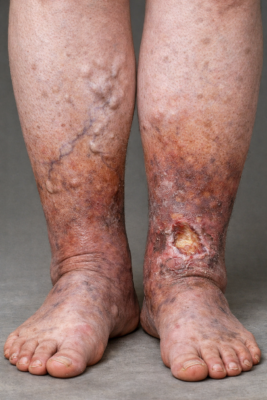
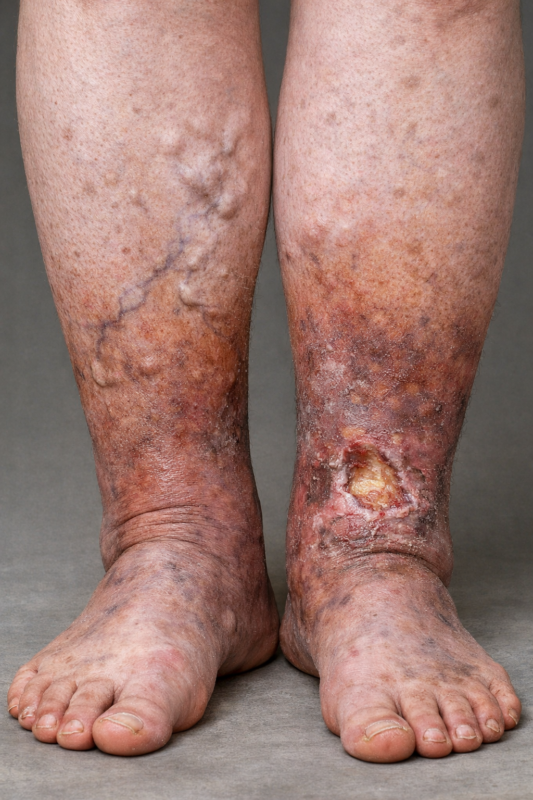
In Australia, Chronic Venous Insufficiency (CVI) affect more women than men, with a ratio of 25%–40% in women and 10%–20% in men (Al Shammeri et al., 2014). As a consequence of this condition, swollen legs are a common concern. CVI occurs when the veins in the legs struggle to return blood efficiently back to the heart, often leading to leg swelling, heaviness, aching, and visible varicose veins.
At Melbourne Massage and Treatment in Fitzroy North, since I specialised in Lymphoedema therapy, I regularly support clients experiencing leg swelling related to venous conditions too. Understanding how to manage the condition can significantly improve comfort, mobility and long-term leg health.
What Is Chronic Venous Insufficiency?
Chronic venous insufficiency is a condition defined as chronic when lasting for more than 3 months.
CVI develops when the valves inside the leg veins become weakened or damaged and stop acting as they should, which is why blood finds difficulty in flowing back to the heart. This results in swelling in the lower legs.
Common symptoms include:
- Persistent swelling in the lower legs or ankles
- Aching, heaviness or fatigue in the legs
- Skin changes such as dryness or discolouration
- Varicose veins
- Tightness or discomfort after prolonged sitting or standing
Without appropriate management, CVI can progress and increase the risk of skin complications or infection.
The Different Levels of Chronic Venous Insufficiency
Find below a table that describes how Clinical, Etiological, Anatomical, and Pathophysiological (CEAP) classify chronic venous insufficiency.
| Stage | Description |
|---|---|
| C0 | No visible/palpable signs of venous disease |
| C1 | Telangiectasias or reticular veins |
| C2 | Varicose veins |
| C3 | Oedema |
| C4 | Skin changes secondary to chronic venous disease (haemosiderin, lipodermatosclerosis, atrophie blanche) |
| C5 | Healed ulcer |
| C6 | Recurrent active venous ulcer |
The more advanced the stage, the more likely the hospitalisation of the patient for infections. This is not only a cost to the public health system, but to the Australia popolation too.
Compression Therapy: A Key Part of Managing Swollen Legs
The most effective way to manage swelling related to Chronic Vein Insufficiency is compression therapy.
Compression garments are helpful as they apply controlled pressure to the legs, which supports the veins and encourages blood and fluid to move back toward the heart. Unfortunately, there is no quick fix for swollen limbs, and for many people with chronic swelling, compression becomes an essential part of daily management.
But, you have to be aware that compression should always be prescribed and fitted appropriately. Indeed, the compression has to have the right gradient pressure, so stronger pressure at the bottom and weaker at the top; otherwise, we risk getting the liquid stuck in the leg and not moving.
On the other hand, with certain arterial conditions, compression may not be suitable; therefore, it is important that you talk to your GP about getting a referral to a vein specialist to know what’s the best approach for your swollen legs.
When Varicose Veins Are Present
If varicose veins are present, low-level compression is often recommended initially. This provides gentle support to the venous system while remaining comfortable for everyday use.
The goal is to:
- Support vein function
- Reduce fluid build-up
- Improve comfort during daily activities
- Help prevent worsening swelling
In fact, each individual may require a different compression level depending on their condition and tolerance, but also the integrity of the skin.
Compressions indeed are tight to put on, and for those with weak and fragile skin, it can be difficult to maintain skin integrity while wearing compression.
Why Flat-Knit Compression Garments Are Often Recommended
For clients with persistent swelling or changes in limb shape, flat-knit compression garments are frequently recommended.
Flat-knit garments offer several advantages:
- They provide stronger containment for swelling
- They can be custom-fitted for better comfort and effectiveness – class 3 and 4
- They help prevent fluid from accumulating in specific areas
- They are often more suitable for long-term management
Because every leg shape and swelling pattern is different, proper measurement and fitting are essential. At Melbourne Massage and Treatment, Lymphoedema clinic in Fitzroy North, I provide assessments and measurements for your swollen legs, so that I can provide garments that fit you for your specific presentation.
Accessing Compression Garments Through the SWEP Program (Victoria)
If you live in Victoria, you may be eligible to access compression garments through the SWEP program (State Wide Equipment Program).
SWEP helps eligible residents obtain essential medical equipment, including compression garments used in the management of venous conditions and lymphatic swelling.
As a SWEP-registered therapist, I can guide clients through the process, including:
- Clinical assessment
- Measurement for appropriate compression garments
- Assistance with the SWEP application process
- Ongoing monitoring and adjustments
The SWEP is free to access and does provide funding for 4 garments a year, specifically:
- $150 per garment if off the shelf
- $300 per garment if made on measurements
For Chronic Vein Insufficiency, most often the off-the-shelf garments are the ones to go for. But still, you have to know what class would best work for you, and what size would best work for you.
Movement: An Often Overlooked Therapy
Movement, as per my favourite medicine, is another important component in managing swollen legs.
In fact, blood flow, but even lymph flow, happens better when muscles contract and work.
For the legs, the calf muscles act as a natural pump, helping push blood and fluid upward when we walk or move. When we remain seated or standing for long periods, this pump becomes less effective.
Simple strategies include:
- Regular walking
- Gentle ankle movements during long periods of sitting
- Light leg exercises
- Avoiding prolonged immobility when possible
Even small amounts of regular movement can make a noticeable difference in managing swelling.
Protecting the Skin: A Crucial Step in Preventing Infection
People with chronic leg swelling are more vulnerable to skin breakdown and infection, and this is due to a series of reasons, such as:
- Increased venous pressure damages small blood vessels
- Reduced oxygen and nutrient delivery to the skin
- Chronic swelling stretches and weakens the skin
- Inflammation causes skin changes
Keeping the skin healthy is essential, and to do so, you should:
- Moisturising daily to prevent dryness and cracking
- Maintaining clean and intact skin
- Monitoring for redness, warmth or sudden swelling changes
- Seeking professional advice if signs of infection appear
Healthy skin acts as a barrier against bacteria and reduces the risk of complications. Pathogens in the air, bacteria that live on your skin would go crazy in proliferation if they get in touch with the warm and moist, rich protein that sits beneath the skin.
Professional Support in Fitzroy North
Managing chronic venous insufficiency and swollen legs often requires a combination of strategies, including compression therapy, movement, and proper skin care.
At Melbourne Massage and Treatment in Fitzroy North, I provide professional assessment and support tailored to your individual condition.
As a Lymphoedema Therapist and SWEP-registered provider, I can assist with:
- Assessment of leg swelling
- Compression garment fitting and recommendations
- Guidance on the SWEP funding process
- Ongoing support to help manage symptoms effectively
I will not grow tired of repeating to my patients and their GPs that early management can significantly reduce discomfort and prevent complications.
This is not only to reduce the cost management of this presentation, but to avoid patient suffering of skin infections, having to deal with hospitalisation, and other potential severe presentations that an unmanaged CVI can lead to.
And to support you along this journey, to start with, I can offer a FREE 15-minute online consultation, where we can chat about your clinical history and see if there is a need for a referral to a specialist, before applying for the SWEP program.
Book Now A Free 15 Minutes Online Consultation

Giovanni La Rocca
Giovanni moved to Melbourne, Australia, from Italy in 2008 and became a citizen in 2017. He started studying massage therapy in 2016, then completed a Bachelor of Health Science in Clinical Myotherapy in August 2024. During those years, he also specialised in Thai Massage and Manual Lymphatic Drainage for presentations like Lipoedema and Lymphoedema. Nowadays, he runs his clinic in Fitzroy North, Melbourne, where he integrates movement therapy into his practice to enhance overall well-being. He also values meditation, having completed several Vipassana courses. Committed to continuous learning, he aims to share his expertise in integrated therapies to help others achieve balance and resilience.