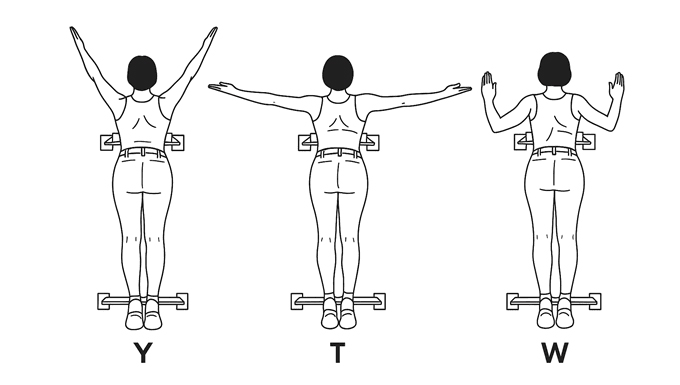
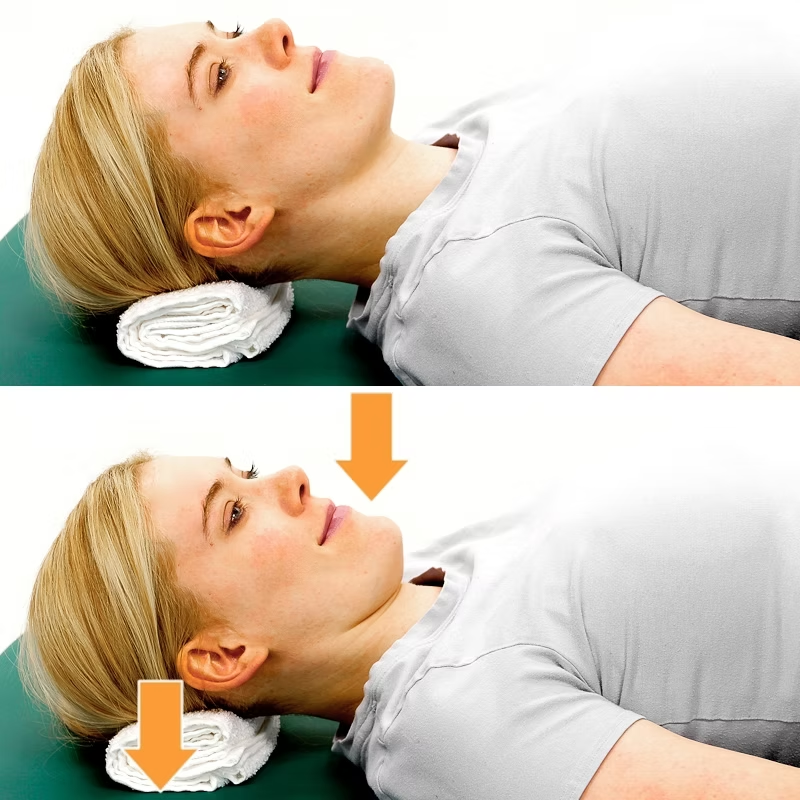
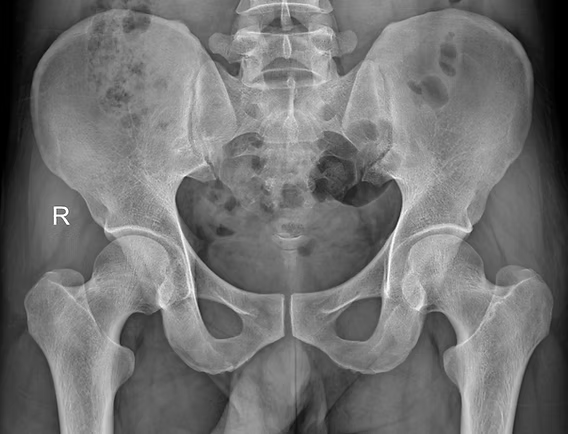
When the space between the collarbone and first rib gets tight, during movement or even at complete rest, it can lead to Thoracic Outlet Syndrome (TOS). Between the two structures mentioned above, we have the passage of the thoracic plexus (nerves) and blood vessels. The compression of those structure, can result in pain, weakness and numbness radiating down the shoulder, arm, and hand. Because TOS has multiple causes and presentations, effective treatment depends heavily on accurate assessment and an individualised approach, and that’s where myotherapy can play a crucial role. What Causes Thoracic Outlet Syndrome? As there are different tissues passing by this space, the nature of TOS can be broadly categorised into three types: Neurogenic TOS: Compression of the brachial plexus (nerves). Venous TOS: Compression of the subclavian vein. Arterial TOS: Compression of the subclavian artery. But not only can different tissues be compressed, but different structures can be responsible for the compression. Indeed, the compression can be due to the scalene muscle, pectoralis minor or bone. And here are some common causes: Muscle imbalances that lead to poor posture (forward head/rounded shoulders); Repetitive overhead activities (which lead to constant compression of the tissues); Trauma (e.g. whiplash or clavicle fracture); Anatomical variations (such as a cervical rib). The Role of Myotherapy in TOS Assessment As a myotherapist, when treating someone with suspicious TOS, we go for a series of assessments that we compare to the clinical history and symptoms. The test itself would aim to reproduce the patient’s symptoms and guide us on what potential structure is compressed. If we are suspicious of TOS, we can aim to reduce tension in soft tissue and give exercises that can reinforce those structures to alleviate any compression in the area. Orthopedic Testing & Myotome Assessment Some common assessments include: Adson’s Test (for scalene involvement) – It consists of reproducing a drop of heart bit in the wrist (affected side) by asking the patient to abduct and extend the arm while rotating (same side) and extending the neck. This would add extra compression on the suspected structures. Roos/Elevated Arm Stress Test (to reproduce vascular or neural symptoms) – It is about asking the patient to lift the arm at 90°/90° and start closing and opening their hands repetitively for 30 seconds to 1 minute. A drop of strength or symptom reproduction would lead to a positive test. Costoclavicular Maneuver (to assess space between clavicle and first rib) – It is delivered by having the patient with depressed and retracted shoulders. The positivity of this test is given by the reproduction of symptoms or a reduction in the distal wrist. Wright’s Hyperabduction Test (for pectoralis minor tightness) – The patients get asked to lift their arm (affected side) above their head while the therapist stands behind and keeps count of the wrist heartbeat. Any symptoms, reproduction, or drop in bit is considered positive. In addition to those tests, we would use: Myotome testing: which assesses the motor function of specific spinal nerve roots; Clinical history: Any history of previous injury, surgeries, work and sport loads; Type and timing of symptoms: When and how those symptoms are reproduced on daily life. All this said, we always have to consider that as therapists, myo or physio as per osteo exc… we can assume that the positivity of many of those test leads to a positive or negative conclusion regarding TOS. Hands-on treatment and exercises in combination can be the easy steps to take to treat the presentation, but can not always guarantee the best outcome, due to each individual’s unique presentation. Hands-On Treatment and Exercise Prescription Once we have more understanding of what is potentially happening in terms of compression, a myotherapy treatment focuses on addressing the underlying causes: Manual Therapy Myofascial release of the scalene, pectoralis minor, and upper trapezius muscles. Trigger point therapy to reduce local and referred pain patterns. Joint mobilisation to improve scapular movement and rib mechanics. Neural gliding techniques to encourage nerve mobility and reduce irritation. Exercise Rehabilitation Postural re-education, particularly strengthening the deep neck flexors and lower trapezius. Scapular stabilisation exercises to improve shoulder mechanics. Breathing retraining is necessary if dysfunctional patterns (like apical breathing) are contributing to compression. Neurodynamic stretches are appropriate for nerve mobility. Together, these interventions help reduce symptoms, improve function, and support long-term recovery. The time frame for improvement, if not complete reduction of the symptoms, can be different per individual, but we can estimate a period of time that goes between 12 and 16 weeks. If no changes are reproduced within this time frame, that’s where we would refer the patient elsewhere for further investigations, like a scan. When Is Surgery Needed for Thoracic Outlet Syndrome? Surgical intervention is typically reserved for cases where conservative care fails or in cases of vascular TOS, where there’s a risk of thrombosis or embolism, but also where anatomical variations, like a cervical rib is present. Surgical procedures may include: Scalenectomy (removal of the scalene muscles) First rib resection Clavicle decompression or repair if there’s previous trauma These operations aim to create more space in the thoracic outlet, thus relieving the compression. Post-Surgical Recovery and the Role of Myotherapy In case of surgery, as a myotherapist, we can still help and ensure a correct recovery post-intervention. Treatment like MLD can help in flushing excess liquid out of the surgery area, but again, we would look into exercises as a form of recovery and rehabilitation of the area affected by the surgery and or affected by the lack of strength that is a consequence of a prolonged period of muscle weakness. More broadly, myotherapy treatment can help with: Pain management Scar tissue Muscle guarding or weakness Neurological symptoms that may persist or reappear Do You Need a Scan if we’re suspicious of TOS? Imaging, as discussed in other blogs, may be recommended when we are suspicious of other presentations, or if standard method are not creating any difference. For example: To rule out cervical disc herniation, tumours, or other causes of neurovascular symptoms. When […]
Tag Archives: MLD
Cosmetic surgeries have become increasingly common, with procedures such as liposuction, tummy tucks, facelifts, and breast augmentations helping people achieve their desired aesthetic goals. However, while the surgical aspect gets most of the attention, what often goes under-discussed is the importance of post-operative care, especially Manual Lymphatic Drainage (MLD) in promoting faster, smoother recovery and reducing the risk of ending with fibrosis tissue build up underneath the skin. What Is Manual Lymphatic Drainage (MLD)? MLD is a gentle, rhythmic massage technique designed to stimulate the lymphatic system and encourage the natural drainage of lymph fluid. The lymphatic system plays a crucial role in immune function and fluid balance. After cosmetic surgery, lymphatic flow can become disrupted due to inflammation, surgical trauma, or temporary damage to lymph vessels. While the first few days post-surgery are dedicated to acute recovery and the taking of Antibiotic to reduce the risk of infection post-surgery, as soon as this risk is passed, that’s when you want to start your MLD journey. Why Is MLD Important After Cosmetic Procedures? Cosmetic surgeries often cause swelling, bruising, and fluid accumulation (known as seroma or edema). This is due to the body reacting to an invasive procedure and removing tissue beneath the skin. MLD helps: ✅ Reduce post-surgical swelling ✅ Accelerate the removal of metabolic waste and excess fluid ✅ Improve skin texture and reduce fibrosis (hardened tissue) ✅ Speed up visible results by enhancing contour definition ✅ Decrease discomfort by reducing pressure from trapped fluids As with any surgery, when lymphatic drainage massage is applied, no pain is to be experienced. While I treat someone with MLD I always pass this information up front, to ensure that if they experience any type of pain, I get told about it, so that I can go lighter with pressure. Which Procedures Benefit Most from Lymphatic Drainage? MLD is commonly recommended after: Liposuction (including 360 lipo or Brazilian Butt Lift – BBL) Tummy tucks (abdominoplasty) Facial surgeries (rhinoplasty, facelifts, blepharoplasty) Breast augmentation or reduction Body contouring procedures As a Lymphoedema therapist, I do get surgeons referring me patients to assist them with post-op management, especially when swelling or fibrosis is a concern. When Should You Start Lymphatic Drainage? As briefly explained above, the ideal time to begin MLD is as soon as you stop your antibiotic cycle, and is your surgeon or GP call to when you are safe to do so. On the other hand: Typically, MLD is started 3 to 5 days post-surgery, once acute inflammation has settled and the incision sites are closed or protected. A full course may include 6–10 sessions spaced out over a few weeks for optimal results. Always follow the advise of the surgeon about post surgery, but, when you safe to do, the more movement we add to Lymphatic Draiange, the better the recovery would go. Is MLD Safe post-cosmetic surgery? When performed by a qualified lymphatic therapist, lymphatic drainage is non-invasive, safe, and effective. It’s gentle enough for delicate post-op tissue and can significantly improve comfort and healing time. My qualification in Lymphatic Drainage was done with the Vodder Academy whicg holds the gold standards for MLD practice, and is worldwide well known for the quality of their practice. On the other hand, I also hold a qualification in Clinical Myotherapy, which allows me to help people recover from injury and stick to their fitness goals via training and exercises. When Can I Book My Appointment for Post-Cosmetic Surgery Recovery? My studio, Melbourne Massage and Treatment, is located in Fitzroy North, on the corner of St George Rd and Holden St. I work Monday to Saturday, and to book an appointment, you can just head online to the booking page and choose the best time/days that work for you. Given the number of session needed for this type of work, I always suggest to book a series of session in a raw, from to 3 session per week for the first 2 weeks. Session by session we do evaluate together the progress, and chose together what’s the next step. If you have any questions, please do not hesitate to contact me. FAQs – Cosmetic Surgery & Lymphatic Drainage
Manual Lymphatic Drainage (MLD) is an ideal treatment to reduce swelling and oedema, and if so, at Melbourne Massage and Treatment, I offer manual lymphatic drainage during pregnancy. Swelling, heaviness in the legs, water retention, and aching joints are all common during a pregnancy. One treatment that is safe, gentle, and highly effective in reducing these symptoms is Manual Lymphatic Drainage (MLD). In this blog, we’ll explore the benefits, safety considerations, positioning, and when lymphatic drainage may or may not be recommended. What Is Manual Lymphatic Drainage for Pregnancy? Lymphatic drainage is a gentle, rhythmic technique designed to stimulate the lymphatic system. This improves the movement of lymph fluid, helping the body eliminate unwanted substances, reduce fluid retention, and improve overall well-being. Manual lymphatic drainage is beneficial for pregnant individuals (Cataldo Oportus et al., 2013), particularly for managing swelling, improving circulation, and supporting relaxation. Benefits of Lymphatic Drainage During Pregnancy In a city like Melbourne, where the weather can get really hot, those temperatures can be an extra challenge during pregnancy. Here is a list of MLD benefits for your gestation time: 1. Reduction of Swelling (Oedema) Swelling in the legs, ankles, and feet is extremely common in pregnancy due to increased pressure on the lymphatic and circulatory systems. Lymphatic drainage helps move fluid away from congested areas, relieving discomfort and heaviness. 2. Relief from Pregnancy-Related Back Pain During pregnancy, the increasing weight can affect posture and strain the back. Lymphatic drainage, performed in a comfortable side-lying position, helps reduce tension through its profound relaxation effect. 3. Improved Circulation Changes in blood volume and circulation during pregnancy can cause fluid retention and fatigue. Lymphatic drainage promotes healthy blood and lymph flow, improving oxygen and nutrient delivery to both mother and baby. 4. Mental and Emotional Well-being One of the most underestimated benefits of lymphatic drainage is how deeply relaxing it is. Better sleep, reduced stress, and a sense of lightness are very common outcomes. At Melbourne Massage and Treatment in Fitzroy North,you would receive pregnancy lymphatic drainage massage in a seated or semi-reclined position on a hydraulic table, which allows maximum comfort and safety throughout the treatment. FAQ – Pregnancy Lymphatic Drainage Massage in Melbourne Reference Cataldo Oportus, S., de Paiva Rodrigues, L., Pereira de Godoy, J. M., & Guerreiro Godoy, M. de F. (2013). Lymph Drainage in Pregnant Women. Nursing Research and Practice, 2013, 1–3.
Muscle tension headache and migraine are two different types of presentation that have in common a pain, which can also be debilitating, in the head area. Back in 2019, in Australia, 3 million people were estimated to suffer from migraine (Wijeratne et al., 2023), where, define how many people are suffering from muscular tension head-ache is a bit more tricky, as is not a presentation that can be easily tracked, due to self managed protocols, and other miss data counting. That said, they have different origins, symptoms, and treatment options. In this blog post, we will explore the key differences between muscle tension headaches and migraines, helping you understand how to identify and manage them. What Are Muscle Tension Headaches? Muscle tension headaches, or tension-type headaches, are the most common. This type of headache originates from cervical or facial muscle tensions, which recreates a pattern of pain on the head of facial area. As with all muscles, but even joints, the pain that we can experience can be local or in an area around the tense spot. These headaches are often linked to stress, lack of good posture, anxiety, and even sleep disturbances. They can be chronic or occasional, but compared to migraine, they lack neurological symptoms. Symptoms of Muscle Tension Headaches: Dull, aching pain or pressure around the head, especially in the forehead, temples, and back of the head. A sensation of tightness or “band-like” pressure around the head. Mild to moderate intensity (usually not as severe as a migraine). Pain can last from 30 minutes to several hours, sometimes even days. Tenderness or tightness in the neck, shoulders, and scalp. Causes of Muscle Tension Headaches: Stress: Emotional and mental stress is one of the primary causes of muscle tension in the neck and scalp muscles. Lack of good posture: Sitting or standing with poor posture and lack of strength in the musculoskeletal system, especially for long work, can strain muscles and trigger headaches. Sleep issues: Sleep deprivation or poor-quality sleep can exacerbate muscle tension and lead to headaches. The body recovers from the fatigue of the day before during sleep, especially in the early morning hours. Sleep deprivation would increase the chance of a headache. Dehydration: Not drinking enough water can lead to tension and headache symptoms. The body withdraws water from the brain to keep the organ functioning, causing physical brain shrinkage, which leads to headaches. Recent studies have indicated that chronic tension-type headaches (CTTH) are often exacerbated by environmental stressors, and poor posture in daily activities can cause muscle imbalance and contribute to the frequency of these headaches (Bendtsen et al., 2018; Grazzi et al., 2016). Treatment Options: Pain relief: Over-the-counter pain relievers, like ibuprofen or acetaminophen, can help ease the discomfort. Heat pack: Applying a warm compress to the neck and shoulders can help relax tense muscles. Keep always in mind that heat application should be limited to 10-15 minutes, once or twice a day. Massage: Gentle massage of the neck and shoulder muscles can reduce tightness and alleviate headache symptoms. Stress management: Practising relaxation techniques such as deep breathing, thai yoga, and meditation can reduce stress and prevent muscle tension headaches. Strengthen muscles: Strengthening the muscles around your cervical and shoulder area can help reduce the chance of suffering a headache by reducing the inflammatory response that the muscle would activate due to a lack of strength. What Are Migraines? As I mentioned above, the significant difference between headaches and migraines is due to neurological symptoms, a unique characteristic of migraines. Migraines are neurological events that involve complex brain activity. They are characterised by intense, throbbing pain, usually on one side of the head. They are often accompanied by other symptoms such as nausea, vomiting, and sensitivity to light and sound. Migraines are more debilitating than muscle tension headaches and can last a few hours to several days. The intensity of the headache doesn’t have to be severe. Symptoms of Migraines: Although many people experience nausea, vomiting, and light sensitivity, migraine symptoms can vary, with some individuals experiencing dizziness or visual disturbances without significant head pain. Throbbing or pulsing pain, usually on one side of the head. Nausea and vomiting. Sensitivity to light, sound, and sometimes smells (aura). Visual disturbances such as flashing lights or blind spots (this is known as an aura, which can occur before or during the headache). Dizziness or feeling lightheaded. Migraines are understood to be primarily driven by neurovascular changes and neuronal hyperexcitability (Feng et al., 2021). A review by Wagner et al. (2021) found that the pathophysiology of migraines involves alterations in neurotransmitter systems, notably serotonin and CGRP (calcitonin gene-related peptide), which contribute to the vasodilation and pain signaling pathways. Causes of Migraines: Genetics: Migraines tend to run in families, suggesting a genetic component. Hormonal changes: For many women, changes in estrogen levels, such as during menstruation, pregnancy, or menopause, can trigger migraines. Environmental triggers: Bright lights, strong smells, certain foods (like chocolate, cheese, or caffeine), weather changes, lack of sleep, and allergies that cause sinus issues are common migraine triggers. Neurological factors: Migraines may involve changes in the brain’s nerve pathways, chemicals, and blood vessels, which cause inflammation and pain. Treatment Options for Migraines: Prescription medications: Triptans and anti-nausea medications are commonly prescribed to treat the acute pain of migraines. Preventive medications: For frequent migraine sufferers, medications such as beta-blockers, antidepressants, or anti-seizure drugs may be prescribed to reduce the frequency and severity of attacks. Lifestyle changes: Regular sleep, a healthy diet, and consistent exercise can help reduce the frequency of migraines. Cognitive-behavioural therapy (CBT): Managing stress through therapy can help alleviate migraine triggers. Alternative therapies: Acupuncture, biofeedback, and massage therapy are sometimes used as complementary treatments for migraine management. Recent studies support preventive treatments for chronic migraines, such as CGRP antagonists (Kundera et al., 2020) and neuromodulation techniques like transcranial magnetic stimulation (Lefaucheur et al., 2017). Key Differences Between Muscle Tension Headaches and Migraines Although muscle tension headaches and migraines involve head pain, they differ […]
Menopause is a natural phase in every woman’s life, but it comes with a variety of physical, emotional, and mental challenges. As hormone levels shift, particularly estrogen, progesterone, and testosterone, many women experience symptoms like hot flashes, mood swings, sleep disturbances, and weight gain. Fortunately, for managing menopause symptoms, various lifestyle changes can be put in place, such as exercise, a balanced diet, improved sleep hygiene, and stress management techniques. In this blog, we will explore how adopting a healthier lifestyle can significantly improve your menopausal experience. Exercise and Physical Activity For Managing Menopause Symptoms Exercise is again the best recommendation for health improvement that can be offered here. Of course, implementing exercises alone without following any other changes or advice (where needed) is not going to do the trick. But let’s start from here. Exercises can improve overall health and have specific benefits that help ease common issues like weight gain, mood swings, and hot flashes. But not only that. Indeed, exercises, and in particular strength training, are positive stress, which allows the body to regenerate and ensure the slowing down of bone and muscle mass, which is one of the main issues that a woman going through menopause is going to face. Here is a list of exercise routines that you could focus on. But keep in mind that if you really want to choose, I would strongly suggest Strength Training. Aerobic Exercise:Walking, swimming, cycling, or jogging would help in improving circulation, promote heart health, and relieve stress (for the last one, especially if done in open-air environment). Regular aerobic exercise has also been shown to reduce the frequency and intensity of hot flashes. Plus, it aids in weight management, especially during menopause when metabolism slows. Strength Training:Engaging in strength training exercises, such as weightlifting or resistance band workouts, helps preserve muscle mass and improve bone density, which decreases as estrogen levels decline. This is essential for reducing the risk of osteoporosis and maintaining strong bone and muscle mass. Yoga or Pilates:Both yoga and Pilates are great for improving flexibility, balance, and muscle strength while reducing stress and anxiety. These low-impact exercises help maintain your physical health and mental well-being, both of which can be affected by hormonal fluctuations during menopause. Tai Chi or Qigong:These ancient practices involve slow, deliberate movements and deep breathing. They are excellent for enhancing balance, reducing stress, and promoting relaxation—especially helpful for managing mood swings and anxiety. Eating an Anti-Inflammatory Diet A nutrient-rich diet can significantly help in managing menopause symptoms. By incorporating specific foods and avoiding certain triggers, you can reduce inflammation, balance hormones, and support your body’s needs during this transition. Phytoestrogens:Phytoestrogens are plant-based compounds that mimic estrogen in the body and can help alleviate symptoms like hot flashes and night sweats. Foods rich in phytoestrogens include soy products (tofu, tempeh, edamame), flaxseeds, lentils, chickpeas, and whole grains. Calcium and Vitamin D:As estrogen levels decline, the risk of bone loss and osteoporosis increases. To support bone health, incorporate calcium-rich foods such as leafy greens (kale, broccoli, sesame seeds), fortified plant-based milks, and dairy products. Vitamin D is crucial for calcium absorption, so get it from sun exposure or foods like fatty fish (salmon, mackerel) and fortified foods. Vitamin D is cumulative, so during the longer days of the year, ensure to spend some extra time in the sun. But of course, do so during the safest hours and not at UV light pick time. Regarding Vitamin D and Calcium supplements, there is a strong debate about whether they are good or what potential side effects they have, so you’d better talk to your GP about the specifications. Healthy Fats:Omega-3 fatty acids found in fatty fish, flaxseeds, chia seeds, and walnuts have anti-inflammatory properties that can help reduce joint pain and inflammation during menopause. These healthy fats also support heart health, which is increasingly important as estrogen levels drop. Whole Grains and Fibre:Fibre helps stabilise blood sugar levels and improves digestion, which can be helpful as metabolism slows. Incorporate fiber-rich foods like whole grains (brown rice, oats, rye), fruits, vegetables, and legumes to support digestive health and reduce bloating. In the case of beans and grain, ensure that they are soaked when needed to reduce the bloat side effect. Limit Sugary and Processed Foods:Foods high in sugar and processed carbs can cause blood sugar spikes and crashes, leading to irritability and fatigue. This is where having a variety of fresh food is a key component. So yes, no one wants you to overstress about what you eat or not, but, generally speaking, if you have never looked into a balanced anti-inflammatory diet, it is time to do so. Reducing Alcohol and Inflammatory Foods Both alcohol and inflammatory foods can exacerbate menopause symptoms, so limiting or avoiding them can provide significant relief. Limit Alcohol:While alcohol might seem like a way to unwind, it can actually trigger hot flashes, disrupt sleep, and contribute to mood swings. Moderation is key—try limiting your alcohol intake to no more than one drink per day, and if possible, reduce it further to see if it improves your symptoms. Alcohol is a substance that the body does not recognise, and it has quite a hard time breaking it down. Avoid Inflammatory Foods:Highly processed foods, refined sugars, and trans fats can increase inflammation in the body and worsen menopause symptoms like joint pain, fatigue, and mood swings. Instead, focus on anti-inflammatory foods such as berries, leafy greens, fatty fish, and nuts to support your body during this phase. Inflammatory foods are all those that contain Omega-6 fatty acids, which are long-chain fatty acids, that would get collected in your Lymphatic System at first, and attacked by the macrophages (white cells), inciting an inflammatory response. Caffeine:Excessive caffeine can disrupt sleep and worsen hot flashes. If you find that caffeine aggravates your symptoms, consider reducing your intake or cutting back on coffee and other caffeinated beverages, especially in the afternoon or evening. Here is a great podcast from ZOE podcast about […]
Musculoskeletal pain can be complex, and orthopedic tests and hands-on treatment, sometimes, can be a limited tool to individualise what is happening with the body’s internal structure. Indeed, there are times when a deeper look is required to ensure we are on the right path. This is where body scans imaging comes into play to identify presentations like tendinopathy, bursitis, ligament tear or other underlying conditions. The Role of Body’s Scan in Diagnosing Pathology Body scans include a series of imaging technologies, such as ultrasound, x-ray, MRI, to name a few. Ultrasound is a highly effective imaging tool used to assess soft tissue structures in real-time. Unlike X-rays, which primarily show bone, ultrasound provides detailed images of muscles, tendons, bursae, and ligaments. This makes it an excellent tool for diagnosing conditions such as: Tendinopathy – A chronic condition involving tendon degeneration due to overuse or injury. Bursitis – Inflammation of the bursae, the small fluid-filled sacs that reduce friction between tissues. Those tissue types are found along different body joints, like the shoulder and the hip. Ligament Tears – Partial or complete tears of ligaments, often occurring after trauma or excessive stress. Baker’s cyst – is a fluid-filled swelling that forms behind the knee, often resulting from knee joint conditions like arthritis or meniscal tears, causing discomfort and limited mobility. When we are suspicious of one of those presentations, due to positive results obtained by orthopedic test and medical history, including mechanism of injury, we attempt a recovery process, based on the type of injury, symptoms, and other relevant information. Along this recovery process, we may start with isometric exercises. If, with the first 6 weeks, and a series of sessions, 3 to 4 sessions with this time frame, we still don’t see a major recovery, then we may want to get extra investigation ongoing via an ultrasound scan, which can clarify the underlying pathology. It allows us to confirm or rule out certain conditions, ensuring that treatment strategies are aligned with the actual tissue damage (if any is present). On the other hand, based always on the individual case, we could also require X-rays, which are often more helpful in diagnosing conditions related to the bones, such as arthritis or fractures, as they provide a clear view of bone structure and joint spaces. MRI is a scan that is used for Brain imaging, and when the investigation needs higher details, like when looking at the spine or a joint that via ultrasound was not giving any sign of issue. Ultrasound is also comparable to MRI, as it is faster, easier to deliver, and has fewer complications. How can myotherapy treatment help recovery from what a body scans would show? As we already discussed in another blog, Myotherapy is a practice that looks into the well-being of the skeletal muscle structure. To understand what can be done about a painful presentation, we would initially take a detailed clinical history, then look into objective measurements, such as your movement and body presentation. Given the result we can obtain, we would build up a treatment plan which includes: Hands-on Treatment – Techniques such as deep tissue massage, myofascial release, and dry needling can help reduce pain and improve mobility. Exercise Prescription – Strengthening and mobility exercises help restore function and prevent future injuries. Load Management Strategies – Proper guidance on activity levels ensures tissues heal without excessive strain. That management technique would then be combined and adjusted around the scan’s results. Here are a few examples: Bursitis: If a bursitis is confirmed, medications may be given to reduce the inflammation of the bursa, for that, we concentrate on MLD treatment to further reduce the inflammation and exercises to build strength on the structure that needs support. Ligament tear: When talking of ligament tear, the healing time can dilagate to months if not also a year, so we know now why the 6 weeks program may was not as responsive. We will keep focusing on the strength of the muscle that surrounds the specific joint, and use hands-on treatment to boost blood to the area affected. Arthritis: Medication or dietary change may be put in consideration for pain management and inflammatory reduction. Also in this case, MLD can be used to manage the pain response, and exercises for mantain movement in the affected joint/s. When Should You Consider an Ultrasound or other body scans? If you experience ongoing pain, swelling, or restricted movement that is not improving with therapy, an ultrasound or other scan helps identify the cause. This can prevent prolonged discomfort and allow for a more targeted treatment approach. At Melbourne Massage and Treatment, in Fitzroy North, we aim to provide the most effective care possible. If you’re dealing with persistent musculoskeletal pain, book a consultation with Giovanni today. Together, we’ll determine the best action to get you back to optimal function. Frequently Asked Questions (FAQs) About Musculoskeletal Pain and Body Scans Imaging 1. What are body scans, and how do they help diagnose musculoskeletal pain?Body scans include imaging technologies such as ultrasound, X-ray, and MRI. These scans help diagnose soft tissue injuries (like tendinopathy, bursitis, and ligament tears) or bone-related conditions (such as fractures or arthritis). They provide a clearer picture of what might be causing pain, inflammation, or restricted movement. 2. Why is ultrasound commonly used in diagnosing soft tissue injuries?Ultrasound is highly effective for real-time imaging of soft tissues like muscles, tendons, bursae, and ligaments. It helps diagnose conditions such as tendinopathy, bursitis, and ligament tears, providing a dynamic view of the area being studied without the need for invasive procedures. 3. When should I consider getting an ultrasound or other scans for my injury?If you’re experiencing persistent pain, swelling, or limited mobility that isn’t improving with initial therapy (such as exercises or hands-on treatment), it might be time to consider an ultrasound or other scans. These can help identify the underlying cause of your symptoms and allow for a more targeted treatment approach. 4. How do orthopedic […]
Lymphoedema and Lipoedema are chronic conditions characterised by swelling and fat accumulation, respectively, often accompanied by inflammation. Thanks to emerging research, we do not know that dietary choices, particularly the consumption of long-chain fatty acids, can influence the inflammatory processes associated with these conditions. This is why it is important to consider an Anti-Inflammatory Diet when suffering from those presentations. The Role of Long-Chain Fatty Acids in Inflammation Long-chain fatty acids are absorbed into the lymphatic system in structures called chylomicrons. Once these chylomicrons are processed, the released fatty acids can interact with macrophages—immune cells responsible for detecting and responding to pathogens. This interaction can trigger an inflammatory response, contributing to the chronic inflammation observed in both lymphoedema and Lipoedema. Why does the Lymphatic System absorb Long-Chain Fatty Acids? The lymphatic system plays a crucial role in the absorption and transport of dietary fats, particularly long-chain fatty acids. This process is essential for efficient lipid metabolism and overall energy distribution in the body. Absorption of Long-Chain Fatty Acids Long-chain fatty acids are released from dietary fats in the small intestine during digestion. These fatty acids are absorbed by the enterocytes (intestinal cells), where they are reassembled into triglycerides and packaged into lipoprotein particles known as chylomicrons. Due to their size and composition, chylomicrons are too large to enter the blood capillaries directly. Instead, they are absorbed into specialized lymphatic vessels called lacteals, located within the villi of the small intestine. This lymphatic absorption allows the efficient transport of large lipid molecules into the systemic circulation. Transport Through the Lymphatic System Once inside the lacteals, chylomicrons travel through the lymphatic system, merging into larger lymphatic vessels and eventually entering the bloodstream via the thoracic duct, which empties into the left subclavian vein near the heart. This pathway enables the gradual release of lipids into the circulation, allowing tissues to access these essential nutrients for energy production, cell membrane synthesis, and other vital functions. Benefits of an Anti-Inflammatory Diet Adopting an anti-inflammatory diet can help mitigate these effects by reducing the intake of pro-inflammatory long-chain fatty acids and emphasising foods that support lymphatic health. Key components of such a diet include: High Fibre Intake: Consuming fruits and vegetables rich in fibre promotes the production of short-chain fatty acids in the gut, which have anti-inflammatory properties. Omega-3 Fatty Acids: Incorporating sources of omega-3s, such as fatty fish, flaxseeds, and walnuts, can reduce inflammation and edema. Anti-Inflammatory Spices: Spices like turmeric, garlic, and curry leaves possess natural anti-inflammatory effects and can be beneficial additions to the diet. Foods to Limit or Avoid for a Good Anti-Inflammatory Diet To further reduce inflammation, it’s advisable to limit the consumption of: Processed Foods: Often high in trans fats and refined sugars, these can exacerbate inflammatory responses. Excessive Salt and Caffeine: High intake of salt and caffeine may contribute to fluid retention and should be moderated. Alcohol and Sweets: These can increase inflammation and are best consumed in moderation. Personalised Nutritional Guidance As a certified lymphoedema therapist trained by the Vodder Academy, I understand the importance of a holistic approach to managing lymphoedema and Lipoedema. Integrating an anti-inflammatory diet tailored to your individual needs can play a crucial role in reducing inflammation and improving overall health. For personalised advice and support, consider consulting with a healthcare professional or a registered dietitian experienced in managing these conditions. By making informed dietary choices, you can actively contribute to managing inflammation and supporting your lymphatic health. For more insights on managing lymphoedema and Lipoedema through diet, you might find this video informative. Melbourne Massage and Treatment and Lymphoedema/Lipoedema presentation Even though I am not a dietitian or nutritionist, so I can not give any direct recommendations on your diet or food intake, as a Lymphoedema therapist, I can still help you manage your presentation by offering services like Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). So, if you need to improve your Lymphoedema or Lipoedema presentation, book your free 15-minute phone consultation now to understand how Melbourne Massage and Treatment services can benefit you. FAQ about Anti-Inflammatory Diet and Lymphoedema/Lipoedema presentation Q: How do dietary choices influence inflammation in lymphoedema and Lipoedema? A: Dietary choices play a significant role in modulating inflammation associated with lymphoedema and Lipoedema. Consuming foods high in long-chain fatty acids can lead to their absorption into the lymphatic system, where they may interact with macrophages—immune cells responsible for detecting and responding to pathogens. This interaction can trigger an inflammatory response, contributing to the chronic inflammation observed in both conditions. Adopting an anti-inflammatory diet can help mitigate these effects by reducing the intake of pro-inflammatory foods and emphasizing those that support lymphatic health. Q: What are long-chain fatty acids, and how do they affect inflammation? A: Long-chain fatty acids are a type of fat molecule commonly found in various foods, including certain oils, meats, and processed products. When consumed, these fatty acids are absorbed into the lymphatic system in structures called chylomicrons. Once processed, the released fatty acids can interact with macrophages, triggering an inflammatory response. This process can exacerbate the chronic inflammation associated with lymphoedema and Lipoedema. Q: Which foods are high in long-chain fatty acids and should be limited? A: Foods rich in long-chain fatty acids that may promote inflammation include: Certain oils Meats Processed products Limiting the intake of these foods can help reduce inflammation. Q: What are the key components of an anti-inflammatory diet that are beneficial for lymphoedema and Lipoedema? A: An anti-inflammatory diet focuses on incorporating foods that help reduce inflammation and support lymphatic health. Key components include: High Fibre Intake: Consuming fruits and vegetables rich in fibre promotes the production of short-chain fatty acids in the gut, which have anti-inflammatory properties. Omega-3 Fatty Acids: Incorporating sources of omega-3s, such as fatty fish, flaxseeds, and walnuts, can reduce inflammation and edema. Anti-Inflammatory Spices: Spices like turmeric, garlic, and curry leaves possess natural anti-inflammatory effects and can be beneficial additions to the diet. Q: Are there specific foods I should […]
If you or someone you know is struggling with the lingering symptoms of Long Covid, you are not alone. After the initial acute phase of COVID-19, many people continue to experience debilitating symptoms such as fatigue, breathlessness, and brain fog that can last for weeks or even months. These prolonged effects, commonly referred to as Long Covid, have created a pressing need for effective treatment strategies to manage and alleviate the symptoms. One promising approach gaining attention is Manual Lymphatic Drainage (MLD) Massage, a gentle and non-invasive therapy that can support the recovery process for Long Covid patients. At Melbourne Massage and Treatment, Giovanni, a highly trained therapist from the Vodder Academy, is helping clients recover from the lingering effects of COVID-19 using this technique. But how exactly does MLD work, and can it help you overcome the frustrating symptoms of Long Covid? What is Manual Lymphatic Drainage Massage (MLD)? MLD is a specialised massage technique that uses gentle, rhythmic movements to stimulate the lymphatic system—the body’s waste removal and immune system. The lymphatic system is responsible for draining toxins, bacteria, and waste from the body’s tissues. It plays an essential role in inflammation control, immunity, and tissue recovery. MLD can help to enhance the flow of lymph, reduce chronic inflammation, alleviate congestion, and promote overall healing. Trained at the renowned Vodder Academy, Giovanni uses the Dr Vodder method of MLD, a highly effective and evidence-based technique. This form of lymphatic drainage focuses on increasing lymph flow and addressing issues such as fluid retention, swelling, and inflammation, which are common in patients suffering from post-viral syndromes, including Long Covid. Long Covid Symptoms: A Multifaceted Condition Long Covid is a condition where individuals experience lingering symptoms after the acute infection phase has passed. Some of the most common symptoms include: Fatigue: Extreme tiredness that doesn’t improve with rest Breathlessness: Difficulty breathing or catching your breath even after mild exertion Cognitive Dysfunction: Often referred to as “brain fog”, which includes issues with concentration, memory, and clarity of thought Muscle and Joint Pain: Persistent aches and pains that can make everyday tasks difficult Sleep Disturbances: Trouble falling or staying asleep due to physical discomfort or anxiety While medical management of Long Covid usually focuses on symptom control, the current lack of effective pharmaceutical treatments leaves many patients seeking alternative therapies. That’s where Manual Lymphatic Drainage can make a significant difference. How MLD Helps with Long Covid Symptoms A recent study, Manual Lymph Drainage for Post-COVID-19 Related Cough, Breathlessness, and Fatigue, explored the use of MLD as a treatment for individuals suffering from persistent Long COVID symptoms. This study found that MLD helped reduce symptoms like fatigue, breathlessness, and chronic cough, with improvements starting as early as the third treatment. Patients reported increased energy levels, better sleep, and enhanced functional capacity after just a few sessions. Giovanni’s expertise with MLD can be crucial in addressing the inflammation, poor lymphatic drainage, and respiratory issues often associated with Long Covid. Key Benefits of MLD for Long Covid Symptoms Recovery: Reduces Inflammation One of the key factors contributing to Long Covid symptoms is chronic inflammation. MLD helps to reduce systemic inflammation by promoting the drainage of inflammatory waste and toxins, which can alleviate discomfort and promote healing. Improves Breathing Function Many Long Covid sufferers experience breathlessness, a symptom that can greatly affect quality of life. MLD targets the lymphatic pathways in the chest and lungs, which can help reduce inflammation in the respiratory system, clear mucus, and improve lung function. The technique also includes special “bronchitis” maneuvers that help open up the lungs and reduce coughing. Boosts Energy Levels Fatigue is one of the most disabling Long COVID symptoms. By supporting lymphatic flow and reducing congestion, MLD can improve circulation and oxygen delivery to the body’s tissues, helping to restore energy levels and combat the persistent tiredness that plagues many Long Covid sufferers. Supports Immune System Recovery Long Covid symptoms often result from an immune response gone awry. MLD can help recalibrate immune function, promote lymphatic circulation, and enhance the body’s natural ability to heal itself. Enhances Mental Clarity Brain fog and cognitive dysfunction are common complaints among people with Long Covid. By reducing inflammation and promoting better circulation, MLD may help improve mental clarity and cognitive function, allowing patients to regain focus and reduce feelings of confusion or mental fatigue. Improves Sleep Quality Many Long Covid sufferers report difficulties with sleep. By reducing pain and inflammation, MLD helps induce a relaxation response in the body, which can promote deeper, more restful sleep. Giovanni’s Approach: Tailored MLD Treatment for Long Covid Symptoms Giovanni, a skilled therapist with extensive training in the Vodder Academy’s MLD method, offers personalised treatments for those struggling with Long Covid. Each session is tailored to the individual’s specific symptoms, addressing areas such as: Chest and Lungs: To reduce inflammation and congestion Neck and Shoulders: To alleviate stiffness and promote relaxation Facial Area: For sinus congestion or post-viral inflammation Whole Body: To improve general circulation, reduce swelling, and stimulate the lymphatic system. When working with this type of presentation, it is also valid to consider a shorter initial session to ensure that MLD does not spike up your symptoms. If you are not sure what works best for you, just ask Giovanni. Giovanni’s gentle, compassionate approach helps create a safe space for clients to heal. Many clients report feeling noticeably better after just a few sessions, with improvements in breathing, energy, and mental clarity. Read here about the Melbourne Massage and Treatment testimonials. Real-World Results: Case Studies In a study of two Long Covid patients undergoing MLD treatment, both reported substantial improvements in their symptoms. After just a few sessions, they experienced reductions in breathlessness, fatigue, and overall discomfort. By the time of their follow-up treatment, both patients reported feeling the best they had since before contracting COVID-19, with increased energy, improved sleep, and less reliance on medication. Why Choose MLD for Long Covid Recovery? Non-invasive and Drug-free: MLD offers a natural, non-pharmaceutical […]
Hello, and welcome! I’m Giovanni, and today I want to share some insight into the available treatment options for lymphoedema. If you or someone you know is dealing with this condition, I understand how overwhelming it can feel to navigate the many different approaches to treatment. As someone specialising in lymphoedema management through Manual Lymphatic Drainage (MLD) and Complex Decongestive Therapy (CDT), I aim to provide a holistic approach to managing and reducing the symptoms of lymphoedema. I’ve studied with the Vodder Academy and am a Clinical Myotherapist, so my work is built on solid, evidence-based practices. But I also believe that looking at all available treatment options for lymphoedema —medical, surgical, and holistic—is key to finding a management strategy that works for you. What is Lymphoedema? Before we dive into treatment options, let me quickly touch on what lymphoedema is. Lymphoedema is a condition that causes fluid retention and swelling, usually in the arms or legs, as a result of damage or blockage to the lymphatic system. This can occur after surgery, radiation treatment, or due to inherited conditions. While lymphoedema may be chronic, the good news is that with the proper treatment, symptoms can often be managed or reduced significantly. Medical Treatment Options for Lymphoedema Medical treatments for lymphoedema typically focus on managing the fluid buildup and improving lymphatic drainage. Here’s a quick overview of what you might expect in a clinical setting: Compression Therapy Compression garments are often a cornerstone of lymphoedema management. They help reduce swelling by applying controlled pressure, which encourages the flow of lymph fluid. These garments come in different forms, including- Stocking – Sleeves – Bandages They can be custom-fitted to provide maximum comfort and effectiveness. Compression stockings are recommended to be purchased from a clinic that takes measurements of your limb and makes the stockings based on the measurements. I often refer my patients to Sigvaris in West Melbourne for these types of services.’ The benefit of this approach is that you will have a compression that is ideal for your limb, with no greater risk of fluid congestion and other side effects. Pharmaceuticals and Diuretics In some cases, medications may be prescribed to address symptoms like inflammation or to reduce fluid retention. However, it’s important to note that diuretics are generally not a primary treatment for lymphoedema, as they don’t directly address the underlying lymphatic issue. Other medications that are prescribed for Lymphoedema are creams to maintain skin moisturised in order to reduce the chance of cracking and skin damage. Manual Lymphatic Drainage (MLD) I specialise in MLD, a gentle, hands-on technique that stimulates the anastomosis of the lymphatic system and encourages the movement of excess fluid from swollen areas. MLD can be incredibly effective in reducing swelling and relieving discomfort. It works by stretching and letting the skin recoil under some really gentle pressure. This way, the lymphatic system is stimulated to work harder, and takes up the fluid to healthier parts of the body where it can be processed more efficiently. Combine Decongestive Therapy (CDT) It is part of the treatment I offer for Lymphoedema patients here at Melbourne Massage and Treatment. It consists of bandages used to compress the affected area. The compression is applied after MLD has been delivered, and it is applied to maintain fluid movement throughout the anastomosis, which is the alternative connection of the lymphatic system through which the liquid moves after the MLD stimulation. The bandages are applied and are recommended to stay on for about 24 hours. After this time, once you remove them, you will wash them, roll them and come back for another treatment. A back-to-back treatment would ensure that the swelling of the lymphoedema can be managed and reduced as quickly as possible. Laser therapy Laser therapy is a non-invasive treatment that can be used in a clinical setting to treat specific lymphoedema presentations. Indeed, Laser therapy is used when the patient already presents with fibrosis, the hardening of the skin. Low-frequency lasers are the ones used most often, and we know there are also portable pen lasers that are efficient enough for this therapy. Pneumatic compression therapy: This therapy consists of using a sleeve pump machine that gets placed over the affected area and inflates sequentially to apply pressure. The rhythmic compression helps stimulate lymphatic flow, reduces swelling, and improves circulation by encouraging the movement of excess fluid toward lymphatic drainage sites. All those therapies are recommended in combination. To start with, for the best results and quick reduction, MLD and CDT would be more effective. Surgical Treatment Options for Lymphoedema While surgery is generally considered a last resort for lymphoedema, there are certain cases where it may be necessary or beneficial: Liposuction for Lymphoedema This technique is sometimes used to remove excess fat tissue that has accumulated as a result of chronic lymphoedema. It’s not a cure, but it can help reduce the volume of swelling and improve the appearance of the affected area. Lymphovenous Anastomosis (LVA)/Bypass It involves connecting the lymphatic vessels and nearby veins, allowing excess lymph fluid to drain into the bloodstream instead of accumulating in tissues. Vascularized lymph node transfer (VLNT) a surgical technique used to treat lymphoedema by transplanting healthy lymph nodes along with their blood supply to the affected area. The transplanted lymph nodes, typically harvested from the patient’s groin or other regions, are reconnected to the recipient’s blood vessels. Lymph Node Transplantation In some specialised cases, surgeons may transplant healthy lymph nodes from one part of the body to another to help restore lymphatic drainage. This option is more complex and is usually reserved for severe, treatment-resistant lymphoedema. Surgery, of course, comes with risks and recovery time, so it is typically considered only after all other treatments have been explored. Lymphoedema Holistic Treatments: Taking a Whole-Body Approach While medical and surgical treatment options for lymphoedema can certainly help with this presentation, I firmly believe that a holistic approach is crucial for long-term success. Here are some natural and complementary therapies […]
When the lymphatic system stop working, either because for a congential malfunctioning, or because of a an external intervention, which did lead to lymphatic system damage, the individual may start experiencing symptoms of Lymphoedema. At Melbourne Massage and Treatment in Fitzroy North, Giovanni understand how challenging lymphoedema can be, which is why he provide expert care through Manual Lymphatic Drainage (MLD) and Combined Decongestive Therapy (CDT). These non-invasive treatments help manage the symptoms and improve your quality of life. What is Lymphoedema? Lymphoedema occurs when the lymphatic system is blocked or malfunctioning, leading to a buildup of lymphatic fluid. This fluid results in swelling in the affected areas, often in the arms, legs, or other extremities. Lymphoedema can be primary (a hereditary condition) or secondary (often caused by injury, surgery, or infection). The fluid that builds up in the body is a fluid that is naturally produced by the body and is released under the skin and between tissues by the bloodstream. It is reached in protein, bacteria, viruses, dust, and other minor substances that the body is unsure how to handle. Stages of Lymphoedema Lymphoedema progresses in stages, with each stage representing the severity of the condition. Recognizing the symptoms early on can help prevent the condition from advancing, so it’s important to be aware of the subtle changes in your body. Stage 0: Latent or Subclinical Stage In this early stage, there are no visible signs or symptoms of lymphoedema, but the lymphatic system may already be compromised. People in Stage 0 may experience a feeling of heaviness, discomfort, or mild swelling, int the limbs affected by this presentation, but these symptoms typically disappear after resting or with limb elevation. The fluid retention is still minimal and may not be noticed by the individual, but it can be detected through careful assessment. Stage 1: Reversible Stage At this stage, swelling is more noticeable, but the skin is still soft, and the swelling can still decrease with limb elevation and movement. When the swelling is present, the skin will feel puffy or tight, and there may be a sensation of heaviness in the affected area. In this relevant early stage, it i still easy to intervene for prevent further degeneration, and if you are unsure of what you are experiencing, reach out Giovanni for a 15 minutes free consultation, in which, at least thanks to the analysis of your clinical history, we can already evaluate if what you are experiencing is a Stage 1 Lymphoedema. Stage 2: Spontaneously Irreversible Stage In Stage 2, the swelling becomes more persistent and is not fully responsive to movement and limb elevation. The asking of the affected area may begin to feel firmer, and there can be noticeable thickening of the skin. This is the stage where fibrosis (scarring of the tissue) starts to develop, and it’s crucial to stop this from going any worse. While the swelling might fluctuate, it becomes more difficult to manage without intervention. At this point, manual treatments like Manual Lymphatic Drainage (MLD) can significantly help reduce swelling and improve the overall function of the lymphatic system. Stage 3: Lymphostatic Elephantiasis The final stage of lymphoedema is characterized by extreme swelling and thickened, hardened skin. The affected area may look large, disfigured, and become painful to the touch. Tissue fibrosis is advanced, and the skin may develop ulcerations or infections due to poor circulation and immune system function. Indeed, along with the swelling and the fibrosis buildup, the outer layer of the skin is placed further away from the blood capillary, which is responsible for releasing oxygen and other substances essential for skin regeneration.Therefore, as the skin breaks open, due to its poor condition, it is more subject to infections and contamination of pathogens. Stage 3 lymphoedema is debilitating and requires ongoing care and treatment to prevent complications and manage symptoms. At this stage, a combination of therapies such as Combined Decongestive Therapy (CDT) and MLD becomes vital for managing the swelling and restoring lymphatic flow. Common Symptoms of Lymphoedema Lymphoedema symptoms can vary from person to person and depend on the stage of the condition. The common symptoms include: Swelling: The most obvious sign of lymphoedema is swelling in the affected area, typically starting in the arms or legs. The swelling is often gradual and may worsen over the course of the day, especially after prolonged standing or sitting. Tightness or Heaviness: Affected limbs may feel heavy or tight, particularly after physical activity or at the end of the day. This sensation is often worse in the early stages and may become more pronounced as the condition progresses. Pain or Discomfort: Pain, tenderness, or discomfort in the swollen area is common, especially when there is fibrosis (hardening) of the tissues. The pain can range from mild to severe, depending on the stage. Reduced Range of Motion: As the swelling and fibrosis increase, it can lead to a limited range of motion, particularly in the arms and legs. This can impact daily activities and mobility. Skin Changes: In later stages of lymphoedema, the skin may appear thickened or leathery, with a shiny, tight appearance. There may also be visible folds in the skin, particularly around the knees, elbows, or ankles. Frequent Infections: Swollen tissues have a reduced ability to fight off infections, so people with lymphoedema are more susceptible to bacterial and fungal infections, which can further complicate the condition. Numbness or Tingling: As the swelling progresses, the nerves in the affected area may be compressed, leading to sensations of tingling, numbness, or even burning. Increased Skin Sensitivity: The skin in the affected area may become more sensitive, prone to rashes, or develop sores due to the increased swelling and poor circulation. Commonly Affected Areas of the Body Lymphoedema can affect different parts of the body, but the most common areas are: Arms: After surgery, particularly mastectomy (breast cancer surgery) that involves the removal of lymph nodes, the arms are a common site for lymphoedema. The swelling […]