, which is essential for a great recovery. But not only that Reducing the swelling around the cutting area or below the area affected by the operation would guarantee a fast return to movement. This is because the less swelling, the easier it is to move the joint. But also, MLD comes with a deep relaxation effect, which would put you in a state of relaxation and would help you move more easily. So MLD, by boosting the lymphatic system, reduces the swelling and allows the body’s natural healing process. What to do if you have to go for surgery then? If you are up for surgery soon and you have no contraindication to MLD, what you can do to guarantee a faster recovery is, keep moving as much as you can, stay active, and book yourself in for a few MLD treatments just for the days before your surgery is due. That would help with the Lymphatic System recovery, as a more robust and healthier Lymphatic System would recover faster. And as the risk of infection and post-surgery is under control, and your blood pressure is within the acceptable range (this depends on what type of surgery you had), get moving as much as possible and come back for a few more sessions of MLD. MLD post-Surgery – Does It Work For Any Surgery? C-section (preeclampsia) bone fracture liposuction carpal tunnel knee reconstruction hip replacement day hospital intervention MLD Post-Surgery – What You Should Know As often happens with cancer surgery, lymph nodes get removed if they are contaminated by cancerous cells. After surgery, you may also be treated with chemotherapy or radiotherapy in the area affected by the surgery. Lymph node removal prevents the cancer cells from spreading throughout the rest of the body, so it is often an inevitable step in this type of intervention. The risk of developing lymph node removal, on the other hand, is represented by the development of Lymphoedema after a cancer surgery, which depends on many different factors, including lifestyle, genetics, radiation therapy and more. I dedicated a series of blogs to the Lymphoedema topic, which you can find here. On the other hand, If you are concerned about Lymphoedema presentation, get in touch now to discuss how Giovanni can assist you. Giovanni’s Training For MLD I trained for MLD on two separate occasions with the Vodder Academy, whose courses in Australia are offered by Moving Lymph. The first course I did was in 2021, and I trained to work on patients who had an intact lymphatic system. My training was already complete to work with patients who undergo surgery. It was then in 2024 that I took a course for Lymphoedema therapy. This second had a strong focus on conditions where the lymphatic system is interrupted. Either because of a congenital presentation (primary lymphoedema) or because of external intervention (secondary Lymphoedema). FAQ – MLD post-Surgery
Tag Archives: brunswick
As previously spoken in another blog post, sitting on the floor and working at the pc would be a better anatomical position than sitting on a chair. Why does sitting on the floor work better than sitting on a chair? Sitting on a chair is uncomfortable, especially in the long term. As a massage therapist, most of my clients are people who have cervical pain or suffer from headaches. Sitting at a desk for hours does more damage than you may realise. So, let’s start with the lower body portion. Staying seated on a chair does direct pressure on the thigh, and by doing so, muscles like the hamstring and gluteus muscles get compressed. By compressing this group of muscles, they get weak and stop functioning as they should. In addition, direct pressure is also applied to the sciatica nerve, the main nerve of the lower body portion. The piriformis often compresses the Sciatica nerve. This muscle runs beneath the Gluteus Max and connects the medial portion of the sacrum to the greater trochanter of the femur. So, the deactivation of those muscles would then manifest itself when we try to walk or, in any case, extend the leg. As the “firing pattern” blog post shows, the hamstring and gluteus max muscles are crucial in leg extension and help prevent lower back pain. This is what happens to the muscle part of the lower body portion. But this is not the only issue the body faces with so many hours sitting on a chair. There is more. So sitting on a chair does limit the body’s movement. The decline of the body’s movement creates a cascade of side effects, including mobility reduction in joints like the Hip, Ankle, Feet, and Thoracic. As all those joints don’t move, there is also a diminish in the proprioception body/brain. Another issue is the compensation of the stability joint over the mobility joint. Indeed, when a mobility joint gets stiff, the stability joint above and below would try to compensate. What’s a common finding pain-wise with sitting on a chair for long hours? The prevalent finding is a sore neck. The sore neck happens as the thoracic stuff up. Indeed the lower cervical portion of the vertebrae, which are stability joints, try to compensate for the thoracic stiffness and, in the long term, would cause neck pain, shoulder pain and headaches. Sitting on the floor can improve mobility. Sitting on the floor can help improve your mobility by allowing you to move your body in many different ways without the need to stand up. That movements are what your body needs as mobility exercises. That movement is your body’s way of improving its posture. Indeed, movement is a crucial component in pain prevention. And this doesn’t happen on a chair. How to switch habits? As for all the habit changes, this has to be gradual and not radical. So, start sitting on the floor for 1 hour a day. Give yourself the time to adapt to the change. Slowly you can incorporate more hours, but not in a row. Maybe one hour in the morning and one in the afternoon. Also, incorporate some standing time to sitting on the chair and floor. Implement change, too, within your training. You are doing something new, and your body needs to adapt. As shown in this clip, start, start implementing a habit of sitting on the floor by doing step-by-step movements: Step 1: Move one leg forward, and bend down the other knee. Step 2: Bring both knees down Step 3: Swing the lower leg to the side (either Lx or Rx) Step 4: Let your body weight go, and sit down Step 5: Now let your lower leg come forward and sit cross-leg. Step 6: Do from step 5 to step 1 in reverse By clicking here, and here you will find the links to a Thai Yoga exercise that can help a lot with improving hip mobility.
Fibromyalgia is a health condition that causes widespread pain and sensitivity to touch. This type of condition is more common in women than in men, and it is still unknown to science why some people may suffer from Fibromyalgia, even though it is known that stress can play a significant role. On the other hand, genetics can also be the reason why someone can suffer from Fibromyalgia. Fibromyalgia signs and symptoms Symptoms of fibromyalgia may include: headaches sleep disturbances numbness and tingling of the hands and feet muscle and joint stiffness after a period of rest (after sleeping) restlesconditionsndrome Diagnosis of fibromyalgia To be diagnosed with Fibromyalgia, you have to visit your GP first, who may refer you to a specialist. The most widely used clinical criteria for diagnosing fibromyalgia are sourced from the American College of Rheumatology: pain and symptoms over the past week, based on the total of: number of painful areas out of 18 parts of the body The severity of these symptoms: fatigue waking unrefreshed cognitive problems (that can be memory or thought) Plus other general physical symptoms Symptoms lasting at least 3 months, with unchanged Exclusion of other health problems that could reproduce the pain and other symptoms. Treatment and management So, currently, there is no direct cure for fibromyalgia, but there are many treatments that can help manage this condition, like: improving your sleep routine more of a balanced diet relaxation meditation exercise MLD You can also talk to your GP to see what medications can reduce or manage the pain. How MLD can help with Fibromyalgia? Manual Lymphatic Drainage (MLD) is a gentle, non-invasive manual therapy that aims at boosting the Lymphatic System. Along with the delivery of MLD, the therapist would gently stretch your skin and let the skin recoil, with a pain-free touch. This constant repetitive skin stimulation has a positive impact on the parasympathetic nervous system, which is the portion of the nervous system responsible for what we call “rest and digest” mode. Other benefits delivered from MLD are: Oedema reduction Deep relaxation Inflammation reduction Body’s fluid stimulation Skin health improvement Chronic pain management
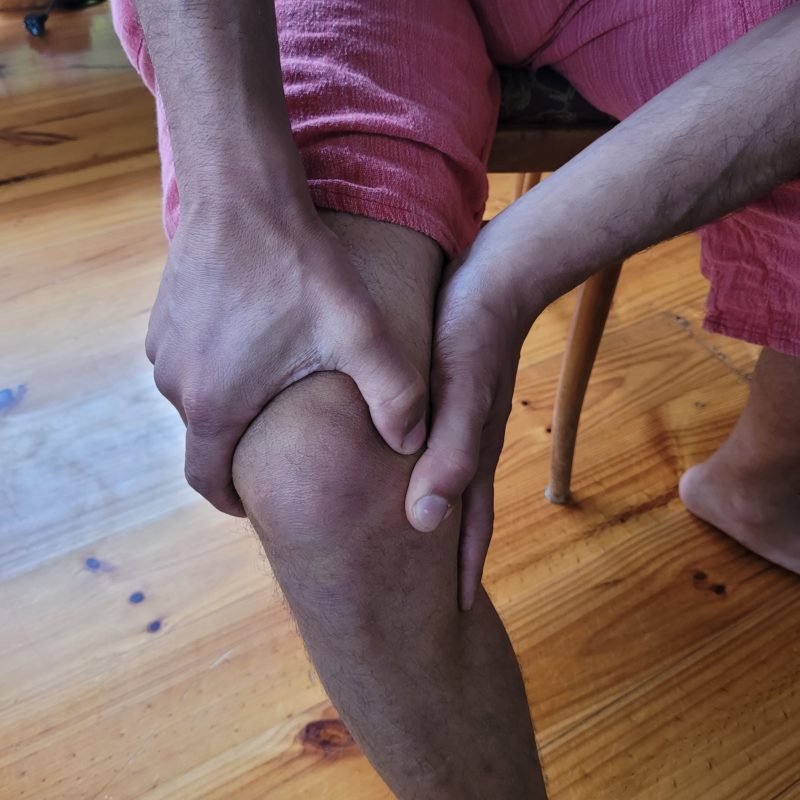
Patellar tracking disorder is a condition that occurs when the patella, also known as the kneecap, moves out of its original place when the leg straightens or bends. What causes Patella Tracking Disorder? In most cases, the kneecap shifts towards the outside of your leg, called “Lateral Patella tracking”. Occasionally in some cases, it may shift toward the medial side too. Why this shift happens due to the force applied to the kneecap itself. It was said that the knee joint is a hinge joint, which connects the tibia and fibula of your leg with the femur. The kneecap is held in its natural position by ligaments on the medial and lateral sides and by tendons on the top side. Below the patella is a cartilage layer that helps the patella glide along the femur’s groove. When the cartilage below the patella does wear out, it can create pain and discomfort in the knee. The misalignment of the patella results from tendons, muscles or ligaments that are either too tight or too loose. Lateral patella tracking VS Medial patella Tracking In the case of Lateral Patella Tracking, the Vastus Lateralist is over-developed compared to the Vastus Medialis or the IT Band (Iliotibial Band) pulling too much. Vastus L. can overtake Vastus M’s strengthening due to the muscle size. Indeed the V.L. is visibly bigger than the V. M. On the other hand, tension along Gluteus Max and or tensions in the TFL can play a role in the pulling of the IT band. Are you in Pain, and you suspect to have a Patella Tracking disorder? Get in touch with Giovanni now. [contact-form][contact-field label=”Name” type=”name” required=”true” /][contact-field label=”Email” type=”email” required=”true” /][contact-field label=”Website” type=”url” /][contact-field label=”Message” type=”textarea” /][/contact-form] Risk factors for Patella Tracking Disorder Here is a list of reasons that can lead to Patella Tracking Disorder: Footwear Running Weakness in the quads muscle Unbalance of muscle between the inner and outer regions of your tight Sports that require excessive knee bending, jumping or squatting Improper form or techniques while working out or during sports activities Overweight Genetics (structural reasons) Incidents or trauma to the knees Malformation within the femur bond Damaged cartilage Symptoms Pain is the most symptom of Patella tracking disorder. The pain caused by this condition can occur during regular activity such as standing up, walking and or sitting down. Any knee movement can recreate the pain. In the case of arthritis, the pain can be more intense, and swelling is present at the knee joint. Treatment Options At Melbourne Massage and Treatment, the services available for Patella tracking are multiple. Depending on the severity of the condition, Myotherapy treatment and or MLD are the most recommended. Thanks to Dry Needling and/or Joint Mobilisation therapy, Myotherapy treatment can help rebalance the muscle forces surrounding the knee cap. On the other hand, MLD can help in reducing the inflammation and the swelling present eventually on the knee joint. What then Giovanni would look in, too, is also the mobility of ankles and hips. The correct mobility of these two joints would ensure that the knee is not compensating for the poor joint quality of movement, which can be part of why the patella tracking disorder is in the first place.
On the occasion of my 4th time in Chiang Mai, since 2018, I am dedicating this post to Thai Massage in Pichest Boonthumme Style. When and where did it all start? In March 2018, I started studying and practising Thai Massage. I came here to Chiang Mai, to see Pichest Boonthumme, after a friend’s recommendation. I was looking into finding someone, that could teach and share a massage technique, not only based on sequence and repetitive movement. As often happens, as long as you ask, what you are looking for will show up. And now, after 3 long years of the Covid pandemic and limitations on travelling, I am back in Chiang Mai. This is my first trip out of Australia since 2019, so it was an excellent way to celebrate the freedom of travelling, once again. Being back at Pichest Thai Massage School is always challenging. Even though I spent the last three years training for Remedial Massage, Myotherapy and MLD, when I came here, there was always something new to learn. Along with that new practice, there is always the Thai/Buddhist philosophy aspect of how to see things. I did really like the way Pichest, with his limited English, can explain the complex way life can present and shape, and how simple it is to learn how to deal with it. Just observe the breath. Well, no surprise, as this is the principle of Vipassana Meditation itself. That said, what most often happens is that people who come here to study with Pichest ask to learn how to breathe, even before they can receive a massage. Many people come here because they heard of how good Pichest is at giving massages. And they all come with the expectation to get fixed. And it is just hilarious to see how Pichest, every time, turn these people away from treatment and asks them to learn how to breathe. We are used to thinking of Thai Massage as a painful approach, a strong technique, and it is. But not because we are physically suffering means we are getting better. If we can’t deal with the pain if we stop breathing as we perceive that pain, we keep creating tension in the body and will not let the healing process happen. Breathing during a massage comes with a series of benefits: helps the blood to be pushed around Oxygenation of the muscle tissues Improve relaxation It helps in dealing with the pain reproduced by the touch of a tense area Stimulates the Vagus Nerve, which controls the parasympathetic nervous system On the other hand, before we start doing deep work on the body, the patient does better take 5 minutes to practice breathing, and the first area to work would be around the posterior portion of the shoulder and the hip or Tibia area, to stimulates the blood flow within the body. In conclusion, Thai Massage as we know it in the West is a bit of a distortion of the real thing. Thai Massage, as with any deep tissue massage, can replicate pain, but the pain must be good, not sharp. The pain must help to release tensions and not increase them. And to be a Thai Massage therapist, you better know your anatomy well. Are you curious to find out what a traditional Thai Massage is like? Bookings are open for Traditional Thai Massage at Melbourne Massage and Treatment Fitzroy North studio.
Frozen shoulder is also known as per the name “adhesive capsulitis”. A frozen shoulder as per the name is a shoulder that would barely move. Both signs and symptoms typically begin slowly and then get worse. Recovery time is subjective. Causes and Symptoms of frozen shoulder. Causes A common cause of a Frozen Shoulder is having to keep a shoulder still for an extended period, like after an accident. Even if it is not clear yet why there are also psychosomatic reasons why a shoulder can get frozen. Another reason why a shoulder could get to freeze is traumatic events, such as a high level of stress or a physical accident. On the physical level, what happen is that connective tissues that surround the shoulder joint, like a capsule, thickens and tightens around the shoulder joint, and by doing so, it does restrict the joint’s movement. Symptoms Frozen Shoulder symptoms developed in 3 different stages. The stage’s timing is subjective. Freezing stage Shoulder range of motion starts decreasing, and pain shows up/increases. Frozen stage The Shoulder would freeze up. The movement is minimal, even though it is less painful. Thawing stage In this stage, the range of motions are slowly coming back Pain can be worst at night. This may happen because of the sleeping position or because the sensory feeling is more acute at night than in the daytime when the body perceives more sensations. Suffering from Frozen Shoulder and need some help. Book now an MLD treatment at Melbourne Massage and Treatment. Risk factors for Frozen Shoulder Age and gender Women are more luckily to suffer from this condition. Also, age plays a crucial role in this type of pathology. People 40 and over are luckier indeed to develop F.S. Systemic diseases Here is a list of specific conditions that can increase the possibility of suffering from F.S.: Diabetes Overactive thyroid (hyperthyroidism) Underactive thyroid (hypothyroidism) Cardiovascular disease Parkinson’s disease Prevention There are not many preventive factors when it gets to F.S. This is because the main cause of F.S. is holding the shoulder back from doing movements, due to a previous injury, most of the time. What can help, and this is how Melbourne Massage and Treatment services come in handy is to do MLD sessions on the area surrounding the injury. How MLD can help by stimulating the lymphatic system work and boosting the recovery process. Also, MLD would help in reducing inflammation. Other massage technique such as Myotherapy or Remedial Massage and or Thai Massage, is not as effective for this type of condition. Another successful method that can help once Frozen Shoulder is already developed is by using Hydrodilatation. This methodology consists in injecting sterile water into the joint capsule to stretch the open space and bring the shoulder back to its ROM.
Parkinson’s disease is a brain disorder that causes unintended or uncontrollable movements, such as shaking, stiffness, and difficulty with balance and coordination. Symptoms usually begin gradually and worsen over time. As the disease progresses, people may have difficulty walking and talking. (1) The mechanism behind Parkinson’s disease. So far, we know that Parkinson’s affects more men than women. Regarding the mechanism behind Parkinson, we have to look into the loss of neuro cells in the Basal Ganglia, a brain area that controls the body’s movement. These specific neuro cells produce a brain substance called Dopamine, which is related to body movement. Still, scientists don’t know what can make the cell in the Basal Ganglia die. Along with the loss of dopamine production in the Basal Ganglia, for those who suffer from Parkinson, there is also to consider the loss of the nerve endings that produce norepinephrine. Norepinephrine is the primary chemical messenger of the sympathetic nervous system (SNS). As the Sympathetic Nervous System controls many automatic body functions, such as heart rate and blood pressure, this can explain how the symptoms related to Parkinson’s itself. Parkinson’s disease Symptoms A tremor in hands, arms, legs, jaw, or head Muscle stiffness, where muscle remains contracted for a long time Slowness of movement Impaired balance and coordination, sometimes leading to falls Other symptoms may include: Depression and other emotional changes Difficulty swallowing, chewing and speaking Urinary problems or constipation Skin problems How can massage help? Scientist suggests that massage can help reduce muscle stiffness and rigidity, symptoms often found in Parkinson’s patient. Massages are also suitable for reducing stress and promoting relaxation. Said so, receiving a massage enables the patient to individualism what is more sensitive to the touch and what can promote more benefit if stimulated. Indeed, at the end of the massage, specific exercises can focus on relieving tension from that body’s area. At Melbourne Massage and Treatment, Giovanni offers various services that can help reduce tensions with Parkinson’sons’ disease. Since Parkinson’s is a condition found mostly in older people, treatments like Myotherapy, Remedial Massage and MLD could be more indicated. Said so, regarding MLD, we always want to double confirm that there is no other condition, related or not related to Parkinson that could be partial or absolute contraindications. Reference: 1) https://www.nia.nih.gov/health/parkinsons-disease
Sitting on the floor is the new mobility movement. Sitting at the desk and sitting on the floor. Working in the office is a challenging task for the body, and in the last few years, something made this task even worst. Covid-19 forced millions of people worldwide to work from home. Consequently, many people reduce their daily movement activity and start increasing their stress response to work and everyday life. But what does covid-19 have to do with seating on the floor, you may ask yourself? Well, for convenience, and other rules, such as hygiene too, we nowadays spend most of our time sitting on chairs. At least within Western cultural settings. Asian Squat But as we all know, floor seating is an ancient practice in the East side of the world. In our collective mind, we all can refer to Asian people squatting anywhere they can, and with not much problem. In the West, squatting is associated with going to the gym, training, and being sporty. It is funny, isn’t it?! So, that’s where covid-19 is linked to seating on the floor. I am working from home and sitting on the floor. Due to the covid pandemic, many people have started working from home. But the home ergonomics for office work differ from those in the office. In addition to this, we have to add that as big and comfortable as a chair can be, it is always a chair. Indeed, the chair is a silent killer. Sitting on a chair limits our ability to move around as discomfort arises. Think now about sitting on the floor and standing back up. For the average adult, doing this task is not a comfortable thing. Why so? Well, because we are not used to it. All this year, sitting on a chair did reduce our body adaptability to the ground sitting. Sitting on a chair for long hours would: stiff up the hips, which are in constant flexion increase pressure on the Lumbar back arch the thoracic area, with an increase in kyphosis reduce the necessity for mobility In fact, within 20 minutes of no movement, a muscle would adapt to the shape it is sitting into. On the other hand, as the muscle starts losing its neuroplasticity, the joints controlled by those muscles would start stiffening up too. This is such a domino effect that it would break the equilibrium along the stability/mobility joints chain. How to prevent this? Well, sitting on the floor is a good start. Sitting on the floor comes with the benefits of more mobility options. As we may feel uncomfortable with the sitting position, changing position would be a spontaneous and comfortable act once on the floor. But as we are so used to sitting on chairs, starting sitting on the floor for 8 hours a day can be challenging. So, rather than sitting on a chair all day, initially switching between floor sitting, chair and standing up is good. This process would allow the body to slowly break the bad habit of rounding onto the desk from the stiff chair seating. Also, the body is not designed to either sit on a chair or stand up for so long for so many days. So the habit of changing position would improve mobility, and with it, many other things would come down to and ease. In conclusion, to improve the Upper Cross Syndrome (UCS) presentation of someone who spends long hours sitting at a desk, the steps to take are: reduce the symptoms of pain and discomfort in the Cx area start losing up the thoracic area Improving hip mobility allows the person to spend more time on the floor. The work that needs to be done within the thoracic area is to lose the vertebrae by doing some mobs and reducing tension on the lat dorsi muscle. In this next post, we will look into the following: How to sit on the floor and how to stand back up Exercises that can help to improve the floor seating time. Would you like to improve your mobility? Book Now a Thai yoga class with Giovanni or a Massage session to learn more about what can help you.
Mobility is the degree to which a joint can move before being restricted by surrounding tissues. Not all the joints taught are considered mobility joints. The Mobility and Motility Joints Theory Starting from the big toes joint and moving up the body to the upper cervical joints, we can count one by one a mobility joint alternating with a stability joint. So this would be like this: Big toes – M. Metatarsal – S Ankle -M Knee – S Hip – M Lumbar -S Toracic – M Lower Cervical – S Upper Cervical – M Shoulder – M Elbow – S Wrist – M Tarsal – S Fingers – M The major differences are: A Muscular structure surrounds mobility joints Stability joints are surrounded by ligaments and tendons Mobility joints move in more planes than stable ones. The stability joints, indeed are essential to the body mechanics to ensure that gravity and force applied to the body by its own weight are well distributed. First thing first. Now, if we plan to strengthen our body, like by going to the gym, running or doing any sports activity, ideally we would like to ensure that the mobile joints can deliver the minimum required of ROM. Why? Well, if the mobility joints are stiff or not mobile enough, the priority of moving would not diminish and the stability joints, are going to do their best to compensate. But let’s see this with an example. Mark (name of fantasy) who is an office worker, spends about 40 hours a week at his desk, and to reduce the work and life stress decided to start a routine run 3 to 4 times a week for 1 hour per time. Mark thinks that to go for a run, you don’t need training and has no clue about the mobility, stability and strengthening chain. After a few weeks that is enjoying his new routine, Mark start experiencing knee pain. Mark also didn’t realise that due to the long hours of sitting at the office, his hips joint are tight, and his external rotators, such as the gluteus max and piriformis, are tight. As per consequence, when Mark stands up, the angle of the gate (AOG), which refers to the rotation of the foot in a standing position, is up to 4 toes per side. (3 toes is the max AOG we expect in the foot). Now, what happens next is that when Mark goes running, his ankle mobility and hip mobility are visibly restricted. So, he will lean forward with the upper body, by having tight hips, and strike the floor with the feet externally rotated, so all the body weight will be loaded in the middle of the foot. As a result, the Stability Joint that sits between the ankle and hip, so the knee, will compensate for the other two joint dysfunctions. In this case, the knees would take extra pressure medially and stretch out laterally. So, what should Mark do?! Well, initially, to stop the pain from happening, stopping running would be a good idea. Said so, that would not fix the problem. What Mark should do, is: Massage to boost the change within the tight joints and reduce the knee pain Start a mobility program to improve the Hip and Ankle functionality Exercises that aim to reduce tension in the external rotator reinforce the internal rotator (Gluteus Med and Min) Train on how to run These are the basic steps to implement a model of Mobility, Stability, and Strengthening. Does this model apply to other sports activities? Of course, it does. Visualise your body as a giant mechanical machine made of rope and hinges. The mechanical result will not be ideal if the hinges are stiff and the ropes are tight. To improve the result, each component needs to be looked after. So what message would be the most recommended? Along with Melbourne Massage and Treatment services, Thai Massage, Remedial Massage, and Myotherapy are soon the most recommended services Giovanni offers to improve the body’s mobility. Regarding mobility training, Thai Yoga is also an effective way to improve joint mobility, as these exercises focus primarily on improving joint mobility. What there is to consider is the patient’s presentation, medical history and pre-existent injuries. If there are no significant concerns, I suggest Thai Massage as the best approach. For people who have presentations such as Diabetes n1 or hypertension, Myotherapy treatment or Remedial Massage is mainly recommended.
A bunion is a bond malformation at the base of the big toes. The leading causes for bunion are: foot stress high foot arch wearing high heels narrow shoes A bunion is often correlated to Osteoarthritis. Osteoarthritis is due to the cartilage degeneration that separates 2 bonds. In this case, the 2 bonds are at the base of the big toes. This result in pain at big toe extension and during walking. Bunion’s Symptoms Visible malformation, like a bump, on the side of the big toes joint; Sharp pain in the thumb; Difficulties in walking; Stiffness; The big toes point laterally towards the other toes Intervention About what to do for a bunion presentation is to get in touch with a podiatrist as soon as possible. Massage therapy is recommended too, but it is a limited tool for helping in fixing the issue. Along with Remedial Massage, Thai Massage, Myotherapy and MLD treatment, what can be done to alleviate the pain is to treat the surrounding structures, such as the plantar of the foot and the metatarsal area. So, can it alleviate bunion pain and or invert the condition? Yes, it is. Today’s blog post is called “Happy Bunion Story”. So, back in Dec. ’21, Steph start having foot pain, due to osteoarthritis. The reasons behind her conditions are: High foot arch Long hour standing up for work (she is an amazing Wedding and Fashion photographer) Wearing high heels (she used to do modelling) The combination of those resulted in a degeneration of big toes cartilage and a bunion forming. As Steph complained about pain in the big toes, I told her what possibly was happening there. Soon after, she visited her GP and got some X-Ray done, and the result was not much of a surprise. After finding out about her new condition, Steph consulted a podiatrist, who suggested starting a daily routine of exercises for her big toes. Resisted big toes flexion (with a rubber band) Wearing spacer in between the toes Toes abduction from a seated position. But this is not all. The podiatrist even told her to wear an insole in her shoes. Furthermore, she was recommended to buy specific shoes that “protect her foot”. I saw the shoes myself, and I can tell you they didn’t look good. They were thick, big, and didn’t look comfortable to wear. Another podiatrist opinion A few months passed, and I went to see Andy, a podiatrist promoting barefoot wear for my own flat feet condition. As I was talking to Andy about my feet, I couldn’t resist getting an opinion in regard to what Steph was going through. Andy, without much hesitation, suggested that she wear barefoot shoes and continue the exercises. Next, we went down to Sole Mechanic, in Hampton, a shoe shop specialising in barefoot wear. Beforehand we researched different brands and decided to give a goal to the barefoot shoes, “Vivo Barefoot”. Sole Mechanic Experience The experience at Sole Mechanic was a positive one. We booked an appointment for 2 of us, 1 hour all up, so the staff has enough time to guide you through what barefoot is about and the best option. We went through the ankle and toes Range Of Motion and barometric platform test and tried a couple of shoes each. Vivobarefoot, given its ethical approach to shoe wear, was since the start our choice, and so far, the best option we could go for. At this stage, we have a couple of shoes each from Vivo barefoot, one for everyday wear and one for hiking. Back to the “Happy Bunion Story” So, after all this time, Steph now enjoys walking pain-free. The bunion, thanks to the exercises and to Steph’s determination in practising them daily and the new shoes that have a wider shoe box, is reduced, as the Big Toe is now diverging towards the medial side (away from the other toes). Osteoarthritis is a condition that can’t be fixed. Still, when Steph occasionally feels pain we do an MLD session which can help reduce the inflammation symptoms and help in pain management. Said so, the pain is a rare thing and not a daily issue. Furthermore, Steph is not wearing the insole anymore. As suggested by the Sole Mechanic staff, removing the insole is a process that can be done step by step. So, since Feb ’22 when we bought the first pair of Vivobearfoot shoes, took her approximately 2 to 3 months to abandon the insole, and now it is about three months that she is not using it anymore. Hopefully, this post gives you some hope and insights into what’s happening with bunions. If you are in pain and need to reduce the inflammation response to the bunion, MLD may be best for you as a short-term solution. Otherwise, book an appointment with Andy to find out the best way to adjust the shape of your foot as much as possible.